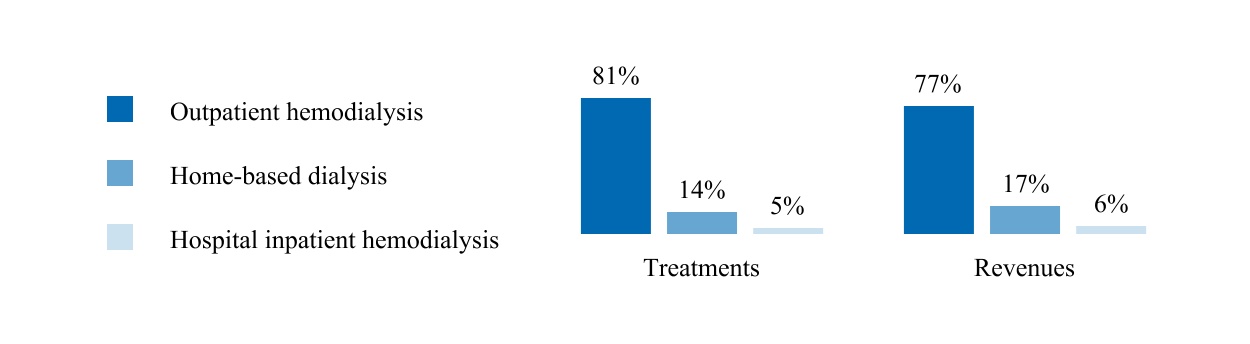UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
Washington, D.C. 20549
FORM 10-K
| | | | | |
| ☒ | ANNUAL REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
For the Fiscal Year Ended December 31, 20202023
or
| | | | | |
| ☐ | TRANSITION REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
For the transition period from ___________ to ___________
Commission File Number: 1-14106
DAVITA INC.
(Exact name of registrant as specified in charter)
| | | | | | | | |
| Delaware | | 51-0354549 |
| (State of incorporation) | | (I.R.S. Employer Identification No.) |
| | | | | | | | |
| 2000 16th Street |
| Denver, | CO | 80202 |
Telephone number (720) 631-2100
Securities registered pursuant to Section 12(b) of the Act:
| | | | | | | | | | | | | | |
| Title of each class: | | Trading symbol(s): | | Name of each exchange on which registered: |
| Common Stock, $0.001 par value | | DVA | | New York Stock Exchange |
Securities registered pursuant to Section 12(g) of the Act:
None
Indicate by check mark if the registrant is a well-known seasoned issuer, as defined in Rule 405 of the Securities Act. Yes ☒ No ☐
Indicate by check mark if the registrant is not required to file reports pursuant to Section 13 or Section 15(d) of the Exchange Act. Yes ☐ No ☒
Indicate by check mark whether the registrant (1) has filed all reports required to be filed by Section 13 or 15(d) of the Securities Exchange Act of 1934 during the preceding 12 months (or for such shorter period that the registrant was required to file such reports) and (2) has been subject to such filing requirements for the past 90 days. Yes ☒ No
Indicate by check mark whether the registrant has submitted electronically every Interactive Data File required to be submitted pursuant to Rule 405 of Regulation S-T (§232.405 of this chapter) during the preceding 12 months (or for such shorter period that the registrant was required to submit such files). Yes ☒ No ☐
Indicate by check mark whether the registrant is a large accelerated filer, an accelerated filer, a non-accelerated filer, a smaller reporting company, or an emerging growth company. See the definitions of “large"large accelerated filer,” “accelerated" "accelerated filer,” “smaller" "smaller reporting company”company" and “emerging"emerging growth company”company" in Rule 12b-2 of the Exchange Act:
| | | | | | | | | | | | | | | | | |
| Large accelerated filer | ☒ | | | Accelerated filer | ☐ |
| Non-accelerated filer | ☐ | | Smaller reporting company | ☐ |
| | | | Emerging growth company | ☐ |
If an emerging growth company, indicate by check mark if the registrant has elected not to use the extended transition period for complying with any new or revised financial accounting standards provided pursuant to Section 13(a) of the Exchange Act. ☐
Indicate by check mark whether the registrant has filed a report on and attestation to its management's assessment of the effectiveness of its internal control over financial reporting under Section 404(b) of the Sarbanes-Oxley Act (15 U.S.C. 7262(b)) by the registered public accounting firm that prepared or issued its final report. ☒
Indicate by check mark whether the registrant is a shell company (as defined in Rule 12b-2 of the Exchange Act). Yes ☐ No ☒
If securities are registered pursuant to Section 12(b) of the Act, indicate by check mark whether financial statements of the registrant included in the filing reflect the correction of an error to previously issued financial statements. ☐
Indicate by check mark whether any of those error corrections are restatements that required a recovery analysis of incentive-based compensation received by any of the registrant’s executive officers during the relevant recovery period pursuant to §240.10D-1(b). ☐
As of June 30, 2020,2023, the aggregate market value of the Registrant'sregistrant's common stock outstanding held by non-affiliates based upon the closing price on the New York Stock Exchange was approximately $9.7$9.2 billion.
As of January 29, 2021,31, 2024, the number of shares of the Registrant’sregistrant’s common stock outstanding was approximately 109.487.7 million shares.
Documents incorporated by reference
Portions of the Registrant’sregistrant’s proxy statement for its 20212024 annual meeting of stockholders are incorporated by reference in Part III of this Form 10-K.
DAVITA INC.
INDEX
| | | | | | | | | | | | | | |
| | | | | Page No. |
| | | PART I. | | |
| Item 1. | | | | |
| Item 1A. | | | | |
| Item 1B. | | | | |
| Item 1C. | | | | |
| Item 2. | | | | |
| Item 3. | | | | |
| Item 4. | | | | |
| | | | | |
| | | PART II. | | |
| Item 5. | | | | |
| Item 6. | | | | |
| Item 7. | | | | |
| Item 7A. | | | | |
| Item 8. | | | | |
| Item 9. | | | | |
| Item 9A. | | | | |
| Item 9B. | | | | |
| Item 9C. | | | | | |
| | | | |
| | PART III. | | |
| Item 10. | | | | |
| Item 11. | | | | |
| Item 12. | | | | |
| Item 13. | | | | |
| Item 14. | | | | |
| | | | |
| | PART IV. | | |
| Item 15. | | | | |
| Item 16. | | | | |
| | | | |
| | | | |
| | | | |
PART I
Item 1. Business
Unless otherwise indicated in this Annual Report on Form 10-K “DaVita”report "DaVita", “the Company” “we”"the Company" "we", “us”"us", “our”"our" and other similar terms refer to DaVita Inc. and its consolidated subsidiaries. Our annual report on Form 10-K, quarterly reports on Form 10-Q, current reports on Form 8-K and amendments to those reports filed or furnished pursuant to section 13(a) or 15(d) of the Securities Exchange Act of 1934, as amended, are made available free of charge through our website, located at http://www.davita.com, as soon as reasonably practicable after the reports are filed with or furnished to the Securities and Exchange Commission (SEC). The SEC also maintains a website at http://www.sec.gov where these reports and other information about us can be obtained. The contents of our website are not incorporated by reference into this report.
Overview of DaVita Inc.
DaVita is a leading healthcare provider focused on transforming care delivery to improve quality of life for patients globally. We are one of the largest providers of kidney care services in the U.S. and have been a leader in clinical quality and innovation for overmore than 20 years. DaVita isWe care for our patients at every stage and setting along their kidney health journey–including earlier diagnosis and prevention, supporting the transplant process, helping with end of life and ensuring they are supported at home, in our dialysis centers, in the hospital and/or skilled nursing facilities and at the end of life. We are committed to bold, patient-centric care models, implementing the latest technologies and moving towardadvancing integrated care offerings. Over the years,In our unwavering pursuit of a healthier tomorrow, we have established a value-based culture with a philosophy of caring that is focused on both our patients and teammates. This culture and philosophy fuel our continuous drive toward achieving our mission to be the provider, partner and employer of choicechoice.
There are five stages of chronic kidney disease (CKD). These stages are generally based on how well the kidneys work to filter waste and fulfilling our visionextra fluid out of the blood–with higher stages of CKD corresponding to "buildprogressing levels of kidney disease. Stage 1 CKD is the greatest healthcare communityclosest to healthy kidney function. Stage 5 classification indicates that a patient has severe kidney damage.
A patient diagnosed with Stage 5 CKD has kidneys that have lost nearly all functionality or have failed. If the world has ever seen."
Thepatient's kidneys fail, they are then diagnosed with end stage renal disease (ESRD), also known as end stage kidney disease (ESKD). Because loss of kidney function is normally irreversible. Kidney failure is typically caused by Type I and Type II diabetes, hypertension, polycystic kidney disease, long-term autoimmune attack on the kidneys and prolonged urinary tract obstruction. End stage renal disease or end stage kidney disease (ESRD or ESKD) is the stage of advanced kidney impairment that requiresirreversible, ESKD patients require continued dialysis treatments or a kidney transplant to sustain life. Dialysis is the removal of toxins, fluids and salt from the blood of patients by artificial means. Patients suffering from ESRDESKD generally require regular life-sustaining dialysis at least three times a weektherapy for the rest of their lives.lives or until they receive a kidney transplant.
The treatment goal for CKD patients prior to Stage 5 is to manage and slow the progression of the disease to preserve kidney functionality. Because kidney failure is typically caused by one or more comorbidities such as Type I and Type II diabetes, hypertension, polycystic kidney disease, long-term autoimmune attack on the kidneys or prolonged urinary tract obstruction, slowing the progression generally involves working with nephrologists or dieticians to help control blood pressure, monitor blood glucose and maintain healthy diet and exercise routines, among other things. If the kidney disease continues to progress, the goal is to safely transition the patient to the dialysis treatment of their choice.
Our businesses
We are one of the two largest dialysis providers in the United States. Our U.S. dialysis and related lab services (U.S. dialysis) business treats patients with chronic kidney failure, and ESRDESKD, in the United States, and is our largest line of business. As of December 31, 2020, we provided dialysis and administrative services and related laboratory services throughout the U.S. via a network of 2,816 outpatient dialysis centers in 46 states and the District of Columbia, serving a total of approximately 204,200 patients and provided hospital inpatient dialysis services in approximately 900 hospitals. Our robust platform to deliver kidney care services also includes established nephrology and payor relationships as well as home programs. relationships.
In addition, as of December 31, 2020, we2023, our international operations provided dialysis and administrative services to a total of 321367 outpatient dialysis centers located in ten11 countries outside of the U.S., serving approximately 36,20049,400 patients. The Company
Finally, our U.S. integrated kidney care (IKC) business provided integrated care and disease management services to 58,000 patients in risk-based integrated care arrangements and to an additional 17,000 patients in other integrated care arrangements across the United States as of December 31, 2023.
We also consists of ourmaintain a few other ancillary services and strategic initiatives, which include the aforementionedinvestments outside of our U.S. dialysis, U.S. IKC, or international operations, (collectively, our ancillary services), as wellwhich we refer to as our U.S. other ancillary services.
We refer to our U.S. integrated kidney care business, U.S. other ancillary services and international operations as, collectively, our "ancillary services." We also have a separate corporate administrative support.support function that supports our U.S. dialysis business and these ancillary services. Each of our businesses are described in greater detail in the sections that follow.
Our care model
Our patient-centric care model leverages our platform of kidney care services to maximize patient choice in both models and modalities of care. We believe that the flexibility we offer coupled with a focus on comprehensive kidney care supports our commitments to help improve equitable clinical outcomes and quality of life for our patients. ForAccording to the eighth consecutive year,most recently published data, for the nine most recently reported years, we arehave continued as an industry leader in the Centers for Medicare & Medicaid Services’ (CMS) Quality Incentive Program (QIP), which promotes high quality services in outpatient dialysis facilities treating patients with ESRD. We areESKD. In addition, according to the most recently published data, for the eight most recently reported years, we have also continued as an industry leader for the seventh consecutive year under CMS’ Five-Star Quality Rating system, which rates eligible dialysis centers based on the quality of outcomes to help patients, their families, and caregivers make more informed decisions about where patients receive care. AccordingWe have seen strong results from our participation in the ESRD Treatment Choices (ETC) Model, which was launched by the CMS Center for Medicare and Medicaid Innovation (CMMI) in January 2021 with the stated intent to "encourage greater use of home dialysis and kidney transplants for Medicare beneficiaries with ESKD, while reducing Medicare expenditures and preserving or enhancing the most recently collected data, we are an industry leader for the total numberquality of patients in home-based dialysis services.care furnished to beneficiaries with ESKD."
Our quality clinical outcomes are driven by our experienced and knowledgeable teammates.caregivers. We employ registered nurses, licensed practical or vocational nurses, patient care technicians, social workers, registered dietitians, biomedical technicians and other administrative and support teammates who strive to achieve superior clinical outcomes at our dialysis facilities. In addition to our teammates at our dialysis facilities, as of December 31, 2020,2023, our domestic Chief Medical Officer leads a team of 18 senior22 nephrologists in our physician leadership team as part of our domestic Office of the Chief Medical Officer (OCMO). Our international Chief Medical Officer leads a team of 11 seniornine nephrologists in our physician leadership team as part of our international OCMO.OCMO as of December 31, 2023. Our OCMO teammates represent a variety of academic, clinical practice, and clinical research backgrounds. We also have a Physician CounselCouncil that serves as an advisory body to senior management, which iswas composed of nine10 physicians with extensive experience in clinical practice and have sevenfive Group Medical Directors as of December 31, 2020.2023.
On June 19, 2019,collaboration between nephrologists, providers, and transplant programs, resulting in a more complete understanding of each patient’s clinical needs. We believe this more complete understanding allows for better care coordination and earlier intervention, which we completed the salebelieve ultimately leads to improved clinical outcomes, lower overall costs and improved patient experiences. Our IKC business provides comprehensive care management for complex chronic kidney disease patients nationwide, with payment models that include a variety of structures to advance and encourage integrated and value-based care. Among other arrangements, our DaVita Medical Group (DMG) business, a patient and physician-focused integrated healthcare delivery and management company, to Collaborative Care Holdings, LLC, a subsidiary of UnitedHealth Group Inc. As a result, the DMGIKC business has been classified as discontinued operationspercent-of-premium arrangements in several Medicare Advantage ESRD Chronic Special Needs Plans and its resultsis an active participant in CMMI’s Comprehensive Kidney Care Contracting (CKCC) model that seeks to manage the care of operations are reported as discontinued operations for all periods presented inlate stage CKD and ESKD patients to delay the consolidated financial statements included in this report.
For financial information about DMG, see Note 22 to the consolidated financial statements included in this report.
COVID-19 and its impact on our business
As a caregiving organization, we are exposed to and will continue to be impacted by the effectsprogression of the novel coronavirus (COVID-19) pandemic. DaVita’s teammates include, among others, dialysis nurses, patient care technicians, social workers, dieticians and other caregivers who are on the front lines of the ongoing COVID-19 pandemic providing critical, life-sustaining care for our patients. We are closely monitoring the impact on our business of the pandemic and the resulting economic environment, including the impact on our patients, teammates, physician partners, suppliers, vendors and business partners.
During this time of great challenge, our top priorities continue to be the health, safety and well-being of our patients, teammates and physician partners and helping to ensure that our patients have the ability to maintain continuity of care throughout this crisis, whether in the hospital, outpatient or home setting. To that end, we have dedicated and continue to dedicate substantial resources in response to COVID-19, including the implementation of additional protocols in coordination with the Centers for Disease Control and Prevention (CDC) on infection control and clinical best practices to help safely maintain continuity of care for our patients and help protect our caregivers. We also have been collaborating with the CDC, the U.S. Department of Health and Human Services (HHS), CMS, the American Society of Nephrology, and dialysis providers nationwide to help ensure that the dialysis community is able to support patients nationwide during this global health crisis.
The protocols and initiatives we have implemented in response to COVID-19 include steps designed to implement dedicated care shifts for patients with confirmed or suspected COVID-19 and other enhanced clinical practices, including procuring additional equipment and clinical supplies, including personal protective equipment (PPE) and providing financial support to our teammates associated with relief reimbursement. These efforts are part of a wider Prepare, Prevent, Respond and Recover protocol that we have implemented in connection with the pandemic, which also includes operational protocols such as the redistribution of teammates, machines and supplies across the country as needed and increased investment in and utilization of telehealth capabilities. We also have maintained business process continuity during the pandemic by enabling most back office teammates to work remotely. Our response protocol generally has allowed us to maintain continuity of care for our patients and we carefully monitor the efficacy of these protocols and their impact on our operations and strategic priorities as the pandemic continues. If we are required to maintain certain restrictive operational initiatives for an extended period of time, it may adversely impact our strategic initiatives, such as our strategy to continue to build on our abilities to offerkidney disease, promote home dialysis, options. Certain temporary changes madeand incentivize transplants. Our IKC business also utilizes other value-based payment methodologies in response to the COVID-19 pandemic could become permanent,its care coordination and disease management contracts, which could have an adverse impact on our business. In addition, any staffing shortages or disruptions, or any equipment or clinical supply shortages, disruptions or delays or associated price increases, could impact our ability to provide dialysis services or the cost of providing those services. Due in part to the protocolsinclude two-sided shared savings/shared losses and initiatives described above, we have incurred significant costs related to COVID-19 in 2020, and we expect to continue to incur extended and significant additional costs in connection with our response to COVID-19.
We have worked with certain government agencies to respond to the COVID-19 pandemic, and in certain cases have sought waivers of regulatory requirements. We also are working to help make COVID-19 vaccines available to our patients and teammates, including through coordination with state and federal governments on direct vaccine distribution so that we can administer vaccines to our patients and teammates. These vaccines are currently available under emergency use authorizations, and there can be no assurance that our patients and caregivers will choose to receive a COVID-19 vaccine or that the vaccines will prove to be as safe and effective as currently understood by the scientific community. In addition, we may encounter difficulties with the availability and storage of the vaccines, or administration of the vaccines, some of which have multiple dose requirements. We operate in a complex and highly regulated environment, and the novel nature of our COVID-19 response, including, for example, with respect to regulatory waivers and our administration of the newly developed COVID-19 vaccines, may increase our exposure to legal, regulatory and clinical risks.
In addition, the Coronavirus Aid, Relief, and Economic Security (CARES) Act and subsequent COVID-19 relief legislation temporarily suspended Medicare’s 2% sequestration from May 1, 2020 through December 31, 2020, and the Consolidated Appropriations Act subsequently extended this sequestration suspension until March 31, 2021. While in effect, this legislation, has increased, and will continue to increase, our revenues. Furthermore, a significant initial part of the federal government response to the COVID-19 pandemic was the CARES Act's authorization of $100 billion in funding to be distributed to healthcare providers through the federal Public Health and Social Services Emergency Fund (Provider Relief Fund). While we declined approximately $250 million of government funding received in the second quarter of 2020 from the
Provider Relief Fund, certain of our competitors accepted such funds. There can be no assurance that financial or other assistance will be available from the government if we have a need for such assistance in the future.
We believe the ultimate impact of this public health crisis on the Company will depend on future developments that are highly uncertain and difficult to predict, including among other things the severity and duration of the pandemic; further spread or resurgence of the virus, including as a result of the emergence of new strains of the virus; its impact on the CKD patient population and our patient population; the availability, acceptance, impact and efficacy of COVID-19 vaccines and other treatments or therapies; the pandemic’s continuing impact on the U.S. and global economies and unemployment; the responses of our competitors to the pandemic and related changes in the marketplace; and the timing, scope and effectiveness of federal, state and local governmental responses.
For additional discussion of the COVID-19 pandemic and our response, including its impact on us and related risks and uncertainties, please see the discussion below under the heading "Human Capital Management", as well as the risk factor in Item 1A Risk Factors under the heading “We face various risks related to the dynamic and evolving novel coronavirus pandemic, any of which may have a material adverse impact on us,” and Item 7. Management’s Discussion and Analysis of Financial Condition and Results of Operations.outcomes-based pay-for-performance compensation arrangements.
U.S. dialysis business
Our U.S. dialysis business is a leading provider of kidney dialysis services for patients suffering from ESRD.ESKD. As of December 31, 2020,2023, we provided dialysis, administrative and administrativerelated laboratory services in the U.S. through a network of 2,8162,675 outpatient dialysis centers in 46 states and the District of Columbia, serving a total of approximately 204,200200,800 patients. We also have contracts to provide hospital inpatient dialysis services in approximately 900790 hospitals and related laboratory services throughout the U.S.
According to the United States Renal Data System (USRDS), there were over 555,000 ESRD556,000 ESKD dialysis patients in the U.S. in 2018.2021. Based on the most recent 20202023 annual data report from the USRDS, the underlying ESRDESKD dialysis patient population has growngrew at an approximate compound annual rate of 3.7%3.3% from 20082011 to 20182021 and 3.4% from 2016 to 2021 as compared to a decline in compound rateannual growth of 3.5%1.1% from 20132020 to 2018,2021, which suggests that the rate of growth of the ESRDESKD patient population is declining relative to long term trends. AAs the USRDS report presents data through December 31, 2021, it reflects the initial compounding impact of COVID-19 on this patient base. In general, a number of factors may impact ESRDESKD growth rates, including, among others, mortality rates for dialysis patients or CKD patients, the aging of the U.S. population, transplant rates, incidence rates for diseases that cause kidney failure such as diabetes and hypertension, mortality rates for dialysis patients and growth rates of minority populations with higher than average incidence rates of ESRD.ESKD or other changes in demand for dialysis treatments over time, including for example, as a result of the development and application of certain innovative technologies, drugs or other treatments. Certain of these factors, in particular mortality rates for dialysis or CKD patients, have been impacted by the COVID-19 pandemic.
Since 1972, the federal government has provided healthcare coverage for ESRD patients under the Medicare ESRD program regardless of age or financial circumstances. ESRD is the first and only disease state eligible for Medicare coverage both for dialysis and dialysis-related services and for all benefits available under the Medicare program. For patients with Medicare coverage, all ESRD payments for dialysis treatments are made under a single bundled payment rate. See page 7 for further details.
Although Medicare reimbursement limits the allowable charge per treatment, it provides industry participants with a relatively predictable and recurring revenue stream for dialysis services provided to patients without commercial insurance. For the year ended December 31, 2020, approximately 90% of our total dialysis patients were covered under some form of government-based program, with approximately 74% of our dialysis patients covered under Medicare and Medicare Advantage plans.
Treatment options for ESRDESKD
Treatment options for ESRDESKD are dialysis and kidney transplantation.
Dialysis options
•Hemodialysis
Hemodialysis is the most common form of ESRD treatment, is usually performed at a freestanding outpatient dialysis center, at a hospital-based outpatient center, or at the patient’s home.ESKD treatment. The hemodialysis machine uses an artificial kidney,a filter, called a dialyzer, to remove toxins, fluids and salt from the patient’s blood. The dialysis process occurs across a semi-permeable membrane that divides the dialyzer into two distinct chambers. While blood is circulated through one chamber, a pre-mixed fluid is circulated through the other chamber. The toxins, salt and excess fluids from the blood cross the membrane into the fluid, allowing cleansed blood to return back into the patient’s body. Each hemodialysis treatment that occurs
Hemodialysis is usually performed at a freestanding outpatient dialysis center, at a hospital-based outpatient center, in a skilled nursing facility or at the patient's home. Our freestanding outpatient dialysis centers typically lasts approximately threeare staffed with members of our care team and one-half hours and isstore the supplies necessary for treatment. Treatments are usually performed three times per week.
Hospital inpatient hemodialysis services are required for patients with acute kidney failure primarily resulting from trauma, patients in early stages of ESRDESKD and ESRDESKD patients who require hospitalization for other reasons. Hospital inpatient hemodialysis is generally performed at the patient’s bedside or in a dedicated treatment room in the hospital, as needed.
Some ESRDESKD patients who are healthier and more independent may perform home hemodialysis with the help of a care partner in their home or residence through the use of a hemodialysis machine designed specifically for home therapy that is portable, smaller and easier to use. Patients receive training, support and monitoring from registered nurses, usually in our outpatient dialysis centers, in connection with their home hemodialysis treatment. Home hemodialysis is typically performed with greater frequency than dialysis treatments performed in outpatient dialysis centers and on varying schedules.
•Peritoneal dialysis
Peritoneal dialysis uses the patient’s peritoneal or abdominal cavity to eliminate fluid and toxins and is typically performed at home. The most common methods of peritoneal dialysis are continuous ambulatory peritoneal dialysis (CAPD) and continuous cycling peritoneal dialysis (CCPD). Because it does not involve going to an outpatient dialysis center three times a week for treatment, peritoneal dialysis is generally an alternative to hemodialysis for patients who are healthier, more independent and desire more flexibility in their lifestyle.
CAPD introduces dialysis solution into the patient’s peritoneal cavity through a surgically placed catheter. Toxins in the blood continuously cross the peritoneal membrane into the dialysis solution. After several hours, the patient drains the used dialysis solution and replaces it with fresh solution. This procedure is usually repeated four times per day.
CCPD is performed in a manner similar to CAPD, but uses a mechanical device to cycle dialysis solution through the patient’s peritoneal cavity while the patient is sleeping or at rest.
Kidney transplantation
Although kidney transplantation, when successful, is generallyconsidered the most desirable form of therapeutic intervention, the shortage of suitable donors, side effects of immunosuppressive pharmaceuticals given to transplant recipients and dangers associated with transplant surgery for some patient populations have generally limited the use of this treatment option. AnIn accordance with an executive order signed in July 2019 (the 2019 Executive Order) directed, the HHS to developU.S. Department of Health and Human Services (HHS) developed policies addressing, among other things, the goal of making more kidneys available for transplant. As directed by the 2019 Executive Order, the CMS, through its Center for Medicare and Medicaid Innovation (CMMI),CMMI, also subsequently released the framework for certain proposed and existing voluntary and mandatory payment models, thatincluding ETC described above, which would adjust payment incentives to encourage kidney transplants. For more information regarding the 2019 Executive Order andabout these payment models, please see the discussion below under the heading “-"—New models of careIntegrated Kidney Care and Medicare and Medicaid program reforms.”"
U.S. dialysis services we provide
Outpatient hemodialysis services
As of December 31, 2020, we operated or provided administrative services through a network of 2,816 outpatient dialysis centers in the U.S. that are designed specifically for outpatient hemodialysis. In 2020, our overall network of U.S. outpatient dialysis centers increased by 63 primarily as a result of the opening of new dialysis centers and acquisitions, net of center closures, representing a total increase of approximately 2.3% from 2019.
As a condition of our enrollment in Medicare for the provision of dialysis services, we contract with a nephrologist or a group of associated nephrologists to provide medical director services at each of our dialysis centers. In addition, other nephrologists may apply for practice privileges to treat their patients at our centers. Each center has an administrator, typically a registered nurse, who supervises the day-to-day operations of the center and its staff. The staff of each center typically consists
of registered nurses, licensed practical or vocational nurses, patient care technicians, a social worker, a registered dietician, biomedical technician support and other administrative and support personnel.
Under Medicare regulations, we cannot promote, develop or maintain any kind of contractual relationship with our patients that would directly or indirectly obligate a patient to use or continue to use our dialysis services, or that would give us any preferential rights other than those related to collecting payments for our dialysis services. Our total patient turnover at centers we consolidate, which is based upon all causes, averaged approximately 25%26% in 20202023 and 24%27% in 2019.2022. The overall number of patients to whom we provided services in the U.S. in 2020 decreased2023 increased by approximately 1.3%0.7% from 2019,2022, primarily due to an increasegrowth in new admits as well as a decrease in mortality rates, which havehad been impacted bythroughout the course of the COVID-19 pandemic, and a decline in new admissions. This was partially offset by new dialysis patients who started treating at our centers during the year from acquisitions and non-acquired growth.
Hospital inpatient hemodialysis services
As of December 31, 2020,2023, we providedhave contracts to provide hospital inpatient hemodialysis services, excluding physiciandialysis services to patients in approximately 900790 hospitals throughout the U.S. We render these services based on a contracted per-treatment fee that is individually negotiated with each hospital. When a hospital requests our services, we typically administer the dialysis treatment at the patient’s bedside or in a dedicated treatment room in the hospital, as needed.
Home-based dialysis services
Home-based dialysis services includes home hemodialysis and peritoneal dialysis. Many of our outpatient dialysis centers offer certain support services for dialysis patients who prefer and are able to perform either home hemodialysis or peritoneal dialysis in their homes. Home-based hemodialysis support services consist of providing equipment and supplies, training, patient monitoring, on-call support services and follow-up assistance. Registered nurses train patients and their families or other caregivers to perform either home hemodialysis or peritoneal dialysis. The 2019 Executive Order and related HHS guidance described above also included a stated goal of increasing the relative number of new ESRDESKD patients that receive dialysis at home as compared to those receiving dialysis in center or at a hospital.home.
According to the most recent 20202023 annual data report from the USRDS, in 20182021 approximately 12%15% of ESRDESKD dialysis patients in the U.S. performperformed home-based dialysis.
Treatments and revenues by modality:
The following graph summarizes our U.S. dialysis treatments by modality and U.S. dialysis patient servicesservice revenues by modality for the year ended December 31, 2020.2023.
Other
ESRDESKD laboratory services
We operate onea separately licensed and highly automated clinical laboratory which specializes in ESRDESKD patient testing. This specialized laboratory provides routine laboratory tests for dialysis and other physician-prescribed laboratory tests for ESRD patients which are integral componentsESKD patients. The vast majority of the overall dialysis services that we provide. Our laboratory provides these tests predominantlyare performed for our network of ESRDESKD patients throughout the U.S. These tests are performed for a variety of reasons, including to monitor a patient’s ESRDESKD condition, including the adequacy of dialysis, as well as other medical conditions of the patient. Our laboratory utilizes information systems which provide information to certain members of the dialysis centers’ staff and medical directors regarding critical outcome indicators.
Management services
We currently operate or provide management and administrative services pursuant to management and administrative services agreements to 5359 outpatient dialysis centers located in the U.S. in which we either own a noncontrolling interest or which are wholly-owned by third parties. Management fees are established by contract and are recognized as earned typically based on a percentage of revenues or cash collections generated by the outpatient dialysis centers.
Sources of revenue—concentrations and risks
Our U.S. dialysis revenues represent approximately 91%89% of our consolidated revenues for the year ended December 31, 2020.2023. Our U.S. dialysis revenues are derived primarily from our core business of providing dialysis services and related laboratory services and, to a lesser extent, the administration of pharmaceuticals and management fees generated from providing management and administrative services to certain outpatient dialysis centers, as discussed above.
The sources of our U.S. dialysis revenues are principally from government-based programs, including Medicare and Medicare Advantage plans, Medicaid and managed Medicaid plans, other government-based programs including our agreement with the Veterans Administration, and commercial insurance plans. Our largestThe following table summarizes our U.S. dialysis revenues by payor source of revenue is from Medicare and Medicare Advantage plans which accounted for 57% of our overall U.S. dialysis patient servicesservice revenues for the year ended December 31, 2020. Other sources of our U.S. dialysis patient services revenues for the year ended December 31, 2020, were from commercial payors (including hospital inpatient dialysis services) accounting for 32% of revenues, Medicaid and managed Medicaid plans accounting for 7% of our revenues and other government programs accounting for 4% of our revenues.2023:
| | | | | |
| Medicare and Medicare Advantage plans | 56 | % |
| Medicaid and managed Medicaid plans | 8 | % |
| Other government-based programs | 3 | % |
| Total government-based programs | 67 | % |
| Commercial (including hospital dialysis services) | 33 | % |
| Total U.S. dialysis patient service revenues | 100 | % |
Medicare revenue
Medicare fee for service
Since 1972, the federal government has provided healthcare coverage for qualified ESRD revenuepatients under the Medicare ESRD program regardless of age or financial circumstances. ESRD is the first and only disease state eligible for Medicare coverage both for dialysis and dialysis-related services and for all benefits available under the Medicare program.
Government dialysis related payment rates in the U.S. are principally determined by federal Medicare and state Medicaid policy. For patients with Medicare coverage, all ESRD payments for dialysis treatments are made under a single bundled payment rate which provides a fixed payment rate to encompass all goods and services provided during the dialysis treatment that are related to the dialysis treatment, including certain pharmaceuticals, such as Epogen® (EPO)erythropoiesis-stimulating agents (ESAs), calcimimetics, vitamin D analogs and iron supplements, irrespective of the level of pharmaceuticals administered to the patient or additional services performed. Prior to January 2021, calcimimetics, a drug class taken by many patients with ESRD to treat mineral bone disorder, was separately billable through a transitional drug add-on payment adjustment (TDAPA); however, since January 1, 2021 and as described more fully below, calcimimetics has been included in the ESRD bundled payment. Most lab services are also included in the bundled payment.
Although Medicare reimbursement limits the allowable charge per treatment, it provides industry participants with a relatively predictable and recurring revenue stream for dialysis services provided to patients without commercial insurance. For the year ended December 31, 2023, approximately 89% of our total U.S. dialysis patients were covered under some form of government-based program, with approximately 74% of our dialysis patients covered under Medicare and Medicare Advantage plans.
Under this ESRD Prospective Payment System (PPS), the bundled payments to a dialysis facility may be reduced by as much as 2% based on the facility’s performance in specified quality measures set annually by CMS through its QIP. CMS established QIP through the Medicare Improvements for Patients and Providers Act of 2008 to promote high quality services in outpatient dialysis facilities treating patients with ESRD. QIP associates a portion of Medicare reimbursement directly with a facility’s performance on quality of care measures. Reductions in Medicare reimbursement result when a facility’s overall score on applicable measures does not meet established standards. The bundled payment rate is also adjusted for certain patient characteristics, a geographic usage index and certain other factors.
Uncertainty about future payment rates remains a material risk to our business, as well as the potential implementation of or changes in coverage determinations or other rules or regulations by CMS or Medicare Administrative Contractors that may impact reimbursement. An important provision in the Medicare ESRD statute is an annual adjustment, or market basket update, to the ESRD PPS base rate. Absent action by Congress, the ESRD PPS base rate is automatically updated annually by a formulaican inflation adjustment.adjustment based on historical data and forecasts and does not always cover the actual inflationary increase. Due in part to continued higher than expected inflation rates, the annual update for the 2024 ESRD PPS base rate did not accurately forecast the cost increase experienced by providers.
On September 18, 2020, pursuant to the 2019 Executive Order, CMS, through CMMI, published the final ESRD Treatment Choices mandatory payment model (ETC).ETC Model. The ETC Model launched on January 1, 2021, and will be administered through CMMI and in approximately 30% of our dialysis clinics across the country. CMS subsequently issued several clarifying rules through November 2022 and continues to evaluate the model.
On November 9, 2020,October 27, 2023, CMS issued a final rule to update the Medicare ESRD PPS payment rate and policies.policies for calendar year 2024. Among other things, the final rule providedupdates the Acute Kidney Injury dialysis payment rate for the inclusion of calcimimetics in the ESRD bundled payment as described above; specified TDAPAs for certain new renal dialysis drugsservices furnished by ESRD facilities and biological products; and amended the reporting measures inrequirements for the ESRD QIP. CMS estimates that the overall impact of the final rule will increase ESRD facilities’ average reimbursement by 1.6%2.1% in 2021.2024.
As a result of the Budget Control Act of 2011 (BCA) and subsequent activity in Congress, a $1.2 trillion sequester (across-the-board spending cuts) in discretionary programs took effect in 2013 reducing Medicare payments (currently by 2%), which was subsequently extended through fiscal year 2027. The CARES Act that was signed into law on March 27, 2020 included a provision that2032. Federal COVID-19 relief legislation suspended the 2% Medicare sequestration from May 1, 2020 through December 31, 2020,2021. The Protecting Medicare and the Consolidated AppropriationsAmerican Farmers from Sequester Cuts Act, 2021 signed into law on December 27, 202010, 2021, extended the suspension of the 2% Medicare sequestration untilfrom December 31, 2021 through March 31, 2021. In the year ended December 31, 2020, our revenues increased due to this suspension2022, with 1% Medicare sequestration beginning April 1, 2022 through June 30, 2022 and we estimate that this suspension will increase our revenues while it remains in effect. When the temporary suspension is no longer2% Medicare sequestration beginning July 1, 2022 and thereafter. While in effect, the across-the-board spending cutssuspension of the BCA will continue to adversely affectsequestration significantly increased our business, results of operations, financial condition and cash flows.revenues.
Most ESRD patients receiving dialysis services become eligible for primary Medicare coverage at various times, depending on their age or disability status, as well as whether they are covered by a commercial insurance plan. Generally, for a patient not covered by a commercial insurance plan, Medicare becomescan become the primary payor for ESRD patients receiving dialysis services either immediately or after a three-month waiting period. ForIn most cases, for a patient covered by a commercial insurance plan, Medicare generally becomeswill either become the primary payor after 33 months, which includes the three-month waiting period, or earlier if the patient’s commercial insurance plan coverage terminates.terminates or if the patient chooses Medicare over the commercial plan. When Medicare becomes the primary payor, the payment rates we receive for
that patient shift from the commercial insurance plan rates to Medicare payment rates, which are on average significantly lower than commercial insurance rates.
Medicare pays 80% of the amount set by the Medicare system for each covered dialysis treatment. The patient is responsible for the remaining 20%. In mostmany cases, a secondary payor, such as Medicare supplemental insurance, a state Medicaid program or a commercial health plan, covers all or part of these balances. Some patients who do not qualify for Medicaid, but otherwise cannot afford secondary insurance in the form of a Medicare Supplement Plan, can apply for premium payment assistance from charitable organizations to obtain secondary coverage. If a patient does not have secondary insurance coverage, we are generally unsuccessful in our efforts to collect from the patient the remaining 20% portion of the ESRD composite rate that Medicare does not pay. However, we are able to recover some portion of this unpaid patient balance from Medicare through an established cost reporting process by identifying these Medicare bad debts on each center’s Medicare cost report.
In recent years, federal legislative and executive action has been focused on developing new models of kidney care for Medicare beneficiaries. For additional detail on thesecharitable premium assistance and other developments in models of care,certain associated risks, see the discussion belowrisk factor in Item 1A. Risk Factors under the heading “—New models of care"Changes in federal and Medicare and Medicaid program reforms.”state healthcare legislation or regulations..."
Medicare Advantage revenue
Medicare Advantage (MA, managed Medicare or Medicare Part C) plans are offered by private health insurers who contract with CMS to provide their members with Medicare Part A, Part B and/or Part D benefits. These MA plans include health maintenance organizations, preferred provider organizations, private fee-for-service (FFS) organizations, special needs plans (SNPs) or Medicare medical savings account plans. The 21st Century Cures Act (the Cures Act) included a provision that, effective January 1, 2021, allowshas allowed Medicare-eligible beneficiaries with ESRD to choose coverage under an MA plan. Prior to the Cures Act, MA plans were only available to ESRD patients if the patient was remaining on an MA plan that they had enrolled in prior to being diagnosed with ESRD, or in certain other limited situations such as a SNP. As a result, this provision under the Cures Act could broadenhas broadened access for Medicare ESRD patients to certain enhanced benefits offered by MA plans. MA plans usually provide reimbursement to us at a negotiated rate that is generally higher than Medicare FFS rates. In February 2023, CMS released the CY 2024 MA Advance Notice (the Notice). Among other changes, the Notice contains information about potential future MA rate increases and updates certain policies associated with risk adjustments. We continue to monitor MA notices, regulatory updates and guidance, as well as enforcement for impact on our business.
Medicaid revenue
Medicaid programs are state-administered programs partially funded by the federal government. These programs are intended to provide health coverage for patients whose income and assets fall below state-defined levels and who are otherwise uninsured. These programs also serve as supplemental insurance programs for co-insurance payments due from Medicaid-eligible patients with primary coverage under the Medicare program. Some Medicaid programs also pay for additional services, including some oral medications that are not covered by Medicare. We are enrolled in the Medicaid programs in the states in which we conduct our business.
Commercial revenue
BeforeAs discussed above, if a patient has commercial insurance, then that commercial insurance plan is generally responsible for payment of dialysis services for up to the first 33 months before that patient becomes eligible to elect to have Medicare as their primary payor for dialysis services, a patient’s commercial insurance plan, if any, is generally responsible for payment of such dialysis services for up to the first 33 months, as discussed above.services. Although commercial payment rates vary, average commercial payment rates established under commercial contracts are generally significantly higher than Medicare rates. The payments we receive from commercial payors generate nearly all of our profits and all of our non-hospital dialysis profits come from commercial payors. Payment methods from commercial payors can include a single lump-sum per treatment, referred to as bundled rates, or in other cases separate payments for dialysis treatments and pharmaceuticals, if used as part of the treatment, referred to as FFS rates. Commercial payment rates are the result of negotiations between us and insurerscommercial payors or third-partythird party administrators. Our commercial contracts sometimes contain annual price escalator provisions. We are comprehensively contracted, and the vast majority of patients insured through commercial health plans are covered by one of our commercial contracts, though we also receive payments from a limited set of commercial patients that are covered by a health plan that considers us out-of-network. While our out-of-network payment rates are on average higher than in-network commercial contract payment rates. Somerates, we have made efforts to be contracted with the majority of our commercial contracts pay us under a single bundled payment rate for all dialysis services provided to covered patients. However, some of our commercial contracts also pay us for certain other services and pharmaceuticals in addition to the bundled payment. Our commercial contracts typically contain annual price escalator provisions.payors offering health plans.
Approximately 25%27% of our U.S. dialysis patient servicesservice revenues and approximately 10%11% of our U.S. dialysis patients are associated with non-hospital commercial payors for the year ended December 31, 2020.2023. Non-hospital commercial patients as a percentage of our total U.S. dialysis patients for 2020 were relatively flat2023 increased slightly compared to 2019.2022. Less than 1% of our U.S. dialysis revenues are due directly from patients. There is noNo single commercial payor that accounted for more than 10% of total U.S. dialysis revenues for the year ended December 31, 2020.2023. See Note 2 to the consolidated financial statements included in this report for disclosure on our concentration related to our commercial payors on a total consolidated revenue basis.
Both the number of our patients under commercial plans and the rates under these commercial plans are subject to change based on a number of factors. These factors include, among others, a highly competitive rate environment that shapes our ongoing negotiations with commercial payors; changes in commercial plan design; and the health of the U.S. economy including the continuing impact of COVID-19 and efforts to contain the virus. In addition, changes in state and federal legislation, regulations, rules, laws, guidance or other requirements may impact the availability and scope of commercial insurance, including, among others, developments that impact the healthcare exchanges introduced by the Patient Protection and Affordable Care Act of 2010, as amended by the Health Care and Education Reconciliation Act of 2010 (Affordable Care Act (ACA)) and commercial payor participation in that marketplace as well as developments that impact the availability of charitable premium assistance. For additional detail on the potential impact of these factors onand other risks associated with our commercial revenue, see the risk factors in Item 1A1A. Risk Factors under the headings "Our business is subject to a complex seriesset of governmental laws, regulations and requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation"other requirements...;" "Changes in federal and state healthcare legislation or regulations could have a material adverse effect on our business, results of operations, financial condition and cash flows"regulations...;"We continuously have ongoing negotiations with commercial payors, and if the average rates that commercial payors pay us decline significantly, if patients in commercial plans are subject to restriction in plan designs or if we are unable to maintain contracts with payors with competitive terms, including, without limitation, reimbursement rates, scope and duration of coverage and in-network benefits, it would have a material adverse effect on our business, results of operations, financial condition and cash flows"; "If the number or percentage of patients with higher-paying commercial insurance declines, it could have a material adverse effect on our business, results of operations, financial conditiondeclines...;" and "Macroeconomic conditions and cash flows"; and "We face various risks related to the dynamic and evolving novel coronavirus pandemic, any of which may have a material adverse impact on us.global events..."
Revenue from other pharmaceuticals
Effective January 1, 2018, both oral and intravenous forms of calcimimetics became the financial responsibility of our U.S. dialysis business for our Medicare patients and are reimbursed under Medicare Part B. Since the effective date through December 31, 2020, the oral and intravenous forms of calcimimetics were separately reimbursed through a TDAPA and not as part of the ESRD PPS bundled payment. These separate reimbursement payments for calcimimetics were subject to change on an annual basis. During the initial pass-through TDAPA period, Medicare payments were based on a pass-through rate of the average sales price plus approximately 6% before sequestration (or 4% adjusted for sequestration), and in 2020 they were based on a pass-through rate of the average sales price plus 0%, before sequestration. As expected, as of January 1, 2021, calcimimetics was entered into the ESRD PPS bundled payment.
Physician relationships
Joint venture partners
We own and operate certain of our dialysis centers through entities that are structured as joint ventures. We generally hold controlling interests in these joint ventures, with certain nephrologists, hospitals, management services organizations, and/or other healthcare providers holding minority equity interests. These joint ventures are typically formed as limited liability companies. For the year ended December 31, 2020,2023, revenues from joint ventures in which we have a controlling interest represented approximately 27%29% of our net U.S. dialysis revenues. We expect to continue to enter into new U.S. dialysis-related joint ventures in the ordinary course of business.
Community physicians
An ESRDESKD patient generally seeks treatment or support for their home treatment at an outpatient dialysis center near their home where their treating nephrologist has practice privileges. Our relationships with local nephrologists and our ability to provide quality dialysis services and to meet the needs of their patients are key factors in the success of our dialysis operations. Over 5,4005,200 nephrologists currently refer patients to our outpatient dialysis centers.
Medical directors
Participation in the Medicare ESRD program requires that dialysis services at an outpatient dialysis center be under the general supervision of a medical director. Per these requirements, this individual is usually a board certified nephrologist. We have engagedengage physicians or groups of physicians to serve as medical directors for each of our outpatient dialysis centers. At some outpatient dialysis centers, we also separately contract with one or more other physicians or groups to serve as assistant or associate medical directors over other modalities such as home dialysis. We have over 1,000900 individual physicians and physician groups under contract to provide medical director services.
Medical directors for our dialysis centers enter into written contracts with us that specify their duties and fix their compensation generally for periods of ten years. The compensation of our medical directors is the result of arm’s length negotiations, consistent with fair market value, and generally depends upon an analysis of various factors such as the
physician’s duties, responsibilities, professional qualifications and experience, as well as the time and effort required to provide such services.
Our medical director contracts and joint venture operating agreements generally include covenants not to compete or own interests in other competing outpatient dialysis centers operated by other providers within a defined geographic area for various time periods, as applicable. These non-compete agreements do not restrict or limit the physicians from practicing medicine or prohibit the physicians from referring patients to any outpatient dialysis center, including competing centers.dialysis centers operated by other providers. In January 2023, the Federal Trade Commission (FTC) proposed a new rule that would generally prohibit employers from using non-compete clauses in contracts with workers that extend beyond the termination of the employment or independent contractor relationship. The comment period for the proposed rule has closed. It is unclear if and when a final rule will be issued and whether it would be subject to legal challenges. In addition, Congress and more than half of the states' legislatures, introduced legislation in 2023 that would place restrictions on non-compete agreements between employers and workers. While few of these states passed legislation, it is possible that similar legislation could be introduced in 2024. We are monitoring these developments and any state follow-on regulations for any potential impact on us, including on our agreements with teammates, our arrangements with medical directors, joint venture operating agreements, or the terms of any of our existing agreements with physicians should the new rules ultimately be finalized and implemented in this area.
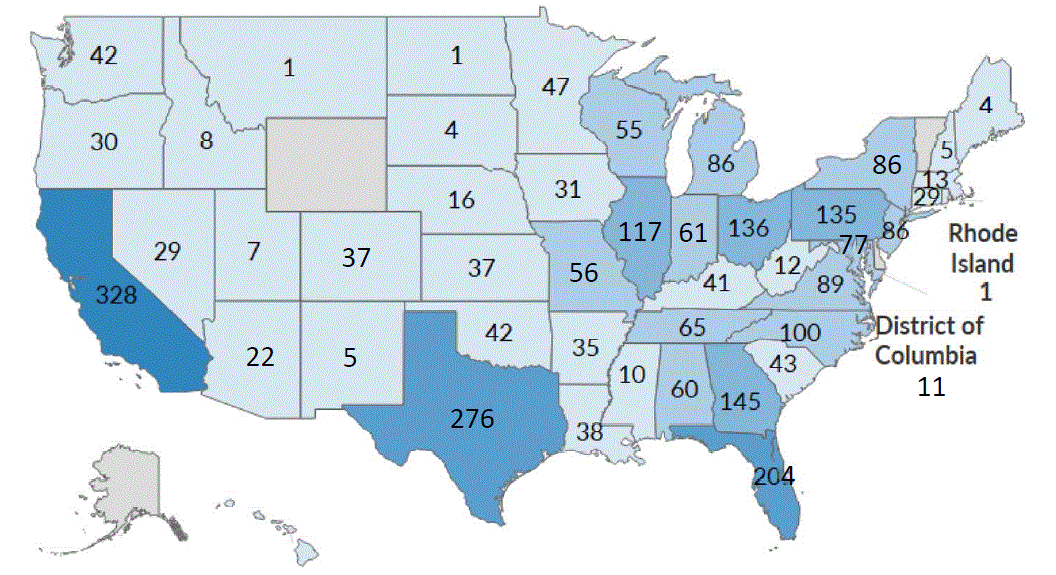
Location of our U.S. dialysis centers
AsWe operated 2,675 outpatient dialysis centers in the U.S. as of December 31, 2020, we operated or provided administrative services to a total2023 and 2,616 of 2,816 U.S. outpatient dialysis centers. A total of 2,763 of suchthese centers are consolidated in our financial statements. Of the remaining 53 non-consolidated59 nonconsolidated U.S. outpatient dialysis centers, we own a noncontrolling interestinterests in 5056 centers and provide management and administrative services to three centers that are wholly-owned by third parties. The locations of the 2,7632,616 U.S. outpatient dialysis centers consolidated in our financial statements at December 31, 2020,2023, were as follows:
Ancillary services, and strategic initiatives, including our international operations
Our ancillary services and strategic initiatives relate primarily to our core business of providing kidney care services and, asservices. As of December 31, 2020,2023, these consisted primarily of our U.S. integrated kidney care physician services, ESCO joint ventures (ESCO JVs), and(IKC) business, certain U.S. other ancillary businesses (including our clinical research programs, as well astransplant software business, and venture investment group), and our international operations.
Ancillary Services and Strategic Initiatives
We have made and continue to make investments in building our integrated care capabilities, including the operation of certain strategic business initiatives that are intended to integrate and coordinate care amongstamong healthcare participants across the renal care continuum from chronic kidney disease (CKD)CKD to ESRDESKD to kidney transplant. Through improved technology and data sharing, as well as an increasing focus on value-based contracting and care, these initiatives seek to bring together physicians, nurses, dieticians, pharmacists, hospitals, dialysis clinics, transplant centers, payors and payorsother specialists with a view towards improving clinical outcomes for our patients and reducing the overall cost of comprehensive kidney care. Certain of our ancillary services are described below.
U.S. Integrated Kidney Care
•Integrated Kidney Care services.Care. VillageHealth DM, LLC, also doing business as DaVita Integrated Kidney Care (DaVita IKC), provides advanced integrated care management services to health plans and government programs for members/beneficiaries diagnosed with ESRD, chronic kidney disease, and/or poly-comorbid conditions.ESKD and CKD. Through a combination of health monitoring, clinical coordination, innovative interventions, predictive analytics, medical claims analysis and information technology, we endeavor to assist our health plan and government program customers and patients in obtaining superior renal healthcare and improved clinical outcomes, as well as helping to reduce overall medical costs. Integrated kidney care management revenues from commercial and Medicare Advantage insurers can be based upon either an established contract fee recognized as earned for services provided over the contract period, or related to the operation of risk-based and value-based care programs, including pay for performance, shared savings, pay-for-performance, and capitation contracts. DaVita IKC also contracts with payors to operate Medicare Advantage ESRD Special Needs Planssupport MA ESKD chronic condition special needs plans (C-SNPs) to provide ESRDESKD patients full service healthcare. We are at risk for all medical costs of the program in excess of the capitation payments.healthcare and integrated care management services. DaVita IKC supportssupported our ESCOESKD seamless care organizations (ESCO) joint ventures,venture programs until their completion in 2021, and more recently has been provisionally accepted to participatecurrently participates in one ofboth the involuntary and certain voluntary payment models administered by CMMI. As further described below under the heading "—Government regulation—CMMI Payment Models", we have invested resources, and expect to continue to invest substantial resources in these models as part of our overall plan to grow our integrated kidney care business and value-based care initiatives. See Note 1, Other revenues, in the Company's consolidated financial statements for more information on how the Company accounts for its integrated care arrangements.
The Company is also developing, and has entered into, various forms of technology-based, administrative, financial and other collaboration and incentive arrangements with physician partners and other providers in support of our innovative care model, developing and expanding IKC programs and arrangements.
•Physician services. Nephrology Practice Solutions (NPS) is an independent business that partners with physicians committed to providing outstanding clinical and integrated care to patients. NPS provides nephrologist recruitment and staffing services in select markets whichthat are billed on a per searchper-search basis. NPS also offers physician practice management services to nephrologists under administrative and management services agreements. These administrative and management services include physician practice management, billing and collections, credentialing, coding and other support services that enable physician practices to increase efficiency and manage their administrative needs. Additionally, NPS owns and operates nephrology practices in multiple states. Fees generated from these services are recognized as earned typically based upon flat fees or cash collections generated by the physician practice.
•ESCO JVs. Certain of our dialysis clinics have entered into partnerships with various nephrology practices, health systems, and other providers to establish three ESCO JVs in Phoenix-Tucson Arizona, South Florida, and Philadelphia Pennsylvania-Camden, New Jersey. The ESCO JVs were formed under the CMS Innovation Center’s CEC Model, a demonstration to assess the impact of care coordination for ESRD patients in a dialysis-center oriented ACO setting. Each ESCO JV has a shared risk arrangement with CMS and the programs are evaluated on a performance year basis. The delivery of improved quality outcomes for patients and program savings depend on the contributions of the dialysis center teammates, nephrologists, health system and hospital partners, pharmacy providers, other primary care and specialty care providers and facilities, and integrated care management support from DaVita IKC, which is also the manager of the ESCO JVs. The CEC Model ended the South Florida ESCO JV program on December 31, 2020, while the Phoenix-Tucson Arizona and Philadelphia Pennsylvania-Camden, New Jersey programs are scheduled to end on March 31, 2021.U.S. Other Ancillary services
•Clinical research programs. DaVita Clinical Research (DCR) is a provider-based specialty clinical research organization with a fullwide spectrum of services for clinical drug research and device development. DCR uses its extensive applied database and real-world healthcare experienceexpertise to assist in the design, recruitment and completion of retrospective and prospective pragmatic and clinical trials.studies. Revenues are based upon an established fee per study generated fees, as determined by contract with drug companies and other sponsors, and are recognized as earned according to the contract terms.
•Transplant software business. DaVita's transplant software business, MedSleuth, works with transplant centers across the U.S. to provide greater connectivity among transplant candidates, transplant centers, physicians and care teams to help improve the experience and outcomes for kidney and liver transplant patients.
•Venture group. DaVita Venture Group (DVG) focuses on innovative products, solutions and businesses that improve care for patients with kidney disease and related conditions. DVG identifies companies and products for
acquisitions, strategic partnerships, and venture investment opportunities. DVG’s focus includes innovation in digital health, pharmaceuticals, medical devices, and care delivery models.
For additional discussion of our ancillary services, and strategic initiatives, see Part II Item 7, "Management’s Discussion and Analysis of Financial Condition and Results of OperationsOperations.".
International dialysis operations
As of December 31, 2020, weWe operated or provided administrative services to a total of 321367 outpatient dialysis centers which includes consolidated and nonconsolidated centers located in ten11 countries outside of the U.S., serving approximately 36,200 patients.49,400 patients as of December 31, 2023. Our international dialysis operations have continued to grow steadily and expand as a result of acquiring and developing outpatient dialysis centers in various strategic markets. Our international operations are included as part ofin our ancillary services and strategic initiatives.services.
The locationsAs of ourDecember 31, 2023, the international outpatient dialysis centers arewe operate were located as follows:
| | | | | |
| Brazil | 6999 | |
| Poland | 6863 | |
| Germany | 5951 | |
Malaysia(1) | 3940 | |
| Colombia | 2835 | |
| United Kingdom | 27 | |
| Saudi Arabia | 2326 | |
United Kingdom | 21 | |
| Portugal | 913 | |
Singapore(1) | 36 | |
Japan(1) | 5 | |
China(1) | 2 | |
| | 321367 | |
(1)Includes centers that are operated, managed or managedadministered by our Asia Pacific joint venture (APAC JV).
For additional discussion of our International business, see Part II Item 7, "Management’s Discussion and Analysis of Financial Condition and Results of Operations."
Corporate administrative support
Corporate administrative support consists primarily of labor, benefits and long-term incentive compensation costs and professional fees for departments which provide support to allmore than one of our different operating lines of business. These expenses are included in our consolidated general and administrative expenses.
Government regulation
We operate in a complex regulatory environment with an extensive and evolving set of federal, state and local governmental laws, regulations and other requirements. These laws, regulations and other requirements are promulgated and overseen by a number of different legislative, regulatory, administrative and quasi-regulatory bodies, each of which may have varying interpretations, judgments or related guidance. As such, we utilize considerable resources on an ongoing basis to monitor, assess and respond to applicable legislative, regulatory and administrative requirements, but there is no guarantee that we will be successful in our efforts to adhere to all of these requirements. Additional discussion on certain of these laws, regulations and other requirements is set forth below in this section.
The foregoing are each themselves comprised of numerous associated regulations or other requirements that have varying levels of impact on our business. If any of our personnel, representatives, third party vendors or operations are alleged to have violated these or other laws, regulations or requirements, we could experience material harm to our reputation and stock price, and it could impact our relationships and/or contracts related to our business, among other things. If any of our personnel, representatives, third party vendors or operations are found to violate these or other laws, regulations or other requirements, we could suffer additional severe consequences that wouldcould have a material adverse effect on our business, results of operations, financial condition and cash flows, andflows. The consequences could materially harm our reputation and stock price, including,include, among others:
•Loss of required certifications, suspension or exclusion from or termination of our participation in federal or state government programs (including, without limitation, Medicare, Medicaid and CMMI demonstration programs);
•Refunds of amounts received in violation of law or applicable payment program requirements dating back to the applicable statute of limitation periods;
•Loss of licenses required to operate healthcare facilities or administer pharmaceuticals in the states in which we operate;
•Reductions in payment rates or coverage for dialysis and ancillary services and pharmaceuticals;
•Criminal or civil liability, fines, damages or monetary penalties, which could be material and/or could materially harm our reputation or stock price;penalties;
•Imposition of corporate integrity agreements, corrective action plans or consent agreements;
•Enforcement actions, investigations, or audits by governmental agencies and/or state law claims for monetary damages by patients who believe their protected health information (PHI) has been used, disclosed or not properly safeguarded in violation of federal or state patient privacy laws, including, among others, the Health Insurance Portability and Accountability Act of 1996 (HIPAA) and the Privacy Act of 1974;
•Enforcement actions, investigations or audits by government agencies and/or initiated by qui tam relators related to interoperability and related data sharing and access requirements and regulations;
•Mandated changes to our practices or procedures that significantly increase operating expenses that could subject us to ongoing audits and reporting requirements as well as increased scrutiny of our billing and business practices, which could lead to potential fines, among other things;
•Termination of various relationships and/or contracts related to our business, such as joint venture arrangements, medical director agreements, hospital services and skilled nursing home agreements, real estate leases, value-based care arrangements, clinical incentive programs, payor contracts and consulting or participating provider agreements with physicians;physicians, among others; and
•Harm to our reputation which could negatively impact our business relationships and stock price, affect our ability to attract and retain patients, physicians and teammates, affect our ability to obtain financing and decreaseour access to new business opportunities, among other things.
We expect that our industry will continue to be subject to extensive and complex regulation, the scope and effect of which are difficult to predict. We are currently subject to various legal proceedings, such as lawsuits, investigations, audits and inquiries by various government and regulatory agencies, as further described in Note 1615 to the consolidated financial statements, and our operations and activities could be reviewed or challenged by regulatory authorities at any time in the future. In addition, each of the laws, regulations and other requirements, including interpretations thereof, that govern our business may continue to change over time, and there is no assurance that we will be able to accurately predict the nature, timing or extent of such changes or the impact of such changes on the markets in which we conduct business or on the other participants that operate in those markets. For additional detail on risks related to each of the foregoing, see the discussion in Item 1A. Risk Factors under the headings, "Our business is subject to a complex set of governmental laws, regulations and other requirements requirements...;" and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm stock price, and in some circumstances, could materially harm our reputation"; and "We are, and may in the future be, a party to various lawsuits, demands, claims, qui tam suits, governmental investigations and audits and other legal matters, any of which could result in, among other things, substantial financial penalties or awards against us, mandated refunds, substantial payments made by us, required changes to our business practices, exclusion from future participation in Medicare, Medicaid and other healthcare programs and possible criminal penalties, any of which could have a material adverse effect on our business, results of operations, financial condition, cash flows, reputation and stock price.matters..."
Licensure and Certification
Our dialysis centers are certified by CMS, as required for the receipt of Medicare payments. Certain of our payor contracts also condition payment on Medicare certification. In some states, our outpatient dialysis centers also are required to secure additional state licenses and permits. Governmental authorities, primarily state departments of health, periodically inspect our centers to determine if we satisfy applicable federal and state standards and requirements, including the conditions for coverage in the Medicare ESRD program.
We have experienced some delays in obtaining Medicare certifications from CMS, though recent changes by CMS in the prioritizing of dialysis providers as well as legislation allowing private entities to perform initial dialysis facility surveys for certification has helped to decrease or limit certain delays.
In addition, in NovemberSeptember 2019, CMS finalized updates to the Provider Enrollment Rule creating onerous disclosure obligations for all providers enrolledenrolling in Medicare, Medicaid and the Children’s Health Insurance Plan (CHIP). The final rule implements greaterprovides CMS with stronger revocation authority, and increases the bar for re-enrollment, and permits CMS to impose a Medicare reapplication bar where a prospective provider's Medicare enrollment application is denied because the provider submitted incomplete, false, or misleading information for providers who are terminated from the Medicare program. ItCMS may also institutes penalties fordeny enrollment to providers who submit incomplete or inaccurate information or who have affiliations with other providers that CMS has determined pose undue risk of fraud, waste or abuse. If we fail to comply with these and other applicable requirements on our licensure and certification programs,
particularly in light of increased penalties that include a 10-year bar to Medicare re-enrollment, under certain circumstances it could have a material adverse impact on our business, results of operations, financial condition, cash flows and reputation.
In addition to certification by CMS, our dialysis centers are also certified by each state Medicaid program, are licensed in those states that require licensing for dialysis clinics, and are required to obtain licenses, permits and certificates, including for such areas as biomedical waste. Failure to obtain the correct certifications, permits and certificates as well as a failure to adhere to the requirements thereunder, may result in penalties, fines, and the loss of the right to operate, any of which could have a material adverse impact on our business, results of operations, financial condition, cash flows and reputation.
Federal Anti-Kickback Statute
The federal Anti-Kickback Statute prohibits, among other things, knowingly and willfully offering, paying, soliciting or receiving remuneration, directly or indirectly, in cash or kind, to induce or reward either the referral of an individual for, or the purchase, or order or recommendation of, any good or service, for which payment may be made under federal and state healthcare programs such as Medicare and Medicaid.
Federal criminal penalties for the violation of the federal Anti-Kickback Statute include imprisonment, fines and exclusion of the provider from future participation in the federal healthcare programs, including Medicare and Medicaid. Violations of the federal Anti-Kickback Statute are punishable by imprisonment for up to ten years and statutory fines of up to $100,000 or both. Larger criminal fines can be imposed upon corporations under the provisions of the U.S. Sentencing Guidelines and the Alternate Fines Statute. Individuals and entities convicted of violating the federal Anti-Kickback Statute are subject to mandatory exclusion from participation in Medicare, Medicaid and other federal healthcare programs for a minimum of five years. Civil penalties for violation of this law include statutory amounts of up to $100,000 (adjusted for inflation) in monetary penalties per violation, repaymentsassessments of up to three times the total payments between the parties to the arrangement, and permissive exclusion from participation in the federal healthcare programs or suspension from future participation in Medicare and Medicaid. Court decisions have held thatThe Patient Protection and Affordable Care Act and the statute may be violated even if only one purposeHealth Care Reconciliation Act of remuneration is to induce referrals. The ACA2010, as amended (collectively, the ACA), amended the federal Anti-Kickback Statute to clarify the intent that is required to prove a violation. Under the statute as amended, the defendant may not need to have actual knowledge of the federal Anti-Kickback Statute or have the specific intent to violate it. In addition, the ACA amended the federal Anti-Kickback Statuteit and to provide that any claims for items or services resulting from a violation of the federal Anti-Kickback Statute are considered false or fraudulent for purposes of the False Claims Act (FCA). and can result in treble damages and other penalties under the FCA.
The federal Anti-Kickback Statute includes statutory exceptions and regulatory safe harbors that protect certain arrangements. Business transactions and arrangements that are structured to comply fully withwithin an applicable safe harbor do not violate the federal Anti-Kickback Statute. Transactions and arrangements that do not satisfy all elements of a relevant safe harbor do not necessarily violate the law. When an arrangement doesis not satisfystructured fully within a safe harbor, the arrangement must be evaluated on a case-by-case basis in light of the parties’ intent and the arrangement’s potential for abuse. Arrangements that do not satisfy a safe harborabuse, and may be subject to greater scrutiny by enforcement agencies.
On November 20, 2020, In addition, HHS' Office of Inspector General (OIG) and CMS in 2020 released a final rule implementing modifications to the Federal Anti-Kickback Statute and Civil Monetary Penalties Statute that are intended to promote value-based and coordinated care arrangements as well as reduce other regulatory burdens. The changes implemented by
In the final rules went into effect on January 19, 2021. We continue to assess the anticipated impactordinary course of these modifications on our business results of operations, and financial condition.
DaVita and its ancillary businesses and subsidiaries enter into severalnumerous arrangements with physicians and other potential referral sources, that potentially implicate the Anti-Kickback Statute,Statute. Examples of such as:
Medicalarrangements include, among other things, medical director agreements,. Because our medical directors may refer patients to our dialysis centers, our arrangements with these physicians are designed to substantially comply with the safe harbor for personal service arrangements. Although we endeavor to structure the Medical Director Agreements we enter into with physicians to substantially comply with the safe harbor for personal service arrangements, including the requirement that compensation be consistent with fair market value, the safe harbor requires that when services are provided on a part-time basis, the agreement must specify the schedule of intervals of services, and their precise length and the exact charge for such services. Because of the nature of our medical directors’ duties, it is impossible to fully satisfy this technical element of the safe harbor. As a result, these arrangements could be subject to scrutiny since they do not expressly describe the schedule of part-time services to be provided under the arrangement.
Joint ventures. As noted above, we own a controlling interest in numerous U.S. dialysis related joint ventures. Our internal policies, procedures, and template agreements were developed and are utilized for compliance with the Anti-Kickback Statute. However, we recognize that at times these joint ventures, do not fully satisfy all of the requirements of the safe harbor for investments in small entities. Although failure to complyleases and subleases with a safe harbor does not render an arrangement illegal under the federal Anti-Kickback Statute, an arrangement that does not operate within a safe harbor may be subject to scrutiny by both federal and state government enforcement agencies including the OIG and the Department of Justice (DOJ). Joint ventures that fall outside the safe harbors are evaluated on a case-by-case basis under the federal Anti-Kickback Statute.
Lease arrangements. We lease space from entities in which physicians, hospitals or medical groups hold ownership interests, and we sublease space to referring physicians. We endeavor to structure these arrangements to comply with the federal Anti-Kickback Statute safe harbor for space rentals in all material respects.
Consulting agreements. From time to time, we enter into consulting agreements, with physicians. Engaged physicians providehospital services including providing input on processes,agreements, discharge planning services and protocols as well as providing education on assorted topics. We endeavor to structure theseagreements, acute dialysis services agreements, value-based care arrangements, to comply with the federal Anti-Kickback Statute safe harbor for personal services in all material respects.
Employmentemployment and coverage agreements,. Our subsidiary Nephrology Practice Solutions and its affiliated entities employs and contracts with physicians and Advanced Practice Providers to provide administrative and clinical services. We endeavor to structure these arrangements to comply with the federal Anti-Kickback Statute safe harbor for employment and personal services in all material respects.
Common stock. Someincentive performance arrangements. In addition, some referring physicians may own ourDaVita Inc. common stock. We believe that these interests materially satisfy the requirements of the Anti-Kickback Statute safe harbor for investments in large publicly traded companies.
Discounts. OurFurthermore, our dialysis centers and subsidiaries sometimes enter into certain rebate, pricing, or other contracts to acquire certain discounted items and services at a discount that may be reimbursed by a federal healthcare program. We
Agreements and other arrangements can still be appropriate under the federal Anti-Kickback Statute even if they fail to meet all parameters of a relevant safe harbor provision; and we endeavor to structure our vendor contracts that include discount or rebate provisions to comply with the federal Anti-Kickback Statutearrangements within applicable safe harbor for discounts.harbors, although some arrangements are not structured fully within a safe harbor.
If any of our current or previous business transactions or arrangements, including but not limited to those described above, were found to violate the federal Anti-Kickback Statute, we, among other things, could face criminal, civil or administrative sanctions, including possible exclusion from participation in Medicare, Medicaid and other state and federal healthcare programs. Any findings that we have violated these laws could have a material adverse impact on our business, results of operations, financial condition, cash flows, reputation and stock price.
Stark Law
The Stark Law is a strict liability civil law that prohibits a physician who has a financial relationship, or who has an immediate family member who has a financial relationship, with entities providing Designated Health Services (DHS), from referring Medicare and Medicaid patients to such entities for the furnishing of DHS, unless an exception applies. DHS is defined to mean any of the following enumerated items or services; clinical laboratory services; physical therapy services; occupational therapy services; radiology services, including magnetic resonance imaging, computerized axial tomography scans, and ultrasound services; radiation therapy services and supplies; durable medical equipment and supplies; parenteral and enteral nutrients, equipment, and supplies; prosthetics, orthotics and prosthetic devices and supplies; home health services; outpatient prescription drugs; inpatient and outpatient hospital services; and outpatient speech-language pathology services. The types of financial arrangements between a physician and a DHS entity that trigger the self-referral prohibitions of the Stark Law are broad and include direct and indirect ownership and investment interests and compensation arrangements. The Stark Law also prohibits the DHS entity receiving a prohibited referral from presenting, or causing to be presented, a claim or billing for the services arising out of the prohibited referral. The prohibition applies regardless of the reasons for the financial relationship and the referral; unlike the federal Anti-Kickback Statute, intent to induce referrals is not required. If the Stark Law is implicated, the financial relationship must fully satisfy a Stark Law exception. If an exception to the Stark Law is not satisfied, then the parties to the arrangement could be subject to sanctions. Sanctions for violation of the Stark Law include denial of payment for claims for services provided in violation of the prohibition, refunds of amounts collected in violation of the prohibition, a civil penalty of up to $15,000 (adjusted for inflation) for each service arising out of the prohibited referral, a statutory civil penalty of up to $100,000 (adjusted for inflation) against parties that enter into a scheme to circumvent the Stark Law prohibition, civil assessment of up to three times the amount claimed, and potential exclusion from the federal healthcare programs, including Medicare and Medicaid. Amounts collected for prohibited claims must be reported and refunded generally within 60 days after the date on which the overpayment was identified. Furthermore, Stark Law violations and failure to return overpayments timely can form the basis for FCA liability as discussed below. In addition, CMS released a final rule implementing modifications to the Stark Law intended to promote value-based and coordinated care arrangements as well as reduce other regulatory burdens.
The definition of DHS under the Stark Law excludes services paid under a composite rate, even if some of the components bundled in the composite rate are DHS. Although the ESRD bundled payment system is no longer titled a composite rate, we believe that the former composite rate payment system and the current bundled system are both composite systems excluded from the Stark Law. Since most services furnished to Medicare beneficiaries provided in our dialysis centers are reimbursed through a bundled rate, we believe that the services performed in our facilities generally are not DHS, and the Stark Law referral prohibition does not apply to those services.DHS. Certain separately billable drugs (drugs furnished to an ESRD patient that are not for the treatment of ESRD that CMS allows our centers to bill for using the so-called AY modifier) may be considered DHS. However, we have implemented certain billing controls designed to limit DHS being billed out of our dialysis clinics. Likewise, the definition of inpatient hospital services, for purposes of the Stark Law, also excludes inpatient dialysis performed in hospitals that are not certified to provide ESRD services. Consequently, we believe that our arrangements with such hospitals for the provision of dialysis services to hospital inpatients doshould not trigger the Stark Law referral prohibition.
In addition, although prescription drugs are DHS, there is an exception in the Stark Law for calcimimetics, EPO and other specifically enumerated dialysis drugs when furnished in or by an ESRD facility such that the arrangement for the furnishing of the drugs does not violate the Stark Law.
WeIn the ordinary course of business operations, DaVita and its ancillary businesses and subsidiaries have entered into severalmany different types of financial relationshipsarrangements with referring physicians that potentially implicate the Stark Law, including, compensationbut not limited to, medical director agreements, joint ventures, leases and subleases with entities in which physicians, hospitals or medical groups hold ownership interest, consulting agreements, hospital services agreements, discharge planning services agreements, acute dialysis services agreements, value-based care arrangements, employment agreements and incentive performance arrangements. In addition, some referring physicians may own our common stock in reliance on the Stark Law exception for investment interests in large publicly traded companies.
If our dialysis centersinterpretation of the applicability of the Stark Law to our operations is incorrect, the controls we have implemented fail, an arrangement is entered into outside of our processes, or we were to bill for a non-exempted drug and the financial relationships with the referring physician did notfail to satisfy an applicable exception to the Stark Law, we could be found to be in violation of the Stark Law and required to change our practices, face civil penalties, pay substantial fines, return certain payments received from Medicare and beneficiaries or otherwise experience a material adverse effect as a result of a challenge to payments made pursuant to referrals from these physicians under the Stark Law. Additionally, certain of our subsidiaries, were they to bill DHS, would implicate the Stark Law. As such we endeavor to structure arrangements with relevant physicians to fit within the existing exceptions to the Stark Law. If we were to fail to satisfy an applicable exception,effect.
we could similarly be required to change practices, face penalties and fines, return certain payments or otherwise face adverse consequences.
On December 2, 2020, CMS released a final rule implementing modifications to the Stark Law. The purpose of these modifications is to promote value-based and coordinated care arrangements as well as reduce other regulatory burdens. The changes implemented by the final rules went into effect on January 19, 2021. We continue to assess the anticipated impact of these modifications on our business, results of operations and financial condition.
Medical director agreements. We endeavor to structure our medical director agreements to satisfy the personal services arrangement exception to the Stark Law. While we believe that the compensation provisions included in our medical director agreements are the result of arm’s length negotiations and result in fair market value payments for medical director services, an enforcement agency could nevertheless challenge the level of compensation that we pay our medical directors.
Lease agreements. We lease space from entities in which referring physicians hold interests and we sublease space to referring physicians at some of our dialysis centers. The Stark Law provides an exception for lease arrangements if specific requirements are met. We endeavor to structure our leases and subleases with referring physicians to satisfy the requirements for this exception.
Consulting agreements. From time to time, we enter into consulting agreements with physicians. Engaged physicians provide services including providing input on processes, services and protocols as well as providing education on assorted topics. We endeavor to structure these arrangements to comply with the Stark Law exception for personal services.
Employment agreements. We employ physicians to provide administrative and clinical services. We endeavor to structure these arrangements to comply with the relevant Stark Law exceptions.
Common stock. Some referring physicians may own our common stock. We believe that these interests satisfy the Stark Law exception for investments in large publicly traded companies.
Joint ventures. Some of our referring physicians also own equity interests in entities that operate our dialysis centers and subsidiaries. We believe that none of the Stark Law exceptions applicable to physician ownership interests in entities to which they make DHS referrals apply to the kinds of ownership arrangements that referring physicians hold in several of our subsidiaries that operate dialysis centers. Accordingly, these dialysis centers do not bill Medicare for DHS, if any, when provided based on the referral from any physician owners. If the dialysis centers bill for DHS referred by physician owners, the dialysis centers or subsidiaries could be subject to the Stark Law penalties described above unless a relevant exception to the Stark Law applies.
Ancillary services. The operations of our ancillary and subsidiary businesses are also subject to compliance with the Stark Law, and any failure to comply with these requirements, particularly in light of the strict liability nature of the Stark Law, could subject these operations to the Stark Law penalties and sanctions described above.
If CMS or other regulatory or enforcement authorities determined that we have submitted claims in violation of the Stark Law, or otherwise violated the Stark Law, we would be subject to the penalties described above. In addition, it might be necessary to restructure existing compensation agreements with our medical directors and to repurchase or to request the sale of ownership interests in subsidiaries and partnerships held by referring physicians or, alternatively, to refuse to accept referrals for DHS from these physicians, or take other actions to modify our operations. Any suchfinding by CMS or other regulatory or enforcement authorities that we have violated the Stark Law or related penalties and restructuring or other required actions could have a material adverse effect on our business, results of operations, financial condition, cash flows, stock price and reputation.
False Claims Act
The federal FCA is a means of policing false claims, false bills or false requests for payment in the healthcare delivery system. In part, the FCA authorizes the imposition of up to three times the government’s damages and civil penalties, plus up to approximately $28,000 per claim, on any person who, among other acts:
•Knowingly presents or causes to be presented to the federal government, a false or fraudulent claim for payment or approval;
•Knowingly makes, uses or causes to be made or used, a false record or statement material to a false or fraudulent claim;
•Knowingly makes, uses, or causes to be made or used, a false record or statement material to an obligation to pay the government, or knowingly conceals or knowingly and improperly, avoids or decreases an obligation to pay or transmit money or property to the federal government; or
•Conspires to commit the above acts.
In addition, the FCA imposes severe penalties for the knowing and improper retention of overpayments collected from government payors. Under these provisions, within 60 days of identifying and quantifying an overpayment, a provider is required to follow certain notification and repayment processes. An overpayment impermissibly retained could subject us to liability under the FCA, exclusion from government healthcare programs, and penalties under the federal Civil Monetary Penalty statute. As a result of these provisions, our procedures for identifying and processing overpayments may be subject to greater scrutiny.
The federal government has used the FCA to prosecute a wide variety of alleged false claims and fraud allegedly perpetrated against Medicare and state healthcare programs, including coding errors, billing for services not rendered, the submission of false cost reports, billing for services at a higher payment rate than appropriate, billing under a comprehensive code as well as under one or more component codes included in the comprehensive code and billing for care that is not considered medically necessary. The ACA provides that claims tainted by a violation of the federal Anti-Kickback Statute are false for purposes of the FCA. Some courts have held that filing claims or failing to refund amounts collected in violation of the Stark Law can form the basis for liability under the FCA. In addition to the provisions of the FCA, which provide for civil enforcement, the federal government can use several criminal statutes to prosecute persons who are alleged to have submitted false or fraudulent claims for payment to the federal government.
Fraud and abuse under state law
SomeState fraud and abuse laws related to anti-kickback, physician self-referral, beneficiary inducement and false claims often mirror those requirements of the applicable federal laws, or, in some instances contain additional or different requirements. If we were found to violate these state laws and regulations, we, among other things, could face criminal, civil or administrative sanctions, including loss of licensure or possible exclusion from Medicaid and other state and federal healthcare programs. Any findings that we have violated these laws and regulations could have a material adverse impact on our business, operations, financial condition, cash flows, reputation and stock price.
In addition to these fraud waste and abuse laws, some states in which we operate dialysis centers have laws prohibiting physicians from holding financial interests in various types of medical facilities to which they refer patients. Some of these laws could potentially be interpreted broadly as prohibiting physicians who hold shares of our publicly traded stock or are physician owners from referring patients to our dialysis centers if the centers use our laboratory subsidiary to perform laboratory services for their patients or do not otherwise satisfy an exception to the law. States also have laws similar to or stricter than the federal Anti-Kickback Statute that may affect our ability to receive referrals from physicians with whom we have financial relationships, such as our medical directors. Some state anti-kickback laws also include civil and criminal penalties. Some of these laws include exemptions that may be applicable to our medical directors and other physician relationships or for financial interests limited to shares of publicly traded stock. Some, however, may include no explicit exemption for certain types of agreements and/or relationships entered into with physicians. If these laws are interpreted to apply to referring physicians with whom we contract for items or services, including medical director and similar services,directors, or to referring physicians with whom we hold joint ownership interests or to referring physicians who hold interests in
DaVita Inc. limited solely to our publicly traded stock, and for which no applicable exception exists, we may be required to terminate or restructure our relationships with or refuse referrals from these referring physicians and could be subject to criminal, civil and administrative sanctions, refund requirements and exclusions from participation in government healthcare programs, including Medicare and Medicaid, which could have a material adverse effect on our business, results of operations, financial condition, cash flows, reputation and stock price.
Corporate Practice of Medicine and Fee-Splitting
There are states in which we operate that have laws that prohibit business entities not owned by health care providers, such as our Company and our subsidiaries, from practicing medicine, employing physicians to practice medicineand other licensed health care providers providing certain clinical services or exercising control over medical or clinical decisions by physicians and potentially other types of licensed health care providers (known collectively as the corporate practice of medicine). These states may also prohibit entities from engaging in certain financial arrangements, such as fee-splitting, with physicians. In some states these prohibitions are expressly stated in a statute or regulation, while inphysicians and potentially other states the prohibition is a mattertypes of judicial or regulatory interpretation.licensed health care providers. Violations of the corporate practice of medicine, fee-splitting and related laws vary by state and may result in physicians and potentially other types of licensed health care providers being subject to disciplinary action, as well as to forfeiture of revenues from payors for services rendered. For lay entities, violationsViolations may also bring both civil and, in more extreme cases, criminal liability for engaging in medical practice without a license.license and violating the corporate practice of medicine, fee-splitting and related laws. Some of the relevant laws, regulations, and agency interpretations in states with corporate practice of medicine restrictions have been subject to limited judicial and regulatory interpretation. Moreover, state laws are subject to change.
False Claims Act
The federal FCA is a means of policing false bills or false requests for payment in the healthcare delivery system. In part, the FCA authorizes the imposition of up to three times the government’s damages and civil penalties on any person who, among other acts:
•Knowingly presents or causes to be presented to the federal government, a false or fraudulent claim for payment or approval;
•Knowingly makes, uses or causes to be made or used, a false record or statement material to a false or fraudulent claim;
•Knowingly makes, uses, or causes to be made or used, a false record or statement material to an obligation to pay the government, or knowingly conceals or knowingly and improperly, avoids or decreases an obligation to pay or transmit money or property to the federal government; or
•Conspires to commit the above acts.
In addition, amendments to the FCA impose severe penalties for the knowing and improper retention of overpayments collected from government payors. Under these provisions, within 60 days of identifying and quantifying an overpayment, a provider is required to follow certain notification and repayment processes. An overpayment impermissibly retained could subject us to liability under the FCA, exclusion from government healthcare programs, and penalties under the federal Civil Monetary Penalty statute. As a result of these provisions, our procedures for identifying and processing overpayments may be subject to greater scrutiny.
On June 19, 2020, the DOJ issued a final rule announcing penalties for a violation of the FCA ranging from $11,665 to $23,331 for each false claim, plus up to three times the amount of damages caused by each false claim, which can be as much as the amounts received directly or indirectly from the government for each such false claim. The federal government has used the FCA to prosecute a wide variety of alleged false claims and fraud allegedly perpetrated against Medicare and state healthcare programs, including coding errors, billing for services not rendered, the submission of false cost reports, billing for services at a higher payment rate than appropriate, billing under a comprehensive code as well as under one or more component codes included in the comprehensive code and billing for care that is not considered medically necessary. The ACA provides that claims tainted by a violation of the federal Anti-Kickback Statute are false for purposes of the FCA. Some courts have held that filing claims or failing to refund amounts collected in violation of the Stark Law can form the basis for liability under the FCA. In addition to the provisions of the FCA, which provide for civil enforcement, the federal government can use several criminal statutes to prosecute persons who are alleged to have submitted false or fraudulent claims for payment to the federal government.
Civil Monetary Penalties Statute
The Civil Monetary Penalties Statute, 42 U.S.C. § 1320a-7a, authorizes the imposition of civil money penalties, assessments, and exclusion against an individual or entity based on a variety of prohibited conduct, including, but not limited to:
•Presenting, or causing to be presented, claims for payment to Medicare, Medicaid, or other third-party payors that the individual or entity knows or should know are for an item or service that was not provided as claimed or is false or fraudulent;
•Offering remuneration to a Federalfederal healthcare program beneficiary that the individual or entity knows or should know is likely to influence the beneficiary to order or receive healthcare items or services formfrom a particular provider;
•Arranging contracts with an entity or individual excluded from participation in the Federalfederal healthcare programs;
•Violating the federal Anti-Kickback Statute;
•Making, using, or causing to be made or used, a false record or statement material to a false or fraudulent claim for payment for items and services furnished under a Federalfederal healthcare program;
•Making, using, or causing to be made any false statement, omission, or misrepresentation of a material fact in any application, bid, or contract to participate or enroll as a provider of services or a supplier under a Federalfederal healthcare program; and
•Failing to report and return an overpayment owed to the federal government.
Substantial civil monetary penalties may be imposed under the federal Civil Monetary Penalty Statute and vary, depending on the underlying violation. In addition, an assessment of not more than three times the total amount claimed for each item or service may also apply, and a violator may be subject to exclusion from Federalparticipation in federal and state healthcare programs.
Foreign Corrupt Practices Act
We are subject to the provisions of the Foreign Corrupt Practices Act (FCPA) in the United States and similar laws in other countries, which generally prohibit companies and those acting on their behalf from making improper payments to foreign government officials and others for the purpose of obtaining or retaining business. A violation of the FCPA or other similar laws by us and/or our agents or representatives could result in, among other things, the imposition of fines and penalties, changes to our business practices, the termination of or other adverse impacts under our debt arrangements and contracts or debarment from bidding on contracts, and/or harm to our reputation, any of which could have a material adverse effect on our business, results of operations, financial condition, cash flows and cash flows.stock price.
Privacy and Security
The Health Insurance Portability and Accountability Act of 1996 and its implementing privacy and security regulations, as amended by the federal Health Information Technology for Economic and Clinical Health Act (HITECH Act), (collectively referred to as HIPAA), require us to provide certain protections to patients and their health information. The HIPAA privacy and security regulations extensively regulate the use and disclosure of PHI and require covered entities, which include healthcare providers, to implement and maintain administrative, physical and technical safeguards to protect the security of
such information. Additional security requirements apply to electronic PHI. These regulations also provide patients with substantive rights with respect to their health information.
The HIPAA privacy and security regulations also require us to enter into written agreements with certain contractors, known as business associates, to whom we disclose PHI. Covered entities may be subject to penalties for, among other activities, failing to enter into a business associate agreement where required by law or as a result of a business associate violating HIPAA if the business associate is found to be an agent of the covered entity and acting within the scope of the agency. Business associates are also directly subject to liability under the HIPAA privacy and security regulations. In instances where we act as a business associate to a covered entity, there is the potential for additional liability beyond our status as a covered entity.
Covered entities must report breaches of unsecured PHI to affected individuals without unreasonable delay but not to exceed 60 days of discovery of the breach by a covered entity or its agents. Notification must also be made to the HHS and, for breaches of unsecured PHI involving more than 500 residents of a state or jurisdiction, to the media. All non-permitted uses or disclosures of unsecured PHI are presumed to be breaches unless the covered entity or business associate establishes that there is a low probability the information has been compromised. Various state laws and regulations may also require us to notify affected individuals, and U.S. state attorneys general, or other regulators or law enforcement, in the event of a data breach involving individually identifiable information without regard to whether there is a low probability of the information being compromised.
Penalties for impermissible use or disclosure of PHI were increased by the HITECH Act by imposing tiered penalties of more than $50,000 per violation and up to $1.5 million per year for identical violations. In addition, HIPAA provides for criminal penalties of up to $250,000 and ten years in prison, with the severest penalties for obtaining and disclosing PHI with
the intent to sell, transfer or use such information for commercial advantage, personal gain or malicious harm. Further, state attorneys general may bring civil actions seeking either injunction or damages in response to violations of the HIPAA privacy and security regulations that threaten the privacy of state residents.
In addition to the protection of PHI, healthcare companies must meet privacy and security requirements applicable to other categories of personal information. Companies may process consumer information in conjunction with website and corporate operations. They may also handle employee information, including Social Security Numbers, payroll information, and other categories of sensitive information, to further their employment practices. In processing this additional information, companies must comply with the applicable privacy and security requirements of comprehensive privacy and data protection laws, consumer protection laws, labor and employment laws, and its publicly-available notices.
DataOutside of the United States, data protection laws and regulations are evolving globally, and may add additionalin different stages of maturity. For example, Europe is subject to the mature General Data Protection Regulation (GDPR) in contrast to Saudi Arabia's Personal Data Protection Law (PDPL) which is nascent. This presents compliance costs and legal risks to our international operations. In Europe,The countries within the General Data Protection Regulation (GDPR) became effective on May 25, 2018. TheDaVita International group can be broadly divided into GDPR applies to entities that are established incountries (Germany, Poland, Portugal, and the European Union (EU), as well as extendsUnited Kingdom) and non-GDPR countries (Brazil, China, Colombia, Japan, Malaysia, Saudi Arabia, and Singapore). When providing services or using personal data, we must ensure compliance with the scope of EU data protection laws to foreign companies processing data of individuals in the EU. applicable legislation.
The GDPR imposes a comprehensive data protection regime with the potential for regulatory fines as well as data breach litigation by impacted data subjects. Under the GDPR, regulatory penalties may be passed by data protection authorities for up to the greater of 4% of worldwide turnover or €20 million. The United Kingdom has implemented similar legislation (UK GDPR) that carries similar compliance and operational costs, and carries similar fines of complianceup to the greater of £17.5 million or 4% of global turnover. In non-GDPR countries, the cost of non-compliance varies but can also be just as significant as those under the GDPR. For example, the maximum fine for non-compliance with anddata protection laws in Brazil is 50 million Brazilian real (approximately $11 million) or 2% of the company’s turnover, while the maximum fine in China is RMB 50 million (approximately $7 million) or 5% of the previous year's annual revenue. In addition to fines, data protection authorities in non-GDPR countries may also impose criminal sanctions as well as other burdens imposed by, the GDPR and other new laws, regulations and policies implementing the GDPR may impact our European operations and/or limit the ways in which we can provide services or usepenalties, such as orders to cease processing personal data, collected while providing services. In July 2020, the Court of Justice of the European Union issued an opinion in the Schrems II case that invalidated the E.U.-U.S. Privacy Shield as a basis for transferring EUorders to delete personal data, to the U.S. The Court upheld European Commission-approved Standard Contractual Clauses (SCCs) as a basis for transfers of EU personalor warnings and reprimands.
Privacy and data to the United States, but imposed additional compliance burdens on companies to ensure their ability to comply with such contractual obligations. In October 2020, the U.S. government has issued guidance to companies on how to assess their ability to comply with transfer obligations, and in November 2020, the European Data Protection Board (EDPB), tasked with overseeing compliance with the GDPR, published, further to its initial guidance, its recommendations on measures to supplement data transfer rules to ensure compliance with EEA data protection law. In addition, the European Commission has also published a draft implementing a decision on new SCCs for the transfer of personal data to third countries which may be a significant task to put into place given its requirements. These developments add a layer of complexity to compliance efforts around international data transfers and compliance with the GDPR. If we fail to comply with the requirements of GDPR, we could be subject to penalties that would have a material adverse impact on our business, results of operations, financial condition and cash flows.
Data protection laws are also evolving nationally, providing for enhanced state privacy rights that are broader than the current federal privacy rights, and may add additional compliance costs and legal risks to our U.S. operations. For example, the California Consumer ProtectionPrivacy Act of 2018 (CCPA) became effective January 1, 2020 and enforceable, which was significantly amended by the California Attorney General on July 1, 2020. The CCPA is aPrivacy Rights Act (CPRA), the Colorado Privacy Act, as well as multiple other states, afford consumers expanded privacy law that requires certain companies doing business in California to enhance privacy disclosures regarding the collection, use and sharing of a consumer's personal data. The CCPA grants consumers additional privacy rights that are broader than current Federal privacy rights. The CCPA also permits the imposition ofprotections. These provide for civil penalties grants enforcement authority tofor violations, and the state Attorney GeneralCCPA and providesCPRA provide for a private right of action for consumers wheredata breaches. Additionally, several privacy bills have been proposed both at the federal and state level that may result in additional legal requirements that impact our business. On a related front, states continue to enact laws focusing on consumer health data that are similar to other comprehensive data laws, but impose more stringent consent requirements (e.g., opt-in consent for certain personal information is breached due to unreasonable information security practices. Since its passage, several other states, including Nevada
types of processing) for consumer health data. These laws carry statutory damages and Maine, have expanded theirin some cases allow for a private right of action. These state data protection laws (both the comprehensive laws and other states are considering similar legislation. These laws impose organizational requirements and grant individual rights that are comparable to those established in the CCPA. Additionally, in November 2020, California voters passed the California Privacy Rights Act (CPRA). The CPRA, which is expected to take effect on January 2023, significantly expands the data protection obligations imposed by the CCPA on companies doing business in California, including additional consumer rights processes, limitations on data uses, and opt outs for certain uses of sensitive data. It also will create a new California data protection agency to enforce the law, and require certain businesses with higher risk privacy and security practices to submit annual audits to the agency on a regular basis. The CPRAhealth-focused laws) will likely result in broader increased regulatory scrutiny in Californiaapplicable states of businesses’businesses' privacy and security practices, could lead to a further rise in data protection litigation, and will require additional compliance investment and potential business process changes in the meantime.changes.
In addition to the breach reporting requirements under HIPAA, companies are subject to state breach notification laws. Each state enforces a law requiring companies to provide notice of a breach of certain categories of sensitive personal information, e.g. Social Security Number, financial account information, or username and password. A company impacted by a breach must notify affected individuals, attorney’s general or other agencies within a certain time frame. If a company does not provide timely notice with the required content, it may be subject to civil penalties brought by attorney’s generalsattorneys general or affected individuals.
Companies must also safeguard personal information in accordance with federal and state data security laws and requirements. These requirements are akin to the HIPAA requirements to safeguard PHI, described above. The Federal Trade Commission,FTC, for example, requires companies to implement reasonable data security measures relative to its operations and the
volume and complexity of the information it processes. Also, various state data security laws require companies to safeguard data with technical security controls and underlying policies and processes. Due to the constant changes in the data security space, companies must continuously review and update data security practices to seek to mitigate any potential operational or legal liabilities stemming from data security risks. For additional details on the risks of compliance with applicable privacy and security laws, regulations and standards, see the discussion in Item 1A. Risk Factors under the heading "Privacy and information security laws are complex..." For additional information about our assessment of our cybersecurity risks, see the discussion in Item 1C. Cybersecurity.
Integrated Kidney Care, Medicare and Medicaid program reforms and Other Healthcare reformRegulations
In March 2010, broad healthcare reform legislation was enacted in the U.S. through the ACA, but the ACA’sThe regulatory framework and otherof the healthcare reforms continuemarketplace continues to evolve as a result of executive, legislative, regulatory and administrative developments and judicial proceedings. There have been multiple attempts to repeal or amendThese changes shape the ACA through legislative action and legal challenges, and the most recent challenge is currently before the U.S. Supreme Court. A repeal or other significant change to the ACA could have a material impact onlandscape for our current dialysis business if, for example, programs under the ACA were cancelled, including, among others, Medicaid expansion, CMMI models or the health insurance exchanges. Our revenue and operating income levels are highly sensitive to the percentage of our patients with higher-paying commercial health insurance and any legislative, regulatory or other changes that decrease the accessibility and availability, including the duration, of commercial insurance may have a material adverse impact on our business. In the event the health insurance exchange markets are significantly impaired as a result of legislative developments or other changes, it may adversely impact the percentage of our patients with higher-paying commercial health insurance, particularly if patients become unemployed due to factors related to the COVID-19 pandemic or otherwise and are unable to turn to the exchanges as an alternative to employer-based coverage.
Any changes in legislation, regulation or market conditions in connection with or resulting from the recent elections, could also impact our business in a number of ways, some of which may be material. For example, proposed legislative developments or administrative decisions, such as the creation of a public health insurance option similar to Medicare, government programs that impact access to Medicaid expansion or funding to families to purchase plans through health insurance exchanges or changes to the eligibility age for Medicare beneficiaries, eliminating the eligibility cap for the advance premium tax credit (APTC) and enhancing activities aimed at enrolling eligible individuals in Medicaid could impact the percentage of our patients with higher-paying commercial health insurance, impact the scope of coverage under commercial health plans and increase our expenses, among other things. Particularly in light of the ongoing COVID-19 pandemic, considerable uncertainty exists surrounding the continued development of the ACA and related regulations, programs and models, as well as similar healthcare reform measures and/or other potentialfor emerging comprehensive and integrated kidney care programs. The following discussion describes certain of these changes at the federal and/or state level to laws, regulations and other requirements that govern our business.in further detail.
New models of care and Medicare and Medicaid program reforms
CMMI Payment Models:As noteddescribed above, the 2019 Executive Order directed CMS to createhas launched payment models through CMMI to evaluate the effects of creating payment incentives for the greater use of homehome-based dialysis and kidney transplants for those already on dialysis. CMS, through CMMI, publisheddialysis, improve quality of care for kidney patients and reduce expenditures. The first of these, the final ETC mandatory payment model, on September 18, 2020. The ETC will be administered through CMMI and launched in approximately 30% of dialysis clinics across the country on January 1, 2021.
In addition, CMS subsequently issued several clarifying rules through November 2022 and continues to evaluate the model. CMS also announced the implementation of fourtwo voluntary kidney care payment models, Kidney Care First (KCF) and Comprehensive Kidney Care Contracting (CKCC), with the stated goal of helping healthcare providers reduce the cost and improve the quality of care for patients with late-stage chronic kidney disease and ESRD. CMS has stated these payment models are aimed to prevent or delay the need for dialysis and encourage kidney transplantation. These payment models have a scheduled commencement date of April 2021, though applicants now have the option to delay implementation until January 2022. Though we have applied for, and been provisionally accepted to participate in certainCertain of these voluntary models, we continue to assess these models and their viability for us and the industry. These voluntary models continue CMMI’s prior work with various healthcare providers to develop, refine and implement ACOs and other innovative models of care for Medicare and Medicaid beneficiaries, including, without limitation, the CEC Model (which includes the development of ESRD Seamless Care Organizations), the Duals Demonstration, and other models. We participated in the CEC Model with CMMI, including with organizations in Arizona, Florida, and adjacent markets in New Jersey and Pennsylvania. The CEC ESCOs Model overall ended in Florida in December 2020, while the Arizona and adjacent markets in New Jersey and Pennsylvania are scheduled to end in March 2021. We may choose to participate in additional models either as a partner with other providers or independently. Even in areas where we are not directly participating in these or other CMMI models, some of our patients may be assigned to an ACO, another ESRD Care Model, or another program, in which case the quality and cost of care that we furnish will be included in an ACO's, another ESRD Care Model's, or other program's calculations.
In addition, as to the aforementioned new models of care, federal bipartisan legislation related to full capitation demonstration for ESRD was introduced in Congress in September 2020 as the BETTER Kidney Care Act. This proposed legislation, which has not secured introduction in the current Congress, would build on prior coordinated carepayment models, such as the CEC Model, and would establish a demonstration programFirst Performance Period for the provisionKidney Care Choices Model CKCC Options (the CKCC Model) commenced on January 1, 2022. As described above, we have invested substantial resources, and expect to continue to invest substantial resources in these models as part of our overall plan to grow our integrated kidney care business and value-based care initiatives.
For additional details on the risks related to integrated kidney care and Medicare fee-for-serviceand Medicaid program reforms, see the discussion in Item 1A. Risk Factors under the headings "If we are not able to successfully implement our strategy with respect to our integrated kidney care and value-based care initiatives...;" and "If we are unable to compete successfully..."
Healthcare Reform, ACA and Related Regulations: The ACA regulatory framework of the healthcare marketplace continues to evolve as a result of executive, legislative, regulatory and administrative developments and judicial proceedings. For example, the expanded access to healthcare developed under the ACA has been both positively and negatively impacted over time by subsequent legal, regulatory and judicial action. In 2021 and 2022, respectively, the American Rescue Plan and Inflation Reduction Act of 2022 included several provisions designed to expand health coverage, including the expansion and extension of premium tax credits that assist consumers who purchase health insurance on marketplaces developed under the ACA and temporarily offering incentives to expand Medicaid coverage for states that have not yet done so. Our revenue and operating income levels are highly sensitive to the percentage of our patients with higher-paying commercial health insurance and any legislative, regulatory or other changes that decrease the accessibility and availability, including the duration, of commercial insurance is likely to have a material adverse impact on our business.
Changes to the political environment may increase the likelihood of legislative or regulatory changes that would impact us, such as changes to the healthcare regulatory landscape. Examples of such potential changes also could include, among other things, legislative, regulatory, or executive developments or changes to the eligibility age for Medicare beneficiaries. Some of
dialysisthese or other changes could in turn impact the percentage of our patients with higher-paying commercial health insurance, impact the scope or terms of coverage under commercial health plans and/or increase our expenses, among other things. The timing of legislative, regulatory or executive action related to these potential initiatives, if any, remains uncertain, particularly in light of the current economic and transplant patients. We have madepolitical environment, and continueas such, considerable uncertainty exists surrounding the continued development of the ACA and related regulations, programs and models, as well as similar healthcare reform measures and/or other potential changes at the federal and/or state level to make investments in buildinglaws, regulations and other requirements that govern our integrated care capabilities, but there can be no assurances that initiatives such as this or similar legislation will be introduced or passed into law, and the ongoing COVID-19 pandemic may delay the progress of any such initiatives. If such legislation is passed, there can be no assurances that we will be able to successfully execute on the required strategic initiatives that would allow us to provide a competitive and successful integrated care program on the broader scale contemplated by legislation like this, and in the desired time frame. Additionally, the ultimate terms and conditions of any such potential legislation remain unclear. For example, our costs of care could exceed our associated reimbursement rates under such legislation. For additional detail on the evolving health care landscape and associated developments in our competitive environment, see the risk factor in Item 1A Risk Factorsbusiness.
21st Century Cures Act:As described above under the heading "—"If we are unable to compete successfully, including, without limitation, implementing our growth strategy and/or retaining patients and physicians willing to serve as medical directors, it could materially adversely affect our business, results of operations, financial condition and cash flows.Medicare Advantage revenue,"
CMS has also issued final rules related to the Cures Act. The Cures Act included a provision that, effective January 1, 2021, allows Medicare eligible beneficiaries with ESRD to choose coverage under a Medicare Part C MA managed care plan. This provision could broadenbroadened patient access to certain enhanced benefits offered by MA plans. MA plans usually provide reimbursement to us at a negotiated rate that is generally higher than Medicare FFS rates. We continue to evaluate the potential impact of thisThis change in benefit eligibility has increased the percentage of our patients on MA plans as there remains significant uncertainty ascompared to Medicare Part B plans, though it is unclear how many or which newly eligible ESRD patients will continue to seek to enroll in MA plans for their ESRD benefits over time. In addition, the Cures Act also includes provisions related to data interoperability, information blocking and how quickly any such changes would occur. This uncertainty may be heightened by components of the aforementioned final rules, which include a provision that, among other things, removes the objective time and distance standards relating to network adequacy for outpatient dialysis centers for MA plans. The removal of these standards could result in MA plans seeking to limit provider networks available to dialysis patients. If MA plans attempt to use this revision to the rules to limit or restrict their networks, this may adversely impact the number of ESRD patients that select MA plans and also may result in the Company not being an in-network provider for significant MA plans.patient access. For details on the risks associated with these changes,provisions of the Cures Act, see the risk factors in Item 1A1A. Risk Factors under the headings, "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements,requirements...;" "If the number or any changes in those requirements, could have a material adverse effect on our business, resultspercentage of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation;patients with higher-paying commercial insurance declines...;" and "We continuously have ongoing negotiations with commercial payors, and if the average rates that commercial payors pay us decline significantly, if patients in commercial plans are subject"Failing to restriction in plan designseffectively maintain, operate or ifupgrade our information systems or those of third-party service providers upon which we are unable to maintain contracts with payors with competitive terms, including, without limitation, reimbursement rates, scope and duration of coverage and in-network benefits, it would have a material adverse effect on our business, results of operations, financial condition and cash flows".rely..."
The Cures Act also includes provisions related to data interoperability, information blocking, and patient access. CMS and the Office of the National Coordinator for Health Information Technology (ONC) recently issued final rules related to these provisions, which include, among other things, requirements surrounding information blocking, changes to ONC's Health IT Certification Program and requirements that CMS-regulated payors make relevant claims/care data and provider directory information available through standardized patient access and provider directory application programming interfaces (APIs) that connect to provider electronic health records. We have made and continue to make investments in building data interoperability capabilities, including as part of building on our integrated care capabilities as noted above, and continue to evaluate the potential impact of the CMS and ONC final rules.
Plan Price Transparency Rules: In addition, recent price and patient responsibility transparency regulations require most group health plans, and health insurance issuers in the group and individual markets, to make certain pricing and patient responsibility information publicly available. CertainOn July 1, 2022, most group health plans and issuers of group or individual health insurance were required to begin publishing machine-readable files that include negotiated rates for all covered items and services with all providers and out-of-network allowed amounts. For plan years that begin on or after January 1, 2023, most group health plans, and health insurance issuers in the group and individual markets, must provide enrollees with out-of-pocket cost and underlying provider negotiated rate information in a consumer-friendly format for an initial list of 500 designated services (which do not include dialysis). A plan or issuer may choose to include more than these 500 services, and for plan years that begin on or after January 1, 2024, most group health plans, and health insurance issuers in the group and individual markets, must provide enrollees with this information for all covered items and services.
In addition to the aforementioned pricing transparency rules, the government has also implemented certain additional pricing transparency requirements that apply to certain types of providers, including DaVita. Under the No Surprises Act, which went into effect January 1, 2021 while others2022, certain providers, including DaVita, are required to develop and disclose a “Good Faith Estimate” (GFE) that details the expected charges for furnishing certain items or services, although the government is currently only enforcing portions of this requirement with respect to uninsured or self-pay patients. The GFE is currently required to include specific information regarding the service provided and diagnostic codes, among other things, and is subject to formatting requirements, notice requirements, availability and dispute resolution procedures; in the future, GFEs will go into effect January 1, 2024. There is a possibility thatbe required to include additional information, including co-provider service estimates. Similar to the aforementioned pricing transparency rules, the impact of the GFE requirements on DaVita remains uncertain at this time, in part due to ongoing rulemaking around the No Surprises Act as well as the delayed effective date of certain provisions of the GFE framework, uncertainty around operational timeframes, potential penalties and patient reaction, among other things. While the ultimate impact of these requirements remains uncertain, any changes by group health plans, health insurance issuers in the group and individual markets, or consumer choices resulting from these requirements could have a material adverse impact on our business, results of operations, and financial condition, and could materially harm our reputation.
COVID-19 Response: In response to COVID-19, federal and state governments developed and passed legislation, rule making, interpretive guidance and modifications to agency policies and procedures, designed to provide emergency economic relief measures. These governmental responses included, among other things, regulations couldfrom OSHA and CMS that impact our revenueoperations. To the extent certain of these rules have remained in place following the conclusion of the COVID-19 public health emergency, they have added complexity and results of operations.uncertainty to the already complex and highly regulated environment in which we operate.
Other regulations
Our U.S. dialysis and related lab services operations are subject to various state hazardous waste and non-hazardous medical waste disposal laws. These laws do not classify as hazardous most of the waste produced from dialysis services. Occupational Safety and Health AdministrationOSHA regulations require employers to provide workers who are occupationally subject to blood or other potentially infectious materials with prescribed protections. These regulatory requirements apply to all healthcare facilities, including dialysis centers, and require employers to make a determination as to which employees may be exposed to blood or other potentially infectious materials and to have in effect a written exposure control plan. In addition, employers are required to provide or employ hepatitis B vaccinations, personal protective equipment and other safety devices, infection control training, post-exposure
evaluation and follow-up, waste disposal techniques and procedures and work practice controls. Employers are also required to comply with various record-keeping requirements.
In addition, a fewcertain states in which we do business have certificate of need programs regulating the establishment or expansion of healthcare facilities, including dialysis centers. Furthermore, given the evolving nature of our business, agencies, including but not limited to the Food and Drug Administration, FTC, and HHS's Office of Civil Rights, will continue to introduce and/or enforce existing laws and regulations that we may need to comply with. For additional information of the risks to our business associated with the impact of these and other laws and regulations, see the risk factors in Item 1A. Risk Factors under the headings, "Our business is subject to a complex set of governmental laws, regulations, and other requirements..." and "Changes in federal and state healthcare legislation or regulations..."
State laws and initiatives
There have been several statestate-based policy initiatives to limit payments to dialysis providers or impose other burdensome operational requirements, which, if passed, could have a material adverse impact on our business, results of operation, financial condition and cash flows. For example, on October 24,13, 2019, the Service Employees International Union - United Healthcare Workers West (SEIU) proposed a California statewide ballot initiative (Proposition 23)bill (AB 290) was signed into law that soughtlimits the amount of reimbursement paid to impose certain regulatory requirements on dialysis clinics, including requirements relatedproviders for services provided to physician staffing levels, clinical reporting, clinical treatment optionspatients with commercial insurance who receive charitable premium assistance (reimbursement cap). The implementation of AB 290 has been stayed pending resolution of legal challenges. The trial court recently issued a decision relating to these challenges to AB 290 that may result in the stay being lifted and limitations onat least some provisions of the ability to make decisions on closing or reducing serviceslaw being implemented in the near future, although any appeal of the decision may result in the stay being continued. In addition, California passed into law California Senate Bill No. 525 (SB 525), which raises minimum wage for dialysis clinics. While this ballot initiative was rejected by voters in 2020, we incurred substantial costs to oppose it.many California healthcare workers, effective as of June 1, 2024. We may continue to face ballot initiatives or other proposed regulations or legislation or ballot initiatives in California or other states in future years, which may require us to incur further substantial costs and which, if passed, could have a material adverse impact on our business, results of operations, financial condition and cash flows.
Evolving proposed or issued laws, requirements, rules and guidance that impact our business, including without limitation as may be described above, and any failure on our part to adequately adjust to any resulting marketplace developments could have a material adverse effect on our business, results of operations, financial condition and cash flows. For additional discussion on the risks associated with the evolving payment and regulatory landscape for kidney care, see the discussion in Item 1A1A. Risk Factors, including the discussion under the heading,headings, "Our business is subject to a complex seriesset of governmental laws, regulations and requirementsother requirements..." and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation" and "Changes"Changes in federal and state healthcare legislation or regulations could have a material adverse effect on our business, results of operations, financial condition and cash flows".regulations..."
Corporate compliance program
Our businesses are subject to extensive regulations. Management has designed and implemented a corporate compliance program as part of our commitment to comply fully with applicable criminal, civil and administrative laws and regulations and to maintain the high standards of conduct we expect from all of our teammates. We continuously review this program and work to enhance and evolve it as appropriate. The primary purposes of the program include:
•Assessing and identifying health care regulatory risks for existing and new businesses;
•Training and educating our teammates and certain affiliated professionals to promote awareness of legal and regulatory requirements, a culture of compliance, and the necessity of complying with all applicable laws, regulations and requirements;
•Developing and implementing compliance policies and procedures and creating controls to support compliance with applicable laws, regulations and requirements and our policies and procedures;
•Auditing and monitoring the activities of our operating units and business support functions to identify and mitigate risks and potential instances of noncompliance in a timely manner; and
•Ensuring that we promptly take steps to resolve any instances of noncompliance and address areas of weakness or potential noncompliance.
We have a code of conduct that each of our teammates, members of our Board of Directors (Board), certain affiliated professionals and certain third parties must follow, and we have an anonymous compliance hotline for teammates and patients to report potential instances of noncompliance that is managed by a third party. Our Chief Compliance Officer administers the compliance program. The Chief Compliance Officer reports directly to our Chief Executive Officer (CEO) and the Chair of the Compliance and Quality Committee of our Board of Directors (Board Compliance and Quality Committee). Previously, we were subject to a five-year Corporate Integrity Agreement (CIA) with OIG. The term of the CIA expired on October 22, 2019, and we were notified on May 20, 2020 that the OIG had closed out its review. The CIA (i) required that we maintain certain elements of our compliance programs; (ii) imposed certain expanded compliance-related requirements during the term of the CIA; (iii) required ongoing monitoring and reporting by an independent monitor, imposed certain reporting, certification, records retention and training obligations, allocated certain oversight responsibility to the Board’s Compliance and Quality Committee, and necessitated the creation of a Management Compliance Committee and the retention of an independent compliance advisor to the Board; and (iv) contained certain business restrictions related to a subset of our joint venture arrangements.Board.
Any futureWe could be subject to penalties sanctions or other consequences could be more severe in certain circumstances if the OIG or a similar regulatory authority determines that we knowingly and repeatedly failed to comply with applicable laws, regulations or requirements, that apply to our business, including, among other things substantial monetary penalties and exclusion from participation in federal healthcare programs that could have a material adverse effect on our business, results of operations, financial condition, and cash flows, reputation and stock price.
Competition
The U.S. dialysis industry has experienced consolidation over the last 20 years, but remains highly competitive. Patient retention andcompetitive, with many new entrants aggressively entering the continued referrals of patients from referral sources such as hospitals and nephrologists, as well as acquiring or developing new outpatient dialysis centers are some of the important parts of our growth strategy.kidney healthcare business space. In our U.S. dialysis business, we continue to face intense competition from large and medium-sized providers, among others, which compete directly with us for limited acquisition targets, for individual patients who may choose to dialyze with us and forto engage physicians qualified to provide required medical director services. Competition for growth in existingIn addition to these large and expanding geographies or areas is intense and is not limited to large competitorsmedium sized dialysis providers with substantial financial resources orand other established participants in the dialysis space. Wespace, we also compete with new dialysis providers, individual nephrologists and former medical directors or physicians that have opened their own dialysis units or facilities. Moreover, as we continue our international dialysis expansion into various international markets, we face competition from large and medium-sized providers, among others, for acquisition targets as well as physician relationships. We also experience competitive pressures from other dialysis and healthcare providers in recruiting and retaining qualified skilled clinical personnel as well as in connection with negotiating contracts with commercial healthcare payors and inpatient dialysis service agreements with hospitals. Acquisitions, developing new outpatient dialysis centers, patient retention and physicianreferrals, and referral source relationships, in which such sources understand us to be the clinical and operational leaders in the market are significant components of our growth strategy and our business could be adversely affected if we are not able to continue to make dialysis acquisitions on reasonable and acceptable terms, continue to develop new outpatient dialysis centers, maintain or establish new relationships with physiciansour referral sources' trust in our capabilities or if we experience significant patient attrition or lack of new patient growth relative to our competitors.
Together with ourOur largest competitor, Fresenius Medical GroupCare (FMC), we account for approximately 73% of outpatient dialysis centers in the U.S. Many of the centers not owned by us, FMC or other large for profit dialysis providers are owned or controlled by hospitals or non-profit organizations. Hospital-based and non-profit dialysis units typically are more difficult to acquire than physician-owned dialysis centers.
FMC also manufactures a full line of dialysis supplies and equipment in addition to owning and operating outpatient dialysis centers worldwide. This may, among other things, give FMC cost advantages over us because of its ability to manufacture its own products. Additionally, FMC has been one of our largest suppliers of dialysis products and equipment over the last several years. In January 2021, upon the expiration of our prior agreement with FMC on December 31, 2020, we entered into and subsequently extended a new agreement with FMC to purchase a certain amount of dialysis equipment, parts and supplies from FMC which extends through December 31, 2024. The amount of purchases from FMC over the remaining term of this agreement will depend upon a number of factors, including the operating requirements of our centers, the number of centers we acquire, and growth of our existing centers.
There have been a numberAs we continue to expand our efforts to grow across the full continuum of announcements bykidney care from CKD care to dialysis treatment to transplant facilitation, we also face competition outside dialysis. In the integrated care market, we face competition from other dialysis providers who, similar to DaVita, may be seeking to expand arrangements with payors, physicians and hospitals. We also face competition from non-traditional dialysis providers and others in this space, who have made a number of announcements, initiatives and capital raises in areas along the full continuum of kidney care from CKD to dialysis to transplant. These business entities, certain of which relate to entry intocommand considerable resources and capital, increasingly compete with us in the integrated kidney care market, and they may also focus their efforts on the development of more traditional dialysis and pre-dialysis space,competition or the commencement of other new business activities or the development of innovative technologies, drugs or the commencement of new business activitiesother treatments that could impact the rate of growth of the kidney care patient population or otherwise be disruptivetransformative to the industry. These developments over time may shift the competitive landscape in which we operate. For additional discussion on these developments and associated risks, see the risk factorfactors in Item 1A1A. Risk Factors under the heading, “headings, "If we are unable to compete successfully, including, without limitation, implementing our growth strategy and/or retaining patients and physicians willing to serve as medical directors, it could materially adversely affect our business, results of operations, financial condition and cash flowssuccessfully...”" and "If we are not able to successfully implement our strategy with respect to our integrated kidney care and value-based care initiatives..."
Insurance
We are predominantlyprimarily self-insured with respect to professional and general liability, and workers' compensation and automobile risks, and a portion of our employment liability practice risks, through wholly-owned captive insurance companies. We are also predominantly self-insured with respect to employee medical and other health benefits. We also maintain insurance, excess coverage, or reinsurance for property and general liability, professional liability, directors’ and officers’ liability, workers' compensation, cybersecurity and other coverage in amounts and on terms deemed appropriate by management, based on our actual claims experience and expectations for future claims. Future claims could, however, exceed our applicable insurance coverage. Physicians practicing at our dialysis centers are required to maintain their own malpractice insurance, and our medical directors are required to maintain coverage for their individual private medical practices. Our liability policies cover our medical directors for the performance of their duties as medical directors at our outpatient dialysis centers.
Human capital management
Overview
At DaVita, we are guided by our Mission—to be the provider, partner and employer of choice—and a set ofour Core Values—Service Excellence, Integrity, Team, Continuous Improvement, Accountability, Fulfillment and Fun—which are reinforced at all levels of the organization. Our teammates share a common passion for equitably improving patients' lives and are the cornerstone for the health of DaVita.
We strive to be a community first and a company second, and affectionately call ourselves a Village. To be a healthy Village, we need to attract, retain and motivate highly qualifieddevelop talented and diverse teammates. To do so, we have implemented strategies that support our mission to be the employer of choice, such as:
•Designing programs and processes to cultivate a diverse talent pipeline that allowscan allow us to hire ahead of needs;
•Providing development and professional growth opportunities; and
•Offering a robust and competitive total rewards program.
These efforts are underpinned by a foundational focus on diversity and belonging that starts at the top with our Board of Directors and executive leadership and permeates through our Village as further described below.
We believe that this intentional investment of time and resources fosters a special community of teammates that, in turn, inspires the Villageleads to take better care offor our patients and better care of the communities in which we live.serve.
As of December 31, 2023, we employed approximately 70,000 teammates, including our international teammates.
Oversight & Management
Our Board of Directors provides oversight on human capital matters, receiving regular updates from our Chief People Officer about People Services’ activities, strategies and initiatives, and through the Board’s annual work with our Chief Executive OfficerCEO on management development and succession planning. Among other things, our Board of Directors and/or its committees also receive reports related to pay equity, risks and trends related to labor and human capital management issues and generalother issues generally pertaining to our teammates. The Board, in conjunction with its committees, also oversees the Company's activities, policies and programs related to corporate environmental and social responsibility, including considering the impact of such activities, policies and programs on the Company, teammates, patients and communities.communities, among others.
These reports and recommendations to the Board and its committees are part of our broader People Services leadership and oversight framework, which includes guidance from various stakeholders across the business and benefits from the fullbroad participation of senior leadership.
Diversity & Belonging
Our investment in our teammates is underscored by our commitment to Diversity & Belonging (D&B). Our D&B vision is "a diverse Village where everyone belongs." Our 3,137 dialysis centers operate in communities large and small, in nearly every state in the U.S. as well as ten other countries: Brazil, China, Columbia, Germany, Malaysia, Poland, Portugal, Saudi Arabia, Singapore, and the United Kingdom. Our Village's diversity is inherent in the teammates who work in our centers, the patients we care for, the physicians with whom we partner, and the communities where we serve.
To help achieve this vision, we empower all leaders and teammates to cultivate D&B in their centers and on their teams. One way we do this is by sharing tools and resources like our Belonging Teammate and Belonging Leader Guides, which encourage teammates to connect with each other to learn about individual experiences with belonging and better understand the impact of unconscious bias.
We take a collaborative, leader-led approach to building our D&B program. Everyone from our front-line patient care technicians (PCTs) and nurses to our divisional vice presidents, our CEO, and our Board of Directors has a role in implementing our strategy. It truly does take a Village to bring our vision to life.
We published our second D&B Report in May 2023, which shared progress on our four strategic pillars - belonging, representation, economic mobility, and health equity - as well as other diversity metrics and roadmap for delivering our vision of cultivating "a diverse Village where everyone belongs." Our 3,042 dialysis centers operate in communities large and small, in nearly every state in the U.S. as well as 11 other countries. Our Village's diversity is inherent in the teammates who work in our centers, the patients we care for, the physicians with whom we partner and the communities where we serve.
To help achieve this vision, we empower all leaders and teammates to cultivate D&B in their centers and on their teams. Our intensive training for leaders sets the tone from the top, and we continue to expand our suite of resources for all teammates. Our executive team participated in an immersive nine-month Inclusive Leadership training. In 2022, we began scaling this experience to our vice presidents. Thus far, 86% of leaders at the VP level or above have completed this development program to advance our efforts toward creating trust and safety, respecting and valuing others and providing fair and consistent support. We have adapted this development program into a multi-week intensive course for manager and director-level teammates, which launched in the fourth quarter of 2023.
Over the past several years, our D&B efforts have focused primarily on supporting strong representation of women and people of color in our Village and ensuring that we are creating a welcoming, open environment where all teammates, patients, physicians and care partners belong.
In 2023, we expanded our network of employee resource groups to create a community for teammates from underrepresented groups. Based on our most recent internal surveys, 81% of teammates indicated that they feel a sense of belonging within the DaVita community. We also launched our fourth annual Week of Belonging in 2023, engaging teammates globally with activities and education designed to further create a sense of belonging.
As of December 31, 2020,2023, our Village in the U.S. was comprisedcomposed of 78% women and 54%57% people of color. We are proud of the fact that in the U.S. as of December 31, 2020,2023, 74% of our managers and 54%62% of our directors are women and that leaders with profit and loss responsibility are 52%53% women and 27%30% people of color. We also are proudSince 2018, we have seen a 6% increase in representation of women at the fact that ourVP level and for the first time ever, surpassed 40% women VP representation in 2023. In the same time period, we have seen a 6% increase in the representation of people of color at the VP level, from 16% in 2018 to 22% in 2023.
Our Board of
Directors is comprisedcomposed of 44%40% women and 33%10% people of color. With respect to Board leadership positions, we are one of the fewminority of companies in the S&P 500 to have a woman serving as the Chair of the Board. Additionally, we are part of the top 15th percentile of companies in the Fortune 500 and S&P 500 to have a person of color serve as our CEO. We publish our demographic data in our EEO-1 Report, which is included in our Sustainability Accounting Standards Board Report. As of Directors, and 75%December 31, 2023, we are meeting or exceeding 64% of our Board committees are led by women or people of color.EEO-1 benchmarks.
Talent Pipeline and Career Development
We understand that a key component of developing strong representation of women and people of color in leadership is to have recruiting practices focused on diversity. Some of ourOur practices include:
•Diverse Sourcing: Our recruiters are trained on how to source for diverse candidates to ensure we have a robust pipeline at all levels of the organization.
•Diversity in Hiring: We are committed to increasing diverse representation via our hiring practices. One way we do this is with diverse interview panels as well as diverse candidate slates to help ensure a fair and equitable process.
•Diverse Partnerships: We have external partnerships with organizations like Forte Foundation, and Management Leadership for Tomorrow and various Historically Black Colleges and Universities to help create equal opportunities for diverse candidates.
•Redwoods Leadership: We partner closely with diverse student body organizations at colleges and universities to source applicants for our Redwoods leadership development programs. Our 2023 incoming Redwoods class was 54% women and 37% people of color.
Helping teammates and leaders reach the next stage in their career and increasingincrease their earningsearning potential is onecomplements our Employer of our passions.Choice strategy. We have severala robust set of career development programs thatofferings to support teammates to furtherin reaching their careers. To help ensure that teammates have the support needed to succeed in their current roles, and grow their careers, weprofessional ambitions. We have invested in an end-to-end career development pipeline that includes programs and initiatives that provide financial, academiceducational and social support to our clinical and operations personnel to help achieve their higher education and leadership goals. For example, approximately 86%
Our DaVita Ladders program unlocks clarity, competitive pay and transparent career journeys to systematically create more effective leaders. Through DaVita Ladders, the Village can offer teammates and leaders:
•Clarity around role expectations;
•A universal language to describe and understand career progression across the business units and regions;
•Aiding talent mobility efforts to empower teammates with the ability to explore alternative career pathways based on interest, competency, and skill;
•A tool to support all aspects of the talent lifecycle through selection practices, personal development review (PDR) discussions, and succession planning, among other things;
•Standardization in how we execute performance and talent conversations that are aligned to factors for role success; and
•Market informed pay structure, pay design and guidance to our pay for performance philosophy.
Predominately all of our teammates are clinical field/operations personnel, and we have many programs in place to help guide their potential journey at DaVita. Beginning withprofessional development journeys. DaVita Ladders includes Clinical Ladders for our clinical teammates, and since rolling out our Clinical Ladders to our nurse and patient care technician teammates, we have celebrated more than 20,000 promotions. We have now expanded Clinical Ladders to approximately 49,000 teammates.
Additionally, we are proud to offer programs that cover certification fees for PCTssupport teammates to coachingincrease their earnings potential. For example, our Bridge to Your Dreams program supports high performing teammates pursuing an associate's degree in nursing with financial assistance, resources and tuition programs that help guide PCTsrole placement support to becoming registered nurses (RNs) tobecome a DaVita nurse. We also offer programs that help develop high potential nurses, clinical coordinators and clinic nurse managers into operational managers, and ultimately toalong with programs that prepare and coach operational managers for potential regional operations director roles,roles. These are just some of the many other career development opportunities we have in place for our teammates.
Our goal is to make resources available to teammates at each step of a possible career path. We are proud of the work we have done in this area, with approximately 58% of our Facility Administrators and managers having been promoted internally, and over 2,000 teammates actively enrolled in the Bridge to Your Dreams program, as of December 31, 2023.
Total Rewards Program and Pay Equity
Our paytotal rewards philosophy and practices are designed to be competitive in the local market and to reward strong team and individual performance. We believe merit-driven pay encourages teammates to do their best work, including in caring for our patients, and we strive to link pay to performance so we can continue to incentivize the provision of extraordinary care to our patients and grow our Village.
To helpattract, retain and grow our teammates, reachwe have a holistic approach to total rewards that includes financial, physical and emotional support. Highlights include, among other things:
•Healthcare benefits including a menu of plan designs and health savings accounts.
•Free health programs in support of the most prevalent health conditions affecting our teammates, including hypertension, diabetes prevention/maintenance, musculoskeletal issues and weight loss/management.
•Financial wellness elements including 401(k) match, employee stock purchase plan (ESPP), a deferred compensation plan, financial planning support and access to free banking services. Additionally, DailyPay is a service that provides teammates with financial flexibility by allowing them to access earned but unpaid wages before payday.
•Family support programs to our teammates and their full potential, wefamilies that include family care programs for back-up child and elder care, family planning support for fertility, adoption and surrogacy, parental support for children’s educational and special needs and parental leave programs. We also offer a total rewards package. More than just pay, our comprehensive compensation package connects teammates to robust health care coverage, resourcesnumber of scholarships for retirement planningteammates' children and savings, opportunities for career development, and well-being resources for every stage of life.
To support our teammates in maintaining strong physical and mental health, we offer a variety of physical and mental health benefits programs, including, among other things:grandchildren.
•Teammate Assistance Program that offers counseling sessions annually to all teammates and their household members, along with work/life resourcescritical incident support for work related trauma, on both a personal and tools that include telephonic or facegroup level, with access to face legal consultation and expert financial planning/consultation.ten free sessions annually for each household member.
•Free access to Headspace, an application for digital meditation and mindfulness, and referrals/consultations on everyday issues such as dependent care, auto repair, pet care and home improvement.
•Vitality Points, a voluntary wellness incentive program that encourages teammates and their spouses/domestic partners to engage with their provider to manage their overall health. In addition, it allows participating teammates and spouses/domestic partners to earn credits toward their medical premium for getting a biometric screening and engaging in healthy actions should they not meet certain targets.with a primary care provider.
•Short & Long term disability for full time teammates and Life/AD&D coverage at both the basic and supplemental levels.
•Our DaVita Village Network, which provides financial support to eligible teammates experiencing a specific tragedy or hardship and helps cover additional costs that local fundraising and insurance dodoes not fully cover.
In support of our teammates and their families, we also offer family support programs that include family care programs for back-up child and elder care, parental support and parental leave programs. We also offer a number of scholarships for teammates' children and grandchildren.
We also offer a robust suite of financial well-being programs for eligible teammates including, among others, a 401(k) program with company match, an employee stock purchase plan, health savings account funding for certain high deductible health plans and a deferred compensation plan. We also offer DailyPay, a service that provides teammates with financial flexibility by allowing them to access earned but unpaid wages before payday for a nominal fee.
Pay Equity
At DaVita, we are committed to equal pay for equal work; meaning, teammates in the same position, performing at the same level, and in similar geographies, are paid fairly relative to one another, regardless of their gender, race or ethnicity. We believe that equitable pay is a critical component of establishing a fair work environment where all teammates are valued and feel like they belong. Fair pay is essential to our ability to attract and motivate the highly qualified and diverse teammates who are at the center of our current and future success.
AgileContinued Response Teammate Feedback and Responding to the Public Health CrisisCOVID-19
The COVID-19 pandemic tested our ability to respond to external developmentsfederal public health emergency (PHE) ended in May 2023, and care for our teammates in real time. In responseas we adapt to the hardship imposed by the pandemic on our teammates,evolving health and in recognition of their dedication and commitment to our patients’ health, DaVita provided financial relief to over 50,000 teammates, such as a “Village Lives” award of $100 per week from March through May 2020, as well as other relief payments during the pandemic. In addition, we did not furlough, layoff or reduce pay for any teammates due to the pandemic. One of our key goals during the pandemic was to maintain frequent communication and engagement with teammates, including “town hall” calls, emails and more. As the pandemic has persisted,regulatory environment, we continue to provide essential relief programs to support these teammates, including backup childcare, modified sick policies and certain increased overtime pay for front-line positions.
Most importantly,prioritize the health, well-being and safety of our teammates, in the Villagephysician partners and their families remains a top priority throughout this ongoing pandemic. We implemented guidance earlyfamilies. To the extent operations and protocols in the pandemic to help mitigate health and safety risks imposed by COVID-19, including, among other things:
•Securing necessary supplies of personal protective equipment;
•Restricting visitors to our centers;
•Screening teammates, patients and visitors for signs and symptoms of, or exposure to, COVID-19, before allowing entry into our clinics or business offices;
•Implementing an early universal masking policy;were dependent on PHE waivers of certain requirements under federal health care legislation and
•Providing guidance on staying safe outside regulation, we prepared in advance for the sunsetting of our centers.
We also converted our live, in-person teammate and leadership development programs to virtual delivery,these federal waivers to help ensure that our teammates across our global Village couldcontinuity of care and teammate safety. We completed an internal assessment on dependencies for PHE-specific waivers and identified clinics with varying levels of waiver dependencies. As a result, we were well-positioned to wind down the remaining few practices with waiver dependencies by May 2023 in the ordinary course. We have integrated key stand-alone COVID-19 practices into standard infection control workflows. We continue to grow personallyoffer COVID-19 testing and professionally and have access to career development resources despite the ongoing pandemic.
We believe our ability to engage with teammates and respond to these developments has helped us to better care for them. By caring for our teammates, we were generally able to maintain continuity of carevaccines for our patients and support the broader healthcare community throughout this unprecedented public health crisis.
As of December 31, 2020, we employed approximately 67,000 teammates, including our international teammates.
For additional information about certain risks associated with our human capital management, see the risk factorfactors in Item 1A1A. Risk Factors under the heading,headings, "IfOur business is labor intensive and if our labor costs continue to rise, including due to shortages, changes in certification requirements and/or higher than normal turnover rates in skilled clinical personnel; or currently pending or future governmental laws, rules, regulations or initiatives impose additional requirements or limitations on our operations or profitability; or, if we are unable to attractrise...;" and retain key leadership talent, we may experience disruptions in our business operations"Macroeconomic conditions and increases in operating expenses, among other things, which could have a material adverse effect on our business, results of operations, financial condition and cash flows.global events..."
We also encourage you to visit our website at www.davita.comdavitacommunitycare.com for more detailed information regarding certain aspects of theour human capital and ESG related programs and initiatives described herein, including our Policy on FairD&B Report and Equitable Pay,Community Care Report, as well as our efforts to care for our patients, our community and our world. Nothing on our website, sections thereof or documents linked thereto, shall be deemed incorporated by reference into this Form 10-K.report.
Item 1A. Risk Factors
This Annual Report on Form 10-K contains forward-looking statements within the meaning of the federal securities laws. Please read the cautionary notice regarding forward-looking statements in Item 7 of Part II of this Annual Report on Form 10-K under the heading “Management’s"Management’s Discussion and Analysis of Financial Condition and Results of Operations.”" These forward-looking statements involve risks and uncertainties, including those discussed below, which could have a material adverse effect on our business, cash flows, financial condition, results of operations and/or reputation. The risks and uncertainties discussed below are not the only ones facing our business. Additional risks and uncertainties not currently known to us or that we currently deem to be immaterial could also have a material adverse effect on our business, cash flows, financial condition, results of operations and/or reputation.
Summary Risk Factors
The following is a summary of the principal risks and uncertainties that could adversely affect our business, cash flows, financial condition and/or results of operations, and these adverse impacts may be material. This summary is qualified in its entirety by reference to the more detailed descriptions of the risks and uncertainties included in this Item 1A1A. below and you should read this summary together with those more detailed descriptions.
These principal risk and uncertainties relate to, among other things:
Risks Related to the Operation of our Business
•our negotiations and arrangements with commercial payors, including with respect to value-based care and Medicare Advantage plans, the average rates that commercial payors pay us, any restrictions in plan designs or other contractual terms, including, without limitation, the scope and duration of coverage and in-network benefits;
•the number or percentage of our patients with higher-paying commercial insurance;
•our ability to successfully implement our strategy with respect to home-based dialysis;
•changes in the structure of and payment rates under government-based programs;
•changes in clinical practices, payment rates or regulations impacting pharmaceuticals;
•our ability to compete successfully, including, without limitation, implementing our growth strategy and/or retaining patients and physicians willing to serve as medical directors;
•our acquisitions, mergers, joint ventures or dispositions;
•servicesour ability to appropriately estimate the amount of dialysis revenues and related refund liabilities;
•changes in physician referrals to our dialysis centers, whether due to governmental laws, regulations or other requirements, new competition, a perceived decrease in the quality of service levels at our centers or other reasons;;
•increasespolitical, economic, legal, operational and other risks as we expand our operations and offer our services in labor costs, including, without limitation, due to shortages, changes in certification requirements and/or higher than normal turnover rates in skilled clinical personnel; or currently pending or future governmental laws, rules, regulations or initiatives;markets outside of the U.S., and utilizing third-party suppliers and service providers operating outside of the U.S.; •our ability to attract and retain key leadership talent;
•our ability to attract and retain employees or our ability to manage operating cost increase or productivity decreases whether due to union organizing activities or legislative or other changes;
General Risks
•liability claims for damages and other expenses that are not covered by insurance or exceed our existing insurance coverage;
•our ability to successfully maintain an effective internal control over financial reporting;
Risks Related to the Operation of our Business
We face various risks related
Macroeconomic conditions and global events have impacted and will continue to impact our business and cost structure in a variety of ways, and these and other uncontrollable events may in the dynamicfuture impact the rate of growth of our patient population and evolving novel coronavirus pandemic, anyour ability to grow the business. There can be no assurance that we will be able to successfully execute cost savings or other initiatives in a manner that will offset the impact of these conditions, which may havecould result in a material adverse impact on us.
The disease causedWe continue to be impacted by general conditions in the novel coronavirus (COVID-19) is impactingglobal economy and marketplace, many of which may be interrelated. These conditions relate to, among other things, inflation, interest rates, challenging labor market conditions, supply chain challenges, continuing effects of COVID-19 and other factors that may impact our long term rate of growth of our patient population. Certain of these impacts could be further intensified by concurrent global events such as the worldongoing conflict between Russia and our businessUkraine and in many different ways.Israel, Gaza and the surrounding areas, which have continued to drive sociopolitical and economic uncertainty and volatility across the globe. The ultimate impact of COVID-19these and other conditions on us will dependour business over time depends on future developments that are highly uncertain and difficult to predict, including among other things, the severity and duration of the pandemic; further spread or resurgence of the virus, including as a result of the emergence of new strains of the virus; its impact on the chronic kidney disease (CKD) population and our patient population; the availability, acceptance, impact and efficacy of COVID-19 treatments, therapies and vaccines; the pandemic’s continuing impact on the U.S. and global economies and unemployment; the responses of our competitors to the pandemic and related changes in the marketplace; and the timing, scope and effectiveness of federal, state and local governmental responses. The impact could come in many forms, including but not limited to those described below.predict.
•We also have risk associated with COVID-19. We have experienced and expect to continue to experience a negative impact on revenue and non-acquired growth from COVID-19 due to lower treatment volumes, including from the negative impact of COVID-19 on the mortality rates of our patients, which has in turn impacted our patient census, that is the result of changes in rates of mortality. Because ESRD patients may be older and generally have comorbidities, several of which are risk factors for COVID-19, we believe the mortality rate of infected patients is, and will continue to be, higher in the dialysis population than in the general population, and COVID-19 also could impact the CKD population differentially. Over the longer term, we believe that changes in mortality in both the CKD and ESRD populations due to COVID-19 will depend primarily on the infection rate, case fatality rate, the age and health status of affected patients, the access to and efficacy of vaccinations as well as willingness to be vaccinated.the direct and indirect impact of COVID-19 on our missed treatment rate and new admissions. We expect that these changes arethe impact of COVID-19 is likely to continue to negatively impact our revenue and non-acquired growth even asfor a period of time due to the pandemic subsides. However, determiningongoing impact of the virus on ESKD and CKD patient mortality rates, among other things. New admission rates, future revenues and non-acquired growth could also continue to be negatively impacted over time to the extent to which these impacts should be directly attributable to COVID-19 is difficultthat the CKD population experiences elevated mortality levels due to testingCOVID-19. As further described below in the risk factor under the heading, "If we are unable to compete successfully...", certain other events beyond our control could also impact the rate of growth of our ESKD patient population. Any decrease in growth rates for the ESKD or CKD patient population, higher mortality rates for dialysis patients or other reductions in demand for dialysis treatments, if sustained or significant, could have a material adverse effect on our business, results of operations, financial condition and reporting limitations, and other factors may drive treatment volumes and new admissions over time,cash flows. Any such asimpact would be magnified to the number of transplants or deferred admissions. The magnitude of these cumulative impacts has been substantial and, depending on the ultimate severity and duration of the pandemic could be material.extent it also
��� The COVID-19 pandemic and effortsresulted in a lower number of patients with commercial insurance or a lower percentage of patients under commercial insurance relative to contain the virus have led togovernment-based programs.
Ongoing global economic deteriorationconditions and rapidpolitical and sharpregulatory developments, such as general labor, supply chain and inflationary pressures have also increased, and will continue to increase, our expenses, including among other things, staffing and labor costs. Our business is labor intensive and our financial and operating results have been and continue to be sensitive to variations in labor-related costs and productivity. We have historically faced and expect to continue to face difficulties in hiring and retaining caregivers due in part to a nationwide shortage of clinical personnel. We expect certain of these increased staffing and labor costs to continue, due to, among other factors, recent legislative changes, such as Senate Bill 525 in California, and increased training costs. The cumulative impact of these increased costs could be material. In addition, our industry has experienced increased union organizing activities, including the filing of petitions by unions at certain of our competitors' clinics with a number of those clinics voting to unionize. Potential staffing shortages or other potential developments or disruptions related to our teammates, if material, could ultimately lead to the unplanned closures of certain centers or adversely impact clinical operations, or may otherwise have a material adverse impact on our ability to provide dialysis services or the cost of providing those services, among other things.
The staffing and labor cost inflation described above, in addition to higher equipment and clinical supply costs, among other things, have put pressure on our existing cost structure, and we expect that some of these increased costs will continue as labor market conditions remain challenging, global supply chains continue to experience volatility and disruptions and as inflationary pressures continue. Prolonged volatility, uncertainty, labor supply shortages and other challenging labor market conditions could have an adverse impact on our growth and ability to execute on our other strategic initiatives and a material adverse impact on our labor costs, among other things. Prolonged strain on global supply chains may result in equipment and clinical supply shortages, disruptions, delays or associated price increases that could impact our ability to provide dialysis services or the cost of providing those services, among other things. Moreover, to the extent that monetary policies or other factors impacting structural costs over the long term have contributed to or may in unemployment levels, whichthe future contribute to inflationary pressures, this may in turn continue to increase our labor and supply costs at a rate that outpaces the Medicare or any other rate increases we may receive. In our value-based care and other programs where we assume financial accountability for total patient cost, an increase in our underlying staffing and labor expenses could have an impact on total cost of care. This increase may in turn impact the profitability of those programs relative to their respective funding.
We continue to invest in and implement cost savings initiatives designed to help mitigate these cost and volume pressures. These include, among other things, anticipated cost savings related to general and administrative cost efficiencies, such as ongoing initiatives that increase our use of third party service providers to perform certain activities, including financial reporting and information technology functions, initiatives relating to clinic optimization, initiatives for capacity utilization improvement, and procurement opportunities. We have incurred, and expect to continue to incur charges in connection with the continued implementation of these initiatives, and there can be no assurance that we will be able to successfully execute these initiatives or that they will achieve expectations or succeed in helping offset the impact of these challenging conditions. Any failure on our part to adjust our business and operations in this manner, to adjust to other marketplace developments or dynamics or to appropriately implement these initiatives in accordance with applicable legal, regulatory or compliance requirements could adversely impact our ability to provide dialysis services or the cost of providing those services, among other things, and ultimately could have a material adverse effect on our business, reputation, results of operations, financial condition and cash flows.
Deterioration in economic conditions, whether driven by macroeconomic conditions, global events, domestic political or governmental volatility or other events beyond our control, including the aforementioned inflationary and labor market pressures, volatility and uncertainty, as well as potential volatility in interest rates, could have a material adverse effect on our business, results of operations, financial condition and cash flows. Among other things, the potential decline in federal and state tax revenues that may result from a deterioration in economic conditions may create additional pressures to government sponsored programs. Any potential period of extended or increased job losses in the U.S. as a result of adverse economic conditions, including economic deterioration, could ultimately result in a materially reduced sharesmaller percentage of our patients being covered by commercial insurance plans, with more patientsan employer group health plan and a larger percentage being covered by lower-paying government insurance programs or being uninsured. These effects may persist after the pandemic subsides as, among other things, our patients could experience permanent changes in their insurance coverage as a result of changes to their employment status. In the event such a material reduction occurs in the share of our patients covered by commercial insurance plans, it would have a material adverse impact on our business, results of operations, financial condition and cash flows. The extent of these effects will depend upon, among other things, the extent and duration of theany increased unemployment levels for our patient population, any economic deterioration andor potential recession; the timing and scope of federal, state and local governmental responses to the ongoing pandemic; and patients’ ability to retain existing insurance and their individual choices with respect to their coverage.
• We have dedicatedcoverage, all of which are highly uncertain and continuedifficult to dedicate substantial resourcespredict. Declining economic conditions or other pressures that drive increased focus on healthcare costs may lead, employers to select more restrictive commercial plans with lower reimbursement rates. To the extent that payors are negatively impacted by a decline in response to COVID-19the economy, we may experience further pressure on commercial rates, a slowdown in collections and have had, anda reduction in the amounts we expect to continuecollect. For additional information on risks regarding the potential impact of decreases to have, extended and significant additional costs in connection with our response to COVID-19. The steps we have taken designed to help safely maintain continuitythe percentage or
number of care for our patients and help protect our caregivers, such as our policies to implement dedicated care shifts forwith commercial insurance, see the risk factor under the heading "If the number or percentage of patients with confirmed or suspected COVID-19 and other enhanced clinical practices, have increased, and are expected to continue to increase, our expenses and use of personal protective equipment (PPE). Our response to COVID-19 also has resulted in higher salary and wage expense, and we have provided, and may provide in the future, substantial financial support associated with relief reimbursement to our teammates. Furthermore, the effort and cost needed to procure certain of our equipment and clinical supplies, including PPE, have increased, and we expect these increased costs will continue while the pandemic persists. These efforts are part of a wider Prepare, Prevent, Respond and Recover protocol that we have implemented in connection with the pandemic, which also includes operational initiatives such as the redistribution of teammates, machines and supplies across the country as needed and increased investment in and utilization of telehealth capabilities. Our response protocol generally has allowed us to maintain continuity of care for our patients. If the pandemic requires us to maintain certain restrictive operational protocols for an extended period of time, it may adversely impact our strategic initiatives, such as our strategy to continue to build o our abilities to offer home dialysis options. Certain temporary changes made in response to the COVID-19 pandemic could become permanent, which could have an adverse impact on our business. In addition, any equipment or clinical supply shortages, disruptions or delays or associated price increases could impact our ability to provide dialysis services or the cost of providing those services.higher-paying commercial insurance declines..."
• We have had, and expect to continue to have, increased costs and risk associated with a high demand for our skilled clinical personnel. Historically we have faced costs and difficulties in hiring and retaining nurses and other caregivers due to a nationwide shortage of skilled clinical personnel, and these challenges have been heightened by the increased demand for and demand upon such personnel by the ongoing pandemic, particularly the more recent resurgence of the virus that is more widespread geographically, which, among other things, makes it more difficult for us to reallocate our resources to affected geographies. Any staffing shortages or disruptions could impact our ability to provide dialysis services or the cost of providing those services.
• If we experience a failure of the fitness of our clinical laboratory, dialysis centers and related operations and/or other facilities as a result of the COVID-19 pandemic, or another event or occurrence adversely impacts the safety of our caregivers or patients, we could face adverse consequences, including without limitation, material negative impact on our brand, increased litigation, compliance or regulatory investigations, teammate unrest, work stoppages or other workforce disruptions. Any legal actions brought by patients, teammates, caregivers or others allegedly exposed to COVID-19 at our facilities or by our caregivers may involve significant demands and require substantial legal defense costs, which may not be adequately covered by our professional and general liability insurance.
• If general economic conditions continue toor labor market conditions deteriorate or remain uncertain for an extended period of time, we may experience negative impacts on reimbursement rates or the availability of insurance coverage for our patients, which may in turn materially and unfavorably impact our revenues and financial results. These impacts could lead us to incur future charges to recognize impairment in the carrying amount of our goodwill and other intangible assets.assets, which could have a material adverse effect on our business, results of operations and financial condition. As of December 31, 2023, we had approximately $7 billion of goodwill recorded on our consolidated balance sheet. We account for impairments of goodwill in accordance with the provisions of applicable accounting guidance, and record impairment charges when and to the extent a reporting unit's carrying amount is determined to exceed its estimated fair value. We use a variety of factors to assess changes in the financial condition, future prospects and other circumstances concerning our businesses and to estimate their fair value when applicable. These assessments and the related valuations can involve significant uncertainties and require significant judgment on various matters.
The aforementioned impacts may experiencealso drive an increased need for additional liquidity funded by accessing existing credit facilities, raising new debt in the capital markets, or other sources, and we may seek to refinance existing debt, which may be more difficult or costly as a resultin an uncertain or declining economic environment. For additional information regarding the risks related to our indebtedness, see the discussion in the risk factor under the heading "The level of the pandemic’s impact on capital markets or on us.our current and future debt..." Furthermore, any extended billing or collection cycles, or deterioration in collectability of accounts receivable, will adversely impact our results of operations and cash flows.
• In our value-based care and other programs where we assume financial accountability for total patient cost, an increase in COVID-19 rates among patients could have an impact on total costAny or all of care. This increase may in turn impact the profitability of those programs relative to their respective funding.
• The global nature of the pandemic may have varying impacts on our ongoing operations outside the United States, and may impact our ability to expand our operations into other parts of the world.
The government response to the pandemic has been wide-ranging and will continue to develop over time, particularly in light of the new federal administration. As a result, we may not be able to accurately predict the nature, timingthese economic conditions or extent of resulting changes to the markets in which we conduct business or on the other participants that operate in those markets, or any potential changes to the extensive set of federal, state and local laws, regulations and requirements that govern our business. We believe that these changes may impact our business in a variety of ways, including but not limited to those described below.
• Our need, ability and willingness to use and retain any provider relief or other funds or assistance from the government, the consequences of our decisions with respect thereto, our ability to operate within any restrictions on our business or operations that may be imposed as a condition to participation in any government assistance programs, and the impact of any such programs on our competitors, all will depend, among other things, on the magnitude, timing and nature of COVID-19’s impact on the Companydevelopments, as well as the requirementsother consequences of any such programs, which are uncertain. There can be no assurance that financialthese conditions or other assistance will be available from the government if we have a need for such assistance in the future.
• State and local shelter in place and social distancing restrictions and guidance have required us to significantly increase the use of remote arrangements for our teammates and telehealth technology for our dialysis patients, which broadens our technology footprint for where and how protected health information is used or disclosed, and in turn increases our exposure to the various privacy and information security risks we face, such as the risk of "phishing" and other cybersecurity attacks and the risk of unauthorized dissemination of sensitive personal, proprietary or confidential information.
• We have worked with certain government agencies and other kidney care providers to respond to the COVID-19 pandemic, and in certain cases have sought waivers of regulatory requirements. For example, as part of our efforts to help cohort patients in line with guidance from the CDC, we have sought waivers of certain regulatory requirements related to the survey and acceleration of new clinics and entered into agreements with other kidney care providers to help ensure that patients can receive dialysis in an outpatient setting rather than a hospital. In addition, we are also working to help make COVID-19 vaccines available to patients and teammates, including through coordination with state and federal governments on direct vaccine distribution so that we can administer vaccines to our patients and teammates. These vaccines are currently available under emergency use authorizations and there can be no assurance that our patients and caregivers will choose to receive a COVID-19 vaccine or that the vaccines will prove to be as safe and effective as currently understood by the scientific community. In addition, we may encounter difficulties with the availability, storage of the vaccine, or administration of the vaccines,developments, some of which have multiple dose requirements. We operate in a complexare beyond our control and highly regulated environment, and the novel naturenone of our COVID-19 response, including, for example, with respect to regulatory waivers and our administration of the newly developed COVID-19 vaccines, may increase our exposure to legal, regulatory and clinical risks.
The foregoing and other continued impacts and disruptions to our business as a result of the COVID-19 pandemicwhich we can reasonably predict, could have a material adverse impacteffect on our patients, teammates, physician partners, suppliers, business, operations, reputation, financial condition, results of operations, financial condition and/or cash flows and/or liquidity.materially harm our reputation. In addition, the COVID-19 pandemic heightensthese conditions or developments each may heighten many of the other risks and uncertainties discussed herein. For additional information related to COVID-19 and its impact on our business, see the discussion in Part I, Item 1. Business under the headings, "COVID-19 and its impact on our business" and "Human Capital Management" and Part II, Item 7, “Management's Discussion and Analysis of Financial Condition and Results of Operations.”
Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation.
We operate in a complex regulatory environment with an extensive and evolving set of federal, state and local governmental laws, regulations and other requirements that apply to us. These laws, regulations and other requirements are promulgated and overseen by a number of different legislative, regulatory, administrative, and quasi-regulatory bodies, each of which may have varying interpretations, judgments or related guidance. As such, we utilize considerable resources on an ongoing basis to monitor, assess and respond to applicable legislative, regulatory and administrative requirements, but there is no guarantee that we will be successful in our efforts to adhere to all of these requirements. Laws, regulations and other requirements that apply to or impact our business include, but are not limited to:
•Medicare and Medicaid coverage and reimbursement statutes, and other federal coverage and reimbursement statutes, rules and regulations (including, but not limited to, manual provisions, local coverage determinations, national coverage determinations, payment schedules and agency guidance);
•Medicare and Medicaid provider requirements, including, but not limited to, requirements associated with providing and updating certain information about the Medicare or Medicaid entity, as applicable, and its direct and indirect affiliates;
•Federal fraudSection 1115A of the Social Security Act, which, among other things, authorizes the Center for Medicare and Medicaid Innovation (CMMI) to test certain innovation models;
•Fraud waste and abuse laws and analogous state laws;
•the 21st Century Cures Act (the Cures Act);
•Federal Acquisition Regulations;
•the Foreign Corrupt Practices Act (FCPA);, the Uniting and Strengthening America by Providing Appropriate Tools Required to Intercept and Obstruct Terrorism Act of 2001, Public Law 107-56 (Patriot Act), Executive Order No. 13224 on Terrorist Financing, effective September 24, 2001, and similar laws and regulations;
•Federal and state antitrust and competition laws and regulations;
•laws and regulations related to the corporate practice of medicine;
•individualized state law requirements associated with the operation of our business;laws and
•federal and state laws regulations regarding the collection, use and disclosure of patient health information (e.g., Health Insurance Portability and Accountability Act of 1996 (HIPAA));
•the No Surprises Act;
•laws and regulations regarding the storage, handling, shipment, disposal and/or dispensing of pharmaceuticals and blood products and other biological materials.materials;
In addition, we have been subject to a five-year Corporate Integrity Agreement (CIA) with Office of Inspector General (OIG) for the U.S. Department of Health and Human Services (HHS). The term of the CIA expired on October 22, 2019, and we were notified on May 20, 2020 that the OIG had closed out its review. Any future penalties, sanctions or other consequences imposed on us could be more severe in certain circumstances if the OIG or a similar regulatory authority determines that we knowingly and repeatedly failed to comply with applicable •laws, regulations or other requirements,guidance across jurisdictions that require enhanced disclosures and could adversely impactdue diligence surrounding the impacts of our results of operationsCompany and value chain on, and the financial risks and opportunities for our Company from, environmental, social and governance (ESG) or financial conditionother similar sustainability or could have a negativecorporate responsibility matters, as well as enhanced policies, processes and controls designed to appropriately monitor and track such information and enhanced actions to address our Company's impact on our reputation.these matters; and
The foregoing are each themselves comprised•individualized state laws and regulations associated with the operation of numerous associated regulations or other requirements that have varying levels of impact on our business.
If any of our personnel, representatives, third party vendors, or operations are alleged to have violated these or other laws, regulations or requirements, we could experience material harm to our reputation and stock price, and it could impact our relationships and/or contracts related to our business, among other things. If any of our personnel, representatives, third party vendors or operations are found to violate these or other laws, regulations or requirements, we could suffer additional severe consequences that wouldcould have a material adverse effect on our business, results of operations, financial condition and cash flows, and could materially harm our reputation and stock price, including, among others:
•Loss of required certifications or suspension or exclusion from or termination of our participation in government programs (including, without limitation, Medicare, Medicaid and Center for Medicare and Medicaid Innovation (CMMI)CMMI demonstration programs);
•Refunds of amounts received in violation of law or applicable payment program requirements dating back to the applicable statute of limitation periods;
•Loss of licenses required to operate healthcare facilities or administer pharmaceuticals in the states in which we operate;
•Reductions in payment rates or coverage for dialysis and ancillary services and pharmaceuticals;
•Criminal or civil liability, fines, damages or monetary penalties, which could be material and/or could materially harm our reputation or stock price;penalties;
•Imposition of corporate integrity agreements, corrective action plans or consent agreements;
•Enforcement actions, investigations, or audits by governmental agencies and/or state law claims for monetary damages by patients who believe their protected health information (PHI) has been used, disclosed or not properly safeguarded in violation of federal or state patient privacy laws, including, among others, HIPAA and the Privacy Act of 1974;
•Enforcement actions, investigations, or audits by government agencies related to interoperability and related data sharing and access requirements and regulations;
•Mandated changes to our practices or procedures that significantly increase operating expenses that could subject us to ongoing audits and reporting requirements as well as increased scrutiny of our billing and business practices which could lead to potential fines, among other things;
•Termination of various relationships and/or contracts related to our business, such as joint venture arrangements, medical director agreements, hospital services and skilled nursing home agreements, real estate leases, value-based care arrangements, clinical incentive programs, payor contracts, debt agreements and consulting or participating provider agreements with physicians;physicians, among others; and
•Harm to our reputation, which could negatively impact our business relationships and stock price, affect our ability to attract and retain patients, physicians and teammates, affect our ability to obtain financing and decreaseour access to new business opportunities, among other things.
Any future penalties, sanctions or other consequences could be more severe in certain circumstances if the OIG or a similar regulatory authority determines that we knowingly or repeatedly failed to comply with laws, regulations or requirements that apply to our business. Additionally, the healthcare sector, including the dialysis industry, is also regularly subject to negative publicity, including as a result of governmental investigations, adverse media coverage and political debate surrounding industry regulation.the U.S. healthcare system, among other things. Negative publicity, regardless of merit, regarding the dialysis industry generally, the U.S. healthcare system or DaVita in particular may adversely affect us.
See Note 1615 to the consolidated financial statements included in this report for further details regarding certain pending legal proceedings and regulatory matters to which we are or may be subject from time to time, any of which may include allegations of violations of applicable laws, regulations and requirements.requirements.
Changes in federal and state healthcare legislation or regulations could have a material adverse effect on our business, results of operations, financial condition and cash flows.
Each of the laws, regulations and other requirements that govern our business may continue to change over time, and there is no assurance that we will be able to accurately predict the nature, timing or extent of such changes or the impact of such changes on the markets in which we conduct business or on the other participants that operate in those markets.
Among other things, the regulatory framework of the Patient Protection and Affordable Care Act and the Health Care Reconciliation Act of 2010, as amended (collectively, the ACA), and other healthcare reforms continuemarketplace continues to evolve as a result of executive, legislative, regulatory and administrative developments and judicial proceedings. These changes shape the landscape for our current dialysis businessand ancillary businesses as well as for emerging comprehensive and integrated kidney care markets. For example, an executive order issued in July 2019 (the 2019 Executive Order) directed CMS to create payment models through CMMI to evaluate the effects of creating payment incentives for the greater use of home-based dialysis and kidney transplants for those already on dialysis, improve quality of care for kidney patients and reduce expenditures. In addition, future legislative action related to, among other things, full capitation demonstration for ESRD may ultimately impact our ability to provide a competitive and successful integrated care program at scale. Weas further described below, we have made and continue to makesubstantial investments in building and dedicated resources to our integrated care capabilities, butbusiness, value-based care initiatives and home-based dialysis business to address recent regulatory developments that include innovative payment models, and there canare risks to those investments, or additional investments may be no assurances that initiatives such as this or similar legislation will be passed into law, and the ongoing COVID-19 pandemic may delay the progress of such initiatives. If such legislation is passed, there can be no assurances that we will be able to successfully execute on the required, strategic initiatives that would allow us to provide a competitive and successful integrated care program on the broader scale contemplated by this legislation, and in the desired time frame. Additionally, the ultimate terms and conditions of any such potential legislation remain unclear. For example, our costs of care could exceed our associated reimbursement rates under such legislation. Any failure on our part to adequately implement strategic initiatives to adjust to any marketplace developments resulting from executive, legislative, regulatory or administrative changes such as these could have a material adverse impact on our business.
There have been multiple attempts to repeal or amend the ACA through legislative action and legal challenges, and the most recent challenge is currently before the U.S. Supreme Court. In the event the ACAregulatory environment changes and we do not adequately adapt to such changes.
In addition, access to healthcare has been both positively and negatively impacted over time by legal, regulatory and judicial action and changes to the political environment may increase the likelihood of regulatory or legislative changes that would impact us. If access to healthcare is repealed or significantly altered it wouldor if other reforms limiting access to healthcare are enacted in the future, such changes could impact our business in a number of ways, some of which may be material. The outcome of this U.S. Supreme Court proceeding will likely impact the future viability of ACA policies and programs that impact our business, including, among others, Medicaid expansion, CMMI and the health insurance exchanges. For example, if an ACA repeal ends Medicaid expansion it could have an adverse impact on coverage available to our patients and if such a repeal impacts CMMI’s authority to implement innovative payment models, we may lose the investment of the resources we have dedicated to those programs. In addition, our revenue and operating income levels are highly sensitive to the percentage of our patients with higher-paying commercial health insurance and any legislative, regulatory or other changes that decrease the accessibility and availability, including the duration, of commercial insurance may have a material adverse impact on our business. The ACA's health insurance exchanges, which provide a marketplace for eligible individuals and small employers to purchase health insurance, initially increased the accessibility and availability of commercial insurance. In the event the exchange markets are significantly impaired as a result of legislative developments or other changes, it may adversely impact the percentage of our patients with higher-paying commercial health insurance, particularly if patients become unemployed due to factors related to the COVID-19 pandemic or otherwise and are unable to turn to the exchanges as an alternative to employer-based coverage.
Changes to the political environment resulting from the most recent election cycle may increase the likelihood of changes that would impact us, such as changes to the healthcare regulatory landscape or to the federal corporate tax rate. Examples of such potential changes could include, among other things, legislative developments or administrative decisions such as moving to a universal health insurance or "single payor" system whereby health insurance is provided to all Americans by the government, the availability of a “public health insurance option” similar to Medicare, government programs that impact access to Medicaid expansion or impact funding provided to families to purchase plans through the health insurance exchanges
or changes to the eligibility age for Medicare beneficiaries. Some of these and other related changes could in turn impact the percentage of our patients with higher-paying commercial health insurance, impact the scope or terms of coverage under commercial health plans and increase our expenses, among other things. The timing of any legislative or executive action related to these potential initiatives remains uncertain, particularly in light of the ongoing COVID-19 pandemic, and as such, considerableConsiderable uncertainty exists surrounding the continued development of the ACA and related regulations,healthcare regulatory environment including pilot programs and models, as well as similar healthcare reform measures and/or other changes that may be enactedto laws, regulations and other requirements at the federal and/or state level to laws, regulations and other requirements that govern our business.
Changes to the continuously evolving healthcare regulatory landscape may also have the potential to generate opportunities with relative ease of entry for certain different and/or non-traditional providers and we may be competing with them for patients in an asymmetrical environment with respect to reimbursement rates, data and/or regulatory requirements given our status as an ESRD service provider and relative scale. For example, CMS may consider opening for comment its established Medicare ESRD conditions for coverage. In the event that this process results in reductions or other changes in minimum health and safety standards for the provision of dialysis services, it may change the marketplace in which we operate. If we are unable to successfully adapt to these marketplace developments in a timely and compliant manner, we may experience a material adverse reduction in our overall number of patients, among other things. For additional detail on our evolving competitive environment, see the risk factor under the heading "If we are unable to compete successfully..." Broader changes to the regulatory landscape may also impact our business. For example, in January 2023, the Federal Trade Commission (FTC) proposed a new rule that would generally prohibit employers from using non-compete clauses in contracts with workers that extend beyond the termination of the employment or independent contractor relationship. It is unclear if and when a final rule will be issued and whether it would be subject to legal challenges. In addition, Congress and more than half of the states' legislatures introduced legislation in 2023 that would place some restrictions on non-compete agreements between employers and workers. While few of these states passed such legislation, it is possible that similar legislation could be introduced in 2024. We are monitoring these developments and any state follow-on regulations for any potential impact on our agreements with teammates, our arrangements with medical directors, joint venture operating agreements, or the terms of any of our existing agreements with physicians, among others, should any such legislation or regulation be finalized and implemented.
Although we cannot predict the short- or long-term effects of any legislative or regulatory changes, we believe that future market changes could result in, among other things, more restrictive commercial plans with lower reimbursement rates or higher deductibles and co-payments that patients may not be able to pay. ToBecause our revenue and operating income levels are highly sensitive to the extent that changes in statutes, regulations or related guidance or changes in other market conditions result in a reduction in the percentage and number of our patients with higher-paying commercial health insurance, any legislative, regulatory or other changes that decrease the accessibility and availability, including the duration, of commercial insurance limit the scope or nature of coverage through the exchanges or other health insurance programs or otherwise reduce reimbursement rates for our services from commercial and/or government payors, it couldis likely to have a material adverse effectimpact on our business, results of operations, financial condition and cash flows.business. For additional information on the impact of economic conditions or legislative or regulatory changes on the coverage and rates for our services and the percentage or number of our patients with
commercial insurance, see the risk factorsfactor under the headings "We continuously have ongoing negotiations with commercial payors, and if the average rates that commercial payors pay us decline significantly, if patients in commercial plans are subject to restriction in plan designs or if we are unable to maintain contracts with payors with competitive terms, including, without limitation, reimbursement rates, scope and duration of coverage and in-network benefits, it would have a material adverse effect on our business, results of operations, financial condition and cash flows," andheading "If the number or percentage of patients with higher-paying commercial insurance declines, it could have a material adverse effect on our business, results of operations, financial condition and cash flows.declines..."
The introduction of new or modified rules and regulations also generates continuous risks related to appropriate compliance. Changes to the continuously evolving healthcare regulatory landscape may also have the potential to generate opportunities with relative ease of entry for certain smaller and/or non-traditional providers and we may be competing with them for patients in an asymmetrical environment with respect to data and/or regulatory requirements given our status as an ESRD service provider. These opportunities may be enhanced by disruptions or changes to the healthcare regulatory landscape resulting from the ongoing global health crisis. For additional detail on our evolving competitive environment, see the risk factor under the heading "If we are unable to compete successfully, including, without limitation, implementing our growth strategy and/or retaining patients and physicians willing to serve as medical directors, it could materially adversely affect our business, results of operations, financial condition and cash flows." In general, if we are unable to efficiently and effectively adjust to new or modified rules and regulations, including with respect to regulatory compliance, it may, among other things, erode our patient base or reimbursement rates and could otherwise have a material adverse impact on our business, results of operation, financial condition and cash flows.
There have also been several state initiatives to limit payments to dialysis providers, or impose other burdensome operational requirements which, if passed,or prescribe wage levels. Depending on the extent of the limitations, burdens or prescriptions of such initiatives, the passage of such initiatives into law could have a material adverse impact on our business, results of operation, financial condition and cash flow. For instance, in 2020, voters inexample, California considered a statewide ballot initiative that sought to impose certain regulatory requirements on dialysis clinics, including requirements related to physician staffing levels, clinical reporting, clinical treatment options and limitations onrecently enacted California Senate Bill No. 525 (SB 525), which raises the ability to make decisions on closing or reducing servicesminimum wage for dialysis clinics. While this ballot initiative was rejected by voters in 2020, we incurred substantial costs to oppose it.many California healthcare workers, effective as of June 1, 2024. We may continue to face ballot initiatives or other proposed regulations or legislation or ballot initiatives in California or othervarious states in future years, which may require us to incur further substantial costs and which, if passed, could have a material adverse impact on our business, results of operations, financial condition and cash flows.
Finally, there have also been rule making and legislative efforts at both the federal and state level regarding the use of charitable premium assistance for ESRD patients and may establish new conditions for coverage standards for dialysis facilities.patients. For example, on October 13, 2019, a California bill (AB 290) was signed into law that limits the amount of reimbursement paid to certain providers for services provided to patients with commercial insurance who receive charitable premium assistance. The American Kidney Fund (AKF), an organization that provides charitable premium assistance announced that it would be withdrawing from California as a result of AB 290.(reimbursement cap). The implementation of AB 290 has been stayed pending resolution of legal challenges. The trial court recently issued a decision relating to these challenges butto AB 290 that may result in the stay being lifted and at least some provisions of the law being implemented in the near future, although any appeal of the decision may result in the stay being continued. While it is currently unclear when and how those provisions may be implemented, in the event certain provisions of AB 290 becomes effective andare implemented in their proposed form, including the AKF withdraws from California,reimbursement cap, it may cause otherhave a negative consequence on our business. Depending on what provisions are implemented, organizations that provide charitable premium assistance may choose to withdraw from California, and wewhich would expecthave an adverse impact on the ability of patients to afford Medicare premiums and Medicare supplemental and commercial coverage. We expect that such an adverse impact will in turn adversely impact our business, results of operations, financial condition and cash flows. BillsIn the past, bills similar to AB 290 werehave been introduced in Illinois (SB 600) and Oregon (SB 900) in 2019,other states, but have not been successfully passed to date.none has become law. If these or similar bills are introduced and implemented in other jurisdictions, and organizations that provide charitable premium assistance in those jurisdictions are similarly impacted, it could in the aggregate have a material adverse impact on our business, results of operations, financial condition and cash flows. For additional information on risks associated with charitable premium assistance for ESRD patients and the potential impact of
decreases to the percentage or number of our patients with commercial insurance, see the risk factor under the heading "If the number or percentage of patients with higher-paying commercial insurance declines, it could have a material adverse effect on our business, results of operations, financial condition and cash flows".declines..."
Among other things, legislation, regulations, regulatory guidance, proposed legislation and ballot initiatives and any similar initiatives could result in a reduction in the percentage of our patients with commercial insurance; limit the scope or nature of coverage through the healthcare exchanges established by the ACA or other health insurance programs or otherwise reduce reimbursement rates for our services from commercial and/or government payors; restrict or prohibit the ability of patients with access to alternative coverage from selecting a marketplace plan on or off exchange,exchange; limit the amount of revenue that a dialysis provider can retain for caring for patients with commercial insurance,insurance; impose burdensome operational requirements,requirements; affect payments made to providers for services provided to patients who receive charitable premium assistance and/or otherwise restrict or prohibit the use of charitable premium assistance,assistance; or reduce the standards for network adequacy.adequacy or require disclosure of certain pricing and patient responsibility information. In turn, these potential impacts could cause us to incur substantial costs to oppose any such proposed requirements or measures, impact our dialysis center development plans, and if passed and/or implemented, could materially reduce our revenues and increase our operating and other costs, adversely impact dialysis centers across the U.S. making certain centers economically unviable, lead to the closure of certain centers, restrict the ability of dialysis patients to obtain and maintain optimal insurance coverage and reduce the number of patients that select commercial insurance plans or MA plans for their dialysis care, among other things.
Evolving For additional details regarding insurance coverage for dialysis services, see the discussion in the risk factor under the heading "If the number or percentage of patients with higher-paying commercial insurance declines..." The healthcare legislative and regulatory environment is dynamic and evolving, and any such proposed or issued laws, requirements, rules and guidance thatcould impact our business, including as may be described above, and any failure on our part to adequately adjust to any resulting marketplace developments or regulatory compliance requirements, may, among other things, erode our patient base or reimbursement rates and could otherwise have a material adverse effect on our business, results of operations, financial condition and cash flows.
To the extent that the information above describes statutory and regulatory provisions, it is qualified in its entirety by reference to the particular statutory and regulatory provisions that are referenced. For additional information related to the laws, rules and other regulations described above, please see Part I Item 1 “Business–Government Regulation”1. Business of this Form 10-K.10-K under the heading "Government Regulation."
We are, and may in the future be, a party to various lawsuits, demands, claims, qui tam suits, governmental investigations and audits and other legal matters, any of which could result in, among other things, substantial financial penalties or awards against us, mandated refunds, substantial payments made by us, required changes to our business practices, exclusion from future participation in Medicare, Medicaid and other healthcare programs and possible criminal penalties, any of which could have a material adverse effect on our business, results of operations, financial condition, cash flows, reputation and stock price.
We are, and may in the future be, subject to investigations and audits by governmental agencies and/or private civil qui tam complaints filed by relators and other lawsuits, demands, claims, and legal proceedings and/or other actions, including, without limitation, investigations or other actions resulting from our obligation to self-report certain suspected violations of law.
Any allegations against us, our personnel or our representatives in such matters may among other things harm our reputation, stock price, and our various business relationships and/or contracts related to our business, and these impacts may be material. Responding to subpoenas, investigations and other lawsuits, claims and legal proceedings, as well as defending ourselves in such matters, will continue to require management's attention and cause us to incur significant legal expense. Negative developments, findings or terms and conditions that we might agree to accept as part of a negotiated resolution of pending or future legal or regulatory matters could result in, among other things, harm to our reputation, substantial financial penalties or awards against us, substantial payments made by us, harm to our reputation, required changes to our business practices, impacts on our various relationships and/or contracts related to our business, exclusion from future participation in Medicare, Medicaid and other healthcare programs and, in certain cases, criminal penalties, any of which could have a material adverse effect on us. It is possible that criminal proceedings may be initiated against us and/or individuals in our business in connection with governmental investigations. Other than as may be described in Note 1615 to the consolidated financial statements included in this report, we cannot predict the ultimate outcomes of the various legal proceedings and regulatory matters to which we are or may be subject from time to time, or the timing of their resolution or the ultimate losses or impact of developments in those matters, which could have a material adverse effect on our business, results of operations, financial condition, cash flows, reputation and stock price. See Note 1615 to the consolidated financial statements included in this report for further details regarding these and other legal proceedings and regulatory matters.
If the number or percentage of patients with higher-paying commercial insurance declines, if the average rates that commercial payors pay us decline, if commercial plans subject patients to restriction in plan designs, or if we are unable to maintain contracts with payors with competitive terms, including, without limitation, reimbursement rates, scope and duration of coverage and in-network benefits, it could have a material adverse effect on our business, results of operations, financial condition and cash flows.
A substantial portion of our U.S. dialysis patient service revenues are generated from patients who have commercial payors as their primary payor. The majority of these patients have insurance policies that pay us on terms and at rates that are generally significantly higher than Medicare rates. As such our revenue and net income levels are sensitive to the number of our patients with higher-paying commercial insurance coverage and the percentage of our patients under higher-paying commercial plans relative to government-based programs. The payments we receive from commercial payors generate nearly all of our profit and all of our nonacute dialysis profits come from commercial payors.
When traditional or original Medicare (Medicare) becomes the primary payor for a patient, the payment rate we receive for that patient decreases from the employer group health plan or commercial plan rate to the lower Medicare payment rate. If the number of our patients who have Medicare or another government-based program as their primary payor increases, it could negatively impact the percentage of our patients covered under commercial insurance plans. There are a number of factors that could drive a decline in the number or percentage of our patients covered under commercial insurance plans, including, among other things, improved mortality, changes in the patient's or a family member's employment status, reduced availability of commercial health plans or reduced coverage by such plans through the ACA exchanges or otherwise due to changes to the laws, marketplace, healthcare regulatory system or otherwise. Commercial payors could also cease paying in the primary position after providing 30 months of coverage resulting in potentially material reductions in payment as the patient moves to Medicare primary. Declining macroeconomic conditions could also negatively impact the percentage of our patients covered under commercial insurance plans. To the extent there are job losses in the U.S., we could experience a decrease in the number of patients covered under commercial plans and/or an increase in uninsured and underinsured patients independent of whether general economic conditions improve. If we experience higher numbers of uninsured or underinsured patients, it also would result in an increase in uncollectible accounts.
Our arrangements and negotiations with payors also impact the number or percentage of patients with higher-paying commercial insurance. We continuously are in the process of negotiating existing and potential new agreements with commercial payors who aggressively negotiate terms with us, and we can make no assurances about the ultimate results of these negotiations or the timing of any potential rate changes resulting from these negotiations. A material portion of both our commercial revenue and MA revenue is concentrated with a limited number of commercial payors, and any changes impacting
our highest paying commercial payors or our relationships with these payors will have a disproportionate impact on us. Sometimes many significant agreements are being renegotiated at the same time. We believe payor consolidations have significantly increased the negotiating leverage of commercial payors, and ongoing consolidations may continue to increase this leverage in the future. In addition, our agreements and rates with commercial payors may be impacted by new business activities of these commercial payors as well as steps that these commercial payors have taken and may continue to take to control the cost of and/or the eligibility for access to the services that we provide, including, without limitation, relative to products on and off the healthcare exchanges. These efforts could impact the number of our patients who are eligible to enroll in commercial insurance plans, and remain on the plans, including plans offered through healthcare exchanges. We continue to experience downward pressure on some of our rates with commercial payors as a result of these and other general conditions in the market, including, among other things, as employers seek to shift to less expensive options for medical services or as commercial payors dedicate increased focus on dialysis services.
Our negotiations with commercial payors may relate to commercial fee-for-service contracts, value-based care (VBC) contracts in which we share risk with commercial payors or other structures that allow the parties to share in cost savings upon the achievement of certain outcomes, as well as contracts to provide dialysis services to MA patients. If we fail to maintain contracts with payors and other healthcare providers with competitive or favorable terms, either with respect to commercial plans, commercial VBC contracts, MA plans or otherwise, including, without limitation, with respect to reimbursement rates, scope and duration of coverage and in-network benefits, contract term or termination rights, or if we fail to accurately estimate the price for and manage our medical costs in an effective manner, whether due to inflationary pressures or otherwise, such that the profitability of our commercial or other value-based products is negatively impacted, it could have a material adverse effect on our business, results of operations, financial condition and cash flows. The ultimate result of our negotiations with payors cannot be predicted as they occur in a highly competitive environment and are influenced by changes to payment rates set by CMS and other marketplace dynamics such as those previously discussed. Among other things, these negotiations may result in termination or non-renewals of existing agreements, decreases in contracted rates, and reduction in the number of our patients that are covered by commercial plans, and we may not be able to enter into new agreements on competitive terms or at all. In the event that our ongoing negotiations with commercial payors result in overall rate reductions in excess of overall rate increases, the cumulative effect could have a material adverse effect on our business, results of operations, financial condition and cash flows. In addition, to the extent that these negotiations result in a reduction in the number of our patients covered by plans with commercial payors, it could have a material adverse effect on our business, results of operations, financial condition and cash flows.
Certain payors have been attempting to design and implement plans that restrict or limit coverage for treatment needed by ESRD patients in the commercial market. Among other things, these restrictive plan designs seek to limit the duration and/or the breadth of ESRD benefits, limit in-network providers, set arbitrary provider reimbursement rates, or otherwise restrict access to care, all of which may result in a decrease in the number of patients covered by commercial insurance or the reimbursement rate for ESRD services, among other things. Payors have also disputed the scope and duration of ESRD benefit coverage under their plans, and, among other things, have required patients to seek Medicare coverage for ESRD treatments. On June 21, 2022, the U.S. Supreme Court issued a decision in the matter of Marietta Memorial Hospital Employee Health Benefit Plan, et al. v. DaVita Inc., et al., a case evaluating the scope of the Medicare Secondary Payor Act (MSPA), deciding that a group health plan that limits the benefits for outpatient dialysis, but does so uniformly for all plan participants, does not violate the terms of the MSPA because the plan treats all patients uniformly, regardless of whether a participant has ESRD and regardless of whether the participant is eligible for Medicare. We cannot reasonably estimate the ultimate impact of the U.S. Supreme Court’s decision at this time, as there is significant uncertainty as to, among other things, whether and to what extent payors, including, among others employer group health plans, may seek to design and implement plans to restrict access to ESRD in light of the decision; the results of proposed and pending legislative and regulatory responses to the decision; how courts will interpret other anti-discriminatory provisions of the MSPA that may apply; whether there could be other potential negative impacts of the decision and any resultant plan behavior on our commercial or government mix or the number of our patients covered by commercial insurance; and the timing of each of these items. If more commercial or employer group health plans seek to implement or utilize plan designs that discourage or prevent ESRD patients from retaining their commercial coverage, during upcoming open enrollment periods or otherwise, it may lead to a decrease in the number of patients with commercial plans, the duration of benefits for patients under commercial plans and/or a decrease in the payment rates we receive, any of which could have a material adverse effect on our business, results of operations, financial condition and cash flows.
In addition, some commercial payors are pursuing or have incorporated policies into their provider manuals limiting or refusing to accept charitable premium assistance from non-profit organizations, such as the AKF, which may impact the number of patients who are able to afford commercial plans. Paying for coverage is a significant financial burden for many patients, and ESRD disproportionately affects the low-income population. Charitable premium assistance supports continuity of coverage and access to care for patients, many of whom are unable to continue working full-time as a result of their severe
health condition. Many patients with commercial and government insurance also rely on financial assistance from charitable organizations, such as the AKF. Certain payors have challenged our patients' and other providers' patients' ability to utilize assistance from charitable organizations for the payment of premiums, including, without limitation, through litigation and other legal proceedings. The use of charitable premium assistance for ESRD patients has also faced challenges and inquiries from legislators, regulators and other governmental authorities, including California AB 290 as described in the risk factor under the heading, "Changes in federal and state healthcare legislation or regulations...", and this may continue. In addition, CMS or another regulatory agency or legislative authority may issue a new rule or guidance that challenges or restricts charitable premium assistance. If any of these challenges to kidney patients' use of premium assistance is successful or restrictions are imposed on the use of financial assistance from such charitable organizations or if organizations providing such assistance are no longer available such that kidney patients are unable to obtain, or continue to receive or receive for a limited duration, such financial assistance, it may restrict the ability of dialysis patients to obtain and maintain optimal insurance coverage and could have a material adverse effect on our business, results of operations, financial condition and cash flows. In addition, if our assumptions about how kidney patients will respond to any change in financial assistance from charitable organizations are incorrect, it could have a material adverse effect on our business, results of operations, financial condition and cash flows.
Our negotiations and relationships with payors may also be impacted by legislative or regulatory developments and associated legal rulings. For example, the final rules for the Cures Act, which are described in detail in Part I Item 1. Business of this Form 10-K under the heading "Government Regulation—21st Century Cures Act,"broadened ESRD patient access to certain enhanced benefits offered by MA plans. While these rules increased our MA plan enrollment for ESRD benefits in their first year, the potential ultimate impact of this change in benefit eligibility remains subject to change as market participants continue to adjust to this new regulatory environment, including such changes as, for example, the removal of objective time and distance standards for network adequacy for outpatient dialysis centers. In addition, recent price transparency regulations require most group health plans and health insurance issuers in the group and individual markets to make certain pricing and patient responsibility information publicly available. For additional details regarding these regulations and potential legislative or regulatory changes, the specific risks we face in connection with any decrease in payments we receive for services due to, for example, fewer patients being covered under commercial plans or an increase of patients covered under more restrictive commercial plans, or plans with lower reimbursement rates, please see Part I Item 1. Business of this Form 10-K under the heading "Government Regulation" and the discussion in the risk factor under the heading "Changes in federal and state healthcare legislation or regulations..."
In addition to the aforementioned pricing transparency rules, the government has also implemented certain additional pricing transparency requirements that apply to certain types of providers, including DaVita. Under the No Surprises Act, which went into effect January 1, 2022, certain providers, including DaVita, are required to develop and disclose a "Good Faith Estimate" (GFE) that details the expected charges for furnishing an item or service to an uninsured or self-pay patient. The GFE must include specific information regarding the service provided and diagnostic codes, among other things, and is subject to formatting requirements, notice requirements, availability and dispute resolution procedures. Similar to the aforementioned pricing transparency rules, the impact of the GFE requirements on DaVita remains uncertain at this time, in part due to ongoing rulemaking around the No Surprises Act as well as the delayed effective date of certain provisions of the GFE framework, and uncertainty around operational timeframes, potential penalties and patient reaction, among other things. Patient dissatisfaction with the GFE process, whether with respect to the GFE rate or charges, how such charges are communicated or otherwise, may impact patient choices and over time could have a material adverse impact on our business, results of operations and financial condition, and could materially harm our reputation.
As noted, the foregoing dynamics of our arrangements and negotiations with commercial payors each may have an impact on, among other things, our ability to enter into and maintain contracts with payors with competitive terms, including, without limitation, reimbursement rates, scope and duration of coverage and in-network benefits as well as the number or percentage of our patients with higher-paying commercial insurance. If, as a result of these or other dynamics, we experience a decline in the average rates that commercial payors pay us or a reduction in the number of patients with ESRD coverage under higher-paying commercial plans either in total or relative to the number of patients under government-based programs that pay at lower rates or an increase in the number of patients that are uninsured or underinsured, it could have a material adverse effect on our business, results of operations, financial condition and cash flows.
If we are not able to successfully implement our strategy with respect to our integrated kidney care and value-based care initiatives, including maintaining our existing business and further developing our capabilities in a complex and highly regulated environment, it could result in a loss of our investments and have a material adverse effect on our growth strategy, could adversely impact our business, results of operations, financial condition and cash flows, and could materially harm our reputation.
Our integrated kidney care business manages patients and coordinates their care through value-based care arrangements with commercial payors and through government programs. We have continued to grow this portion of our business both with commercial payors, including as MA has expanded, and with government programs as CMS and CMMI implement new payment models focused on comprehensive and integrated kidney care. As part of our growth strategy, we have invested and expect to continue to invest substantial resources in the further development of our integrated care business and value-based care initiatives. There can be no assurances that we will be able to successfully implement our strategies with respect to integrated kidney care and value-based care in a complex, evolving and highly competitive and regulated environment, including, among other things, maintaining our existing business; recovering our investments; entering into agreements with payors, physicians, third party vendors and others on competitive terms, as appropriate, that prove actuarially sound; structuring these agreements and arrangements to comply with evolving rules and regulations, including, among other things, rules and regulations related to fraud and abuse and the use of protected health information. Implementing our expanded integrated kidney care strategies and value-based care initiatives at scale also increases certain execution and compliance risks associated with developing our operational, IT, billing and telehealth systems, including our ability to accurately capture relevant patient care data, among other things. For additional details on risks associated with information systems and new technology generally, see the risk factor under the heading "Failing to effectively maintain, operate or upgrade our information systems or those of third-party service providers upon which we rely..."
New entrants are aggressively pursuing opportunities to participate in the new CMMI payment models as well as broader risk arrangements with other payors, and with increasing investment and funding, these new entrants may adopt strategies that increase our costs to participate in these payment models and/or adversely impact our ability to enter into competitive arrangements with payors, physicians and hospitals. For additional detail on our evolving competitive environment, see the risk factor under the heading "If we are unable to compete successfully..." If any of these or other of our integrated kidney care and value-based care initiatives are unsuccessful, it could result in a loss of our investments and have a material adverse effect on our growth strategy, could adversely impact our business, results of operations, financial condition and cash flows, and could materially harm our reputation.
In addition, future legislative or regulatory action related to, among other things, existing or future integrated kidney care initiatives, including among others, CMMI payment models, and/or full capitation demonstration for ESRD may impact our ability to provide a competitive and successful integrated care program at scale. There can be no assurances that any other legislation or regulation that aligns with our strategy and investments will be extended, passed into law or enacted. Additionally, the ultimate terms and conditions of any potential legislative or regulatory action impacting integrated kidney care, full capitation demonstrations or the existing CMMI payment models remain unclear. For example, the CKCC program is a 5-year demonstration that launched in 2022. CMMI continues to monitor the performance of these and other kidney care payment models, and there is no assurance that this program will be extended or modified in the future and, among other things, our costs of care could exceed our associated reimbursement rates under such legislation. Irrespective of whether such laws are passed or regulations enacted, there can be no assurances that we will be able to successfully execute on the required strategic initiatives that would allow us to maintain a competitive and successful integrated care program on a broad scale, and in the desired time frame. Any failure on our part to adequately implement strategic initiatives to adjust to any marketplace developments resulting from executive, legislative, regulatory or administrative changes could have a material adverse impact on our business.
If we are not able to successfully implement our strategy with respect to home-based dialysis, including maintaining our existing business and further developing our capabilities in a complex and highly regulated environment, it could have a material adverse effect on our business, results of operations, financial condition and cash flows, and could materially harm our reputation.
Our home-based dialysis services, which include home hemodialysis and peritoneal dialysis (PD), represented approximately 18% of our U.S. dialysis patient service revenues for the year ended December 31, 2023, and have increasingly become an important part of our overall strategy. In addition, home-based dialysis recently has been the subject of increased political and industry focus. For example, in connection with the 2019 Executive Order, HHS set out specific goals related to home dialysis and CMMI’s ESRD Treatment Choices (ETC) mandatory payment model and voluntary payment models included new incentives to encourage dialysis at home. More recently, CMS finalized changes to the ETC model and other regulations to encourage dialysis facilities and healthcare providers to seek to decrease disparities in health equity across racial and socioeconomic status in rates of home dialysis and kidney transplants among ESRD patients. CMS continues to propose
modifications to the ETC model and evaluate the model against the agency's stated goals for the program. We are a leader in home-based dialysis and have made investments in processes and infrastructure to continue to grow this modality. There are, however, risks associated with this growth, including, among other things, financial, legal, regulatory and operational risks related to our ability to design and develop infrastructure and to plan for capacity in a modality that is part of an evolving marketplace. For example, the OIG recently issued its 2024 work plan identifying its interest in auditing home dialysis programs. We may also be subject to associated risks related to our ability to successfully manage related operational initiatives, find, train and retain appropriate staff, contract with payors for appropriate reimbursement, and maintain processes to adhere to the complex regulatory and legal requirements, including without limitation those associated with billing Medicare. For additional detail on risks associated with operating in a highly regulated environment, see the risk factor under the heading "Our business is subject to a complex set of governmental laws, regulations and other requirements..." In addition to the above risks, certain risks inherent to home-based dialysis will increase as we expand our home-based dialysis offerings, including risks related to managing transitions between in-center and home-based dialysis, billing and telehealth systems, among others. For additional detail on risks associated with information systems and new technology generally, see the risk factor under the heading "Failing to effectively maintain, operate or upgrade our information systems or those of third-party service providers upon which we rely..."
An increased focus on home-based dialysis is also indicative of the generally evolving market for kidney care. This developing market may create additional opportunities for competition with relative ease of entry, and if we are unable to successfully adapt to these or other marketplace developments, which, among other things, may include regulatory changes with respect to conditions of coverage, in a timely and compliant manner, we may experience a material adverse impact on our growth in home-based dialysis or a reduction in our overall number of patients, among other things. For additional detail on the competitive landscape in kidney care, see the risk factor under the heading "If we are unable to compete successfully..." If we are not able to successfully implement our strategy with respect to home-based dialysis, including maintaining our existing business and further developing our capabilities in a complex and highly regulated environment, it could have a material adverse effect on our business, results of operations, financial condition and cash flows, and could materially harm our reputation.
Changes in the structure of and payment rates under the Medicare ESRD or Medicare Advantage programs or changes in state Medicaid or other non-Medicare government-based programs or payment rates could have a material adverse effect on our business, results of operations, financial condition and cash flows.
A substantial portion of our dialysis revenues are generated from patients who have Medicare as their primary payor. For patients with Medicare coverage, all ESRD payments for dialysis treatments are currently made under a single bundled payment rate which provides a fixed payment rate to encompass all goods and services provided during the dialysis treatment that are related to the treatment of dialysis, subject to certain adjustments as described below. Most lab services are also included in the bundled payment.
Under the ESRD Prospective Payment System (PPS), bundled payments to a dialysis facility may be reduced by as much as 2% based on the facility's performance in specified quality measures set annually by CMS through the ESRD Quality Incentive Program, which was established by the Medicare Improvements for Patients and Providers Act of 2008. The bundled payment rate is also adjusted for certain patient characteristics, a geographic usage index and certain other factors. In addition, the ESRD PPS is subject to rebasing, which can have a positive financial effect, or a negative one if the government fails to rebase in a manner that adequately addresses the costs borne by dialysis facilities. Similarly, as new drugs, services or labs are added to the ESRD bundle, CMS' failure to adequately calculate or fund the costs associated with the drugs, services or labs could have a material adverse effect on our business, results of operations, financial condition and cash flows. In certain instances, new injectable, intravenous or oral products may be reimbursed separately from the bundled payment for a defined period of time through a transitional drug add-on payment adjustment (TDAPA). For a discussion of certain risks associated with this transitional pricing process, see the risk factor under the heading, "Changes in clinical practices, payment rates or regulations impacting pharmaceuticals and/or devices..."
The current bundled payment system presents certain operating, clinical and financial risks, which include, without limitation:
•Risk that our reimbursement rates are reduced by CMS or are otherwise inadequate. CMS publishes a final rule for the ESRD PPS each year and uncertainty about future payment rates remains a material risk to our business.
•Risk that CMS, on its own or through its contracted Medicare Administrative Contractors (MACs) or otherwise, implements Local Coverage Determinations (LCDs) or implements payment provisions, policy or regulatory mandates, including changes to the existing or future PPS, that limit our ability to either be paid for covered dialysis services or bill for treatments or other drugs and services or other rules that may impact reimbursement. Such payment
rules and regulations and coverage determinations or related decisions could have an adverse impact on our operations and revenue. There is also risk that commercial insurers could seek to incorporate the requirements or limitations associated with such LCDs or CMS guidance into their contracted terms with dialysis providers, which could have an adverse impact on our revenue.
•Risk that a MAC, or multiple MACs, change their interpretations of existing regulations, manual provisions and/or guidance, or seek to implement or enforce new interpretations that are inconsistent with how we have interpreted existing regulations, manual provisions and/or guidance.
•Risk that CMS implements data and related reporting requirements that result in decreased reimbursement and/or increased technology and operational costs.
•Risk that increases in our operating costs will outpace the Medicare rate increases we receive. We expect operating costs to continue to increase due to inflationary factors, such as increases in labor and supply costs, including, without limitation, increases in maintenance costs and capital expenditures to improve, renovate and maintain our facilities, equipment and information technology to meet changing regulatory requirements and business needs, regardless of whether there is a compensating inflation-based increase in Medicare payment rates or in payments under the bundled payment rate system.
•Risk of continued federal budget sequestration cuts or other disruptions in federal government operations and funding. As a result of the Budget Control Act of 2011, the Bipartisan Budget Act (BBA) and subsequent legislation, an annual reduction (currently 2%) to Medicare payments took effect on April 1, 2013, and has been extended through 2032. These across-the-board spending cuts have affected and will continue to adversely affect our business, results of operations, financial condition and cash flows. Any extended disruption in federal government operations and funding, including an extended government shutdown, U.S. government debt default and/or failure of the U.S. government to enact annual appropriations could have a material adverse effect on our business, results of operations, financial condition and cash flows. Additionally, disruptions in federal government operations may delay or negatively impact regulatory approvals and guidance that are important to our operations, and create uncertainty about the pace of upcoming regulatory developments.
•Risk that failure to adequately develop and maintain our clinical or other operational systems or failure of our clinical or operational systems to operate effectively could have a material adverse effect on our business, results of operations, financial condition and cash flows. For example, in connection with claims for which at least part of the government's payments to us is based on clinical performance or patient outcomes or co-morbidities, if our clinical systems fail to accurately capture the data we report to CMS or we otherwise have data integrity issues with respect to the reported information, we might be over-reimbursed by the government, which could, among other things, subject us to liability exclusion from participation in federal healthcare programs and penalties under the federal Civil Monetary Penalty statute, and could adversely impact our reputation.
•Risk of ensuring that we remain complaint with MA marketing requirements as well as our contractual terms with associated plans, as our initiatives associated with MA (including chronic condition special needs and dual eligible special needs plans) continue to evolve and progress. Failure to do so could resolve in termination of agreements with plans as well as enforcement by state and federal agencies for violation of insurance, consumer and fraud and abuse laws and regulations.
We are subject to similar risks for services billed separately from the ESRD bundled payment, including, without limitation, the risk that a MAC, or multiple MACs, change their interpretations of existing regulations, manual provisions and/or guidance; or seek to implement or enforce new interpretations that are inconsistent with how we have interpreted existing regulations, manual provisions and/or guidance.
In addition to the above risks under the current Medicare ESRD program, changing legislation and other regulatory and executive developments have led and may continue to lead to the emergence of new models of care and other initiatives in both the government and private sector that, among other things, may impact the structure of, and payment rates under, the Medicare ESRD program. Moreover, the number of our patients with primary Medicare coverage may be subject to change, particularly with the effectiveness of the Cures Act, which allows Medicare-eligible individuals with ESRD to enroll in MA managed care plans. For additional details regarding the risks we face for failing to adhere to our Medicare and Medicaid regulatory compliance obligations or failing to adequately implement strategic initiatives to adjust to marketplace developments, see the risk factors above under the headings "Our business is subject to a complex set of governmental laws, regulations and other requirements...;" and "Changes in federal and state healthcare legislation or regulations..."
Primary coverage for a significant number of our patients also comes from state Medicaid programs partially funded by the federal government as well as other non-Medicare government-based programs, such as coverage through the Department of Veterans Affairs (VA). As state governments and other governmental organizations face increasing financial hardship and budgetary pressure, including as a result of the COVID-19 pandemic or changes in the political environment, we may in turn face reductions in payment rates, delays in the receipt of payments, limitations on enrollee eligibility or other changes to the applicable programs. For example, certain state Medicaid programs and the VA have recently considered, proposed or implemented payment rate reductions, such as the VA's adoption of Medicare's bundled PPS pricing methodology for any veterans receiving treatment from non-VA providers under a national contracting initiative. Since we are a non-VA provider, these reimbursements are tied to a percentage of Medicare reimbursement, and we have exposure to any dialysis reimbursement changes made by CMS. Approximately 3% of our U.S. dialysis patient service revenues for the year ended December 31, 2023 were generated by the VA. In addition, in 2019, we entered into a Nationwide Dialysis Services contract with the VA that includes five separate one-year renewal periods throughout the term of the contract. The term structure is similar to our prior five-year agreement with the VA, and is consistent with VA practice for similar provider agreements. With this contract award, the VA has agreed to keep our percentage of Medicare reimbursement consistent with that under our prior agreement with the VA during the term of the contract. As with that prior agreement, this agreement provides the VA with the right to terminate the agreements without cause on short notice, among other things. This contract expires at the end of 2024. Should the VA renegotiate, not renew or cancel these agreements for any reason, we may cease accepting patients under this program and may be forced to close centers or experience lower reimbursement rates, which could have a material adverse effect on our business, results of operations, financial condition and cash flows.
State Medicaid programs are increasingly adopting Medicare-like bundled payment systems, but sometimes these payment systems are poorly defined and are implemented without any claims processing infrastructure, or patient or facility adjusters. If these payment systems are implemented without any adjusters and claims processing infrastructure, Medicaid payments will be substantially reduced and the costs to submit such claims may increase, which will have a negative impact on our business, results of operations, financial condition and cash flows. In addition, some state Medicaid program eligibility requirements mandate that citizen enrollees in such programs provide documented proof of citizenship. If our patients cannot meet these proof of citizenship documentation requirements, they may be denied coverage under these programs, resulting in decreased patient volumes and revenue. These Medicaid payment and enrollment changes, along with similar changes to other non-Medicare government programs, could reduce the rates paid by these programs for dialysis and related services, delay the receipt of payment for services provided and further limit eligibility for coverage which could have a material adverse effect on our business, results of operations, financial condition and cash flows.
Our business is labor intensive and if our labor costs continue to rise, including due to shortages, changes in certification requirements and/or higher than normal turnover rates in skilled clinical personnel; or currently pending or future governmental laws, rules, regulations or initiatives impose additional requirements or limitations on our operations or profitability; or, if we are unable to attract and retain employees; or if union organizing activities or legislative or other changes result in significant increases in our operating costs or decreases in productivity, we may experience disruptions in our business operations and increases in operating expenses, among other things, any of which could have a material adverse effect on our business, results of operations, financial condition, cash flows and reputation.
We face increasing labor costs generally, and in particular, we continue to face increased labor costs and difficulties in hiring nurses due to a nationwide shortage of skilled clinical personnel that has been exacerbated by current macroeconomic conditions and developments in the labor market. As referenced above, the current labor market is challenging and continues to experience volatility, uncertainty and labor supply shortages, particularly in healthcare. Our business is labor intensive, and our financial and operating results have been and continue to be sensitive to variations in labor-related costs, productivity and the number of pending or potential claims against us related to labor and employment practices. We have incurred and expect to continue to incur increased labor costs and experience staffing challenges, the ultimate extent of which will depend on current macroeconomic conditions and ancillary impacts on the labor market, among other things. For additional discussion of the risks facing us related to the current labor environment, see the risk factor under the heading "Macroeconomic conditions and global events..."Additionally, to the extent that general inflationary pressures continue or further increase, this may in turn increase our labor and supply costs at a rate that outpaces the Medicare or any other rate increases we may receive.
We compete for nurses with hospitals and other healthcare providers. The ongoing nursing shortage may limit our ability to expand our operations. Furthermore, changes in certification requirements can impact our ability to maintain sufficient staff levels, including to the extent our teammates are not able to meet new requirements, among other things. In addition, if we experience a higher than normal turnover rate for our skilled clinical personnel, our operations and treatment growth may be negatively impacted, which could adversely affect our business, results of operations, financial condition and cash flows. For example, in 2023, we again had significant teammate turnover, which led to increased training costs, among other things. We also face competition in attracting and retaining talent for key leadership positions. If we are unable to attract and retain qualified individuals, we may experience disruptions in our business operations, including, without limitation, our ability to
achieve strategic goals, which could have a material adverse effect on our business, results of operations, financial condition, cash flows and reputation.
Political or other efforts at the national or local level could result in actions or proposals that increase the likelihood of success of union organizing activities at our facilities and ongoing union organizing activities at our facilities could continue or increase for other reasons. Recently, certain of our competitors have experienced union organizing activities, including the filing of petitions by unions at certain of their clinics, with a number of these clinics voting to unionize. While no such petitions have been filed at our dialysis clinics to date, there can be no assurance that such petitions may not be filed in the future or that such petitions, if filed, will not be successful. If a significant portion of our teammates were to become unionized, we could experience, among other things, an upward trend in wages and benefits and labor and employment claims, including, without limitation, the filing of class action suits, or adverse outcomes of such claims; face work stoppages or other business disruptions; or experience negative impacts on our employee culture. In addition, we are and may continue to be subject to targeted corporate campaigns by union organizers in response to which we have been and expect to continue to be required to expend substantial resources, both time and financial. Any of these events or circumstances, including our responses to such events or circumstances, could have a material adverse effect on our employee relations, treatment growth, productivity, business, results of operations, financial condition, cash flows and reputation.
Privacy and information security laws are complex, and if we fail to comply with applicable laws, regulations and standards, including with respect to third-party service providers that utilize sensitive personal information on our behalf, or if we fail to properly maintain the integrity of our data, protect our proprietary rights to our systems or defend against cybersecurity attacks, we may be subject to government or private actions due to privacy and security breaches or suffer losses to our data and information technology assets, any of which could have a material adverse effect on our business, results of operations, financial condition and cash flows or materially harm our reputation.
We must comply with numerous federal and state laws and regulations in both the U.S. and the foreign jurisdictions in which we operate governing the collection, dissemination, access, use, security and privacy of PHI, including, without limitation, HIPAA and its implementing privacy, security, and related regulations, as amended by the federal Health Information Technology for Economic and Clinical Health Act (HITECH) and collectively referred to as HIPAA. We are also required to report known breaches of PHI and other certain personal information consistent with applicable breach reporting
requirements set forth in applicable laws and regulations. From time to time, we may be subject to both federal and state inquiries or audits related to HIPAA, HITECH and other state privacy laws associated with complaints, desk audits, and data breaches. Requirements under HIPAA also continue to evolve. If we fail to comply with applicable privacy and security laws, regulations and standards, including with respect to third-party service providers that utilize sensitive personal information, including PHI, or financial information or payroll data on our behalf or with respect to the use of certain third-party digital advertising technologies, or if we fail to properly maintain the integrity of our data, protect our proprietary rights, or defend against cybersecurity attacks, it could materially harm our reputation and/or have a material adverse effect on our business, results of operations, financial condition and cash flows. These risks may be intensified to the extent that the laws change or to the extent that we increase our use of third-party service providers that utilize sensitive personal information, including PHI, on our behalf.
Data protection laws are evolving globally, and may continue to add additional compliance costs and legal risks to our international operations. In Europe, the General Data Protection Regulation (GDPR) imposes a comprehensiveFor more details on certain international data protection regimelaws and regulations affecting our business, see Part I Item 1. Business of this Form 10-K under the heading "Government Regulation." The costs of compliance with, the potential for regulatory fines as well as data breach litigationand other burdens imposed by impacted data subjects. Under the GDPR, regulatory penalties may be assessed bythese international data protection authorities for up tolaws and regulations including, among others, the greater of 4% of worldwide turnoverEU GDPR and the UK GDPR, and other new laws, regulations and policies implementing these regulations may impact our international operations and may limit the ways in which we can provide services or €20 million.use personal data collected while providing services.
DataPrivacy and data protection laws are also evolving nationally, providing for enhanced state privacy rights that are broader than the current federal privacy rights, and may add additional compliance costs and legal risks to our U.S. operations. For example, the California Consumer Privacy Act (CCPA) and California Privacy Rights Act (CPRA) have been passed into law in the past several years, and they collectively expand our obligations related to the collection, use and sharing of consumer data and also permit additional penalties, grant additional enforcement authority and authorize private rights of action. The costs of compliance with, and the burdens imposed by, the GDPR, the CCPA, the CPRA orthese and other new federal and state laws, regulations or policies may impact our operations and/or limit the ways in which we can provide services or use personal data collected while providing services. If we fail to comply with the requirements of GDPR, the CCPA, the CPRA orthese and other new laws, regulations or policies, we could be subject to damage awards in private litigation or penalties that, in some cases, would have a material adverse impact on our business, results of operations, financial condition and cash flows. For more informationdetails on the privacy and other regulations affecting our business, see “Business–Government Regulation” in Part I Item 11. Business of this Form 10-K.10-K under the heading "
Government Regulation."Scrutiny over cybersecurity standards in the health sector is also increasing. In particular, the HHS Office for Civil Rights,increasing, and ongoing developments in partnership with the Healthcare and Public Health Sector Coordinating Council (HSCC), recently issued cybersecurity guidelines for healthcare organizations that reflect consensus-based, voluntary practices to cost-effectively reduce cybersecurity risks for organizations of varying sizes. Although these HHS-backed guidelines, entitled "Health Industry Cybersecurity Practices: Managing Threats and Protecting Patients," are voluntary, they are likely to serve as an important reference point for the healthcare industry, andthis area may cause us to invest additional resources in technology, personnel and programmatic cybersecurity controls as the cybersecurity risks we face continue to evolve.
Information security risks have significantly increased in recent years in part because of the proliferation of new technologies, the increasing use of the Internet and telecommunications technologies to conduct our operations, and the increased sophistication and activities of organized crime, hackers, terrorists and other external parties, including, among others, foreign state agents. Our business and operations rely on the secure and continuous processing, transmission and storage of confidential, proprietary and other information in our computer systems and networks, including sensitive personal information, such as PHI, social security numbers, and/or credit card information of our patients, teammates, physicians, business partners and others. Our business and operations also rely on certain critical IT vendors that support such processing, transmission and storage (which have become more relevant and important given the information security issues and risks that are intensified through remote work arrangements).
We regularly review, monitor and implement multiple layers of security measures through technology, processes and our people. We utilize security technologies designed to protect and maintain the integrity of our information systems and data, and our defenses are monitored and routinely tested internally and by external parties. Despite these efforts, our facilities and systems and those of our third-party service providers may be vulnerable to privacy and security incidents; security attacks and breaches; acts of vandalism or theft; computer viruses and other malicious code; coordinated attacks by a variety of actors, including, among others, activist entities or state sponsored cyberattacks; emerging cybersecurity risks; cyber risk related to connected devices; misplaced or lost data; programming and/or human errors; or other similar events that could impact the security, reliability and availability of our systems. Internal or external parties mayhave attempted to, and will continue to attempt to, circumvent our security systems, and we have in the past, and expect that we will in the future, defend against, experience, and respond to attacks on our network including, without limitation, reconnaissance probes, denial of service attempts, malicious software attacks including ransomware or other attacks intended to render our internal operating systems or data unavailable, and phishing attacks or business email compromise. Cybersecurity requires ongoing investment and diligence against evolving threats. For example, healthcare companies, including our Company and certain of our third-party service providers, strategic partners, consultants or contractors, are increasingly incorporating self-learning or "artificial intelligence" features into information technology capabilities. The use of this rapidly evolving technology may intensify the cybersecurity and reputational risks we face given its novel and untested nature, particularly to the extent such technology involves the use of protected health information (PHI) or personally identifiable information (PII). Emerging and advanced security threats, including, without limitation, coordinated attacks, require additional layers of security which may disrupt or impact efficiency of operations. As with any security program, there always exists the risk that employees will violate our policies despite our compliance efforts or that certain attacks may be beyond the ability of our security and other systems to detect. There can be no assurance that investments, diligence and/or our internal controls will be sufficient to prevent or timely discover an attack.
Any security breach involving the misappropriation, loss or other unauthorized disclosure or use of confidential information, including, among others, PHI, financial data, competitively sensitive information, or other proprietary data, whether by us or a third party, could have a material adverse effect on our business, results of operations, financial condition, and cash flows and materially harm our reputation. We may be required to expend significant additional resources to modify our protective measures, to investigate and remediate vulnerabilities or other exposures, or to make required notifications. The occurrence of any of these events could, among other things, result in interruptions, delays, the loss or corruption of data, cessations in the availability of systems and liability under privacy and security laws, all of which could have a material adverse effect on our business, results of operations, financial condition and cash flows, or materially harm our reputation and trigger regulatory actions and private party litigation. If we are unable to protect the physical and electronic security and privacy of our databases and transactions, we could be subject to potential liability and regulatory action, our reputation and relationships with our patients, physicians, vendors and other business partners would be harmed, and our business, results of operations, financial condition and cash flows could be materially and adversely affected. Failure to adequately protect and maintain the integrity of our information systems (including our networks) and data, or to defend against cybersecurity attacks, could subject us to monetary fines, civil suits, civil penalties or criminal sanctions and requirements to disclose the breach publicly, and could further result in a material adverse effect on our business, results of operations, financial condition and cash flows or harm our reputation. As malicious cyber activity escalates, including activity that originates outside of the U.S., and as our COVID-19 response increases ourwe continue with certain remote work arrangements and broadens oura broadened technology footprint, the risks we face relating to transmission of data and our use of service providers outside of our network, as well as the storing or processing of data within our network, intensify.have intensified. There have been increased international, federal and state and other privacy, data protection and security enforcement efforts and we expect this trend to continue. While we plan to maintain cyber liability insurance, there can be no assurance that we will successfully be able to obtain such insurance on terms and conditions that are favorable to us or at all. Additionally, any cyber liability insurance may not cover us for all types of losses or harms and may not be sufficient to protect us against the amount of all losses.
We continuously have ongoing negotiations with commercial payors, andFor additional information about our assessment of our cybersecurity risks, see discussion in Part I Item 1C. Cybersecurity of this Form 10-K.
If certain of our suppliers do not meet our needs, if the average rates that commercial payors pay us decline significantly,there are material price increases on supplies, if patients in commercial planswe are subject to restriction in plan designsnot reimbursed or adequately reimbursed for drugs we purchase or if we are unable to maintain contracts with payors with competitive terms, including, without limitation, reimbursement rates, scope and duration of coverage and in-network benefits, it would have a material adverse effect on our business, results of operations, financial condition and cash flows.
A substantial portion of our U.S. dialysis net patient services revenues for the year ended December 31, 2020 was generated from patients who have commercial payors (including hospital dialysis services) as their primary payor. The majority of these patients have insurance policies that pay us on terms and at rates that are generally significantly higher than Medicare rates. The payments we receive from commercial payors generate nearly all of our profit and all of our nonacute dialysis profits come from commercial payors. We continue to experience downward pressure on some of our commercial payment rates as a result of general conditions in the market, including as employers shift to less expensive options for medical services, as a result of consolidations among commercial payors, increased focus on dialysis services and other factors. Commercial payment rates could be materially lower in the future due to theseeffectively access new technology or other factors.
We continuously are in the process of negotiating existing and potential new agreements with commercial payors who aggressively negotiate terms with us, and we can make no assurances about the ultimate results of these negotiations or the timing of any potential rate changes resulting from these negotiations. Sometimes many significant agreements are being renegotiated at the same time. In the event that our ongoing negotiations result in overall commercial rate reductions in excess of overall commercial rate increases, the cumulative effect could have a material adverse effect on our business, results of operations, financial condition and cash flows. We believe payor consolidations have significantly increased the negotiating leverage of commercial payors, and ongoing consolidations may continue to increase this leverage in the future. Our negotiations with payors occur in a highly competitive environment and are also influenced by these marketplace dynamics, and we may experience decreased contracted rates with commercial payors or experience decreases in patient volume, including in instances where we are unable to come to agreement with commercial payors on rates, as our negotiations with commercial payors continue.
Our negotiations with commercial payors may relate to commercial fee-for-service contracts, value-based care (VBC) contracts in which we share risk with commercial payors, as well as contracts to provide dialysis services to Medicare Part C Medicare Advantage (MA) patients. If we fail to maintain contracts with payors and other healthcare providers with competitive or favorable terms, either with respect to commercial plans, commercial VBC contracts, MA plans or otherwise, including, without limitation, with respect to reimbursement rates, scope and duration of coverage and in-network benefits, or if we fail to accurately estimate the price for and manage our medical costs in an effective manner such that the profitability of our value-basedsuperior products, is negatively impacted, it could have a material adverse effect on our business, results of operations, financial condition and cash flows.
These negotiations may also be impacted by legislative or regulatory developments and associated legal rulings. For example, the final rules for the Cures Act included a provision that, effective January 1, 2021, allows Medicare-eligible beneficiaries with ESRD to choose coverage under a MA managed care plan. This provision could broaden patient access to certain enhanced benefits offered by MA plans. MA plans usually provide reimbursement to us at a negotiated rate that is generally higher than Medicare fee-for-service rates. We continue to evaluate the potential ultimate impact of this change in benefit eligibility, as there is significant uncertainty as to how many or which newly eligible ESRD patients will seek to enroll in MA plans for their ESRD benefits and how quickly any such changes would occur. This uncertainty may be heightened by components of the aforementioned final rules, which include a provision that, among other things, removes the objective time and distance standards relating to network adequacy for outpatient dialysis centers for MA plans. If MA plans attempt to use this revision to the rules to limit or restrict their networks, this may adversely impact the number of ESRD patients that select MA plans and also may result in the Company not being an in-network provider for significant MA plans. If kidney patients choose not to enroll in MA plans or choose to leave MA plans, whether due to network adequacy standards or otherwise, or if we fail to provide education to kidney patients in the manner specified by CMS, we could be subject to certain clinical, operational, financial and legal risks, which could have a material adverse effect on our business, results of operations, financial condition and cash flows. In addition, recent price and patient responsibility transparency regulations require health plans to make certain pricing and patient responsibility information publicly available. Certain of the requirements went into effect January 1, 2021 while others will go into effect January 1, 2024. There is a possibility that any changes by health plans resulting from these regulations could impact our revenue and results of operations.
Certain payors have also been attempting to design and implement plans that restrict access to ESRD coverage both in the commercial and individual market. Among other things, these restrictive plan designs seek to limit the duration and/or the breadth of ESRD benefits, limit the number of in-network providers, set arbitrary provider reimbursement rates, or otherwise restrict access to care, all of which may result in a decrease in the number of patients covered by commercial insurance. Payors have also disputed the scope and duration of ESRD benefit coverage under their plans. Any of the foregoing, including developments in plan design or new business activities of commercial payors, may lead to a significant decrease in the number of patients with commercial plans, the duration of benefits for patients under commercial plans and/or a significant decrease in the payment rates we receive, any of which would have a material adverse effect on our business, results of operations, financial condition and cash flows.
In addition, some commercial payors are pursuing or have incorporated policies into their provider manuals limiting or refusing to accept charitable premium assistance from non-profit organizations, such as the American Kidney Fund, which may impact the number of patients who are able to afford commercial plans. Paying for coverage is a significant financial burden for many patients, and ESRD disproportionately affects the low-income population. Charitable premium assistance supports continuity of coverage and access to care for patients, many of whom are unable to continue working full-time as a result of their severe condition. A material restriction in patients' ability to access charitable premium assistance may restrict the ability of dialysis patients to obtain and maintain optimal insurance coverage, and may have a material adverse effect on our business, results of operations, financial condition and cash flows.
For additional details regarding the impact of a decline in our patients under commercial plans, see the risk factor under the heading "If the number or percentage of patients with higher-paying commercial insurance declines, it could have a material adverse effect on our business, results of operations, financial condition and cash flows." For additional details regarding specific risks we face regarding potential legislative or regulatory changes that, among other things, could result in fewer patients covered under commercial plans or an increase of patients covered under more restrictive commercial plans with lower reimbursement rates, see the discussion in the risk factor under the headings "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation;" and "Changes in federal and state healthcare legislation or regulations could have a material adverse effect on our business, results of operations, financial condition and cash flows."
If the number or percentage of patients with higher-paying commercial insurance declines, it could have a material adverse effect on our business, results of operations, financial condition and cash flows.
Our revenue levels are sensitive to the number of our patients with higher-paying commercial insurance coverage and the percentage of our patients under higher-paying commercial plans relative to government-based programs. A patient's insurance coverage may change for a number of reasons, including changes in the patient's or a family member's employment status. A material portion of our commercial revenue is concentrated with a limited number of commercial payors, and any changes impacting our highest paying commercial payors will have a disproportionate impact on us. In addition, many patients with commercial and government insurance rely on financial assistance from charitable organizations, such as the American Kidney Fund. Certain payors have challenged our patients' and other providers' patients' ability to utilize assistance from charitable organizations for the payment of premiums, including, without limitation, through litigation and other legal proceedings. The
use of charitable premium assistance for ESRD patients has also faced challenges and inquiries from legislators, regulators and other governmental authorities, and this may continue. In addition, CMS or another regulatory agency or legislative authority may issue a new rule or guidance that challenges or restricts charitable premium assistance. For additional details, see the risk factor under the headings "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation;" and "Changes in federal and state healthcare legislation or regulations could have a material adverse effect on our business, results of operations, financial condition and cash flows."If any of these challenges to kidney patients' use of premium assistance is successful or restrictions are imposed on the use of financial assistance from such charitable organizations or if organizations providing such assistance are no longer available such that kidney patients are unable to obtain, or continue to receive or receive for a limited duration, such financial assistance, it could have a material adverse effect on our business, results of operations, financial condition and cash flows. In addition, if our assumptions about how kidney patients will respond to any change in financial assistance from charitable organizations are incorrect, it could have a material adverse effect on our business, results of operations, financial condition and cash flows.
When Medicare becomes the primary payor for a patient, the payment rate we receive for that patient decreases from the employer group health plan or commercial plan rate to the lower Medicare payment rate. If the number of our patients who have Medicare or another government-based program as their primary payor increases, it could negatively impact the percentage of our patients covered under commercial insurance plans. There are a number of factors that could drive a decline in the percentage of our patients covered under commercial insurance plans, including, among others, a continued decline in the rate of growth of the ESRD patient population, continued improved mortality or the reduced availability of commercial health plans or reduced coverage by such plans through the ACA exchanges or otherwise dueability to changes to the marketplace, healthcare regulatory system or otherwise. Commercial payors could also cease paying in the primary position after providing 30 months of coverage resulting in potentially material reductions in payment as the patient moves to Medicare primary. Moreover, declining macroeconomic conditions, such as, for example, those resulting from the ongoing COVID-19 pandemic, could also negatively impact the percentage of our patients covered under commercial insurance plans. To the extent there are sustained or increased job losses in the U.S., we could experience a decrease in the number of patients covered under commercial plans and/or an increase in uninsured and underinsured patients independent of whether general economic conditions improve. If we experience higher numbers of uninsured or underinsured patients, it also would result in an increase in uncollectible accounts.
Finally, the ultimate results of our continual negotiations with commercial payors under existing and potential new agreements cannot be predicted and, among other things, could result in a decrease in the number of our patients covered by commercial plans to the extent that we cannot reach agreement with commercial payors on rates and other terms, resulting in termination or non-renewals of existing agreements and our inability to enter into new agreements. Our agreements and rates with commercial payors may be impacted by new business activities of these commercial payors as well as steps that these commercial payors have taken and may continue to take to control the cost of and/or the eligibility for access toeffectively provide the services that we provide, including, without limitation, relative to products onoffer and off the healthcare exchanges. These efforts could impact the number of our patients who are eligible to enroll in commercial insurance plans, and remain on the plans, including plans offered through healthcare exchanges. For additional detail on the risks related to commercial payor activity, including restrictive plan design, see the discussion under the heading "We continuously have ongoing negotiations with commercial payors, and if the average rates that commercial payors pay us decline significantly, if patients in commercial plans are subject to restriction in plan designs or if we are unable to maintain contracts with payors with competitive terms, including, without limitation, reimbursement rates, scope and duration of coverage and in-network benefits, it would have a material adverse effect on our business, results of operations, financial condition and cash flows." We could also experience a further decrease in the payments we receive for services if changes to the marketplace or the healthcare regulatory system result in fewer patients covered under commercial plans or an increase of patients covered under more restrictive commercial plans with lower reimbursement rates, among other things.
If there is a significant reduction in the number of patients under higher-paying commercial plans relative to government-based programs that pay at lower rates or a significant increase in the number of patients that are uninsured and underinsured, it would have a material adverse effect on our business, results of operations, financial condition and cash flows.
If we are not able to successfully implement our strategy with respect to home-based dialysis, including maintaining our existing business and further developing our capabilities in a complex and highly regulated environment, it could have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation. We are also subject to the risk associated with our increased reliance on third party service providers.
Our home-based dialysis services, which include home hemodialysis and peritoneal dialysis (PD), represented approximately 17%We have significant suppliers, with a substantial portion of our U.S.total vendor spend concentrated with a limited number of third party suppliers. These third party suppliers include, without limitation, suppliers of pharmaceuticals or clinical products that may be the primary source of products critical to the services we provide, or to which we have committed obligations to make purchases, sometimes at particular prices. We and other dialysis patient services revenues for the year ended December 31, 2020, andproviders have increasingly
become an important partexperienced supply chain shortages with respect to certain of our overall strategy. In addition, home-based dialysis recently has beenequipment and clinical supplies, such as dialysate, which is the subject of increased politicalfluid solution used in hemodialysis to filter toxins and industry focus. For example,fluid from the blood, and in connection with the 2019 Executive Order, HHS set out specific goals relatedcertain cases, we have had to home dialysis and CMMI’s ESRD Treatment Choices mandatory payment model (ETC) included new incentives to encourage dialysis at home. We are a leader in home-based dialysis and have made investments in processes and infrastructure to continue to grow this modality. There are, however, risks associated with this growth, including, among other things, financial, legal andmake significant operational risks related to our ability to design and develop infrastructure and to plan for capacity in a modality that is part of an evolving marketplace. We may also be subject to associated risks related to our ability to successfully manage related operational initiatives, find, train and retain appropriate staff, contract with payors for appropriate reimbursement, and maintain processes to adhere to the complex regulatory and legal requirements, including without limitation those associated with billing Medicare. For additional detail on risks associated with operating in a highly regulated environment, see "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, couldresponse. Separately, current macroeconomic conditions also have a material adverse effect on our business, results of operations, financial conditionresulted in global supply chain challenges and cash flows, couldhas materially harm our stock price, andimpacted global supply chain reliability, as further described in some circumstances, could materially harm our reputation." In addition to the above risks, certain risks inherent to home-based dialysis will increase as we expand our home-based dialysis offerings, including risks related to managing transitions between in-center and home-based dialysis, billing and telehealth systems, among others. For additional detail on risks associated with information systems and new technology generally, see the risk factor under the heading, "Failing to effectively maintain, operate or upgradeMacroeconomic conditions and global events..."
If any of our information systems or those of third-party service providers upon which we rely,suppliers do not meet our needs for the products they supply, including, without limitation, in the event of supply chain disruptions due to global events, a product recall, other shortage or dispute, and we are not able to find adequate alternative sources at competitive prices; if we experience material price increases from these suppliers or otherwise in connection with our clinical, billing and collections systems could materially adversely affect our business, results of operations, financial condition and cash flows."
An increased focus on home-based dialysis is also indicativeactions to secure needed products that we are unable to mitigate; if some of the generally evolving market for kidney care. This developing market may create additional opportunities for competition with relative ease of entry, anddrugs that we purchase from our suppliers are not reimbursed or not adequately reimbursed by commercial or government payors; or if we are unable to successfully adapt to these marketplace developments in a timelysecure products, including pharmaceuticals at competitive rates and compliant manner, we may see a reduction in our overall number of patients, among other things. Our response towithin the COVID-19 pandemic has also required us to impose certain operational restrictions that may adversely impact certain home-based dialysis initiatives, and the extent of this impact may depend on the severity or duration of the pandemic, among other things. For additional detail on the competitive landscape in kidney care, see the risk factor under the heading "If we are unable to compete successfully, including, without limitation, implementing our growth strategy and/or retaining patients and physicians willing to serve as medical directors,desired time frame; it could materially adversely affectnegatively impact our business, results of operations, financial condition and cash flows," and for additional detail onability to effectively provide the impact of COVID-19 on our home-based dialysis business, see the risk factor under the heading "We face various risks related to the dynamic and evolving novel coronavirus pandemic, any of which mayservices we offer, have a material adverse impact on us."If we are not able to successfully implement our strategy with respect to home-based dialysis, including maintaining our existing business and further developing our capabilities in a complex and highly regulated environment, it could have a material adverse effect on our business, results of operations, financial condition and cash flows, and could materially harm our reputation.
Changes In addition, the technology related to the products critical to the services we provide is subject to new developments which may result in superior products. If we are not able to access superior products on a cost-effective basis, either due to competitive conditions in the structure ofmarketplace or otherwise, or if suppliers are not able to fulfill our requirements for such products, we could face patient attrition and payment rates under the Medicare ESRD programother negative consequences which could have a material adverse effect on our business, results of operations, financial condition and cash flows.
A substantial portionWe also rely increasingly on third party service providers to perform certain functions, including, among others, finance and accounting and information technology functions. This reliance subjects us to risks arising from the loss of control over these services, changes in pricing that may affect our dialysis revenues are generated from patients who have Medicare as their primary payor. For patients with Medicare coverage, all ESRD payments for dialysis treatments are currently made under a single bundled payment rate which provides a fixed payment rateoperating results, and potentially, termination of provisions of these services by our providers. There can be no assurance that our third party service providers will provide, or continue to encompass all goods andprovide, the level of services provided during the dialysis treatment that are related to the treatment of dialysis, subject to certain adjustments as described below. Most lab services are also included in the bundled payment.
Under the ESRD Prospective Payment System (PPS), bundled payments to a dialysis facility may be reducedwe require. Any failure by as much as 2% based on the facility's performance in specified quality measures set annually by CMS through the ESRD Quality Incentive Program, which was established by the Medicare Improvements for Patients and Providers Act of 2008. The bundled payment rate is also adjusted for certain patient characteristics, a geographic usage index and certain other factors. In addition, the ESRD PPS is subject to rebasing, which can have a positive financial effect, or a negative one if the government fails to rebase in a manner that adequately addresses the costs borne by dialysis facilities. Similarly, as new drugs, services or labs are added to the ESRD bundle, CMS' failureour third party service providers to adequately calculate the costs associated with the drugs, services or labsperform their obligations could negatively impact our ability to effectively execute certain important corporate functions and have a material adverse effect on our business, results of operations, financial condition and cash flows. In certain instances, new injectable, intravenous or oral products may be reimbursed separately from the bundled payment through a transitional drug add-on payment adjustment (TDAPA). For a discussion of certain risks associated with this transitional pricing process, see the risk factor under the heading, "Changes in clinical practices, payment rates or regulations impacting pharmaceuticals could have a material adverse effect on our business, results of operations, financial condition, and cash flows and negatively impact our ability to care for patients."
The current bundled payment system presents certain operating, clinical and financial risks, which include, without limitation:
•Risk that our rates are reduced by CMS. CMS publishes a final rule for the ESRD PPS each year and uncertainty about future payment rates remains a material risk to our business.
•Risk that CMS, on its own or through its contracted Medicare Administrative Contractors (MACs) or otherwise, implements Local Coverage Determinations (LCDs) or implements payment provisions, policy or regulatory mandates, including changes to the existing or future PPS, that limit our ability to either be paid for covered dialysis services or bill for treatments or other drugs and services or other rules that may impact reimbursement. Such payment rules and regulations and coverage determinations or related decisions could have an adverse impact on our operations and revenue. There is also risk commercial insurers could seek to incorporate the requirements or limitations associated with such LCDs or CMS guidance into their contracted terms with dialysis providers, which could have an adverse impact on our revenue.
•Risk that a MAC, or multiple MACs, change their interpretations of existing regulations, manual provisions and/or guidance, or seek to implement or enforce new interpretations that are inconsistent with how we have interpreted existing regulations, manual provisions and/or guidance.
•Risk that CMS implements data and related reporting requirements that result in decreased reimbursement and/or increased technology and operational costs.
•Risk that increases in our operating costs will outpace the Medicare rate increases we receive. We expect operating costs to continue to increase due to inflationary factors, such as increases in labor and supply costs, including, without limitation, increases in maintenance costs and capital expenditures to improve, renovate and maintain our facilities, equipment and information technology to meet changing regulatory requirements and business needs, regardless of whether there is a compensating inflation-based increase in Medicare payment rates or in payments under the bundled payment rate system.
•Risk of continued federal budget sequestration cuts or other disruptions in federal government operations and funding. As a result of the Budget Control Act of 2011, the Bipartisan Budget Act (BBA) and the CARES Act, an annual 2% reduction to Medicare payments took effect on April 1, 2013, and has been extended through 2030 (though the reduction was temporarily suspended from May 1, 2020 through March 31, 2021 in connection with COVID-19 relief related legislation). These across-the-board spending cuts have affected and will continue to adversely affect our business, results of operations, financial condition and cash flows. Any extended disruption in federal government operations and funding, including an extended government shutdown, U.S. government debt default and/or failure of the U.S. government to enact annual appropriations could have a material adverse effect on our business, results of operations, financial condition and cash flows. Additionally, disruptions in federal government operations may delay or negatively impact regulatory approvals and guidance that are important to our operations, and create uncertainty about the pace of upcoming regulatory developments.
•Risk that failure to adequately develop and maintain our clinical systems or failure of our clinical systems to operate effectively could have a material adverse effect on our business, results of operations, financial condition and cash flows. For example, in connection with claims for which at least part of the government's payments to us is based on clinical performance or patient outcomes or co-morbidities, if our clinical systems fail to accurately capture the data we report to CMS or we otherwise have data integrity issues with respect to the reported information, we might be over-reimbursed by the government, which could, among other things, subject us to liability exclusion from participation in federal healthcare programs, and penalties under the federal Civil Monetary Penalty statute and could adversely impact our reputation.
We are subject to similar risks for services billed separately from the ESRD bundled payment, including, without limitation, the risk that a MAC, or multiple MACs, change their interpretations of existing regulations, manual provisions and/or guidance; or seek to implement or enforce new interpretations that are inconsistent with how we have interpreted existing regulations, manual provisions and/or guidance.
In addition to the above risks under the current Medicare ESRD program, changing legislation and other regulatory and executive developments have led and may continue to lead to the emergence of new models of care and other initiatives in both the government and private sector that, among other things, may impact the structure of, and payment rates under, the Medicare ESRD program. Moreover, the number of our patients with primary Medicare coverage may be subject to change, particularly with the effectiveness of the Cures Act, which allows Medicare-eligible individuals with ESRD to enroll in Medicare Part C MA managed care plans. For additional details regarding the risks we face for failing to adhere to our Medicare and Medicaid
regulatory compliance obligations or failing to adequately implement strategic initiatives to adjust to marketplace developments, see the risk factor above under the headings "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation;" and "Changes in federal and state healthcare legislation or regulations could have a material adverse effect on our business, results of operations, financial condition and cash flows."
Changes in clinical practices, payment rates or regulations impacting pharmaceuticals and/or devices could have a material adverse effect on our business, results of operations, financial condition, and cash flows and negatively impact our ability to care for patients.
Medicare bundles certain pharmaceuticals into the ESRD PPS payment rate at industry average doses and prices. Variations above the industry average may be subject to partial reimbursement through the PPS outlier reimbursement policy.
Changes to industry averages, which can be caused by, among other things, changes in physician prescribing practices, including in response to the introduction of new drugs, treatments or technologies, changes in best and/or accepted clinical practice, changes in private or governmental payment criteria regarding pharmaceuticals and/or devices, or the introduction of administration policies may negatively impact our ability to obtain sufficient reimbursement levels for the care we provide, which could have a material adverse effect on our business, results of operations, financial condition and cash flows. Physician practice patterns, including their independent determinations as to appropriate pharmaceuticals and dosing, are subject to change, including, for example, as a result of changes in labeling of pharmaceuticals or the introduction of new pharmaceuticals. Additionally, commercial payors have increasingly examined their administration policies for pharmaceuticals and, in some cases, have modified those policies. If such policy and practice trends or other changes to private and governmental payment criteria make it more difficult to preserve our margins per treatment, it could have a material adverse effect on our business, results of operations, financial condition and cash flows. Further, increased utilization of certain pharmaceuticals whose costs are included in a bundled reimbursement rate, or decreases in reimbursement for pharmaceuticals whose costs are not included in a bundled reimbursement rate, could also have a material adverse effect on our business, results of operation, financial condition and cash flows.
Regulations and processes impacting reimbursement for pharmaceuticals and/or devices and any changes thereto could similarly affect our operating results. For example, from January 1, 2018 to December 31, 2020, calcimimetics was part of the Medicare Part B payment and was subject to a TDAPA period prior to being incorporated into the payment bundle on January 1, 2021. During this transitional period, the wider availability of generic supplies of oral calcimimetics drove the acquisition cost of that drug down, which in turn lowered associated reimbursement rates and led to significant fluctuations in our levels of operating income. In addition, we anticipate that a hypoxia-inducible factor (HIF) product could be approved by the FDA and available to the market during 2021, but as of the date hereof, the timing and details of such an approval, including the contents of the applicable FDA label, remain uncertain. We expect that HIF products will be subject to a TDAPA period prior to being incorporated into the payment bundle. We are developing operational and clinical processes designed to provide the drug as may be required under the applicable regulations and as may be prescribed by physicians and also are working to contract with manufacturers of drug(s) to establish terms and access to the product, as well as payors, as applicable, for reimbursement and/or administration of the drug. If HIF products are approved, we could experience significant fluctuations in our associated levels of operating income and could be subject to material financial, operational and/or legal risk if we are not adequately reimbursed for the cost of the drug, if we are unable to implement effective and appropriate operational measures to distribute the drug, if we fail to implement appropriate storage and diversion controls or if we cannot obtain competitive pricing for the HIF, the aggregate impact of these risks could have a material adverse effect on our business, results of operation, financial condition and cash flows.
Similar operating and clinical rigor and appropriate processes will be needed forAmong other potential new drugs, treatments or technologies that are approved and come onto the market. Any failure to successfully contract with manufacturers for competitive pricing, failure to successfully contract with the government or other payors for appropriate reimbursement, or failure to prepare, develop and implement processes that provide for appropriate availability and use in our clinics could have a material adverse impact on our business, results of operations, financial condition and cash flows. Additionally,things, as new kidney care drugs, treatments or technologies are introduced over time, we expect that the use of transitional payment adjustments to incorporate certain of these new drugs, treatments or technologies as defined by the CMS policy into the bundled Medicare Part B ESRD payment may lead to fluctuations in associated levels of operating income and risk that the reimbursement levels of such drugs, treatments or technologies may not adequately cover our cost to obtain the drug or other associated costs. Drivers of these risks include, among other things, the risk that CMS may not provide adequate funding in the Medicare Part B ESRD payment in the transitional or post-transitional period or such items are not covered by transitional add on pricing, in which case there may be
less clarity on the reimbursement, either of which may in turn materially adversely impact our business, results of operations, financial condition and cash flows. For example, in the event that oral phosphate binders are incorporated into the payment bundle, there can be no assurance that CMS will calculate the bundled payment rate in a manner that correctly accounts for the inclusion of these oral medications and the additional costs associated with dialysis providers having to supply such drugs. We are developing operational and clinical processes designed to provide the drug as may be required under the applicable regulations and as may be prescribed by physicians and also are working to contract with manufacturers of drug(s) to establish terms and access to the product, as well as payors, as applicable, for reimbursement and/or administration of the drug. If the government or other payors implement new requirements or protocols for patients to receive the drug and include pricing in the bundle, we could experience significant fluctuations in our associated levels of operating income and could be subject to material financial, operational and/or legal risk if we are not adequately reimbursed for the cost of the drug, if we are unable to implement effective and appropriate operational measures to distribute or bill for the drug, if we fail to implement appropriate storage and diversion controls or if we cannot obtain competitive pricing for the drug. The aggregate impact of these risks could have a material adverse effect on our business, results of operation, financial condition and cash flows.
Similar operating and clinical rigor and appropriate processes will be needed for other potential new drugs, treatments or technologies that are approved and come onto the market, as well as for drugs, treatments or technologies that we contract to receive from different suppliers. Any failure to successfully contract with manufacturers for competitive pricing, failure to successfully contract with the government or other payors for appropriate reimbursement, or failure to prepare, develop and implement processes that provide for appropriate availability and use in our clinics in compliance with applicable laws, including those related to controlled substances, could have a material adverse impact on our business, results of operations, financial condition and cash flows.
We may also be subject to increased inquiries or audits from a variety of governmental bodies or claims by third parties related to pharmaceuticals, which would require management's attention and could result in significant legal expense. Any negative findings could result in, among other things, substantial financial penalties or repayment obligations, the imposition of certain obligations on and changes to our practices and procedures as well as the attendant financial burden on us to comply with the obligations, or exclusion from future participation in the Medicare and Medicaid programs, and could have a material adverse effect on our business, results of operations, financial condition, cash flows and reputation. For additional details, see the risk factor under the heading "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation.requirements..."
Changes in state Medicaid or other non-Medicare government-based programs or payment rates could have a material adverse effect on our business, results of operations, financial condition and cash flows.
Primary coverage for a significant number of our patients comes from state Medicaid programs partially funded by the federal government as well as other non-Medicare government-based programs, such as coverage through the Department of Veterans Affairs (VA). As state governments and other governmental organizations face increasing financial hardship and budgetary pressure, including as a result of the COVID-19 pandemic, we may in turn face reductions in payment rates, delays in the receipt of payments, limitations on enrollee eligibility or other changes to the applicable programs. For example, certain state Medicaid programs and the VA have recently considered, proposed or implemented payment rate reductions.
The VA adopted Medicare's bundled PPS pricing methodology for any veterans receiving treatment from non-VA providers under a national contracting initiative. Since we are a non-VA provider, these reimbursements are tied to a percentage of Medicare reimbursement, and we have exposure to any dialysis reimbursement changes made by CMS. Approximately 3% of our U.S. dialysis net patient services revenues for the year ended December 31, 2020 were generated by the VA.
In 2019, we entered into a Nationwide Dialysis Services contract with the VA that includes five separate one-year renewal periods throughout the term of the contract. The term structure is similar to our prior five-year agreement with the VA, and is consistent with VA practice for similar provider agreements. With this contract award, the VA has agreed to keep our percentage of Medicare reimbursement consistent with that under our prior agreement with the VA during the term of the contract. As with that prior agreement, this agreement provides the VA with the right to terminate the agreements without cause on short notice, among other things. Should the VA renegotiate, not renew or cancel these agreements for any reason, we may cease accepting patients under this program and may be forced to close centers or experience lower reimbursement rates, which could have a material adverse effect on our business, results of operations, financial condition and cash flows.
State Medicaid programs are increasingly adopting Medicare-like bundled payment systems, but sometimes these payment systems are poorly defined and are implemented without any claims processing infrastructure, or patient or facility adjusters. If these payment systems are implemented without any adjusters and claims processing infrastructure, Medicaid payments will be substantially reduced and the costs to submit such claims may increase, which will have a negative impact on our business, results of operations, financial condition and cash flows. In addition, some state Medicaid program eligibility requirements mandate that citizen enrollees in such programs provide documented proof of citizenship. If our patients cannot meet these proof of citizenship documentation requirements, they may be denied coverage under these programs, resulting in decreased patient volumes and revenue. These Medicaid payment and enrollment changes, along with similar changes to other non-Medicare government programs, could reduce the rates paid by these programs for dialysis and related services, delay the receipt of payment for services provided and further limit eligibility for coverage which could have a material adverse effect on our business, results of operations, financial condition and cash flows.
If we are unable to compete successfully, including, without limitation, implementing our growth strategy and/or retaining patients and developing and maintaining relationships with physicians willing to serve as medical directors,and hospitals, it could materially adversely affect our business, results of operations, financial condition and cash flows.
Patient retentionWe operate in a highly competitive and continuously evolving environment across the continuedspectrum of kidney care, and operating in this market requires us to successfully execute on strategic initiatives which, among other things, build or retain our patient population through acquisition or referrals, of patients fromor that develop and maintain our relationships with physicians and hospitals in both the dialysis and pre-dialysis space.
Competition for relationships with certain referral sources, such asincluding nephrologists and hospitals, in existing and nephrologists, as well as acquisitions, are some of the important parts of our growth strategy. In our U.S. dialysis business,expanding geographies or areas is intense, and we continue to face intense competition from large and medium-sized providers, among others, which compete directly with us for the limited acquisition targets as well as for individual patients and physicians qualified to serve as medical directors. U.S. regulations require medical directors, for each center. As welimited acquisition targets and our competitors continuefor individual patients. In addition to growthese large and open new dialysis centers, we may not be able to retain an adequate number of nephrologists to serve as medical directors. Competition in existing and expanding geographies or areas is intense, and is not limited to largemedium-sized competitors with substantial financial resources or toand other established participants in the
dialysis space. Wespace, we also compete with individual nephrologists who have opened their own dialysis units or facilities. Moreover, as we continue our expansion into various international markets, we will continue to face competition from large and medium-sized providers, among others, for acquisition targets.
In addition,Our largest competitor, Fresenius Medical Group, our largest competitor,Care (FMC), manufactures a full line of dialysis supplies and equipment in addition to owning and operating dialysis centers. This may, among other things, give itFMC cost advantages over us because of its ability to manufacture its own products. See further discussion regarding risks associated
We continuously compete for maintaining or developing relationships with physicians that can serve as medical directors at our supplierscenters. Physicians, including medical directors, choose where they refer their patients, and new technologies under the heading "If certainneither of our suppliers do not meetcurrent or former medical directors have an obligation to refer their patients to our needs, if therecenters. Certain physicians prefer to have their patients
treated at dialysis centers where they or other members of their practice supervise the overall care provided as medical director of the center. As a result, referral sources for many of our centers include the physician or physician group providing medical director services to the center. Moreover, because Medicare regulations require medical directors for each of our Medicare certified dialysis centers, our ability to operate our centers depends in part on our ability to secure medical director agreements with a sufficient number of nephrologists. Our medical director contracts are material price increases on supplies, if we are not reimbursedfor fixed periods, generally ten years, and at any given time a large number of them could be up for renewal at the same time. Medical directors have no obligation to extend their agreements with us and, under certain circumstances, our former medical directors may choose to provide medical director services for competing providers or adequately reimbursed for drugs we purchase or ifestablish their own dialysis centers in competition with ours. If we are unable to effectively access new technologycontract with nephrologists to provide medical director services, then we may be unable to satisfy the federal Medicare requirements associated with medical directors and to operate our centers. The aging of the nephrologist population and opportunities presented by our competitors may negatively impact a medical director's decision to enter into or superior products, it couldextend his or her agreement with us and potential declines in the overall number of nephrologists may negatively impact our ability to effectivelyenter into medical director agreements in the future. In addition, if the terms of any existing agreement are found to violate applicable laws, there can be no assurances that we would be successful in restructuring the relationship, which would lead to the early termination of the agreement. If we are unable to obtain qualified medical directors to provide supervision of the services we offeroperations and care provided at our dialysis centers, it could affect not only our ability to operate the center but also the degree to which other physicians to feel confident in referring patients to our dialysis centers. If a significant number of physicians were to cease referring patients to our dialysis centers, whether due to law, rule or regulation, new competition, a perceived decrease in the quality of service levels at our centers or other reasons, it would have a material adverse effect on our business, results of operations, financial condition and cash flows."
In addition, as we continue to traditional dialysisexpand our offerings across the kidney care continuum, our ability to enter into and maintain integrated kidney care relationships with payors, physicians and other providers may have an impact our ability to participate in integrated kidney care. This environment is highly competitive and has been evolving. For example, there have been a number of announcements, initiatives and capital raises by non-traditional dialysis providers and others, which relate to entry into the dialysis and pre-dialysis space, the development of innovative technologies, or the commencement of new business activities that could be disruptivetransformative to the industry. Some of these new entrants have considerable financial resources. Although these and other potential competitors may face operational or financial challenges, the highly-competitive and evolving nature of the dialysis and pre-dialysis marketplaces have presented some opportunities for relative ease of entry for these and other potential competitors. As a result, we may compete with these smaller or non-traditional providers or others in an asymmetrical environment with respect to data and regulatory requirements that we face as an ESRD service provider, thereby negatively impacting our ability to effectively compete. These and other factors have continued to drive change in the dialysis and pre-dialysis space, and if we are unable to successfully adapt to these dynamics, it could have a material adverse impact on our business, results of operations, financial condition and cash flows. As an example, new entrants are aggressively pursuing opportunities to participate in the new CMMI payment models or otherwise establish value-based care programs, and increasing investment in and availability of funding to new entrants in the dialysis and pre-dialysis marketplace that may not be as cautious in adhering to applicable laws and regulations and/or may not be subject to the same regulatory restrictions as the Company, could adversely impact our ability to enter into competitive arrangements.
Furthermore, eachEach of the aforementioned competitive pressures and related risks may be impacted by a continued decline in the rate of growth of the ESRD patient population, higher mortality rates for dialysis patients or other reductions in demand for dialysis treatments.treatments, whether due to the development of innovative technologies or otherwise. The recent 20202023 annual data report from the United States Renal Data System (USRDS)USRDS suggests that the rate of growth of the ESRD patient population is declining relative to long termlong-term trends. As the USRDS report presents data through December 31, 2021, it reflects the initial compounding impact of COVID-19 on this patient base.
A number of factors may impact ESRDESKD growth rates, including, without limitation,among others, mortality rates for dialysis patients or CKD patients, the aging of the U.S. population, transplant rates, incidence rates for diseases that cause kidney failure such as diabetes and hypertension, transplant rates, mortality rates for dialysis patients and growth rates of minority populations with higher than average incidence rates of ESRD. CertainESKD or other changes in demand for dialysis treatments over time, including for example, as a result of these factors,the development and application of certain innovative technologies, drugs or other treatments such as the glucagon-like peptide 1 (GLP-1) receptor agonist, SGLT2 inhibitors, and other classes of drugs or new classes of drugs or other treatments that may, among other things, slow the progression of CKD. Any decrease in particulargrowth rates for the ESRD patient population, higher mortality rates for dialysis patients have been impacted by the COVID-19 pandemic. The magnitude of these cumulative COVID-19 related impacts on our patient census and treatment volumes has been substantial and depending on the ultimate severity and duration of the pandemic, could be material. For additional information, see the risk factor under the heading "Changesor other reductions in the structure of and payment rates under the Medicare ESRD programdemand for dialysis treatments, if sustained or significant, could have a material adverse effect on our business, results of operations, financial condition and cash flows." Any such impact would be magnified to the extent it also resulted in a lower number of patients with commercial insurance or a lower percentage of patients under commercial insurance relative to government-based programs. While we have continued efforts to seek growth opportunities, such as by expanding our business into various international markets, we face ongoing competition from large and medium-sized providers, among others, for acquisition targets in those markets. Providers may reduce pricing in an attempt to capture more volume in the face
of declining ESRD patient growth. Any failure on our part to appropriately adjust our business and operations in light of these complicated marketplace dynamics could have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation.
If we are not able to effectively implementcompete in the markets in which we operate, including by implementing our growth strategy, including byeffectively adjusting our business and operations in light of evolving marketplace dynamics, building or retaining our patient population, maintaining and developing relationships with nephrologists and hospitals, particularly medical director relationships, or making acquisitions at the desired pace or at all; if we are not able to continue to maintain the expected or desired level of non-acquired growth; or if we experience significant patient attrition either as a result of new business activities in the dialysis or pre-dialysis space by our existing competitors, other market participants, new entrants, new technology or other forms of competition, or as a result of reductions in demand for dialysis treatments, including, without limitation, due to increased mortality rates for dialysis patients resulting from COVID-19 or otherwise, reduced prevalence of ESRD, the development of innovative technologies, drugs or other treatments or an increase in the number of kidney transplants, it could materially adversely affect our business, results of operations, financial condition and cash flows.
The U.S. integrated kidney care, U.S. other ancillary services and international operations that we operate or invest in now or in the future may generate losses and may ultimately be unsuccessful. In the event that one or more of these activities is unsuccessful, our business, results of operations, financial condition and cash flows may be negatively impacted and we may have to write off our investment and incur other exit costs.
Our U.S. integrated kidney care and U.S. other ancillary services are subject to many of the same risks, regulations and laws, as described in the risk factors related to our dialysis business set forth in Part I Item 1A. of this Form 10-K, and are also subject to additional risks, regulations and laws specific to the nature of the particular strategic initiative. We have added, and expect to continue to add additional service offerings to our business and pursue additional strategic initiatives in the future as circumstances warrant, which could include healthcare products or services not directly related to dialysis. Many of these initiatives require or would require investments of both management and financial resources and can generate significant losses for a substantial period of time and may not become profitable in the expected timeframe or at all. There can be no assurance that any such strategic initiative will ultimately be successful. Any significant change in market conditions or business performance, including, without limitation, as a result of the political, legislative or regulatory environment, may impact the performance or economic viability of any of these strategic initiatives.
If any of our U.S. integrated kidney care, U.S. other ancillary services or international operations are unsuccessful, it may have a negative impact on our business, results of operations, financial condition and cash flows, and if we determine to exit that line of business we may incur significant termination costs. For discussion of risks and potential impacts specific to our integrated kidney care business and related growth strategy, see the risk factor under the heading "If we are not able to successfully implement our strategy with respect to our integrated kidney care and value-based care initiatives..." In addition, we may incur material write-offs or impairments of our investments, including, without limitation, goodwill or other assets, in one or more of our U.S. integrated kidney care, U.S. other ancillary services or international operations. In that regard, we have taken, and may in the future take, impairment and restructuring charges in addition to those described above related to our U.S. integrated kidney care, U.S. other ancillary services and international operations.
Expansion of our operations to and offering our services in markets outside of the U.S., and utilizing third-party suppliers and service providers operating outside of the U.S., subjects us to political, economic, legal, operational and other risks that could have a material adverse effect on our business, results of operations, financial condition, cash flows and reputation.
We are continuing to expand our operations by offering our services and entering new lines of business in certain markets outside of the U.S., and we have increased our utilization of third-party suppliers and service providers operating outside of the U.S., which increases our exposure to the inherent risks of doing business in international markets. Depending on the market, these risks include those relating to:
•changes in the local economic environment including, among other things, labor cost increases and other general inflationary pressures;
•political instability, armed conflicts or terrorism;
•public health crises, such as pandemics or epidemics;
•social changes;
•intellectual property legal protections and remedies;
•trade regulations;
•procedures and actions affecting approval, production, pricing, reimbursement and marketing of products and services;
•foreign currency and applicable exchange rates;
•additional U.S. and foreign taxes;
•export controls;
•antitrust and competition laws and regulations;
•lack of reliable legal systems which may affect our ability to enforce contractual rights;
•changes in local laws or regulations, or interpretation or enforcement thereof;
•potentially longer ramp-up times for starting up new operations and for payment and collection cycles;
•financial and operational, and information technology systems integration;
•failure to comply with U.S. laws, such as the FCPA, or local laws that prohibit us, our partners, or our partners' or our agents or intermediaries from making improper payments to foreign officials or any third party for the purpose of obtaining or retaining business;
•laws, regulations or other guidance that require enhanced disclosures and due diligence surrounding the impacts of our Company and value chain on, and the financial risks and opportunities for our Company from, ESG or other similar sustainability or corporate responsibility matters, as well as enhanced policies, processes and controls designed to appropriately monitor and track such information and enhanced actions to address our Company's impact on these matters; and
•data and privacy restrictions, among other things.
Issues relating to the failure to comply with applicable non-U.S. laws, requirements or restrictions may also impact our domestic business and/or raise scrutiny on our domestic practices.
Additionally, some factors that will be critical to the success of our international business and operations will be different than those affecting our domestic business and operations. For example, conducting international operations requires us to devote significant management resources to implement our controls and systems in new markets, to comply with local laws and regulations, including to fulfill financial reporting and records retention requirements among other things, and to overcome the numerous new challenges inherent in managing international operations, including, without limitation, challenges based on differing languages and cultures, challenges related to establishing clinical operations in differing regulatory and compliance environments, and challenges related to the timely hiring, integration and retention of a sufficient number of skilled personnel to carry out operations in an environment with which we are not familiar.
Any expansion of our international operations through acquisitions or through organic growth could increase these risks. Additionally, while we may invest material amounts of capital and incur significant costs in connection with the growth and development of our international operations, including to start up or acquire new operations, we may not be able to operate them profitably on the anticipated timeline, or at all.
These risks could have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation.
Failing to effectively maintain, operate or upgrade our information systems or those of third-party service providers upon which we rely, including, without limitation, our clinical, billing and collections systems, or failure to adhere to federal and state data sharing and access requirements and regulations could materially adversely affect our business, results of operations, financial condition, cash flows and reputation.
Our business depends significantly on effective information systems. Our information systems require an ongoing commitment of significant resources to maintain, upgrade and enhance existing systems and develop or contract for new systems in order to keep pace with continuing changes in information processing technology, emerging cybersecurity risks and threats, evolving industry, legal and regulatory standards and requirements, new models of care, and other changes in our business, among other things. For example, the provisions related to data interoperability, information blocking, and patient access in the Cures Act and No Surprises Act include, among other things, changes to the Office of the National Coordinator
for Health Information Technology’s (ONC's) Health IT Certification Program and requirements that CMS-regulated payors make relevant claims/care data and provider directory information available through standardized patient access and provider directory application programming interfaces (APIs) that connect to provider electronic health records. We have made and expect to continue to make significant investments in updating and integrating our clinical IT systems and continuing to build our data interoperability capabilities. Any failure to adequately comply with these and other provisions related to data interoperability, information blocking, and patient access may, among other things, result in fines and sanctions, adversely impact our Medicare business, our ability to scale our integrated care business and our ability to compete with certain smaller and/or non-traditional providers taking advantage of an asymmetrical environment with respect to data and/or regulatory requirements given our status as an ESRD service provider; or otherwise have a material adverse effect on our business, financial condition, results of operations and cash flows. Rulemaking in these areas is ongoing, and there can be no assurances that the implementation of planned enhancements to our systems, such as our implementation of these data interoperability provisions or our other ongoing efforts to upgrade and better integrate our clinical systems, will be successful once the regulatory environment settles or that we will ultimately realize anticipated benefits from investments in new or existing information systems. In addition, we may from time to time obtain significant portions of our systems-related support, technology or other services from independent third parties, which may make our operations vulnerable if such third parties fail to perform adequately.
Failure to successfully implement, operate and maintain effective and efficient information systems with adequate technological capabilities, deficiencies or defects in the systems and related technology, or our failure to efficiently and effectively implement ongoing system upgrades or consolidate our information systems to eliminate redundant or obsolete applications, could result in increased legal and compliance risks and competitive disadvantages, among other things, which could have a material adverse effect on our business, financial condition, results of operations and reputation. For additional information on the risks we face in a highly competitive market, see the risk factor under the heading, "If we are unable to compete successfully..." If the information we rely upon to run our business was found to be inaccurate or unreliable or if we or third parties on which we rely fail to adequately maintain information systems and data integrity effectively, whether due to software deficiencies, human coding or implementation error or otherwise, we could experience difficulty meeting clinical outcome goals, face regulatory problems, including sanctions and penalties, incur increases in operating expenses or suffer other adverse consequences, any of which could be material. Moreover, failure to adequately protect and maintain the integrity of our information systems (including our networks) and data, or information systems and data hosted by third parties upon which we rely, could subject us to severe consequences as described in the risk factor under the heading "Privacy and information security laws are complex..."
Our billing systems, among others, are critical to our billing operations. This includes our systems for our dialysis clinics as well as our systems for our hospital services and our ancillary businesses, including our International business. If there are defects in our billing systems, or billing systems or services of third parties upon which we rely, we may experience difficulties in our ability to successfully bill and collect for services rendered, including, without limitation, a delay in collections, a reduction in the amounts collected, increased risk of retractions from and refunds to commercial and government payors, an increase in our provision for uncollectible accounts receivable and noncompliance with reimbursement laws and related requirements, any or all of which could materially adversely affect our results of operations.
In the clinical environment, a failure of our clinical systems, or the systems of our third-party service providers, to operate effectively could have a material adverse effect on our business, the clinical care provided to patients, results of operations, financial condition and cash flows. For example, in connection with claims for which at least part of the government's payments to us is based on clinical performance or patient outcomes or co-morbidities, if relevant clinical systems fail to accurately capture the data we report to CMS or we otherwise have data integrity issues with respect to the reported information, this could impact our payments from government payors.
Additionally, we expect the highly competitive environment in which we operate to become increasingly more competitive as the market evolves and new technologies are introduced. This dynamic environment requires continuous investment in new technologies and clinical applications. Machine learning and artificial intelligence are increasingly driving innovations in technology, and parts of our operations may employ robotics. If these rapidly evolving technologies or applications fail to operate as anticipated or do not perform as specified, including due to potential design defects and defects in the development of algorithms or other technologies, human error or otherwise, our clinical operations, business and reputation may be harmed. If we are unable to successfully maintain, enhance or operate our information systems, including through the implementation of such technologies or applications in our clinical operations and laboratory, we may be, among other things, unable to efficiently adapt to evolving laws and requirements, unable to remain competitive with others who successfully implement and advance this technology, subject to increased risk under existing laws, regulations and requirements that apply to our business, and our patients' safety may be adversely impacted, any of which could have a material adverse impact on our business, results of operations and financial condition and could materially harm our reputation. For additional detail, see the
discussion in the risk factor under the heading "Our business is subject to a complex set of governmental laws, regulations and other requirements..."
We may engage in acquisitions, mergers, joint ventures, noncontrolling interest investments, or dispositions, which may materially affect our results of operations, debt-to-capital ratio, capital expenditures or other aspects of our business, and, under certain circumstances, could have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation.
Our business strategy includes growth through acquisitions of dialysis centers and other businesses, as well as through entry into joint ventures. We may engage in acquisitions, mergers, joint ventures or dispositions or expand into new business lines or models, which may affect our results of operations, debt-to-capital ratio, capital expenditures or other aspects of our business. For example, in 2023 we closed a transaction with Medtronic, Inc. and one of its subsidiaries (collectively, Medtronic) to form a new, independent kidney care-focused medical device company (Mozarc). The transaction is expected to require us to fund additional consideration to Medtronic in certain circumstances. See the discussion under "Off-balance sheet arrangements and aggregate contractual obligations" in Part II Item 7. "Management's Discussion and Analysis of Financial Condition and Results of Operations."
There can be no assurance that we will be able to identify suitable acquisition or joint venture targets or merger partners or buyers for dispositions or that, if identified, we will be able to agree to terms with merger partners, acquire these targets or make these dispositions on acceptable terms or on the desired timetable. There can also be no assurance that we will be successful in completing any acquisitions, joint ventures, mergers or dispositions that we announce, executing new business lines or models or integrating any acquired business into our overall operations. There is no guarantee that we will be able to operate acquired businesses successfully as stand-alone businesses, or that any such acquired business will operate profitably or will not otherwise have a material adverse effect on our business, results of operations, financial condition and cash flows or materially harm our reputation. In addition, acquisition, merger or joint venture activity conducted as part of our overall growth strategy is subject to
antitrust and competition laws, and antitrust regulators can investigate future (or pending) and consummated transactions. These laws could impact our ability to pursue these transactions or our ability to consummate them on a timely basis; could require us to devote additional resources to potential transactions; and under certain circumstances, could result in mandated divestitures, among other things. If a proposed transaction or series of transactions is subject to challenge under antitrust or competition laws, we may incur substantial legal costs, management’s attention and resources may be diverted, and if we are found to have violated these or other related laws, regulations or requirements, we could suffer severe consequences that could have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation and stock price. For additional detail, see the risk factor under the heading "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation.requirements..." Further, we cannot be certain that key talented individuals at the business being acquired will continue to work for us after the acquisition or that they will be able to continue to successfully manage or have adequate resources to successfully operate any acquired business. In addition, certain of our acquired dialysis centers and facilities have been in service for many years, which may result in a higher level of maintenance costs. Further, our facilities, equipment and information technology may need to be improved or renovated to maintain or increase operational efficiency, compete for patients and medical directors, or meet changing regulatory requirements. Increases in maintenance costs and/or capital expenditures could have, under certain circumstances, a material adverse effect on our business, results of operations, financial condition and cash flows.
Businesses we acquire may have unknown or contingent liabilities or liabilities that are in excess of the amounts that we originally estimated, and may have other issues, including, without limitation, those related to internal controlscontrol over financial reporting or issues that could affect our ability to comply with healthcare laws and regulations and other laws applicable to our expanded business, which could harm our reputation. As a result, we cannot make any assurances that the acquisitions we consummate will be successful. Although we generally seek indemnification from the sellers of businesses we acquire for matters that are not properly disclosed to us, we are not always successful. In addition, even in cases where we are able to obtain indemnification, we may discover liabilities greater than the contractual limits, the amounts held in escrow for our benefit (if any), or the financial resources of the indemnifying party. In the event that we are responsible for liabilities substantially in excess of any amounts recovered through rights to indemnification or alternative remedies that might be available to us, or any applicable insurance, we could suffer severe consequences that would have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation.
In addition, under the terms of the equity purchase agreement for the DMG sale (the DMG sale agreement), we agreed to certain indemnification obligations, including with respect to claims for breaches of our representations and warranties regarding compliance with law, litigation, absence of undisclosed liabilities, employee benefit matters, labor matters, or taxes, among others, and other claims for which we provided the buyer with a special indemnity. As a result, we may become obligated to make payments to the buyer relating to our previous ownership and operation of the DMG business. Any such post-closing liabilities and required payments under the DMG sale agreement, or otherwise, or in connection with any other
past or future disposition of material assets or businesses could individually or in the aggregate have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation.
Additionally, joint ventures or noncontrolling interest investments, including, without limitation, our Asia Pacific joint venture, and minority investments inherently involve a lesser degree of control over business operations, thereby potentially increasing the financial, legal, operational and/or compliance risks associated with the joint venture or minoritynoncontrolling interest investment. In addition, we may be dependent on joint venture partners, controlling shareholders or management who may have business interests, strategies or goals that are inconsistent with ours. Business decisions or other actions or omissions of the joint venture partner, controlling shareholders or management may require us to make capital contributions or necessitate other payments, result in litigation or regulatory action against us, result in reputational harm to us or adversely affect the value of our investment or partnership, among other things. In addition, we have potential obligations to purchase the interests held by third parties in many of our joint ventures as a result of put provisions that are exercisable at the third party's discretion within specified time periods, pursuant to the applicable agreement. If these put provisions were exercised, we would be required to purchase the third party owner's equity interest, generally at the appraised market value. There can be no assurances that these joint ventures and/or minoritynoncontrolling interest investments, including, without limitation, our Asia Pacific joint venture, ultimately will be successful.
If certain of our suppliers do not meet our needs, if there are material price increases on supplies, if we are not reimbursed or adequately reimbursed for drugs we purchase or if we are unable to effectively access new technology or superior products, it could negatively impact our ability to effectively provide the services we offer and could have a material adverse effect on our business, results of operations, financial condition and cash flows.
We have significant suppliers, with a substantial portion of our total vendor spend concentrated with a limited number of third party suppliers. These third party suppliers include, without limitation, suppliers of pharmaceuticals that may be the primary source of products critical to the services we provide, or to which we have committed obligations to make purchases,
sometimes at particular prices. If any of these suppliers do not meet our needs for the products they supply, including, without limitation, in the event of a product recall, shortage or dispute, and we are not able to find adequate alternative sources, if we experience material price increases from these suppliers that we are unable to mitigate, or if some of the drugs that we purchase from our suppliers are not reimbursed or not adequately reimbursed by commercial or government payors, or if we are unable to secure products, including pharmaceuticals at competitive rates and within the desired time frame, it could have a material adverse impact on our business, results of operations, financial condition and cash flows. In addition, the technology related to the products critical to the services we provide is subject to new developments which may result in superior products. If we are not able to access superior products on a cost-effective basis, either due to competitive conditions in the marketplace or otherwise, or if suppliers are not able to fulfill our requirements for such products, we could face patient attrition and other negative consequences which could have a material adverse effect on our business, results of operations, financial condition and cash flows.
Expansion of our operations to and offering our services in markets outside of the U.S. subjects us to political, economic, legal, operational and other risks that could have a material adverse effect on our business, results of operations, financial condition, cash flows and reputation.
We are continuing to expand our operations by offering our services and entering new lines of business in certain markets outside of the U.S., which increases our exposure to the inherent risks of doing business in international markets. Depending on the market, these risks include those relating to:
•changes in the local economic environment;
•political instability, armed conflicts or terrorism;
•public health crises, such as pandemics or epidemics, including the COVID-19 pandemic;
•social changes;
•intellectual property legal protections and remedies;
•trade regulations;
•procedures and actions affecting approval, production, pricing, reimbursement and marketing of products and services;
•foreign currency;
•additional U.S. and foreign taxes;
•export controls;
•antitrust and competition laws and regulations;
•lack of reliable legal systems which may affect our ability to enforce contractual rights;
•changes in local laws or regulations, or interpretation or enforcement thereof;
•potentially longer ramp-up times for starting up new operations and for payment and collection cycles;
•financial and operational, and information technology systems integration;
•failure to comply with U.S. laws, such as the FCPA, or local laws that prohibit us, our partners, or our partners' or our agents or intermediaries from making improper payments to foreign officials or any third party for the purpose of obtaining or retaining business; and
•data and privacy restrictions.
Issues relating to the failure to comply with applicable non-U.S. laws, requirements or restrictions may also impact our domestic business and/or raise scrutiny on our domestic practices.
Additionally, some factors that will be critical to the success of our international business and operations will be different than those affecting our domestic business and operations. For example, conducting international operations requires us to devote significant management resources to implement our controls and systems in new markets, to comply with local laws and regulations, including to fulfill financial reporting and records retention requirements among other things, and to overcome the numerous new challenges inherent in managing international operations, including, without limitation, challenges based on
differing languages and cultures, challenges related to establishing clinical operations in differing regulatory and compliance environments, and challenges related to the timely hiring, integration and retention of a sufficient number of skilled personnel to carry out operations in an environment with which we are not familiar.
Any expansion of our international operations through acquisitions or through organic growth could increase these risks. Additionally, while we may invest material amounts of capital and incur significant costs in connection with the growth and development of our international operations, including to start up or acquire new operations, we may not be able to operate them profitably on the anticipated timeline, or at all.
These risks could have a material adverse effect on our business, results of operations, financial condition, cash flows and could materially harm our reputation.
If our joint ventures were found to violate the law, we could suffer severe consequences that would have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation.
As of December 31, 2020,2023, we owned a controlling interest in numerous dialysis-related joint ventures, which represented approximately 27%29% of our U.S. dialysis revenues for the year ended December 31, 2020.2023. In addition, we also owned noncontrolling equity investments in several other dialysis relateddialysis-related joint ventures. We expect to continue to increase the number of our joint ventures. Many of our joint ventures with physicians or physician groups also have certain physician owners providing medical director services to centers we own and operate. Because our relationships with physicians are governed by the federal and state anti-kickback statutes, we have sought to structure our joint venture arrangements to satisfy as many federal safe harbor requirements as we believe are commercially reasonable. Our joint venture arrangements do not satisfy all of the elements of any safe harbor under the federal Anti-Kickback Statute, however, and therefore are susceptible to government scrutiny. Additionally, our joint ventures and minority investments inherently involve a lesser degree of control over business operations, thereby potentially increasing the financial, legal, operational and/or compliance risks associated with the joint venture or minority investment. If our joint ventures are found to violate applicable laws or regulations, we could suffer severe consequences that would have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation. For additional information on these risks, see the risk factors under the headings "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation"requirements...;" and "We may engage in acquisitions, mergers, joint ventures, noncontrolling interest investments, or dispositions,dispositions..."
Our aspirations, goals and disclosures related to ESG matters expose us to numerous risks, including without limitation risks to our reputation and stock price.
We have a longstanding ESG program and have engaged with key stakeholders to develop ESG focus areas and to set ESG-related goals, many of which may materially affectare aspirational. We have set and disclosed these focus areas, goals and related objectives as part of our resultscontinued commitment to ESG matters, but our goals and objectives reflect our current plans and aspirations and are not guarantees that we will be able to achieve them. Our efforts to accomplish and accurately report on these goals and objectives present numerous operational, reputational, financial, legal and other risks, certain of operations, debt-to-capital ratio, capital expenditureswhich are outside of our control, and could have, under certain circumstances, a material adverse impact on us, including on our reputation and stock price. Examples of such risks include, among others: the availability and cost of low- or non-carbon-based energy sources and technologies for us and our vendors, evolving regulatory requirements affecting ESG standards, frameworks and disclosures, including evolving standards for measuring and reporting on related metrics, the availability of suppliers that can meet our sustainability and other standards, our ability to recruit, develop and retain diverse talent in our labor markets, and our ability to grow our home based dialysis business.
If our ESG practices do not meet evolving investor or other aspects ofstakeholder expectations and standards, then our reputation, our ability to attract or retain employees and our attractiveness as an investment, business partner or acquirer could be negatively impacted. Similarly, our failure or perceived failure to adequately pursue or fulfill our goals and objectives or to satisfy various reporting standards within the timelines we announce, or at all, could also have similar negative impacts and expose us to other risks, which under certain circumstances could be material. If we are not able to adequately recognize and respond to the rapid and ongoing developments and governmental and social expectations relating to ESG matters, this failure could result in missed corporate opportunities, additional regulatory, social or other scrutiny of us, the imposition of unexpected costs, or damage to our reputation with governments, patients, teammates, third parties and the communities in which we
operate, which in turn could have a material adverse effect on our business, financial condition, cash flows and results of operations financial condition and cash flows and could materially harmcause the market value of our reputation."common stock to decline.
There are significant risks associated with estimating the amount of dialysis revenues and related refund liabilities that we recognize, and if our estimates of revenues and related refund liabilities are materially inaccurate, it could impact the timing and the amount of our revenues recognition or have a material adverse effect on our business, results of operations, financial condition and cash flows.
There are significant risks associated with estimating the amount of U.S. dialysis net patient servicesservice revenues and related refund liabilities that we recognize in a reporting period. The billing and collection process is complex due to ongoing insurance coverage changes, geographic coverage differences, differing interpretations of contract coverage and other payor issues, such as ensuring appropriate documentation. Determining applicable primary and secondary coverage for approximately 204,200200,800 U.S. patients at any point in time, together with the changes in patient coverage that occur each month, requires complex, resource-intensive processes. Errors in determining the correct coordination of benefits may result in refunds to payors. Revenues associated with Medicare and Medicaid programs are also subject to estimating risk related to the amounts not paid by the primary government payor that will ultimately be collectible from other government programs paying secondary coverage, the patient's commercial health plan secondary coverage or the patient. Collections, refunds and payor retractions typically continue to occur for up to three years and longer after services are provided. We generally expect our range of U.S. dialysis net patient servicesservice revenues estimating risk to be within 1% of net revenues for the segment. If our estimates of U.S. dialysis net patient servicesservice revenues and related refund liabilities are materially inaccurate, it could impact the timing and the amount of our revenues recognition and have a material adverse impact on our business, results of operations, financial condition and cash flows.
Our ancillary services and strategic initiatives, including, without limitation, our international operations, that we operate or invest in now or in the future may generate losses and may ultimately be unsuccessful. In the event that one
or more of these activities is unsuccessful, our business, results of operations, financial condition and cash flows may be negatively impacted and we may have to write off our investment and incur other exit costs.
Our ancillary services and strategic initiatives are subject to many of the same risks, regulations and laws, as described in the risk factors related to our dialysis business set forth in this Part I, Item 1A, and are also subject to additional risks, regulations and laws specific to the nature of the particular strategic initiative. We expect to add additional service offerings to our business and pursue additional strategic initiatives in the future as circumstances warrant, which could include healthcare services not related to dialysis. Many of these initiatives require or would require investments of both management and financial resources and can generate significant losses for a substantial period of time and may not become profitable in the expected timeframe or at all. There can be no assurance that any such strategic initiative will ultimately be successful. Any significant change in market conditions or business performance, including, without limitation, as a result of the COVID-19 pandemic, or in the political, legislative or regulatory environment, may impact the performance or economic viability of any of these strategic initiatives.
If any of our ancillary services or strategic initiatives, including our international operations, are unsuccessful, it would have a negative impact on our business, results of operations, financial condition and cash flows, and we may determine to exit that line of business. We could incur significant termination costs if we were to exit certain of these lines of business. In addition, we may incur a material write-off or an impairment of our investment, including, without limitation, goodwill or other assets, in one or more of our ancillary services or strategic initiatives. In that regard, we have taken, and may in the future take, impairment and restructuring charges in addition to those described above related to our ancillary services and strategic initiatives, including, without limitation, in our international and pharmacy businesses.
If a significant number of physicians were to cease referring patients to our dialysis centers, whether due to law, rule or regulation, new competition, a perceived decrease in the quality of service levels at our centers or other reasons, it would have a material adverse effect on our business, results of operations, financial condition and cash flows.
Physicians, including medical directors, choose where they refer their patients. Some physicians prefer to have their patients treated at dialysis centers where they or other members of their practice supervise the overall care provided as medical director of the center. As a result, referral sources for many of our centers include the physician or physician group providing medical director services to the center.
Our medical director contracts are for fixed periods, generally ten years, and at any given time a large number of them could be up for renewal at the same time. Medical directors have no obligation to extend their agreements with us and, under certain circumstances, our former medical directors may choose to provide medical director services for competing providers or establish their own dialysis centers in competition with ours. Neither our current nor former medical directors have an obligation to refer their patients to our centers. In addition, there are a number of new entrants into the dialysis space, and physicians, including medical directors, may refer patients to these new entrants rather than the Company.
The aging of the nephrologist population and opportunities presented by our competitors may negatively impact a medical director's decision to enter into or extend his or her agreement with us. Moreover, a perceived decrease in the quality of service levels at our centers or different affiliation models in the changing healthcare environment that limit a nephrologist's choice in where he or she can refer patients, such as an increase in the number of physicians becoming employed by hospitals, may limit a nephrologist's ability or desire to refer patients to our centers or otherwise negatively impact treatment volumes.
In addition, if the terms of any existing agreement are found to violate applicable laws, there can be no assurances that we would be successful in restructuring the relationship, which would lead to the early termination of the agreement. If we are unable to obtain qualified medical directors to provide supervision of the operations and care provided at our dialysis centers, it could affect physicians' desire to refer patients to our dialysis centers. If a significant number of physicians were to cease referring patients to our dialysis centers, it would have a material adverse effect on our business, results of operations, financial condition and cash flows.
If our labor costs continue to rise, including due to shortages, changes in certification requirements and/or higher than normal turnover rates in skilled clinical personnel; or currently pending or future governmental laws, rules, regulations or initiatives impose additional requirements or limitations on our operations or profitability; or, if we are unable to attract and retain key leadership talent, we may experience disruptions in our business operations and increases in operating expenses, among other things, which could have a material adverse effect on our business, results of operations, financial condition and cash flows.
We face increasing labor costs generally, and in particular, we continue to face increased labor costs and difficulties in hiring nurses due to a nationwide shortage of skilled clinical personnel that has been exacerbated by the ongoing COVID-19 pandemic. We have incurred and expect to continue to incur increased labor costs and experience staffing challenges related to
COVID-19 while the pandemic persists, the extent of which will depend on the severity and duration of the pandemic, among other things. For additional discussion of the risks facing us related to COVID-19, see the risk factor under the heading "We face various risks related to the dynamic and evolving novel coronavirus pandemic, any of which may have a material adverse impact on us."We compete for nurses with hospitals and other healthcare providers. This nursing shortage may limit our ability to expand our operations. Furthermore, changes in certification requirements can impact our ability to maintain sufficient staff levels, including to the extent our teammates are not able to meet new requirements, among other things. In addition, if we experience a higher than normal turnover rate for our skilled clinical personnel, our operations and treatment growth may be negatively impacted, which could adversely affect our business, results of operations, financial condition and cash flows. We also face competition in attracting and retaining talent for key leadership positions. If we are unable to attract and retain qualified individuals, we may experience disruptions in our business operations, including, without limitation, our ability to achieve strategic goals, which could have a material adverse effect on our business, results of operations, financial condition and cash flows. For additional information on these risks, see the risk factors under the headings "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation;" and "Changes in federal and state healthcare legislation or regulations could have a material adverse effect on our business, results of operations, financial condition and cash flows."
Our business is labor intensive and could be materially adversely affected if we are unable to attract and retain employees or if union organizing activities or legislative or other changes result in significant increases in our operating costs or decreases in productivity.
Our business is labor intensive, and our financial and operating results have been and continue to be subject to variations in labor-related costs, productivity and the number of pending or potential claims against us related to labor and employment practices. Political or other efforts at the national or local level could result in actions or proposals that increase the likelihood of success of union organizing activities at our facilities and ongoing union organizing activities at our facilities could continue or increase for other reasons. We could experience an upward trend in wages and benefits and labor and employment claims, including, without limitation, the filing of class action suits, or adverse outcomes of such claims, or face work stoppages. In addition, we are and may continue to be subject to targeted corporate campaigns by union organizers in response to which we have been and may continue to be required to expend substantial resources, both time and financial. Any of these events or circumstances could have a material adverse effect on our employee relations, treatment growth, productivity, business, results of operations, financial condition and cash flows.
Failing to effectively maintain, operate or upgrade our information systems or those of third-party service providers upon which we rely, including, without limitation, our clinical, billing and collections systems could materially adversely affect our business, results of operations, financial condition and cash flows.
Our business depends significantly on effective information systems. Our information systems require an ongoing commitment of significant resources to maintain, upgrade and enhance existing systems and develop or contract for new systems in order to keep pace with continuing changes in information processing technology, emerging cybersecurity risks and threats, evolving industry, legal and regulatory standards and requirements, new models of care, and other changes in our business, among other things. For example, the provisions related to data interoperability, information blocking, and patient access in the Cures Act include, among other things, changes to the Office of the National Coordinator for Health Information Technology’s (ONC's) Health IT Certification Program and requirements that CMS-regulated payors make relevant claims/care data and provider directory information available through standardized patient access and provider directory application programming interfaces (APIs) that connect to provider electronic health records. We have made and continue to make investments in building data interoperability capabilities, including as part of building on our integrated care capabilities as noted above, and continue to evaluate the potential impact of the CMS and ONC final rules. Any failure to adequately comply with these rules may adversely impact our Medicare business, our ability to scale our integrated care business and our ability to compete with certain smaller and/or non-traditional providers taking advantage of an asymmetrical environment with respect to data and/or regulatory requirements given our status as an ESRD service provider. There can be no assurances that the implementation of planned enhancements to our systems, such as our implementation of these data interoperability provisions or our other efforts that are currently ongoing to upgrade and better integrate our clinical systems, will be successful or that we will ultimately realize anticipated benefits from investments in new or existing information systems. In addition, we may from time to time obtain significant portions of our systems-related support, technology or other services from independent third parties, which may make our operations vulnerable if such third parties fail to perform adequately.
Failure to successfully implement, operate and maintain effective and efficient information systems with adequate technological capabilities, deficiencies or defects in the systems and related technology, or our failure to efficiently and effectively consolidate our information systems to eliminate redundant or obsolete applications, could result in competitive
disadvantages, which could have a material adverse effect on our business, financial condition and results of operations. For additional information on the risks we face in a highly competitive market, see the risk factor under the heading, "If we are unable to compete successfully, including, without limitation, implementing our growth strategy and/or retaining patients and physicians willing to serve as medical directors, it could materially adversely affect our business, results of operations, financial condition and cash flows." If the information we rely upon to run our business was found to be inaccurate or unreliable or if we or third parties on which we rely fail to adequately maintain information systems and data integrity effectively, whether due to software deficiencies, human coding or implementation error or otherwise, we could experience difficulty meeting clinical outcome goals, face regulatory problems, including sanctions and penalties, incur increases in operating expenses or suffer other adverse consequences, any of which could be material. Moreover, failure to adequately protect and maintain the integrity of our information systems (including our networks) and data, or information systems and data hosted by third parties upon which we rely, could subject us to severe consequences as described in the risk factor under the heading "Privacy and information security laws are complex, and if we fail to comply with applicable laws, regulations and standards, including with respect to third-party service providers that utilize sensitive personal information on our behalf, or if we fail to properly maintain the integrity of our data, protect our proprietary rights to our systems or defend against cybersecurity attacks, we may be subject to government or private actions due to privacy and security breaches or suffer losses to our data and information technology assets, any of which could have a material adverse effect on our business, results of operations, financial condition and cash flows or materially harm our reputation."
Our billing system, among others, is critical to our billing operations. If there are defects in the billing system, or billing systems or services of third parties upon which we rely, we may experience difficulties in our ability to successfully bill and collect for services rendered, including, without limitation, a delay in collections, a reduction in the amounts collected, increased risk of retractions from and refunds to commercial and government payors, an increase in our provision for uncollectible accounts receivable and noncompliance with reimbursement laws and related requirements, any or all of which could materially adversely affect our results of operations.
In the clinical environment, a failure of our clinical systems, or the systems of our third-party service providers, to operate effectively could have a material adverse effect on our business, the clinical care provided to patients, results of operations, financial condition and cash flows. For example, in connection with claims for which at least part of the government's payments to us is based on clinical performance or patient outcomes or co-morbidities, if relevant clinical systems fail to accurately capture the data we report to CMS or we otherwise have data integrity issues with respect to the reported information, this could impact our payments from government payors as well as our ability to retain funds paid to us based on the inaccurate information.
Additionally, we expect the highly competitive environment in which we operate to become increasingly more competitive as the market evolves and new technologies are introduced. This dynamic environment requires continuous investment in new technologies and clinical applications. Machine learning and artificial intelligence are increasingly driving innovations in technology, and parts of our operations may employ robotics. If these technologies or applications fail to operate as anticipated or do not perform as specified, including due to potential design defects and defects in the development of algorithms or other technologies, human error or otherwise, our clinical operations, business and reputation may be harmed. If we are unable to successfully maintain, enhance or operate our information systems, including through the implementation of such technologies or applications in our clinical operations and laboratory, we may be, among other things, unable to efficiently adapt to evolving laws and requirements, unable to remain competitive with others who successfully implement and advance this technology, subject to increased risk under existing laws, regulations and requirements that apply to our business, and our patients' safety may be adversely impacted, any of which could have a material adverse impact on our business, results of operations and financial condition and could materially harm our reputation. For additional detail, see the discussion in the risk factor under the heading "Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputation.”
General Risk Factors
The level of our current and future debt could have an adverse impact on our business, and our ability to generate cash to service our indebtedness and for other intended purposes and our ability to maintain compliance with debt covenants depends on many factors beyond our control.
We have a substantial amount of indebtedness outstanding and we may incur substantial additional indebtedness in the future, including indebtedness incurred to finance repurchases of our common stock pursuant to our share repurchase authorization discussed under "Stock Repurchases""Stock Repurchases" in Part II Item 7, 7. ""Management's Discussion and Analysis of Financial Condition and Results of Operations." As described in Note 1312 to the consolidated financial statements included in this report,
we are party to a senior secured credit agreement (the(as amended, the Credit Agreement), which consists of an up to $1.5 billion secured revolving line of credit, a secured term loan AA-1 facility and a secured term loan B-1 facility and a secured revolving line of credit in the aggregate principal amount of $1 billion.facility. Our long-term indebtedness also includes $3.250$4.250 billion aggregate principal amount of senior notes.
If we are unable to generate sufficient cash to service our indebtedness and for other intended purposes, it could, for example:
•make it difficult for us to make payments on our debt;
•increase our vulnerability to general adverse economic and industry conditions;
•require us to dedicate a substantial portion of our cash flows from operations to payments on our indebtedness, thereby reducing the availability of our cash flow to fund working capital, capital expenditures, acquisitions and investments, repurchases of stock at the levels intended or announced, or at all, and other general corporate purposes;
•limit our flexibility in planning for, or reacting to, changes in our business and the markets in which we operate;
•expose us to interest rate volatility that could adversely affect our business, results of operations, financial condition and cash flows, and our ability to service our indebtedness;
•place us at a competitive disadvantage compared to our competitors that have less debt; and
•limit our ability to borrow additional funds, or to refinance existing debt on favorable terms when otherwise available or at all.
Our senior secured credit facilities bear, and other indebtedness we may incur in the future may bear, interest at a variable rate. As a result, at any given time interest rates on the senior secured credit facilities and any other variable rate debt could be higher or lower than current levels. If interest rates increase, our debt service obligations on our variable rate indebtedness will increase even though the amount borrowed remains the same, and therefore net income and associated cash flows, including cash available for servicing our indebtedness, will correspondingly decrease.
Our indebtedness levels and the required payments on such indebtedness may also be impacted by expected reforms related to LIBOR. The variable interest rates payable under our senior secured credit facilities arehave historically been linked to LIBOR as the benchmark for establishing such rates. The LIBOR benchmark has beenrate used in our senior secured credit facilities ceased to be available starting June 30, 2023. Prior to that date, we transitioned all the subject of recent national, international and other regulatory guidance and reform proposals. The reforms may causedebt from our senior secured credit facilities from LIBOR to perform differently from the past and LIBOR may ultimately cease to exist after 2023. The U.S. Federal Reserve, in conjunction with the Alternative Reference Rates Committee,Secured Overnight Financing Rate (SOFR). SOFR is a steering committee comprisedbroad measure of among other entities, large U.S. financial institutions, is considering replacing U.S. dollar LIBOR with a new index that measures the cost of borrowing cash overnight backedcollateralized by U.S. Treasury securities (SOFR). Whether or notsecurities. The SOFR or any other potential alternative reference rate attains market traction as a LIBOR replacement rate remains in question. Our senior secured credit facilities include mechanics to facilitate the adoption by us and our lenders of an alternative benchmark rate for use in place of LIBOR; however, no assurance can be made that we and our lenders will agree on such an alternative rate and, even if agreed upon, such alternative rate may not perform in a manner similar to LIBOR and may result in interest rates that are higher or lower than those that would have resulted had LIBOR remained in effect.effect, which could impact our cost of capital.
Our ability to make payments on our indebtedness, to fund planned capital expenditures and expansion efforts, including, without limitation, any strategic acquisitions or investments we may make in the future, to repurchase our stock at the levels intended or announced and to meet our other liquidity needs such as for working capital or capital expenditures, will depend on our ability to generate cash. This depends not only on the success of our business but is also subject to economic, financial, competitive, regulatory and other factors that are beyond our control. We cannot provide assurances that our business will generate sufficient cash flows from operations in the future or that future borrowings will be available to us in amounts sufficient to enable us to service our indebtedness or to fund our working capital and other liquidity needs, including those described above. If we are unable to generate sufficient funds to service our outstanding indebtedness or to meet our working capital or other liquidity needs, including those described above, we would be required to refinance, restructure, or otherwise amend some or all of such indebtedness, sell assets, change or reduce our intended or announced uses or strategy for capital deployment, including, without limitation, for stock repurchases, reduce capital expenditures, planned expansions or other
strategic initiatives, or raise additional cash through the sale of our equity or equity-related securities. We cannot make any assurances that any such refinancing, restructurings, amendments, sales of assets, or issuances of equity or equity-related securities can be accomplished or, if accomplished, will be on favorable terms or would raise sufficient funds to meet these obligations or our other liquidity needs.
In addition, we may continue to incur indebtedness in the future, and the amount of that additional indebtedness may be substantial. Although the Credit Agreement includes covenants that could limit our indebtedness, we currently have, and expect to continue to have, the ability to incur substantial additional debt. The risks described in this risk factor could intensify as new
debt is added to current debt levels or if we incur any new debt obligations that subject us to restrictive covenants that limit our financial and operational flexibility. Any breach or failure to comply with any of these covenants could result in a default under our indebtedness. Other risks related to our ability to generate sufficient cash to service our indebtedness and for other intended purposes, include, for example:
•increase our vulnerability to general adverse economic and industry conditions;
•limit our flexibility in planning for, or reacting to, changes in our business and the markets in which we operate;
•expose us to interest rate volatility that could adversely affect our business, results of operations, financial condition and cash flows, and our ability to service our indebtedness;
•place us at a competitive disadvantage compared to our competitors that have less debt; and
•limit our ability to borrow additional funds, or to refinance existing debt on favorable terms when otherwise available or at all.
Any failure to pay any of our indebtedness when due or any other default under our credit facilities or our other indebtedness could have a material adverse effect on our business, results of operations, financial condition and cash flows, and could trigger cross default or cross acceleration provisions in our other debt instruments, thereby permitting the holders of that other indebtedness to demand immediate repayment or cease to make future extensions of credit, and, in the case of secured indebtedness, to take possession of and sell the collateral securing such indebtedness to satisfy our obligations.
The borrowings under our senior secured credit facilities and senior indentures are guaranteed by certain of our domestic subsidiaries, and borrowings under our senior secured credit facilities are secured by substantially all of our and certain of our domestic subsidiaries' assets. Such guarantees and the fact that we have pledged such assets may make it more difficult and expensive for us to make, or under certain circumstances could effectively prevent us from making, additional secured and unsecured borrowings.
We could be subject to adverse changes in tax laws, regulations and interpretations or challenges to our tax positions.
We are subject to tax laws and regulations of the U.S. federal, state and local governments as well as various foreign jurisdictions. We compute our income tax provision based on enacted tax rates in the jurisdictions in which we operate. As the tax rates vary among jurisdictions, a change in earnings attributable to the various jurisdictions in which we operate could result in an unfavorable or favorablea change in our overall tax provision.
Changes in tax laws or regulations may be proposed or enacted that could adversely affect our overall tax liability. There can be no assurance that changes in tax laws or regulations, both within the U.S.domestic and the otherforeign jurisdictions in which we operate, will not materially and adversely affect our effective tax rate, tax payments, results of operations, financial condition and cash flows. For example, changes to the political environment related to the most recent U.S. election cycle increase the likelihood that changes in taxation and related regulations could have a material adverse impact on our results of operations and financial condition. Similarly, changes in tax laws and regulations that impact our patients, business partners and counterparties or the economy generally may also impact our results of operations, financial condition and cash flows.
In addition, tax laws and regulations are complex and subject to varying interpretations, and any significant failure to comply with applicable tax laws and regulations in all relevant jurisdictions could give rise to material penalties and liabilities. We are regularly subject to audits by various tax authorities. For example, our current audits include an audit by the Internal Revenue Service for the years 2014–2017, and itIt is possible that the final determination of this and any othersuch tax audits and any related litigation could be materially different from our historical income tax provisions and accruals. Any changes in enacted tax laws, rules or regulatory or judicial interpretations; any adverse development or outcome in connection with tax audits in any jurisdiction; or any change in the pronouncements relating to accounting for income taxes could materially and adversely impact our effective tax rate, tax payments, results of operations, financial condition and cash flows.
We may be subject to liability claims for damages and other expenses that are not covered by insurance or exceed our existing insurance coverage that could have a material adverse effect on our business, results of operations, financial condition, cash flows and could materially harm our reputation.
Our operations and how we manage our business may subject us, as well as our officers and directors to whom we owe certain defense and indemnity obligations, to litigation and liability. Our business, profitability and growth prospects could suffer if we face negative publicity or we pay damages or defense costs in connection with a claim that is outside the scope or limits of coverage of any applicable insurance coverage, including, without limitation, claims related to adverse patient events, cybersecurity incidents, contractual disputes, antitrust and competition laws and regulations, professional and general liability and directors' and officers' duties. In addition, we have received notices of claims from commercial payors and other third parties, as well as subpoenas and CIDs from the federal government, related to our business practices, including, without limitation, our historical billing practices and the historical billing practices of acquired businesses. Although the ultimate outcome of these claims cannot be predicted, an adverse result with respect to one or more of these claims could have a material adverse effect on our business, results of operations, financial condition and cash flows, and could materially harm our reputation. We maintain insurance coverage for those risks we deem are appropriate to insure against and make determinations about whether to self-insure as to other risks or layers of coverage. However, a successful claim, including, without limitation, a professional liability, malpractice or negligence claim or a claim related to a cybersecurity incident, which is in excess of any applicable insurance coverage, that is outside the scope or limits of any applicable insurance coverage, or that is subject to our self-insurance retentions, could have a material adverse effect on our business, results of operations, financial condition, cash flows and reputation.
In addition, if our costs of insurance and claims increase, then our earnings could decline. Market rates for insurance premiums and deductibles have been steadily increasing. Our business, results of operations, financial condition and cash flows could be materially and adversely affected by any of the following:
•the collapse or insolvency of our insurance carriers;
•further increases in premiums and deductibles;
•increases in the number of liability claims against us or the cost of settling or trying cases related to those claims;
•obtaining insurance with exclusions for things such as communicable diseases; or
•an inability to obtain one or more types of insurance on acceptable terms, if at all.
If we fail to successfully maintain an effective internal control over financial reporting, the integrity of our financial reporting could be compromised, which could have a material adverse effect on our ability to accurately report our financial results, the market's perception of our business and our stock price.
The integration of acquisitions and addition of new business lines into our internal control over financial reporting has required and will continue to require significant time and resources from our management and other personnel and has increased, and is expected to continue to increase our compliance costs. Failure to maintain an effective internal control environment could have a material adverse effect on our ability to accurately report our financial results, the market's perception of our business and our stock price. In addition, we could be required to restate our financial results in the event of a significant failure of our internal control over financial reporting or in the event of inappropriate application of accounting principles.
Deterioration in economic conditions, disruptions in the financial markets or the effects of natural or other disasters, political instability, public health crises or adverse weather events such as hurricanes, earthquakes, fires or flooding could have a material adverse effect on our business, results of operations, financial condition and cash flows.
Deterioration in economic conditions, whether in connection with the COVID-19 pandemic or otherwise, could have a material adverse effect on our business, results of operations, financial condition and cash flows. Among other things, the potential decline in federal and state revenues that may result from such conditions may create additional pressures to contain or reduce reimbursements for our services from Medicare, Medicaid and other government sponsored programs. Increases in job losses in the U.S. as a result of adverse economic conditions, including economic deterioration due to the ongoing COVID-19 pandemic, could result in a smaller percentage of our patients being covered by an employer group health plan and a larger percentage being covered by lower paying Medicare and Medicaid programs. Employers may also select more restrictive commercial plans with lower reimbursement rates. To the extent that payors are negatively impacted by a decline in the economy, we may experience further pressure on commercial rates, a slowdown in collections and a reduction in the amounts we expect to collect. In addition, uncertainty in the financial markets could adversely affect the variable interest rates payable under our credit facilities or could make it more difficult to obtain or renew such facilities or to obtain other forms of financing in the future, if at all. For additional information regarding the risks presented by the COVID-19 pandemic, see the discussion in the risk factor under the heading "We face various risks related to the dynamic and evolving novel coronavirus pandemic, any of which may have a material adverse impact on us." For additional information regarding the risks related to our indebtedness, see the discussion in the risk factor under the heading "The level of our current and future debt could have an adverse impact on our business, and our ability to generate cash to service our indebtedness and for other intended purposes and our ability to maintain compliance with debt covenants depends on many factors beyond our control."
Moreover, as of December 31, 2020, we had approximately $6.919 billion of goodwill recorded on our consolidated balance sheet. We account for impairments of goodwill in accordance with the provisions of applicable accounting guidance, and record impairment charges when and to the extent a reporting unit's carrying amount is determined to exceed its estimated fair value. We use a variety of factors to assess changes in the financial condition, future prospects and other circumstances concerning our businesses and to estimate their fair value when applicable. These assessments and the related valuations can involve significant uncertainties and require significant judgment on various matters, some of which could be subject to reasonable disagreement.
Should our revenues and financial results be materially, unfavorably impacted due to, among other things, a worsening of the economic and employment conditions in the United States that negatively impacts reimbursement rates or the availability of insurance coverage for our patients, we may incur future charges to recognize impairment in the carrying amount of our goodwill and other intangible assets, which could have a material adverse effect on our business, results of operation and financial condition.
Further, someSome of our operations, including our clinical laboratory, dialysis centers and other facilities, may be adversely impacted by the effects of natural or other disasters, political instability, public health crises such as global pandemics or epidemics, including the COVID-19 pandemic, or adverse weather events such as hurricanes, earthquakes, fires or flooding. Each of these effects and risks may be further intensified by the increasing impact of climate change on a global scale. In addition, these risks are particularly heightened for our patients in part because individuals with chronic illness may be more susceptible to the adverse effects of epidemics or other public health crises and also because any natural or other disaster, political instability or adverse weather event that disrupts or limits the operation of any of our centers or other facilities or services may delay or otherwise impact the critical services we provide to dialysis patients. Further, any such event or other occurrence that results in a failure of the fitness of our clinical laboratory, dialysis centers and related operations and/or other facilities or otherwise adversely impacts the safety of our teammates or patients at any of those locations could lead us to face adverse consequences, including, without limitation, the potential loss of data, including PHI or PII, compliance or regulatory investigations, any of which could materially impact our business, results of operationoperations and financial condition, and could materially harm our reputation. For example, our clinical laboratory is located in Florida, a state that has in the past experienced and may in the future experience hurricanes. Natural or other disasters or adverse weather events could significantly damage or destroy our facilities, disrupt operations, increase our costs to maintain operations and require substantial expenditures and recovery time to fully resume operations. In addition, as the effects of climate change progressively surface, such as through potential increases in the frequency and intensity of natural or other disasters or adverse weather events or through laws or regulations adopted in response, we may face increased costs associated with operating our clinics, including, without limitation, with respect to supplies of water or energy costs.
Our presence in markets outside the U.S. may increase our exposure to these and similar risks related to natural disasters, public health crises, political instability, climate change or other catastrophic events outside our control. For additional information regarding the risks related to our international business, see the discussion in the risk factor under the heading "Expansion of our operations to and offering our services in markets outside of the U.S. subjects us to political, economic, legal, operational and other risks that could have a material adverse effect on our business, results of operations, financial condition, cash flows and reputation.U.S...."
Any or all of these factors, as well as other consequences of these events, none of which we can currently predict, could have a material adverse effect on our business, results of operations, financial condition and cash flows or materially harm our reputation.
We may be subject to liability claims for damages and other expenses that are not covered by insurance or exceed our existing insurance coverage that could have a material adverse effect on our business, results of operations, financial condition and cash flows and could materially harm our reputation.
Our operations and how we manage our business may subject us, as well as our officers and directors to whom we owe certain defense and indemnity obligations, to litigation and liability. Our business, profitability and growth prospects could suffer if we face negative publicity or we pay damages or defense costs in connection with a claim that is outside the scope or limits of coverage of any applicable insurance coverage, including, without limitation, claims related to adverse patient events, cybersecurity incidents, contractual disputes, antitrust and competition laws and regulations, professional and general liability and directors' and officers' duties. In addition, we have received notices of claims from commercial payors and other third parties, as well as subpoenas and civil investigative demands from the federal government, related to our business practices, including, without limitation, our historical billing practices and the historical billing practices of acquired businesses. Although the ultimate outcome of these claims cannot be predicted, an adverse result with respect to one or more of these claims could have a material adverse effect on our business, results of operations, financial condition and cash flows, and could materially harm our reputation. We maintain insurance coverage for those risks we deem are appropriate to insure against and make determinations about whether to self-insure as to other risks or layers of coverage. However, a successful claim, including, without limitation, a professional liability, malpractice or negligence claim or a claim related to antitrust and competition laws or a cybersecurity incident, which is in excess of any applicable insurance coverage, that is outside the scope or limits of any applicable insurance coverage, or that is subject to our self-insurance retentions, could have a material adverse effect on our business, results of operations, financial condition, cash flows and reputation.
In addition, if our costs of insurance and claims increase, then our earnings could decline. Market rates for insurance premiums and deductibles have been steadily increasing. Our business, results of operations, financial condition and cash flows could be materially and adversely affected by any of the following:
•the collapse or insolvency of our insurance carriers;
•further increases in premiums and deductibles;
•increases in the number of liability claims against us or the cost of settling or trying cases related to those claims;
•obtaining insurance with exclusions for things such as communicable diseases; or
•an inability to obtain one or more types of insurance on acceptable terms, if at all.
If we fail to successfully maintain an effective internal control over financial reporting, the integrity of our financial reporting could be compromised, which could have a material adverse effect on our ability to accurately report our financial results, the market's perception of our business and our stock price.
The integration of acquisitions and addition of new business lines into our internal control over financial reporting has required and will continue to require significant time and resources from our management and other personnel and has increased, and is expected to continue to increase, our compliance costs. Failure to maintain an effective internal control environment could have a material adverse effect on our ability to accurately report our financial results, the market's perception of our business and our stock price. In addition, we could be required to restate our financial results in the event of a significant failure of our internal control over financial reporting or in the event of inappropriate application of accounting principles.
Provisions in our organizational documents, our compensation programs and policies and certain requirements under Delaware law may deter changes of control and may make it more difficult for our stockholders to change the composition of our Board of Directors and take other corporate actions that our stockholders would otherwise determine to be in their best interests.
Our organizational documents include provisions that may deter hostile takeovers, delay or prevent changes of control or changes in our management, or limit the ability of our stockholders to approve transactions that they may otherwise determine to be in their best interests. These include provisions prohibiting our stockholders from acting by written consent, advance notice requirements for director nominations and stockholder proposals and granting our Board of Directors the authority to issue preferred stock and to determine the rights and preferences of the preferred stock without the need for further stockholder approval.
Most of our outstanding employee stock-based compensation awards include a provision accelerating the vesting of the awards in the event of a change of control. These and any other change of control provisions may affect the price an acquirer would be willing to pay for our Company.
We are also subject to Section 203 of the Delaware General Corporation Law that, subject to exceptions, prohibits us from engaging in any business combinations with any interested stockholder, as defined in that section, for a period of three years following the date on which that stockholder became an interested stockholder.
The provisions described above may discourage, delay or prevent an acquisition of our Company at a price that our stockholders may find attractive. These provisions could also make it more difficult for our stockholders to elect directors and take other corporate actions and could limit the price that investors might be willing to pay for shares of our common stock.
Item 1B. Unresolved Staff Comments.Comments
None.
Item 1C. Cybersecurity
Risk Management and Strategy
Information security risks have significantly increased in recent years in part because of the proliferation of new technologies, the increasing use of the Internet and telecommunications technologies to conduct our operations, and the increased sophistication and activities of organized crime, hackers, terrorists and other external parties, including, among others, foreign state agents. Our business and operations rely on the secure and continuous processing, transmission and storage of confidential, proprietary and other information in our computer systems and networks, including sensitive personal information, such as PHI, social security numbers, and/or credit card information of our patients, teammates, physicians, business partners and others. Our business and operations also rely on certain critical IT vendors that support such processing, transmission and storage (which have become more relevant and important given the information security issues and risks that are intensified through our increased use of remote work arrangements).
To manage risks to our Company, including information and security risks, our Board oversees our enterprise-wide approach to risk management with a fundamental belief that the key components of risk management are:
•Identifying potential risks that we face;
•Assessing the likelihood and potential impact of the risks;
•Adopting strategies and controls designed to manage the risks;
•Reporting on a regular basis regarding the assessment and management of the risks; and
•Monitoring these potential risks on a regular basis.
Our Enterprise Risk Management (ERM) team leads this risk management process, and evaluates risks to the enterprise on short, intermediate and long-term bases. Our ERM team reports to our ERM Committee, a group comprised of members of senior management who meet on a regular basis to oversee the performance of these risk management functions. We assess risks using a probability-magnitude lens, with shorter and intermediate term risks generally given greater weight. We prioritize mitigating activities on shorter and intermediate term risks, but also use risk analyses and oversight to proactively incorporate mitigating activities into our long-term strategy. The ERM process reflects a Company-wide effort designed to identify, assess, manage, report and monitor enterprise risks and risk areas. This effort includes the Company's Enterprise Risk Services (Internal Audit), Sarbanes-Oxley (SOX), Compliance Audit, legal and IT Security teams, among others. The identification and evaluation of cybersecurity threats and risks is integrated into this ERM process.
The ERM process is incorporated into our disclosure controls and procedures. Representatives of each of our ERM, Legal, Internal Audit and Compliance Audit teams sit on the Company’s management Disclosure Committee, which is responsible for, among other things, the design and establishment of disclosure controls and procedures to help ensure the timeliness, accuracy and completeness of corporate disclosure. Our IT Security and Privacy teams, who are responsible for assessing cybersecurity threats and risks, in turn maintain policies and procedures designed to ensure appropriate escalation of cybersecurity incidents to meet external disclosure requirements. Our Chief Information Officer (CIO) and Chief Information Security Officer (CISO) regularly meet and coordinate with our Chief Privacy Officer (CPO). Each of the CIO, CISO and CPO also advise members of the Disclosure Committee, including our Chief Legal and Public Affairs Officer (CLO), on disclosure matters on an as-needed basis.
With respect to assessing privacy, data and cybersecurity risks, the Company adopts a hybrid approach that primarily aligns with the National Institute of Standards and Technology (NIST) Cybersecurity Framework, including the guidance set forth in the NIST HIPAA Security Rule Cybersecurity Guide, while also evaluating against certain elements of the ISO 27001 and 27005 standards that management believes provide additional levels of guidance or structure. We regularly evaluate the Company’s cybersecurity and privacy processes and procedures, both through regular audits by our Internal Audit and IT security teams, as well as regular retention of outside advisors under direction of our IT security team. Among other things, the IT security team oversees an external third party review at least every two years that evaluates the readiness of the entire Company against the NIST Cybersecurity Framework and provides an assessment that measures Capability Maturity Model Integration levels. Additionally, our CISO engages in regular consultations, typically monthly, with third-party cybersecurity advisors. Among other things, these sessions provide the Company with a broader review of the external cybersecurity environment, helping us to stay current on emerging or developing security approaches and risks. Among other initiatives, our CISO and the Company’s IT security team have actively participated in industry conferences and maintain memberships to resources such as the Health Information Sharing and Analysis Center (Health-ISAC), a trusted community of critical infrastructure owners and operators within the Health Care and Public Health sector which, among other things, allows the Company to monitor email updates and alerts coordinated with the U.S. Department of Homeland Security’s Cybersecurity and Infrastructure Security Agency. In order to maintain awareness of privacy, data and cybersecurity risks, the Company incorporates these topics into its annual compliance training materials that are mandatory for all teammates and new hires, and among other things cover HIPAA privacy and security requirements.
We maintain policies and have established processes involving our cybersecurity, privacy and legal teams that assess potential cybersecurity risks associated with our retention and use of third-party service providers. These policies and procedures are generally aligned with the NIST Cybersecurity Framework. Prior to retaining or renewing a third-party vendor, the Company policy requires a risk assessment of such potential new vendor or new engagement through a collaborative process among the Company’s IT security, privacy, insurance and legal teams, among others. Potential vendor engagements also are reviewed to assess a range of other considerations and contractual terms and conditions, including, among other things, a potential vendor’s liability insurance limits, scope and coverage of cyber insurance and privacy data protections. Our IT SOX team also conducts annual SOX reviews for those vendors that are considered in scope for SOX controls. All finalized vendor engagements are considered by Internal Audit as part of our ordinary course risk assessment and audit planning.
Cybersecurity Risks and the Impact on our Company
Due to the continuously evolving series of laws and regulations related to cybersecurity, data protection and privacy that are applicable to our business, as well as the associated risks from cybersecurity threats, we have expended significant resources in order to protect our information systems and data. We regularly review, monitor and implement multiple layers of security measures through technology, processes and our people. We utilize security technologies designed to protect and maintain the integrity of our information systems and data, and our defenses are monitored and routinely tested internally and by external parties. Despite these efforts, our facilities and systems and those of our third-party service providers may be vulnerable to privacy and security incidents; security attacks and breaches; acts of vandalism or theft; computer viruses and other malicious code; coordinated attacks by a variety of actors, including, among others, activist entities or state sponsored cyberattacks; emerging cybersecurity risks; cyber risk related to connected devices; misplaced or lost data; programming and/or human errors; or other similar events that could impact the security, reliability and availability of our systems. Internal or external parties have attempted to, and will continue to attempt to, circumvent our security systems, and we have in the past, and expect that we will in the future, defend against, experience, and respond to attacks on our network including, without limitation, reconnaissance probes, denial of service attempts, malicious software attacks including ransomware or other attacks intended to render our internal operating systems or data unavailable, and phishing attacks or business email compromise. While we have experienced cybersecurity incidents in the past, to date none have had a material impact on our business, results of operations, financial condition and cash flows.
Cybersecurity requires ongoing investment and diligence against evolving threats and in the context of new or developing technologies. For further information regarding the risks we face from cybersecurity threats and how our business strategy, results of operations, and financial condition could be materially affected by such risks, see Item I.A. Risk Factors under the heading, “Privacy and information security laws are complex…”.
Governance
Board Oversight
As part of their oversight responsibilities, the Audit Committee and the Compliance and Quality Committee monitor privacy, data and cyber security as specific risk areas. Both Mr. Schechter, a member of the Audit Committee and the Compliance and Quality Committee, and Ms. Schoppert, a member of the Audit Committee and the Compliance and Quality Committee, hold a CERT Certificate in Cybersecurity Oversight. The Audit Committee engages in regular discussions with management on privacy, data, and cybersecurity risk exposures, receiving quarterly reports from the ERM team and the CIO. The CPO and/or CLO periodically reports to the Audit Committee about the Company’s privacy program, and Internal Audit reports to the Audit Committee quarterly, providing the Audit Committee with results from any privacy, data, or cybersecurity audits.
Among other things, the Company’s privacy team actively develops and implements policies designed to comply with the requirements of privacy laws in the countries where the Company operates. Working with Internal Audit and the CIO, the privacy team assesses the nature and potential severity of privacy risks within DaVita and guides the organization in taking steps to help mitigate such risks. The CPO or CLO provides periodic updates to the Audit Committee on the status of the privacy program. The Audit Committee also oversees the Company's negotiation of any cybersecurity insurance. Currently, the Company maintains a cybersecurity risk insurance policy providing coverage for certain cybersecurity breaches among other specified risks.
Management
As referenced above, our IT Security team, in consultation with our Privacy Office, is primarily responsible for frontline assessments and management of day-to-day risks from cybersecurity threats, including the monitoring and detection of cybersecurity incidents and the execution of DaVita’s cybersecurity and privacy incident response plans, as needed. Pursuant to the plan, the teams are responsible for assessing and classifying cybersecurity incidents and coordinating the response to such incidents, including managing both internal and external reporting obligations and remediation efforts. Our key personnel responsible for privacy and cybersecurity expertise include our CIO, CISO and CPO. Their qualifications include expertise in international privacy laws, compliance, global IT strategy, and security responsibilities, helping to ensure a comprehensive approach to risk management. Our CISO holds a Certified Chief Information Security Officer certification from EC-Council and a Certified Information Security Manager certification from ISACA. Our CPO is a Certified Information Privacy Professional and a Certified Compliance and Ethics Professional, and has more than two decades of experience in creating and implementing privacy and data protection programs that enable multinational organizations to respect and protect personal data and execute mission critical business strategies.
Our IT Security team also operates a 24x7 security operations center through a managed service provider. This dedicated center, alongside active monitoring of the dark web for DaVita-related data, and our use of both internal and external tools, is designed to ensure proactive detection, prevention and remediation of cybersecurity incidents. We inform and develop this integrated approach through our ongoing internal and external evaluations and risk assessments of our IT security program as described above.
Item 2. Properties.Properties
Our corporate headquarters are located in Denver, Colorado, consisting of one owned 240,000 square foot building and one leased 345,900 square foot location. Our headquarters are occupied by teammates engaged in management, finance, marketing, strategy, legal, compliance and other administrative functions. We lease fivesix business offices located in California, Pennsylvania, Tennessee, and Washington as well as ownin the U.S. In addition, our international headquarters is located in the United Kingdom and consists of one leased business office in Washington for our U.S. dialysis business.office. Our laboratory is based in Florida where we operate our lab services out of one leased building. We also lease other administrative offices in the U.S. and worldwide.
ForThe vast majority of our U.S. dialysis business we own the land and buildings for six outpatient dialysis centers.centers are located on premises that we lease. We alsoregularly own 21an insignificant number of properties for development, including operating outpatient dialysis centers and properties we hold for sale. In addition, we lease a total of four owned properties to third-party tenants. Our remaining outpatient dialysis centers are located on premises that we lease.
The majority of our leases for our U.S. dialysis business cover periods from five years to 2015 years and typically contain renewal options of five years to ten years at the fair rental value at the time of renewal. Our leases are generally subject to periodicfixed escalation clauses, or contain consumer price index increases, or contain fixed escalation clauses.increases. Our outpatient dialysis centers range in size from approximately 1,000 to 33,000 square feet, with an average size of approximately 7,800 square feet. Our international leases generally range from one year to ten years.
Some of our outpatient dialysis centers are operating at or near capacity. However, we believe that we have adequate capacity within most of our existing dialysis centers to accommodate additional patient volume through increased hours and/or days of operation, or, if additional space is available within an existing facility, by adding dialysis stations. We can usually relocate existing centers to larger facilities or open new centers if existing centers reach capacity. With respect to relocating centers or building new centers, we believe that we can generally lease space at economically reasonable rates in the areas planned for each of these centers, although there can be no assurances in this regard. Expansion of existing centers or relocation of our dialysis centers is subject to review for compliance with conditions relating to participation in the Medicare ESRD program, among other things. In states that require a certificate of need or center license, additional approvals would generally be necessary for expansion or relocation.
Item 3. Legal Proceedings.Proceedings
The information required by this Part I Item 3 is incorporated herein by reference to the information set forth under the caption “"ContingenciesContingencies"” in Note 1615 to the consolidated financial statements included in this report.
Item 4. Mine Safety Disclosures.Disclosures
Not applicable.
PART II
Item 5. Market for the Registrant’s Common Equity, Related Stockholder Matters and Issuer Purchases of Equity Securities.Securities
Our common stock is traded on the New York Stock Exchange under the symbol DVA. The closing price of our common stock on January 29, 202131, 2024 was $117.37$108.16 per share. According to Computershare, our registrar and transfer agent, as of January 29, 2021,31, 2024, there were 7,5946,687 holders of record of our common stock. This figure does not include the indeterminate number of beneficial holders whose shares are held of record by brokerage firms and clearing agencies.
Our initial public offering was in 1994, and we have not declared or paid cash dividends to holders of our common stock since going public. We have no current plans to pay cash dividends and there are certain limitations on our ability to pay dividends under the terms of our senior secured credit facilities. See “"Liquidity and capital resourcesresources"” under Item 7. "Management’s Discussion and Analysis of Financial Condition and Results of OperationsOperations"” and the notes to the consolidated financial statements.
Stock Repurchases
The following table summarizes our repurchases of our common stock during the fourth quarter of 2020:2023:
| | | | | | | | | | | | | | | | | | | | | | | |
| Period | Total number
of shares
purchased | | Average price
paid per share | | Total number of shares purchased as part of publicly announced plans or programs | | Approximate dollar value
of shares that may yet be purchased under the plans or programs |
| (dollars and shares in thousands, except per share data) |
| October 1-31, 2020 | 1,828 | | | $ | 87.96 | | | 1,828 | | | $ | 515,926 | |
| November 1-30, 2020 | 1,149 | | | 105.54 | | | 1,149 | | | $ | 394,628 | |
| December 1-31, 2020 | 1,216 | | | 111.91 | | | 1,216 | | | $ | 1,929,955 | |
| Total | 4,193 | | | $ | 99.73 | | | 4,193 | | | |
The following table summarizes our repurchases of our common stock during 2020:
| | | | | | | | | | | | | | | | | | | | | | | |
| Period | Total number
of shares
purchased | | Average price
paid per share | | Total number of shares purchased as part of publicly announced plans or programs | | Approximate dollar value
of shares that may yet be purchased under the plans or programs |
| (dollars and shares in thousands, except per share data) |
| January 1 - March 31, 2020 | 4,052 | | | $ | 74.81 | | | 4,052 | | | $ | 1,400,356 | |
| April 1 - June 30, 2020 | — | | | — | | | — | | | $ | 1,400,356 | |
July 1 - September 30, 2020(1) | 8,232 | | | 88.13 | | | 8,232 | | | $ | 676,709 | |
| October 1 - December 31, 2020 | 4,193 | | | 99.73 | | | 4,193 | | | $ | 1,929,955 | |
| Total | 16,477 | | | $ | 87.80 | | | 16,477 | | | |
| | | | | | | | | | | | | | | | | | | | | | | |
| Period | Total number
of shares
purchased | | Average price paid per share (1) | | Total number of shares purchased as part of publicly announced plans or programs | | Approximate dollar value
of shares that may yet be purchased under the plans or programs |
| (dollars and shares in thousands, except per share data) |
| January 1 - March 31, 2023 | — | | | $ | — | | | — | | | $ | 1,596,085 | |
| April 1 - June 30, 2023 | — | | | — | | | — | | | $ | 1,596,085 | |
| July 1 - September 30, 2023 | — | | | — | | | — | | | $ | 1,596,085 | |
| October 1 - December 31, 2023 | 2,904 | | | 97.82 | | | 2,904 | | | $ | 1,311,942 | |
| Total | 2,904 | | | $ | 97.82 | | | 2,904 | | | |
(1)The total number of shares purchased Excludes commissions and the aggregate amount paid for shares repurchased include shares repurchased1% excise tax imposed by the Inflation Reduction Act of 2022.
As of December 31, 2023, we are authorized to make share repurchases pursuant to our modified Dutch auction tender offer at a clearing price of $88.00 per share plus related fees and expenses of $2.5 million.
Effective as of the close of business on November 4, 2019, theDecember 17, 2021 Board terminated all remaining prior shareauthorized repurchase authorizations available to us and approved a new share repurchase authorization of $2.0 billion.
Effective on December 10, 2020, the Board terminated all remaining prior share repurchase authorizations available to us under the aforementioned November 4, 2019 authorization and approved a new share repurchase authorizationplan of $2.0 billion. We are authorizedThis authorization allows us to make purchases from time to time in the open market or in privately negotiated transactions, including without limitation, through accelerated share repurchase transactions, derivative transactions, tender offers, Rule 10b5-1 plans or any combination of the foregoing, depending upon market conditions and other considerations.
As of February 10, 2021,12, 2024, we have a total of $1.807$1.149 billion, excluding excise taxes, available under the current repurchase authorization for additional share repurchases. Although this share repurchase authorization does not have an expiration date, we remain subject to share repurchase limitations, including under the terms of our senior secured credit facilities.
Item 6. Selected Financial Data.
The following financial and operating data should be read in conjunction with Item 7. "Management’s Discussion and Analysis of Financial Condition and Results of Operations” and our consolidated financial statements filed as part of this report. The following table presents selected consolidated financial and operating data for the periods indicated:
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 | | 2017 | | 2016 |
| | (dollars and shares in thousands, except per share data) |
| Income statement data: | | | | | | | | | |
Total revenues(1) | $ | 11,550,604 | | | $ | 11,388,479 | | | $ | 11,404,851 | | | $ | 10,876,634 | | | $ | 10,707,467 | |
Operating expenses and charges(2) | 9,855,968 | | | 9,745,162 | | | 9,879,027 | | | 9,063,879 | | | 8,677,757 | |
| Operating income | 1,694,636 | | | 1,643,317 | | | 1,525,824 | | | 1,812,755 | | | 2,029,710 | |
| Debt expense | (304,111) | | | (443,824) | | | (487,435) | | | (430,634) | | | (414,116) | |
| Debt prepayment, refinancing and redemption charges | (89,022) | | | (33,402) | | | — | | | — | | | — | |
| Other income, net | 16,759 | | | 29,348 | | | 10,089 | | | 17,665 | | | 7,511 | |
| Income from continuing operations before income taxes | 1,318,262 | | | 1,195,439 | | | 1,048,478 | | | 1,399,786 | | | 1,623,105 | |
Income tax expense(3) | 313,932 | | | 279,628 | | | 258,400 | | | 323,859 | | | 431,761 | |
| Net income from continuing operations | 1,004,330 | | | 915,811 | | | 790,078 | | | 1,075,927 | | | 1,191,344 | |
Net (loss) income from discontinued operations, net of tax(4) | (9,653) | | | 105,483 | | | (457,038) | | | (245,372) | | | (158,262) | |
| Net income | 994,677 | | | 1,021,294 | | | 333,040 | | | 830,555 | | | 1,033,082 | |
| Less: Net income attributable to noncontrolling interests | (221,035) | | | (210,313) | | | (173,646) | | | (166,937) | | | (153,208) | |
| Net income attributable to DaVita Inc. | $ | 773,642 | | | $ | 810,981 | | | $ | 159,394 | | | $ | 663,618 | | | $ | 879,874 | |
| | | | | | | | | |
| Earnings per share attributable to DaVita Inc.: | | | | | | | | | |
Basic income from continuing operations(5) | $ | 6.54 | | | $ | 4.61 | | | $ | 3.66 | | | $ | 4.78 | | | $ | 5.12 | |
Diluted income from continuing operations(5) | $ | 6.39 | | | $ | 4.60 | | | $ | 3.62 | | | $ | 4.71 | | | $ | 5.04 | |
| | | | | | | | | |
Weighted average shares for earnings per share(5): | | | | | | | | | |
| Basic shares | 119,797 | | | 153,181 | | | 170,786 | | | 188,626 | | | 201,641 | |
| Diluted shares | 122,623 | | | 153,812 | | | 172,365 | | | 191,349 | | | 204,905 | |
| | | | | | | | | |
| Balance sheet data (as of period end): | | | | | | | | | |
| Working capital | $ | 672,581 | | | $ | 1,318,072 | | | $ | 3,532,998 | | | $ | 5,703,181 | | | $ | 1,283,784 | |
| Total assets | $ | 16,988,516 | | | $ | 17,311,394 | | | $ | 19,110,252 | | | $ | 18,974,536 | | | $ | 18,755,776 | |
| Long-term debt | $ | 7,917,263 | | | $ | 7,977,526 | | | $ | 8,172,847 | | | $ | 9,158,018 | | | $ | 8,944,676 | |
Total DaVita Inc. shareholders' equity(5) | $ | 1,383,566 | | | $ | 2,133,409 | | | $ | 3,703,442 | | | $ | 4,690,029 | | | $ | 4,648,047 | |
(1)On January 1, 2018, we adopted Revenue from Contracts with Customers (Topic 606) using the cumulative effect method for those contracts that were not substantially completed as of January 1, 2018. See Notes 1 and 2 of the consolidated financial statements for further discussion of our adoption of Topic 606.
(2)The following table summarizes losses (gains) on changes in ownership interest, net, accruals for legal matters, impairment charges, restructuring charges and gain on settlement included in operating expenses and charges:
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 | | 2017 | | 2016 |
| | (dollars in thousands) |
| Certain operating expenses and charges: | | | | | | | | | |
| Loss (gain) on changes in ownership interests, net | $ | 16,252 | | | | | $ | (51,888) | | | $ | (6,273) | | | $ | (374,374) | |
| Accruals for legal matters | $ | 35,000 | | | | | | | | | $ | 15,770 | |
| Impairment charges | | | $ | 124,892 | | | $ | 27,969 | | | $ | 336,223 | | | $ | 43,408 | |
| Restructuring charges | | | | | $ | 11,366 | | | $ | 2,700 | | | |
| Gain on settlement | | | | | | | $ | (529,504) | | | |
(3)Tax expense for 2017 included a net tax benefit of $251,510 related to U.S. tax legislation passed in December 2017.
(4)On June 19, 2019, we completed the sale of our DMG business to Collaborative Care Holdings, LLC (Optum), a subsidiary of UnitedHealth Group Inc. Accordingly, DMG's results of operations are reported as net income (loss) from discontinued operations, net of
tax for all periods presented and its assets and liabilities were classified as held for sale for the periods reported prior to close of the transaction.
(5)The following table summarizes our common stock activity:
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 | | 2017 | | 2016 |
| | (dollars and shares in thousands) |
| Share repurchases: | | | | | | | | | |
| Shares | 16,477 | | | 41,020 | | | 16,844 | | | 12,967 | | | 16,649 | |
| Amounts paid | $ | 1,446,767 | | | $ | 2,402,475 | | | $ | 1,153,511 | | | $ | 810,949 | | | $ | 1,072,377 | |
| Shares issued: | | | | | | | | | |
| Stock purchase plan | 222 | | | 315 | | | 398 | | | 360 | | | 438 | |
| Stock award plans | 345 | | | 161 | | | 371 | | | 514 | | | 1,011 | |
Item 7. Management’s Discussion and Analysis of Financial Condition and Results of Operations.Operations
Forward-looking statements
This Annual Report on Form 10-K, including this Management’s Discussion and Analysis of Financial Condition and Results of Operations, contains statements that are forward-looking statements within the meaning of the federal securities laws and as such are intended to be covered by the safe harbor for "forward-looking statements" provided by the Private Securities Litigation Reform Act of 1995. These forward-looking statements could include, among other things, DaVita's response to and the expected future impacts of the novel coronavirus (COVID-19), including statements about our balance sheet and liquidity, our expenses, and expense offsets, revenues, billings and collections, potential need, ability or willingness to use any funds under government relief programs, availability or cost of supplies, treatment volumes, mix expectation, such as the percentage or number of patients under commercial insurance, the availabilitycurrent macroeconomic, marketplace and administration of COVID-19 vaccines,labor market conditions, and overall impact on our patients and teammates, as well as other statements regarding our future operations, financial condition and prospects, expenses, strategic initiatives, government and commercial payment rates, expectations related to value-based care, integrated kidney care and Medicare Advantage (MA) plan enrollment, expectations regarding increased competition and marketplace changes, including those related to new or potential entrants in the dialysis and pre-dialysis marketplace and the potential impact of innovative technologies, drugs or other treatments, expectations regarding the impact of our continuing cost savings initiatives and our ongoing stock repurchase program. All statements in this report, other than statements of historical fact, are forward-looking statements. Without limiting the foregoing, statements including the words "expect," "intend," "will," "could," "plan," "anticipate," "believe," "forecast," "guidance," "outlook," "goals," and similar expressions are intended to identify forward-looking statements. These forward-looking statements are based on DaVita's current expectations and are based solely on information available as of the date of this report. DaVita undertakes no obligation to publicly update or revise any forward-looking statements, whether as a result of changed circumstances, new information, future events or otherwise, except as may be required by law. Actual future events and results could differ materially from any forward-looking statements due to numerous factors that involve substantial known and unknown risks and uncertainties. These risks and uncertainties include, among other things:
•current macroeconomic and marketplace conditions, global events and domestic political or governmental volatility, many of which are interrelated and which relate to, among other things, inflation, potential interest rate volatility, labor market conditions, wage pressure, evolving monetary policies, and the continuing impact of the dynamic and evolving COVID-19 pandemic including, without limitation, on our patients, teammates, physician partners, suppliers, business, operations, reputation, financial condition and results of operations; the government’s response to the COVID-19 pandemic; the availability, acceptance, impact and efficacy of COVID-19 treatments, therapies and vaccines; further spread or resurgence of the virus, including as a result of the emergence of new strains of the virus; the continuing impact of the pandemic on our revenuerevenues and non-acquired growth due to lower treatment volumes; COVID-19's impact on the consequenceschronic kidney disease (CKD) population and our patient population including on the mortality of an extended economic downturn resulting from the impacts of COVID-19, such as athese patients; any potential negative impact on our commercial mix which may persist even afteror the pandemic subsides;number of our patients covered by commercial insurance plans; the potential impact of new or potential entrants in the dialysis and continuing COVID-19-relatedpre-dialysis marketplace and potential impact of innovative technologies, drugs, or other treatments on our patients and industry; our ability to successfully implement cost savings initiatives; supply chain challenges and disruptions; and elevated teammate turnover and training costs such as costs to procure equipment and clinical supplies and higher salary and wage expense. The aforementioned risksexpense, driven in part by persisting labor market conditions and uncertaintiesa high demand for our clinical personnel, any of which may also have the effect of heightening many of the other risks and uncertainties discussed below;below, and in many cases, the impact of the pandemic and the aforementioned global economic conditions on our business may persist even as the pandemic continues to subside;
•the concentration of profits generated by higher-paying commercial payor plans for which there is continued downward pressure on average realized payment rates, andrates; a reduction in the number or percentage of our patients under such plans, including, without limitation, as a result of restrictionscontinuing legislative efforts to restrict or prohibitions onprohibit the use and/or availability of charitable premium assistance, such as AB 290, which may result in the loss of revenues or patients, oras a result of our making incorrect assumptions about how our patients will respond to any change in financial assistance from charitable organizations;
•noncompliance by us or our business associates with any privacyas a result of payors’ implementing restrictive plan designs, including, without limitation, actions taken in response to the U.S. Supreme Court’s decision in Marietta Memorial Hospital Employee Health Benefit Plan, et al. v. DaVita Inc. et al. (Marietta); how and whether regulators and legislators will respond to the Marietta decision including, without limitation, whether they will issue regulatory guidance or security laws or any security breach by us or a third party involvingadopt new legislation; how courts will interpret other anti-discriminatory provisions that may apply to restrictive plan designs; whether there could be other potential negative impacts of the misappropriation, loss or other unauthorized use or disclosureMarietta decision; and the timing of confidential information;each of these items;
•the extent to which the ongoing implementation of healthcare reform, or changes in or new legislation, regulations or guidance, enforcement thereof or related litigation result in a reduction in coverage or reimbursement rates for our services, a reduction in the number of patients enrolled in or that select higher-paying commercial plans, or that are enrolled in or select Medicare Advantageincluding for example MA plans or other material impacts to our business;business or operations; or our making incorrect assumptions about how our patients will respond to any such developments;
•a reduction in government payment rates under the Medicare End Stage Renal Disease program or other government-based programs and the impact of the Medicare Advantage benchmark structure;
•risks arising from potential changes in laws, regulations or requirements applicable to us, such as potential and proposed federal and/or state legislation, regulation, ballot, executive action or other initiatives, including without limitation, those related to healthcare, antitrust matters, including, among others, restrictive covenants and acquisition, merger, joint venture or similar transactions and/or labor matters,matters;
•our ability to attract, retain and motivate teammates and our ability to manage operating cost increases or productivity decreases whether due to union organizing activities, which continue to increase in the dialysis industry, legislative or other changes, demand for labor, volatility and uncertainty in the labor market, the current challenging and highly competitive labor market conditions, or other reasons;
•our ability to respond to challenging U.S. and global economic and marketplace conditions, including among other things our ability to successfully identify cost savings opportunities and to invest in and implement cost savings initiatives such as AB 290ongoing initiatives that increase our use of third-party service providers to perform certain activities, initiatives that relate to clinic optimization and capacity utilization improvement, and procurement opportunities, among other things;
•our ability to successfully implement our strategies with respect to integrated kidney care and value-based care initiatives and home-based dialysis in California;the desired time frame and in a complex, dynamic and highly regulated environment, including, among other things, maintaining our existing business; meeting growth expectations; recovering our investments; entering into or renewing agreements with payors, third party vendors and others on terms that are competitive and, as appropriate, prove actuarially sound; structuring operations, agreements and arrangements to comply with evolving rules and regulations; finding, training and retaining appropriate staff; and further developing our integrated care and other capabilities to provide competitive programs at scale;
•a reduction in government payment rates under the Medicare ESRD program, state Medicaid or other government-based programs and the impact of the MA benchmark structure;
•noncompliance by us or our business associates with any privacy or security laws or any security breach by us or a third party involving the misappropriation, loss or other unauthorized use or disclosure of confidential information;
•legal and compliance risks, such as our continued compliance with complex, and at times, evolving government regulations and requirements and with additional laws that may apply to our operations as we expand geographically or enter into new lines of business, including through acquisitions or joint ventures;
•the impact of the political environment and related developments on the current healthcare marketplace and on our business, including with respect to the future of the Affordable Care Act, the exchanges and many other core aspects
of the current healthcare marketplace, as well as the composition of the U.S. Supreme Court and the newcurrent presidential administration and congressional majority;
•our ability to successfully implement our strategies with respect to home-based dialysis, value-based care and/or integrated kidney care, including maintaining our existing business and further developing our capabilities in a complex and highly regulated environment;
•changes in pharmaceutical practice patterns, reimbursement and payment policies and processes, or pharmaceutical pricing, including with respect to hypoxia inducible factors;
•legal and compliance risks, such as our continued compliance with complex government regulations;
•continued increased competition from dialysis providers and others, andoral phosphate binders, among other potential marketplace changes;things;
•our ability to develop and maintain contractsrelationships with physician medical directors,physicians and hospitals, changing affiliation models for physicians, and the emergence of new models of care or other initiatives introduced by the government or private sector that, among other things, may erode our patient base and impact reimbursement rates, such as accountable care organizations, independent practice associations and integrated delivery systems;rates;
•our ability to complete acquisitions, mergers, dispositions, joint ventures or dispositionsother strategic transactions that we might announce or be considering, on terms favorable to us or at all, or to successfully integrate andany acquired businesses, to successfully operate any business we may acquireacquired businesses, joint ventures or have acquired, orother strategic transactions, to successfully expand our operations and services in markets outside the United States, or to businesses or products outside of dialysis;dialysis services;
•continued increased competition from dialysis providers and others, and other potential marketplace changes, including without limitation increased investment in and availability of funding to new entrants in the dialysis and pre-dialysis marketplace;
•the variability of our cash flows, including without limitation any extended billing or collections cycles; the risk that we may not be able to generate or access sufficient cash in the future to service our indebtedness or to fund our other liquidity needs; and the risk that we may not be able to refinance our indebtedness as it becomes due, on terms favorable to us or at all;
•factors that may impact our ability to repurchase stock under our stock repurchase program and the timing of any such stock repurchases, as well as our use of a considerable amount of available funds to repurchase stock;
•risks arising from the use of accounting estimates, judgments and interpretations in our financial statements;
•impairment of our goodwill, investments or other assets;
•our aspirations, goals and disclosures related to environmental, social and governance (ESG) matters, including, among other things, evolving regulatory requirements affecting ESG standards, measurements and reporting requirements; the availability of suppliers that can meet our sustainability standards; and our ability to recruit, develop and retain diverse talent in our labor markets; and
•uncertainties associated with the other risk factors, trends and uncertainties set forth in Part I Item 1A. of this Annual Report on Form 10-K, and the other risks and uncertainties discussed in any subsequent reports that we file or furnish with the SEC from time to time.
The following should be read in conjunction with our consolidated financial statements.
Company overview
Our principal business is to provide dialysis and related lab services to patients in the United States, which we refer to as our U.S. dialysis business. We also operate variousour U.S. integrated kidney care (IKC) business, our U.S. other ancillary services, and strategic initiatives including our international operations, which we collectively refer to as our ancillary services, as well as our corporate administrative support. Our U.S. dialysis business is a leading provider of kidney dialysis services in the U.S. for patients suffering from chronic kidney failure, also known as end stage renal disease (ESRD) or end stage kidney disease (ESKD).
On June 19, 2019, we completed the sale of our DaVita Medical Group (DMG) business to Collaborative Care Holdings, LLC, a subsidiary of UnitedHealth Group Inc. As a result of this transaction, DMG's results of operations have been reported as discontinued operations for all periods presented and DMG is not included below in this Management's Discussion and Analysis.
Notwithstanding the challenges of responding to the novel coronavirus pandemic (COVID-19), ourOur year-over-year overall financial performance in 20202023 benefited from increased revenue, which was primarily due to higher average revenue per treatmentrevenues in our U.S. dialysis, businessinternational and IKC businesses, as well as acquireddecreases in pharmaceutical costs, contract wage expense and advocacy spend. These positive trends were partially offset by continued increases in compensation expense, severance costs and center closure costs as we continued to focus on cost savings initiatives. In addition, 2023 was negatively impacted by increased legal costs and our continued investment in our integrated care support functions needed to support patient growth in our internationalIKC business. This was partially offset by increases in labor costs (both operating
Operational and overhead), lower margin on calcimimetics, increases in advocacy costs, and increased costs driven by the emergence of COVID-19, including increased costs related to compensation and medical supplies.
Drivers of our financial performance in 2020 included the following:highlights for 2023 include, among other things:
•improved key clinical outcomes in our U.S. dialysis business, including our recognition asrevenue growth of 3.2% from an industry leader for the eighth consecutive yearincrease in CMS’ Quality Incentive Program and for the last seven years under the CMS Five-Star Quality Rating system;average patient services revenue per treatment of $12.20;
•revenue growth of 0.9%35.2% in U.S. dialysis, 5.3%our IKC business which included the recognition of an incremental $55 million in U.S. ancillary services,shared savings revenue from the IKC adjustment described below, and 11.0%9.0% in our international operations;
•a net increaseoperating income of 63 U.S.$1,603 million and 62 international dialysis centers, including entering a new country, the United Kingdom;adjusted operating income of $1,734 million;
•operating cash flows of $1.979 billion from continuing operations;$2,059 million and free cash flows of $1,236 million;
•repurchase of 16,477,3782,903,832 shares of our common stock for aggregate consideration of $1.447 billion,$286 million, and a 1.8% reduction ofin our share count by 12.6% year-over-year;
•refinancing transactions, including the redemption of our 5.125% and 5.0% senior notes, the issuance of ourentry into a new 4.625% and 3.75% senior notes and the repricing of our Term Loan B-1 resultingA-1 facility in lower debt expense;the aggregate principal amount of $1,250 million and a revolving line of credit in an aggregate principal amount up to $1,500 million and purchase of $4,500 million notional amount of forward caps to shield our exposure to significant interest rate increases through 2026; and
•impactleverage ratio, as a multiple of COVID-19Consolidated EBITDA, each as further discusseddefined by our credit agreement, is back within our target range of 3.0x to 3.5x.
Additional highlights include:
•a net decrease of 49 U.S. dialysis centers to improve center capacity utilization, as well as a net increase of 17 international dialysis centers from acquisitions and developments;
•a net increase in Part I. Item 1 U.S. dialysis patients of 0.7% and international patients of 8.4% as of December 31, 2023;
•“Business”continued patient growth in IKC to 58,000 patients in risk-based integrated care arrangements and under the heading "COVID-19an additional 17,000 patients in other integrated care arrangements; and its impact on our business" below.
•invested in Mozarc Medical Holding LLC (Mozarc), an independent new company committed to reshaping kidney health and driving patient-centered technology solutions.
In 2021,2024, we expect that COVID-19treatment volumes will continuereturn to impact our business and financial performance,positive growth as described in further detail below, though the magnitude of these impacts remains difficult to predict and subject to significant uncertainty due to a number of factors, including, among others, the severity and duration of the pandemic; further spread or resurgence of the virus, including as a result of the emergence of new strains of the virus; its impact on the CKD patient population and our patient population; the availability, acceptance, impact and efficacy of COVID-19 treatments, therapies and vaccines; the pandemics' continuing impact on the U.S. and global economies and unemployment; the responses of our competitors to the pandemic and related changes in the marketplace; and the timing, scope and effectiveness of federal, state and local government responses. The continued impacts and disruptions to our business as a result of the COVID-19 pandemic could have a material adverse impact on our patients, teammates, physician partners, suppliers, business, operations, reputation, financial condition, results of operations, cash flows and/or liquidity. On treatment volume, we continue to face pressure primarily driven by thecompounding impact of COVID-19 on historical mortality rates forof dialysis patients. This pressure is also influenced by slowing industry growthpatients and competitive activity. On reimbursement rate, weour patient census subsides. We expect modest growth in aggregate, primarilyimproving adjusted operating income due to the expectedcombination of the net market basket update for Medicare treatments as well as an increaseimpact of our continued improvements in Medicare Advantage enrollment due to the 21st Century Cures Act, partially offset by the scheduled resumption of Medicare sequestration in 2021. Onour billing cycle process and ongoing cost wesavings initiatives. We continue to expect inflationary pressure on wage rates and other costs partially offset by continued savings on pharmaceutical costs. We expectdue to incur significantly less advocacy costs in 2021 than we experienced in 2020.the challenging labor market and other inflationary conditions. We also expect to continue making investments to expandsee continued investment and operating improvement in our ability to offer home-based dialysis service options and further advance our integrated kidney care and value-based care initiatives in 2021. during 2024.Finally, the timing and scope of any potential changes to the regulatory landscape remain uncertain, particularly in light of the ongoing COVID-19 pandemic and the incoming new federal administration, and as such, considerable uncertainty exists surrounding the continued development of the various governmental laws, regulations and other requirements that may impact our business.
The discussion below includes analysis of our financial condition and results of operations for the years ended December 31, 20202023 compared to December 31, 2019.2022. Our Annual Report on Form 10-K for the year ended December 31, 2019,2022, includes a discussion and analysis of our financial condition and results of operations for the year ended December 31, 2018,2021, in its Part II Item 7, "Management's Discussion and Analysis of Financial Condition and Results of Operations".
References to the "Notes" in the discussion below refer to the notes to the Company's consolidated financial statements included in this Annual Report on Form 10-K at Part IV Item 15, "Exhibits, Financial Statement Schedules" as referred from Part II Item 8, "Financial Statements and Supplementary Data."
COVID-19General Economic and its impact on our businessMarketplace Conditions; Legal and Regulatory Developments
As noted above and described in further detail below, developments in Part I Item 1, "Business," we continue to closely monitorgeneral economic and market conditions have directly and indirectly impacted the impact on our business ofCompany and in the pandemic and the resulting economic environment, including thefuture could have a material adverse impact on our patients, teammates, physician partners, suppliers, vendorsbusiness, operations, reputation, financial condition, results of operations, share price, cash flows and/or liquidity. Many of these external factors and business partners. We have dedicated and continue to dedicate substantial resources in response to COVID-19, to help safely maintain continuity of care for our patients throughout this crisis, whether in the hospital, outpatient or home setting, and to help protect our caregivers. Our COVID-19 response has included,conditions are interrelated, including, among other things, inflation, potential interest rate volatility, labor market conditions, wage pressure, the implementationimpact of additional protocols and operational initiatives related to infection control and clinical best practices, redistributionCOVID-19 on the mortality rates of resources across geographies and increased investment in and utilization of telehealth capabilities. We also have maintained business process continuity during the pandemic by enabling most back office teammates to work remotely and implemented guidance early in the pandemic to help mitigate health and safety risks to our teammates imposed by COVID-19. Our response protocol generally has allowed us to maintain continuity of care for our patients and we carefully monitorother ESKD or CKD patients, supply chain challenges and the efficacypotential impact and application of innovative technologies, drugs or other treatments. Certain of these protocols and their impact on our operations and strategic initiativesimpacts could be further intensified by concurrent global events such as the pandemic continues.ongoing conflicts between Russia and Ukraine and in Israel, Gaza and the surrounding areas, which have continued to drive sociopolitical and economic uncertainty across the globe.
Due in partOperational and Financial Impacts
In the fourth quarter of 2023, treatment per day volumes were relatively flat compared to the protocols and initiatives described above,third quarter. On a full year basis, we incurred significant costs related to COVID-19 in 2020, and we expect to continue to incur extended and significant additional costs in connection with our response to COVID-19. For example, we have had, and expect to continue to have, increased costs associated with a high demand for our skilled clinical personnel. Additionally, the steps we have taken designed to help safely maintain continuity of care for our patients and help protect our caregivers, such as our policies to implement dedicated care shifts for patients with confirmed or suspected COVID-19 and other enhanced clinical practices, have increased, and are expected to continue to increase, our expenses and use of personal protective equipment (PPE). Our response to COVID-19 also has resulted in higher salary and wage expense, and we have provided, and may provide in the future, substantial financial support associated with relief reimbursement to our teammates. Furthermore, the effort and cost needed to procure certain of our equipment and clinical supplies, including PPE, have increased, and we expect that these increased costs will continue while the pandemic persists. However, our COVID-19 response reduced certain other expenses in 2020, such as those related to teammate travel, though it remains uncertain how much of these reductions, if any, will persist after the pandemic subsides.
We have experienced and expect to continue to experience a negative impact on revenue and non-acquired growth from COVID-19treatment volume due to lower treatment volumes, including from the cumulative and compounding negative impact of COVID-19 on the mortality rates of our patients and the associated adverse impact on our patient census. However, we have continued to experience improvements with respect to these negative impacts with treatment volumes remaining relatively flat year over year and looking at the full year, we have seen an increase in patient census that iscompared for the result of changes infirst time since 2019. Despite these improvements, new admission rates, of mortality. Because ESRD patients may be oldertreatment volumes, future revenues and generally have comorbidities, several of which are risk factors for COVID-19, we believe the mortality rate of infected patients is, and willnon-acquired growth, among other things, could continue to be higher in the dialysis population than in the general population, and COVID-19 also could impact the CKD population differently. Over the longer term, we believe that changes in mortality in both the CKD and ESRD populations duenegatively impacted over time to COVID-19 will depend primarily on the infection rate, case fatality rate, the age and health status of affected patients, the access to and efficacy of vaccinations as well as willingness to be vaccinated. We expect that these changes are likely to continue to negatively impact our revenue and non-acquired growth even as the pandemic subsides. However, determining the extent to which these impacts should be directly attributable to COVID-19 is difficult due to testingthat the ESKD and reporting limitations, and other factors that may drive treatment volumes and new admissions over time, such as the number of transplants or deferred admissions.CKD populations experience sustained elevated mortality levels. The magnitude of these cumulative impacts has been substantial,could have a material adverse impact on our results of operations, financial condition and depending oncash flows.
Ongoing global economic conditions and political and regulatory developments, such as general labor, supply chain and inflationary pressures have also increased, and will continue to increase, our expenses, including, among others, staffing and labor costs. We continue to experience increased levels of compensation compared to the ultimate severityprior year with contract labor improvements offset by investments in our teammate compensation. We expect certain of these increased staffing and durationlabor costs to continue, due to, among other factors, the continuation of the pandemic,a challenging healthcare labor market. The cumulative impact of these increased costs could be material.
In addition, our industry has experienced increased union organizing activities, including the COVID-19 pandemic and efforts to contain the virus have led to global economic deterioration and rapid and sharp increases in unemployment levels, which ultimately could result in a materially reduced sharefiling of petitions by unions at certain of our patients being covered by commercial insurance plans,competitors' clinics with more patients being covered by lower-paying government insurance programsa number of those clinics voting to unionize. Potential staffing shortages or being uninsured.other potential developments or disruptions related to our teammates, if material, could ultimately lead to the unplanned closures of certain centers or adversely impact clinical operations, or may otherwise have a material adverse impact on our ability to provide dialysis services or the cost of providing those services, among other things.
The cost inflation trends described above have put pressure on our existing cost structure, and as noted above, we expect that certain of those increased costs will persist as inflationary and supply chain pressures and challenging labor market conditions continue. During the fourth quarter of 2023, we continued to invest in and implement cost savings initiatives designed to help mitigate these cost and volume pressures. These effects may persist afterinclude identified cost savings related to the pandemic subsidesachievement of general and administrative cost efficiencies through ongoing initiatives that increase our use of third party service providers to perform certain activities. These opportunities and investments also include, among others, initiatives relating to clinic optimization, capacity utilization improvement and procurement opportunities, as well as investments in revenue cycle management. We have incurred, and expect to continue to incur, charges in connection with the continued implementation of certain of these initiatives. There can be no assurance that we will be able to successfully execute these initiatives or that they will achieve expectations or succeed in helping offset the impact of these challenging conditions.
Legal and Regulatory Developments
On October 13, 2019, California Assembly Bill 290 (AB 290) was signed into law. As drafted, AB 290 would, among other things, ourlimit the amount of reimbursement paid to certain providers for services provided to patients could experience permanent changeswith commercial insurance who receive charitable premium assistance (reimbursement cap). The implementation of AB 290 has been stayed pending resolution of legal challenges. The trial court recently issued a decision relating to these challenges to AB 290 that may result in the stay being lifted and at least some provisions of the law being implemented in the near future, although any appeal of the decision may result in the stay being continued. While it is currently unclear when and how those provisions may be implemented, in the event certain provisions of AB 290 are implemented in their insurance coverage as a resultproposed form, including the reimbursement cap, it may have negative consequences for our business. Depending on what provisions are implemented, organizations that provide charitable premium assistance may choose to withdraw from California, which would have an adverse impact on the
ability of changespatients to their employment status.afford Medicare premiums and Medicare supplemental and commercial coverage. We expect that such an adverse impact will in turn adversely impact our business, results of operations, financial condition and cash flows. In the event such a material reduction occurspast, bills similar to AB 290 have been introduced in other states, but none has become law. If these or similar bills are introduced and implemented in other jurisdictions, and organizations that provide charitable premium assistance in those jurisdictions are similarly impacted, it could in the share of our patients covered by commercial insurance plans, it wouldaggregate have a material adverse impact on our business, results of operations, financial condition and cash flows. The extentFor additional information on risks associated with charitable premium assistance for ESRD patients and the potential impact of these effects will be dependent upon, among other things, the extent and duration of the increased unemployment levels for our patient population, economic deterioration and potential recession; the timing and scope of federal, state and local governmental responsesdecreases to the ongoing pandemic; and patients’ ability to retain existing insurance and their individual choices with respect to their coverage. Despite
the broader economic conditions in the U.S. in 2020, our commercial mix in 2020 was relatively flat as compared to our commercial mix in 2019, which we believe was largely due to the fact that older, higher-risk patients who tend to disproportionately have government health insurance coverage, have been more adversely impacted by COVID-19 to date, but the ultimate impactpercentage or number of COVID-19 on our commercial mix will depend on future developments that are highly uncertain and difficult to predict.
The government response to COVID-19 has been wide-ranging and will continue to develop over time, particularly in light of the new federal administration.As a result, we may not be able to accurately predict the nature, timing or extent of the impact of such changes on the markets in which we conduct business or on the other participants that operate in those markets, or any potential changes to the extensive set of federal, state and local laws, regulations and requirements that govern our business. We have worked with certain government agencies to respond to the COVID-19 pandemic, and in certain cases have sought waivers of regulatory requirements. We also are working to help make COVID-19 vaccines available to our patients and teammates, including through coordination with state and federal governments on direct vaccine distribution so that we can administer vaccines to our patients and teammates. These vaccines are currently available under emergency use authorizations, and there can be no assurance that our patients and caregivers will choose to receive a COVID-19 vaccine or that the vaccines will prove to be as safe and effective as currently understood by the scientific community. In addition, we may encounter difficulties with the availability and storage of the vaccines, or experience other complications related to administering the vaccines, some of which have multiple dose requirements. We operate in a complex and highly regulated environment, and the novel nature of our COVID-19 response, including, for example, with respect to regulatory waivers and our administration of the newly developed COVID-19 vaccines, may increase our exposure to legal, regulatory and clinical risks.
Furthermore, a significant initial part of the federal government response to the COVID-19 pandemic was the Coronavirus Aid, Relief, and Economic Security (CARES) Act, a $2 trillion economic stimulus package that was signed into law on March 27, 2020. The CARES Act included a provision that suspended the 2% Medicare sequestration from May 1, 2020 through December 31, 2020, and in the year ended December 31, 2020 our revenues increased due to this suspension as further described below. The Consolidated Appropriations Act 2021, signed into law on December 27, 2020, extended the suspension of the 2% Medicare sequestration until March 31, 2021. While in effect, this legislation has increased, and will continue to increase our revenues. In addition, the CARES Act authorized $100 billion in funding to be distributed to healthcare providers through the federal Public Health and Social Services Emergency Fund (Provider Relief Fund). While we declined approximately $250 million of government funding received in the second quarter of 2020 from the Provider Relief Fund, certain of our competitors accepted such funds. There can be no assurance that financial or other assistance will be available from the government if we have a need for such assistance in the future.
We believe the ultimate impact of this public health crisis on the Company will depend on future developments that are highly uncertain and difficult to predict, including among other things the severity and duration of the pandemic; further spread or resurgence of the virus including as a result of the emergence of new strains of the virus; its impact on the CKD patient population and our patient population; the availability, acceptance, impact and efficacy of COVID-19 treatments, therapies and vaccines; the pandemic’s continuing impact on the U.S. and global economies and unemployment; the responses of our competitors to the pandemic and related changes in the marketplace; and the timing, scope and effectiveness of federal, state and local governmental responses. At this time, we cannot reasonably estimate the ultimate impact the COVID-19 pandemic will have on us, but the adverse impact could be material.
For additional discussion of the COVID-19 pandemic and our response, including its impact on us and related risks and uncertainties, pleasecommercial insurance, see the discussion in Part I Item 1 "Business" under the headings, "COVID-19 and its impact on our business" and "Human Capital Management", as well as the risk factor in Part I Item 1A. Risk Factorsfactors under the heading "“We face various risks related toChanges in federal and state healthcare legislation or regulations..." and "If the dynamic and evolving novel coronavirus pandemic, anynumber or percentage of which may have a material adverse impact on us.patients with higher-paying commercial insurance declines...”"
Consolidated results of operations
The following table summarizes our revenues, operating income (loss) and adjusted operating income (loss) by line of business. See the discussion of our results for each line of business following this table:table. When multiple drivers are identified in the following discussion of results, they are listed in order of magnitude:
| | | | Year ended December 31, | | Annual change | | Year ended December 31, | | Annual change |
| | | 2020 | | 2019 | | Amount | | Percent | | 2023 | | 2022 | | Amount | | Percent |
| | | (dollars in millions) | | (dollars in millions) |
| Revenues: | Revenues: | | | | | | Revenues: | | | | | | | |
| U.S. dialysis | U.S. dialysis | $ | 10,660 | | | $ | 10,563 | | | $ | 97 | | | 0.9 | % | U.S. dialysis | $ | 10,937 | | | $ | | $ | 10,600 | | | $ | | $ | 337 | | | 3.2 | | 3.2 | % |
| Other - ancillary services | 1,053 | | | 972 | | | 81 | | | 8.3 | % |
| Other - Ancillary services | | Other - Ancillary services | 1,299 | | | 1,101 | | | 198 | | | 18.0 | % |
| Elimination of intersegment revenues | Elimination of intersegment revenues | (162) | | | (146) | | | (16) | | | (11.0) | % | Elimination of intersegment revenues | (96) | | | (91) | | (91) | | | (5) | | (5) | | | (5.5) | | (5.5) | % |
| Total consolidated revenues | Total consolidated revenues | $ | 11,551 | | | $ | 11,388 | | | $ | 162 | | | 1.4 | % | Total consolidated revenues | $ | 12,140 | | | $ | | $ | 11,610 | | | $ | | $ | 530 | | | 4.6 | | 4.6 | % |
| | Operating income (loss): | Operating income (loss): | |
| Operating income (loss): | |
| Operating income (loss): | |
| U.S. dialysis | |
| U.S. dialysis | |
| U.S. dialysis | U.S. dialysis | $ | 1,918 | | | $ | 1,925 | | | $ | (7) | | | (0.4) | % | $ | 1,775 | | | $ | | $ | 1,565 | | | $ | | $ | 210 | | | 13.4 | | 13.4 | % |
| Other - Ancillary services | Other - Ancillary services | (76) | | | (189) | | | 113 | | | 59.8 | % | Other - Ancillary services | (9) | | | (97) | | (97) | | | 88 | | 88 | | | 90.7 | | 90.7 | % |
| Corporate administrative support | Corporate administrative support | (147) | | | (92) | | | (54) | | | (58.7) | % | Corporate administrative support | (163) | | | (130) | | (130) | | | (33) | | (33) | | | (25.4) | | (25.4) | % |
| Operating income | Operating income | $ | 1,695 | | | $ | 1,643 | | | $ | 51 | | | 3.1 | % | Operating income | $ | 1,603 | | | $ | | $ | 1,339 | | | $ | | $ | 264 | | | 19.7 | | 19.7 | % |
| Adjusted operating income (loss):(1) | Adjusted operating income (loss):(1) | |
Adjusted operating income (loss):(1) | |
Adjusted operating income (loss):(1) | |
| U.S. dialysis | |
| U.S. dialysis | |
| U.S. dialysis | U.S. dialysis | $ | 1,918 | | | $ | 1,925 | | | $ | (7) | | | (0.4) | % | $ | 1,900 | | | $ | | $ | 1,668 | | | $ | | $ | 232 | | | 13.9 | | 13.9 | % |
| Other - Ancillary services | Other - Ancillary services | (60) | | | (64) | | | 4 | | | 6.3 | % | Other - Ancillary services | (45) | | | (89) | | (89) | | | 44 | | 44 | | | 49.4 | | 49.4 | % |
| Corporate administrative support | Corporate administrative support | (112) | | | (92) | | | (19) | | | (20.7) | % | Corporate administrative support | (122) | | | (129) | | (129) | | | 7 | | 7 | | | 5.4 | | 5.4 | % |
| Adjusted operating income | Adjusted operating income | $ | 1,746 | | | $ | 1,768 | | | $ | (22) | | | (1.2) | % | Adjusted operating income | $ | 1,734 | | | $ | | $ | 1,450 | | | $ | | $ | 284 | | | 19.6 | | 19.6 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
(1)For a reconciliation of adjusted operating income (loss) by reportable segment, see the "Reconciliations of non-GAAP measures" section below.
U.S. dialysis business
OurAs of December 31, 2023, our U.S. dialysis business is a leading provider of kidney dialysis services, operating 2,8162,675 outpatient dialysis centers and serving a total of approximately 204,200 patients. We also200,800 patients, and contracted to provide hospital inpatient dialysis services in approximately 900790 hospitals. We estimate that we have approximately a 36% share of the U.S. dialysis market based upon the number of patients we serve.
Approximately 91%89% of our 20202023 consolidated revenues were derived directly from our U.S. dialysis business. The principal drivers of our U.S. dialysis revenues include :
•our number of treatments, which is primarily a function of the number of chronic patients requiring approximately three in-center treatments per week as well as, to a lesser extent, the number of treatments for home-based dialysis and hospital inpatient dialysis; and
•our average dialysis patient service revenue per treatment, including the mix of patients with commercial plans and government programs as primary payor.
Within our U.S. dialysis business, our home-based dialysis and hospital inpatient dialysis services are operationally integrated with our outpatient dialysis centers and related laboratory services. Our outpatient, home-based and hospital inpatient dialysis services comprise approximately 77%76%, 17%18% and 6% of our U.S. dialysis revenues, respectively.
In the U.S., government dialysis-related payment rates are principally determined by federal Medicare and state Medicaid policy. For 2020,2023, approximately 68%67% of our total U.S. dialysis patient servicesservice revenues were generated from government-based programs for services to approximately 90%89% of our total U.S. patients. These government-based programs are principally Medicare and Medicare Advantage,MA, Medicaid and managed Medicaid plans, and other government plans, representing approximately 57%56%, 7%8% and 4%3% of our U.S. dialysis patient servicesservice revenues, respectively.
On October 27, 2023, the Centers for Medicare & Medicaid Services (CMS) issued a final rule to update the Medicare ESRD Prospective Payment System payment rate and policies for calendar year 2024. CMS estimates the final rule will affect ESRD facilities' average reimbursement by a productivity-adjusted market basket increase of 2.1% in 2024.Dialysis payment rates from commercial payors vary and a major portion of our commercial rates are set at contracted amounts with payors and are subject to intense negotiation pressure. On average, dialysis-related payment rates from contracted commercial payors are significantly higher than Medicare, Medicaid and other government program payment rates, and therefore the percentage of commercial patients in relation to total patients represents a significant driver of our total average dialysis patient service revenue per treatment. Commercial payors (including hospital dialysis services) represent approximately 32%33% of U.S. dialysis patient servicesservice revenues.
For a discussion of government reimbursement, the Medicare ESRD bundled payment system, Medicare AdvantageMA and commercial reimbursement, see the discussion in Part I.I Item 1. Business under the heading “"U.S. dialysis business – Sources of revenue-concentrations and risks."” For a discussion of operational, clinical and financial risks and uncertainties that we face in connection with the Medicare ESRD bundled payment system, see the risk factor in Part I.I Item 1A. Risk Factors under the heading “"Our business is subject to a complex set of governmental laws, regulations and other requirements and any failure to adhere to those requirements, or any changes in those requirements, could have a material adverse effect on our business, results of operations, financial condition and cash flows, could materially harm our stock price, and in some circumstances, could materially harm our reputationrequirements..." ” For a discussion of operational, clinical and financial risks and uncertainties that we face in connection with commercial payors, see the risk factorsfactor in Item 1A. Risk Factors under the headingsheading "We continuously have ongoing negotiationsIf the number or percentage of patients with higher-paying commercial payors, andinsurance declines, if the average rates that commercial payors pay us decline significantly, if patients in commercial plans are subject to restriction in plan designs or if we are unable to maintain contracts with payors with competitive terms, including, without limitation, reimbursement rates, scope and duration of coverage and in-network benefits, it would have a material adverse effect on our business, results of operations, financial condition and cash flowsdeclines..."; and "If the number of patients with higher-paying commercial insurance declines, it could have a material adverse effect on our business, results of operations, financial condition and cash flows."
Effective January 1, 2018, both oral and intravenous forms of calcimimetics became the financial responsibility of our U.S. dialysis business for our Medicare patients and are reimbursed under Medicare Part B. Since the effective date through December 31, 2020, the oral and intravenous forms of calcimimetics were separately reimbursed through a transitional drug add-on payment adjustment (TDAPA) and not as part of the ESRD PPS bundled payment. These separate reimbursement payments for calcimimetics were subject to change on an annual basis. During the initial TDAPA period, Medicare payments were based on a pass-through rate of the average sales price plus approximately 6% before sequestration (or 4% adjusted for sequestration), and in 2020 they were based on a pass-through rate of the average sales price plus 0%, before sequestration. As expected, as of January 1, 2021, calcimimetics was added to the ESRD PPS bundled payment. We therefore expect our operating income from calcimimetics to be more stable in the future as compared to the past three years under the TDAPA model.
Approximately 4% and 6% of our total U.S. dialysis patient services revenues for the years 2020 and 2019, respectively, are associated with the administration of separately-billable physician-prescribed pharmaceuticals, of which approximately 3% and 4% relate to the administration of calcimimetics, respectively.
We anticipate that we will continue to experience increases in our operating costs in 20212024 that may outpace any net Medicare, commercial or other rate increases that we may receive, which could significantly impact our operating results. In particular, we expect to continue experiencing increases in operating costs that are subject to inflation, such as labor and supply costs, including increases in maintenance costs, regardless of whether there is a compensating inflation-based increase in Medicare, commercial or other payor payment rates or in payments under the ESRD bundled payment rate system. We also continue to expect to incur additional COVID-19-related costs while the pandemic continues.rates. In addition, we expect to continue to incur capital expenditures and associated depreciation and amortization costs to improve, renovate and maintain our facilities, equipment and information technology to meet evolving regulatory requirements and otherwise.
U.S. dialysis patient care costs are those costs directly associated with operating and supporting our dialysis centers, home-based dialysis programs and hospital inpatient dialysis programs, and consist principally of labor, benefits, pharmaceuticals, medical supplies and other operating costs of the dialysis centers.
The principal drivers of our U.S. dialysis patient care costs include:
•clinical hours per treatment, labor rates and benefit costs;
•vendor pricing and utilization levels of pharmaceuticals;
•business infrastructure costs, which include the operating costs of our dialysis centers; and
•certain professional fees.medical supply costs.
Other cost categories that can present significant variability include employee benefit costs, insurance costs and medical supply costs.professional fees. In addition, proposed ballot initiatives or referendums, legislation, regulations or policy changes could cause us to incur substantial costs to prepare for, or implement changes required. Any such changes could result in, among other things, increases in our labor costs or limitations on the amount of revenue that we can retain. For additional information on risks associated with potential and proposed ballot initiatives, referendums, legislation, regulations or policy changes, see the risk factor in Item 1A. Risk Factors under the heading, "Changes in federal and state healthcare legislation or regulations could have a material adverse effect on our business, results of operations, financial condition and cash flows.regulations..."
Our average clinical hours per treatment decreasedwas relatively flat in 20202023 compared to 2019.2022. We are always striving for improved productivity levels, however, changes in thingsfactors such as federal and state policies or regulatory billing requirements
can lead to increased labor costs.costs as can increases in turnover. In 2020,2023, the demand for skilled clinical personnel increasedcontinued, exacerbated by the nationwide shortage of these resources. In 2023 and 2022, we experienced increases in our clinical labor wage rates, which includes contract labor, of approximately 1.3% and 7.4%, respectively. We expect to continue to see higher clinical labor rates in 2024 due to labor market conditions, including changes in local minimum wage laws, and the demand of the pandemic on these resources, intensifying these competitive pressures; however, we managed to increasecontinued competition for skilled clinical personnel. In 2023, our overall clinical teammate retention in 2020. In 2020 and 2019, we experienced an increase in our clinical labor rates of approximately 3.0% and 2.0%, respectively, consistent with general industry trends.turnover was relatively flat from 2022, but remains elevated from historical levels. We also continue to experience increases in the infrastructure and operating costs of our dialysis centers primarily due to the number of new dialysis centers opened, and general increases in rent utilities and repairs and maintenance. In 2020,2023, we continued to implement certain cost control initiatives to help manage our overall operating costs, including labor productivity, and we expect to continue these initiatives in 2021.2024.
Our U.S. dialysis general and administrative expenses represented 9.0%10.1% and 8.1%9.8% of our U.S. dialysis revenues in 20202023 and 2019,2022, respectively. Increases in general and administrative expenses over the last several years were primarily related to strengthening our dialysis business and related compliance and operational processes, responding to certain legal and compliance matters, professional fees associated with enhancing our information technology (IT) systems, such as our new clinical system, and more recentrecently severance costs related to planned administrative efficiencies and advocacy costs in 20202022 related to countering union policy efforts. We expect that these levels of general and administrative expenses will be impacted by lower advocacy costs in 2021 compared to 2020, offset by continued investment in developing our capabilities and executing on our strategic priorities, among other things.
U.S. dialysis results of operations
Revenues:Treatment volume:
| | | | Year ended December 31, | | Annual change | | Year ended December 31, | | Annual change |
| | | 2020 | | 2019 | | Amount | | Percent | | 2023 | | 2022 | | Amount | | Percent |
| | (dollars in millions, except per treatment data) |
| Total revenues | $ | 10,660 | | | $ | 10,563 | | | $ | 97 | | | 0.9 | % |
| Dialysis treatments | Dialysis treatments | 30,314,619 | | | 30,172,699 | | | 141,920 | | | 0.5 | % | Dialysis treatments | 28,910,177 | | | 28,954,433 | | 28,954,433 | | | (44,256) | | (44,256) | | | (0.2) | | (0.2) | % |
| Average treatments per day | Average treatments per day | 96,667 | | | 96,398 | | | 269 | | | 0.3 | % | Average treatments per day | 92,542 | | | 92,506 | | 92,506 | | | 36 | | 36 | | | — | | — | % |
| Treatment days | Treatment days | 313.6 | | | 313.0 | | | 0.6 | | | 0.2 | % | Treatment days | 312 | | | 313 | | 313 | | | (1) | | (1) | | | (0.2) | | (0.2) | % |
| Average patient service revenue per treatment | $ | 350.31 | | | $ | 349.02 | | | $ | 1.29 | | | 0.4 | % |
Normalized non-acquired treatment growth(1) | Normalized non-acquired treatment growth(1) | 1.0% | | 2.2% | | (1.2) | % | Normalized non-acquired treatment growth(1) | (0.1) | % | | (2.0) | % | | | | 1.9 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.numbers
(1)Normalized non-acquired treatment growth reflects year over year growth in treatment volume, adjusted to exclude acquisitions and other similar transactions, and further adjusted to normalize for the number and mix of treatment days in a given period versus the prior period.
Our U.S. dialysis treatment volume is directly correlated with our operating revenues in 2020 increased primarily due to an increase in dialysis treatments and an increase in our average patient service revenue per treatment.expenses. The increasedecrease in our U.S. dialysis treatments in 2023 was primarily driven by approximately one additionalfewer treatment day in 2020 compared to 2019 and an increase in acquired and non-acquired treatments, partially offset by the deconsolidation of two dialysis partnerships, as described below under the heading "Equity investment income". Treatments were negatively impacted by higher mortality than experienced historically as well as a decline in new admissions. We believe the increased mortality rate is largely attributable to the impact of COVID-19 on our patient population. Our U.S. dialysis revenues were positively impacted by an increase in our average patient service revenue per treatment driven by favorable changes in government rate, including an increase in Medicare rates due to a base rate increase in 2020 and the temporary suspension of Medicare sequestration as well as an increase in hospital inpatient dialysis services revenue per treatment, partially offset by a decline in calcimimetics reimbursement.days.
Operating expenses and charges:
| | | | | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, | | Annual change |
| | 2020 | | 2019 | | Amount | | Percent |
| | (dollars in millions, except per treatment data) |
| Patient care costs | $ | 7,222 | | | $ | 7,219 | | | $ | 3 | | | — | % |
General and administrative(1) | 958 | | | 857 | | | 101 | | | 11.8 | % |
| Depreciation and amortization | 595 | | | 583 | | | 11 | | | 1.9 | % |
| Equity investment income | (33) | | | (22) | | | (11) | | | (50.0) | % |
| Total operating expenses and charges | $ | 8,742 | | | $ | 8,638 | | | $ | 104 | | | 1.2 | % |
| Patient care costs per treatment | $ | 238.24 | | | $ | 239.27 | | | $ | (1.03) | | | (0.4) | % |
| | | | | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, | | Annual change |
| | 2023 | | 2022 | | Amount | | Percent |
| | (dollars in millions, except per treatment data) |
| Total revenues | $ | 10,937 | | | $ | 10,600 | | | $ | 337 | | | 3.2 | % |
| Average patient service revenue per treatment | $ | 377.44 | | | $ | 365.24 | | | $ | 12.20 | | | 3.3 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.numbers
U.S. dialysis average patient service revenue per treatment increased primarily due to normal annual rate increases, including a net increase in Medicare rates due to a base rate increase in 2023, partially offset by the phased-in increase of sequestration of 1% in April 2022 and the full 2% beginning July 1, 2022 and thereafter. Other drivers of this change include improved cash collections including on previously reserved balances assumed to be uncollectible, and favorable changes in commercial and MA mix.
Operating expenses and charges:
| | | | | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, | | Annual change |
| | 2023 | | 2022 | | Amount | | Percent |
| | (dollars in millions, except per treatment data) |
| Patient care costs | $ | 7,395 | | | $ | 7,334 | | | $ | 61 | | | 0.8 | % |
General and administrative(1) | 1,102 | | | 1,038 | | | 64 | | | 6.2 | % |
| Depreciation and amortization | 696 | | | 691 | | | 5 | | | 0.7 | % |
| Equity investment income | (30) | | | (28) | | | (2) | | | (7.1) | % |
| Total operating expenses and charges | $ | 9,162 | | | $ | 9,034 | | | $ | 128 | | | 1.4 | % |
| Patient care costs per treatment | $ | 255.78 | | | $ | 253.31 | | | $ | 2.47 | | | 1.0 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers
(1)General and administrative expenses for the year ended December 31, 20202022 included advocacy costs of approximately $67$51 million incurred to counter union policy efforts, including a California statewide ballot initiative.initiative (CA Proposition 29).
Charges impacting operating income
Closure costs. During the year ended December 31, 2023, we continued the strategic review of our outpatient clinic capacity requirements and utilization, which have been impacted both by declines in our patient census in some markets due to the COVID-19 pandemic as well as by our initiatives toward, and advances in, increasing the proportion of our home dialysis patients. This continuing review, begun in the third quarter of 2022, has resulted in higher than normal charges for center capacity closures since its initiation. These capacity closure costs include net losses on assets retired, lease costs, asset impairments and accelerated depreciation and amortization.
During the year ended December 31, 2023, U.S. dialysis center closure costs were approximately $99.1 million, which increased our patient care costs by $28.0 million, our general and administrative expenses by $20.6 million and our depreciation and amortization expense by $50.5 million. By comparison, during the year ended December 31, 2022, U.S. dialysis center closures were approximately $85.7 million, which increased our patient care costs by $20.7 million, our general and administrative expenses by $19.2 million and our depreciation and amortization expense by $45.8 million.
In the upcoming fiscal year, we will continue to optimize our U.S. dialysis center footprint through center mergers and/or closures and expect our center closure levels to mirror the current year's elevated closure levels.
Severance costs. During the fourth quarter of 2022, we committed to a plan to increase efficiencies and cost savings in certain general and administrative support functions. As a result of this plan, we recognized expenses related to termination and other benefit commitments in our U.S. dialysis business of $26.7 million and $17.0 million during the twelve months ended December 31, 2023 and 2022, respectively.
Patient care costs. U.S. dialysis patient care costs are those costs directly associated with operating and supporting our dialysis centers and consist principally of compensation expenses including labor and benefits, pharmaceuticals, medical supplies and other operating costs of the dialysis centers.
U.S. dialysis patient care costs per treatment decreasedincreased primarily due to increased compensation expenses including increased wage rates and headcount, as well as increases in medical supply costs, routine repairs and maintenance, health benefit expenses, professional fees and utilities expense. Other drivers of this change include increases in travel costs, other direct operating expenses associated with our dialysis centers, office equipment expense, and center closure costs, as described above. These increases were partially offset by decreases in pharmaceutical unit costs as well as decreased travel expenses due to COVID-19. These decreases were partially offset by an increase in labor costs and COVID-19-related costs, including compensation, medical supplies and teammate relief reimbursement and benefit program expenses.contract wages.
General and administrative expenses. U.S. dialysis general and administrative expenses in 2020 increased primarily due to an increaseincreases in advocacycompensation expense including increased wage rates and severance costs, incurred to counter union policy efforts, including those related to a California ballot initiative. Theseas described above. Other drivers of this change include higher gains recognized on the sale of our self-developed properties in 2022 and increases were also driven byin IT-related costs, contributions to our charitable foundation, labortravel costs, long-term incentive compensation and COVID-19-related costs, including compensationmarketing and advertising expenses. These increases were partially offset by a decreasedecreases in travel expenses due to COVID-19advocacy costs and a decrease in long-term incentive compensation expense.professional fees.
Depreciation and amortization. Depreciation and amortization expense is directly impacted by the number of our dialysis centers and the information technology that we develop and acquire.acquire as well as changes in useful lives of assets. U.S. dialysis depreciation and amortization expense increased in 2023 primarily due to growth in the number of dialysis centers we operate.accelerated depreciation for expected center closures, as described above.
Equity investment income. U.S. dialysis equity investment income increased primarily due to the deconsolidation of two of our near 50%-ownedincreased profitability at certain nonconsolidated dialysis partnerships at year-end 2019, based on a reassessment of relative rights and powers over these partnerships. Our portion of these partnerships' earnings are now recognized in equity investment income.
Operating income and adjusted operating income
| | | | Year ended December 31, | | Annual change | | Year ended December 31, | | Annual change |
| | | 2020 | | 2019 | | Amount | | Percent | | 2023 | | 2022 | | Amount | | Percent |
| (dollars in millions) |
| (dollars in millions) | | | (dollars in millions) |
| Operating income | Operating income | $ | 1,918 | | | $ | 1,925 | | | $ | (7) | | | (0.4) | % | Operating income | $ | 1,775 | | | $ | | $ | 1,565 | | | $ | | $ | 210 | | | 13.4 | | 13.4 | % |
Adjusted operating income(1) | Adjusted operating income(1) | $ | 1,918 | | | $ | 1,925 | | | $ | (7) | | | (0.4) | % | Adjusted operating income(1) | $ | 1,900 | | | $ | | $ | 1,668 | | | $ | | $ | 232 | | | 13.9 | | 13.9 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
(1)For a reconciliation of adjusted operating income by reportable segment, see the "Reconciliations of non-GAAP measures" section below.
U.S. dialysis operating income was negatively impacted by center closure and severance costs, as described above. Operating income and adjusted operating income in 2020 decreasedincreased compared to 20192022 primarily due to a decrease in calcimimetics margin, increases in labor costs, advocacy costs and charitable contributions; and an increase in COVID-19-related expenses, including compensation, medical supplies, and reimbursement and benefit program expenses, as described above. These decreases to operating income were partially offset by volume growth from approximately one additional treatment day in the year and an increase in our average dialysis patient service revenue per treatment, as described above, as well asand decreases in pharmaceutical unit costs, travelcontract wages and advocacy costs. These increases in operating income and adjusted operating income were partially offset by increases in compensation expenses and decreased gains on sale, each described above, as well as increased costs related to travel, contributions to our foundation, medical supply costs, routine repairs and maintenance, IT-related costs, health benefit expenses and utilities expense. Operating income and adjusted operating income were also impacted by decreased dialysis treatment volume, described above, and increases in other direct operating expenses associated with our dialysis centers, long-term incentive compensation, marketing and advertising expense and office equipment expense.
Other - Ancillary services
Our other operations include ancillary services that are primarily aligned with our core business of providing dialysis services to our network of patients. As of December 31, 2020,2023, these consisted primarily of integrated care (DaVita IKC), ESRD seamless care organizations (ESCOs),our IKC business, certain U.S. other ancillary businesses (including our clinical research programs, (DaVita Clinical Research)transplant software business, and venture investment group), and physician services, as well as our international operations.
These ancillary services, including our international operations, generated revenues of approximately $1.053$1.299 billion in 2020,2023, representing approximately 9%11% of our consolidated revenues.
As further describedof December 31, 2023, DaVita IKC provided integrated care and disease management services to approximately 58,000 patients in the risk factorrisk-based integrated care arrangements and to an additional 17,000 patients in Item 1A. Risk Factors under the heading, "Our ancillary services and strategic initiatives, including, without limitation, our international operations, that we operate or invest in now or in the future may generate losses and may ultimately be unsuccessful. In the event that one or more of these activities is unsuccessful, our business, results of operations, financial condition and cash flows may be negatively impacted and we may have to write off our investment and incur other exit costs," if any of our ancillary services or strategic initiatives, such as our international operations, are unsuccessful, it could have a negative impact on our business, results of operations, financial condition and cash flows, and we may determine to exit that line of business, which could result in significant termination costs. In addition, we have in the past and may in the future incur material write-offs or impairments of our investments, including goodwill, in one or more of these ancillary services.
integrated care arrangements. We also expect to add additional service offerings to our business and pursue additional strategic initiatives in the future as circumstances warrant, which could include, among other things, healthcare services not related to dialysis.kidney disease.
For a discussion of the risks related to IKC and our ancillary services, see the discussion in the risk factors in Item 1A. Risk Factors under the headings, "The U.S. integrated kidney care, U.S. other ancillary services and international operations that we operate or invest in now or in the future..." and "If we are not able to successfully implement our strategy with respect to our integrated kidney care and value-based care initiatives..."
As of December 31, 2020,2023, our international dialysis operations provided dialysis and administrative services through a total of 321business owned or operated 367 outpatient dialysis centers located in ten11 countries outside of the U.S. For 2020,2023, total revenues generated from our international operations were approximately 5%6% of our consolidated revenues.
Ancillary services results of operations
| | | | Year ended December 31, | | Annual change | | Year ended December 31, | | Annual change |
| | | 2020 | | 2019 | | Amount | | Percent | | 2023 | | 2022 | | Amount | | Percent |
| (dollars in millions) |
| (dollars in millions) | | | (dollars in millions) |
| Revenues: | Revenues: | |
| U.S. ancillary | $ | 489 | | | $ | 464 | | | $ | 25 | | | 5.4 | % |
| U.S. IKC | |
| U.S. IKC | |
| U.S. IKC | | $ | 511 | | | $ | 378 | | | $ | 133 | | | 35.2 | % |
| U.S. other ancillary | | U.S. other ancillary | 25 | | | 23 | | | 2 | | | 8.7 | % |
| International | International | 564 | | | 508 | | | 56 | | | 11.0 | % | International | 763 | | | 700 | | 700 | | | 63 | | 63 | | | 9.0 | | 9.0 | % |
| Total ancillary services revenues | Total ancillary services revenues | $ | 1,053 | | | $ | 972 | | | $ | 81 | | | 8.3 | % | Total ancillary services revenues | $ | 1,299 | | | $ | | $ | 1,101 | | | $ | | $ | 198 | | | 18.0 | | 18.0 | % |
| | Operating (loss) income: | Operating (loss) income: | |
| U.S. ancillary | $ | (99) | | | $ | (66) | | | $ | (33) | | | (50.0) | % |
| Operating (loss) income: | |
| Operating (loss) income: | |
| U.S. IKC | |
| U.S. IKC | |
| U.S. IKC | | $ | (39) | | | $ | (125) | | | $ | 86 | | | 68.8 | % |
| U.S. other ancillary | | U.S. other ancillary | (25) | | | (9) | | | (16) | | | (177.8) | % |
International(1) | International(1) | 23 | | | (123) | | | 146 | | | 118.7 | % | International(1) | 55 | | | 37 | | 37 | | | 18 | | 18 | | | 48.6 | | 48.6 | % |
| Total ancillary services loss | Total ancillary services loss | $ | (76) | | | $ | (189) | | | $ | 113 | | | 59.8 | % | Total ancillary services loss | $ | (9) | | | $ | | $ | (97) | | | $ | | $ | 88 | | | 90.7 | | 90.7 | % |
| Adjusted operating (loss) income(2): | Adjusted operating (loss) income(2): | |
| U.S. ancillary | $ | (83) | | | $ | (66) | | | $ | (17) | | | (25.8) | % |
Adjusted operating (loss) income(2): | |
Adjusted operating (loss) income(2): | |
| U.S. IKC | |
| U.S. IKC | |
| U.S. IKC | | $ | (93) | | | $ | (124) | | | $ | 31 | | | 25.0 | % |
| U.S. other ancillary | | U.S. other ancillary | (7) | | | (9) | | | 2 | | | 22.2 | % |
International(1) | International(1) | 23 | | | 2 | | | 21 | | | 1,050.0 | % | International(1) | 55 | | | 44 | | 44 | | | 11 | | 11 | | | 25.0 | | 25.0 | % |
| Total adjusted operating loss: | Total adjusted operating loss: | $ | (60) | | | $ | (64) | | | $ | 4 | | | 6.3 | % | Total adjusted operating loss: | $ | (45) | | | $ | | $ | (89) | | | $ | | $ | 44 | | | 49.4 | | 49.4 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
(1)The reported operating income (loss) and adjusted operating income for the years ended December 31, 20202023 and December 31, 2019, include2022, includes foreign currency losses embedded in equity method income recognized from our APAC joint venture of approximately $3$(1.6) million and $2$(0.3) million, respectively, of foreign currency losses.respectively.
(2)For a reconciliation of adjusted operating (loss) income by reportable segment, see the "Reconciliations of non-GAAP measures" section below.
Revenues:
Our U.S. ancillary servicesIKC revenues were impacted by an increase in 2020 increased due toshared savings from our VBC contracts and an increase in revenues atfrom our integrated care business,special needs plans. Our U.S. other ancillary services revenues were impacted by increased revenues in our clinical research programs. Our international revenues increased due to acquisition-related growth as well as average reimbursement rate increases in certain countries.
Items impacting operating income
IKC adjustment. The increase in IKC revenues for 2023, as described above, was primarily due to the lifting of certain revenue increasesrecognition constraints for some of our value-based care contracts with health plans, allowing us to recognize approximately $55 million in incremental shared savings revenues.
Severance and other costs. During the fourth quarter of 2022, similar to U.S. dialysis, we committed to a plan to increase efficiencies and cost savings in certain general and administrative support functions and other overhead costs. As a result of this plan, we recognized expenses related to termination and other benefit commitments in our special needs plans,IKC business of $0.4 million during the year ended December 31, 2023. By comparison, during the twelve months ended December 31, 2022, we recognized expenses related to termination and other benefit commitments in our IKC business, and similar expenses and other charges in our international operations, of $0.5 million and $7.5 million, respectively.
Goodwill impairment charge and related items. During the fourth quarter of 2023, we recognized a goodwill impairment charge of $26.1 million in our transplant software business. We also recognized a gain of $7.7 million due to a reduction in the estimated value of earn-out obligations from our original acquisition of this business. This impairment charge and related gain resulted from a reduction in estimated fair value for the business driven primarily from the business not achieving its revenue targets, with reduced revenue expectations for future years, as well as an increase in revenues in our ESCO and physician services businesses. These increases were partially offset by a decrease in revenue in our clinical research programs, as well as due to the sale of Lifeline, as described below. Our international revenues increased primarily as a result of acquired treatment growth as we continue to expand our international business.risk-free rate.
Charges impacting operating income:
Loss on changes in ownership interests, net. We sold 100% of the stock of Lifeline, our vascular access business, effective May 1, 2020 and recognized a loss of approximately $16 million on this transaction.
Goodwill impairment charges. During 2019, we recognized goodwill impairment charges of $125 million in our international reporting units. See further discussion of these impairment charges and our reporting units that remain at risk of goodwill impairment in Note 10 to the consolidated financial statements.
Operating loss and adjusted operating loss:
Our U.S. ancillary servicesIKC operating loss in 2020 was negatively impacted by the loss on sale of Lifeline,IKC change in estimate, as described above, and both U.S. ancillaryabove. Our IKC operating loss and adjusted operating loss were negatively impacted by an increase in medical costsdecreased primarily due to COVID-19increased revenues, as described above, partially offset by continued investments in our integrated care businesssupport functions. Our U.S. other ancillary services operating loss was impacted by a goodwill impairment charge and a decrease in revenuerelated gain, as described above. Our U.S. other ancillary services operating loss and adjusted operating loss was impacted by improved performance in our clinical research programs,programs. Our international operating income in 2022 was impacted by severance and other costs in one of our international businesses, as described above. International operating income and adjusted operating income were impacted by acquisition-related growth, partially offset by increases in revenuesequity losses resulting from fluctuations in foreign currency at our integrated careAPAC JV and ESCO businesses. Internationalother direct operating results and adjusted operating results increased in 2020 compared to 2019. International operating results in 2019 were negatively impacted by goodwill impairment charges, as described above, and bothexpenses associated with our international operating results and adjusted operating results benefited in 2020 primarily from acquisition-related growth and the reduction of certain other periodic expenses, partially offset by increased medical supplies costs and higher mortality due to COVID-19.dialysis centers.
Corporate administrative support
Corporate administrative support consists primarily of labor, benefits and long-term incentive compensation expense, as well as professional fees, for departments which provide support to allmore than one of our various operating lines of business. In 2020, corporate support also included an accrual for legal matters. Corporate administrative support expenses are included in general and administrative expenses on our consolidated income statement.statement.
Accruals for legal matters. During 2020,2023, we recorded a net charge of $40 million for a legal matters of $35 million.matter within corporate administrative support.
Corporate administrative support expenses increased $54$33 million in 2020 primarily driven by accruals for legal matters, as described above. In addition, both corporate administrative support and adjusted corporate administrative supportabove, as well as increased compensation expenses, increasedincluding long-term incentive compensation, partially offset by higher legal fees in 2020 due to an increase in severance accruals recorded in the second quarter of 2020 associated with our senior executive leadership transition and an increase in long-term compensation expense.2022.
Corporate-level charges
| | | | Year ended December 31, | | Annual change | | Year ended December 31, | | Annual change |
| | | 2020 | | 2019 | | Amount | | Percent | | 2023 | | 2022 | | Amount | | Percent |
| (dollars in millions) |
| (dollars in millions) | | | (dollars in millions) |
| Debt expense | Debt expense | $ | 304 | | | $ | 444 | | | $ | (140) | | | (31.5) | % | Debt expense | $ | 399 | | | $ | | $ | 357 | | | $ | | $ | 42 | | | 11.8 | | 11.8 | % |
| Debt prepayment, refinancing and redemption charges | $ | 89 | | | $ | 33 | | | $ | 56 | | | 169.7 | % |
| Other income, net | $ | 17 | | | $ | 29 | | | $ | (13) | | | (44.8) | % |
| Debt extinguishment and modification costs | |
| Other (loss) income, net | |
| Other (loss) income, net | |
| Other (loss) income, net | | $ | (19) | | | $ | (16) | | | $ | (3) | | | (18.8) | % |
| Effective income tax rate | Effective income tax rate | 23.8 | % | | 23.4 | % | | 0.4 | % | Effective income tax rate | 18.7 | % | | 20.5 | % | | | | (1.8) | % |
Effective income tax rate from continuing operations attributable to DaVita Inc.(1) | Effective income tax rate from continuing operations attributable to DaVita Inc.(1) | 28.6 | % | | 28.3 | % | | 0.3 | % | Effective income tax rate from continuing operations attributable to DaVita Inc.(1) | 24.3 | % | | 26.5 | % | | | | (2.2) | % |
| Net income attributable to noncontrolling interests | Net income attributable to noncontrolling interests | $ | 221 | | | $ | 210 | | | $ | 11 | | | 5.2 | % | Net income attributable to noncontrolling interests | $ | 265 | | | $ | | $ | 221 | | | $ | | $ | 44 | | | 19.9 | | 19.9 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
(1)For a reconciliation of our effective income tax rate from continuing operations attributable to DaVita Inc., see the "Reconciliations of non-GAAP measures" section below.
Debt expense
Debt expense decreasedincreased primarily due to an increase in our overall weighted average effective interest rate, partially offset by a decrease in our outstanding debt balances and a decrease in theweighted average credit facility balance outstanding. Our overall weighted average effective interest rate on ourall debt, in 2020. Our overall weighted average effectiveincluding the effect of interest rate caps and amortization of debt discount, was 4.52% in 2020 was 3.59%2023 compared to 5.01%3.96% in 2019.2022. See Note 1312 to the consolidated financial statements for further information on the components of our debt and changes in them since 2019.
Debt prepayment, refinancingextinguishment and redemption chargesmodification costs
Debt prepayment, refinancingextinguishment and redemptionmodification charges were $89$8 million in 2020 as a result2023 related to the refinancing of the redemption in full of both our $1.75 billion aggregate principal amount outstanding of 5.125% senior notes and our $1.50 billion aggregate principal amount outstanding of 5.0% senior notes. These 2020 charges represented debt redemption premium charges and deferred financing cost write-offs associated with our prior senior note debt that was paid in full. These charges recognized in 2020 also included $3 million of refinancing charges comprised partially of fees incurred on the repricing of our Term Loan BA and prior revolving line of credit. These costs were composed partially of deferred financing costs written off for the portion of this debt considered extinguished and reborrowed. In 2019, wereborrowed and partially of fees incurred as part of this debt prepayment, refinancing and redemption charges of $33 million as a result of the repayment of all principal balances outstanding under our prior senior secured credit facilities and the redemption of our $1.25 billion aggregate principal amount outstanding of 5.75% senior notes. See further discussion of our 2020 debt prepayment, refinancing and redemption charges in Note 13 to the consolidated financial statements.refinancing.
Other (loss) income
Other (loss) income consists primarily of interest income on cash and cash equivalents and short- and long-term investments, equity investment (loss) income on equity method investments other than dialysis partnerships, realized and
unrealized gains and losses recognized on other investments, impairments on investments, and foreign currency transaction gains and losses. Other income decreased in 2020loss increased primarily due to a decreaseequity investment losses on our new investment in Mozarc which was net of the $15 million gain from the non-cash asset contributed at close. This was partially offset by decreased losses recognized on other investments and an increase in interest income on our holdings of cash and cash equivalents in 2020 and a decrease in foreign currency transaction gains.income.
Provision for income taxes
TheOur effective income tax rate and effective income tax rate from continuing operations attributable to DaVita Inc. increaseddecreased in 20202023 primarily due to an increasedecreases in nondeductible advocacy expenses and benefits realized from tax returns finalized during the year. These decreases were partially offset by nondeductible costs and the impact ofrelated to a discrete benefit included in the 2019 tax rate fromlegal matter and a reduction in the blended state rate. This increase was partially offset by a reductionbenefits recognized for stock compensation in accruals associated with uncertain tax positions in 2020.2023.
Net income attributable to noncontrolling interests
The increase in income attributable to noncontrolling interests in 2020 compared to 2019 was due to improvedan increase in earnings at certain U.S. dialysis partnerships, including, among other things, reimbursements we made to certain of our partnerships.
U.S. dialysis partnerships for certain COVID-19-related expenses, partially offset by the deconsolidation of two dialysis partnerships at year-end 2019.
Accountsaccounts receivable
Our consolidatedU.S. dialysis accounts receivable balances at December 31, 20202023 and December 31, 2019,2022 were $1.824$1.632 billion and $1.796$1.899 billion, respectively, representing approximately 5954 days and 5866 days of revenue (DSO), respectively, net of allowances for uncollectible accounts.respectively. The increasedecrease in consolidated DSO was primarily due to an increase of one day of DSO in our U.S. dialysis business primarily due to held claims for COVID-19-related cohort arrangement billings as well as claimsstrong collections from centers impacted by hurricanes in the fourth quarter of 2020.non-Medicare payors and Medicare timing recoveries. Our DSO calculation is based on the currentmost recent quarter’s average revenues per day. There were no significant changes during 20202023 from 20192022 in the carrying amount of unreserved accounts receivable outstanding over one year old or in the amounts pending approval from third-party payors.
As of December 31, 20202023 and 2019,2022, our net patient servicesU.S. dialysis accounts receivable balances that are more than six months old representsrepresented approximately 17% and 18%, respectively19% of our total netU.S. dialysis accounts receivable balances outstanding. Substantially all revenue realized for patient services is received from government and commercial payors, as discussed above. There were no significant unreserved balances over one year old. Less than 1% of our revenues arein both periods were classified as patient pay.
Amounts pending approval from third-party payors associated with Medicare bad debt claims as of December 31, 20202023 and 2019,2022, other than the standard monthly billing, consisted ofwere approximately $154$107 million and $138$111 million, respectively, and are classified aswithin other receivables. A significant portion of our Medicare bad debt claims are typically paid to us before the Medicare fiscal intermediary audits the claims but are subject to subsequent adjustment based upon the actual results of those audits. Such audits typically occur one to four years after the claims are filed.
Liquidity and capital resources
The following table summarizes our major sources and uses of cash, cash equivalents and restricted cash:
| | Year ended December 31, | | Annual change |
| 2020 | | 2019(1) | | Amount | | Percent |
| (dollars in millions) |
| Year ended December 31, | | | Year ended December 31, | | Annual change |
| 2023 | | | 2023 | | 2022 | | Amount | | Percent |
| (dollars in millions) | | | (dollars in millions) |
| Net cash provided by operating activities: | Net cash provided by operating activities: | |
| Net income | |
| Net income | |
| Net income | Net income | $ | 995 | | | $ | 1,021 | | | $ | (27) | | | (2.6) | % | $ | 957 | | | $ | | $ | 782 | | | $ | | $ | 175 | | | 22.4 | | 22.4 | % |
| Non-cash items in net income | Non-cash items in net income | 1,089 | | | 964 | | | 124 | | | 12.9 | % | Non-cash items in net income | 908 | | | 783 | | 783 | | | 125 | | 125 | | | 16.0 | | 16.0 | % |
| Other working capital changes | Other working capital changes | (78) | | | 111 | | | (190) | | | (171.2) | % | Other working capital changes | 209 | | | 66 | | 66 | | | 143 | | 143 | | | 216.7 | | 216.7 | % |
| Other | Other | (26) | | | (24) | | | (1) | | | (4.2) | % | Other | (14) | | | (66) | | (66) | | | 52 | | 52 | | | 78.8 | | 78.8 | % |
| $ | | | $ | 2,059 | | | $ | 1,565 | | | $ | 494 | | | 31.6 | % |
| | $ | 1,979 | | | $ | 2,072 | | | $ | (93) | | | (4.5) | % |
| | Net cash (used in) provided by investing activities: | |
| Net cash used in investing activities: | |
| Net cash used in investing activities: | |
| Net cash used in investing activities: | |
| Capital expenditures: | |
| Capital expenditures: | |
| Capital expenditures: | Capital expenditures: | |
| Routine maintenance/IT/other | Routine maintenance/IT/other | $ | (399) | | | $ | (375) | | | $ | (24) | | | (6.4) | % |
| Development and relocations | (275) | | | (391) | | | 116 | | | 29.7 | % |
| Routine maintenance/IT/other | |
| Routine maintenance/IT/other | | $ | (406) | | | $ | (431) | | | $ | 25 | | | 5.8 | % |
| Developments and relocations | | Developments and relocations | (162) | | | (172) | | | 10 | | | 5.8 | % |
| Acquisition expenditures | Acquisition expenditures | (182) | | | (101) | | | (81) | | | (80.2) | % | Acquisition expenditures | (26) | | | (57) | | (57) | | | 31 | | 31 | | | 54.4 | | 54.4 | % |
| Proceeds from sale of self-developed properties | Proceeds from sale of self-developed properties | 93 | | | 58 | | | 36 | | | 62.1 | % | Proceeds from sale of self-developed properties | 11 | | | 109 | | 109 | | | (98) | | (98) | | | (89.9) | | (89.9) | % |
| DMG net sale proceeds received, net of DMG cash sold | (47) | | | 3,825 | | | (3,872) | | | (101.2) | % |
| | Other | Other | (15) | | | (20) | | | 5 | | | 25.0 | % |
| $ | (825) | | | $ | 2,995 | | | $ | (3,821) | | | (127.6) | % |
| Other | |
| Other | | (189) | | | (78) | | | (111) | | | (142.3) | % |
| $ | | | $ | (772) | | | $ | (630) | | | $ | (142) | | | (22.5) | % |
| | Net cash used in financing activities: | Net cash used in financing activities: | |
| Debt (payments) issuances, net | $ | (64) | | | $ | (1,995) | | | $ | 1,931 | | | 96.8 | % |
| Net cash used in financing activities: | |
| Net cash used in financing activities: | |
| Debt payments, net | |
| Debt payments, net | |
| Debt payments, net | | $ | (550) | | | $ | (11) | | | $ | (539) | | | (4,900.0) | % |
| Deferred financing and debt redemption costs | Deferred financing and debt redemption costs | (106) | | | (85) | | | (21) | | | (24.7) | % | Deferred financing and debt redemption costs | (70) | | | — | | — | | | (70) | | (70) | | | (100.0) | | (100.0) | % |
| Distributions to noncontrolling interests | Distributions to noncontrolling interests | (253) | | | (233) | | | (20) | | | (8.6) | % | Distributions to noncontrolling interests | (281) | | | (268) | | (268) | | | (13) | | (13) | | | (4.9) | | (4.9) | % |
| Contributions from noncontrolling interests | Contributions from noncontrolling interests | 43 | | | 57 | | | (14) | | | (24.6) | % | Contributions from noncontrolling interests | 15 | | | 15 | | 15 | | | — | | — | | | — | | — | % |
| Stock award exercises and other share issuances | Stock award exercises and other share issuances | (1) | | | 11 | | | (12) | | | (109.1) | % | Stock award exercises and other share issuances | (48) | | | (37) | | (37) | | | (11) | | (11) | | | (29.7) | | (29.7) | % |
| Share repurchases | Share repurchases | (1,458) | | | (2,384) | | | 925 | | | 38.8 | % | Share repurchases | (272) | | | (802) | | (802) | | | 530 | | 530 | | | 66.1 | | 66.1 | % |
| Other | Other | (8) | | | (68) | | | 60 | | | 88.2 | % | Other | 35 | | | (17) | | (17) | | | 52 | | 52 | | | 305.9 | | 305.9 | % |
| $ | (1,847) | | | $ | (4,696) | | | $ | 2,850 | | | 60.7 | % |
| $ | | | $ | (1,170) | | | $ | (1,121) | | | $ | (49) | | | (4.4) | % |
| | Total number of shares repurchased | Total number of shares repurchased | 16,477,378 | | | 41,020,232 | | | (24,542,854) | | | (59.8) | % |
| Total number of shares repurchased | |
| Total number of shares repurchased | | 2,903,832 | | | 8,094,661 | | | (5,190,829) | | | (64.1) | % |
| Free cash flow from continuing operations(2) | $ | 1,188 | | | $ | 1,127 | | | $ | 61 | | | 5.4 | % |
Free cash flow(1) | |
Free cash flow(1) | |
Free cash flow(1) | | $ | 1,236 | | | $ | 817 | | | $ | 419 | | | 51.3 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
(1)Represents consolidated cash flow activity, including cash flows related to discontinued operations.
(2)For a reconciliation of our free cash flow, from continuing operations, see the "Reconciliations of Non-GAAP measures" section below.
Consolidated cash flows
Consolidated cash flows from operating activities for 20202023 and 2022 were $1,979$2,059 million all of which was from continuing operations, compared with consolidated operating cash flows for the same period in 2019 of $2,072and $1,565 million, of which $1,973 million was from continuing operations.respectively. The increase in cash flowflows from continuing operations was primarily driven by a decreaseimprovements in operating results and cash collections on accounts receivable as well as decreases in cash interesttaxes paid partially offset by COVID-19-related expenses in 2020, and increases in laborinterest payments on debt and advocacy costs,other working capital items.
Cash flows used for investing activities in 2023 increased $142 million compared to 2022 primarily due to a decrease in proceeds received on self-developed properties as well as an increaseincreases in DSO of approximately one dayequity investments including the investment in 2020 compared to 2019.Mozarc. These increases were partially offset by decreases in acquisition expenditures combined with decreases in capital expenditures.
Cash flows from investingused in financing activities increased $49 million in 2020 decreased $3,821 million2023 compared to 2019 primarily due to2022. Significant uses of cash during 2023 consisted of the netpay-off of the remaining principal balance outstanding on our prior Term Loan A and prior revolving line of credit in the amount of $1,444 million and $150 million, respectively. Other uses of cash proceeds received from the DMG sale, which closed in June 2019, as well as an increase in acquisition expenditures partially offset by a decrease in capital expenditures. We developed 31 fewer centersincluded regularly scheduled and acquired 51 additional centers in 2020 compared to 2019. See below for additional information regarding the growth inother principal payments under our dialysis centers.senior secured credit facilities totaling approximately $54 million on our prior Term Loan
Cash flows from financing activities improved $2,850A, $16 million in 2020 compared to 2019. Significant sourceson our new Term Loan A-1, described below, $57 million on Term Loan B-1, additional net repayments of cash during 2020 included issuances of $1,500 million in aggregate principal amount of 3.75% senior notes due 2031 in August 2020 and $1,750 million in aggregate principal amount of 4.625% senior notes due 2030 in June 2020, as well as a net draw of $75$15 million on our revolving line of credit.credit, as well as additional required payments under other debt arrangements. Additionally, we recognized financing cash outflows of $30 million in deferred financing costs related to the Amendments to the Senior Secured Credit Agreement and $40 million in cap premium fees for our 2023 forward interest cap agreements. Significant usessources of cash during 2020the period included the subsequent redemptionsrefinancing of the Term Loan A and revolving line of credit with a secured Term Loan A-1 facility in full of $1,500 million inthe aggregate principal amount of 5.0% senior notes due 2025 in August 2020 and $1,750$1,250 million. During the year ended December 31, 2023 we also used cash to repurchase 2,903,832 shares of our common stock.
By comparison, 2022 included a net draw of $165 million in aggregate principal amounton our prior revolving line of 5.125% senior notes due 2024 in July 2020. Othercredit, net debt payments during 2020 primarilywhich consisted of regularly scheduled mandatory principal payments under our senior secured credit facilities totaling approximately $55$98 million on our prior Term Loan A and $27 million on Term Loan B-1, andas well as additional required principal payments under other debt arrangements. In addition, during the twelve months ended December 31, 2022 we incurred bond issuance costs of approximately $38 million, debt redemption premium charges relatedused cash to the redemptionrepurchase 8,094,661 shares of our senior notes due in 2024 and 2025 of approximately $67 million and costs of repricing our Term Loan B of approximately $3 million. See further discussion in Note 13 to the consolidated financial statements related to debt financing activities. By comparison, in 2019 debt payments primarily consisted of principal prepayments totaling $5,142 million on our term debt under our prior senior secured credit facility funded primarily by the net proceeds from the DMG sale and the redemption of all of our outstanding 5.75% senior notes due in 2022 for an aggregate cash payment consisting of principal and redemption premium of $1,262 million, partially offset by funding of our term debt of $4,500 million under our new senior credit facility. Cash flows used for share repurchases also decreased in 2020 as compared to 2019. See below for further information on our share repurchases.common stock.
Dialysis center capacity and growth
We are typically able to increase our capacity by extending hours at our existing dialysis centers, expanding our existing dialysis centers, relocating our dialysis centers, developing new dialysis centers and by acquiring dialysis centers. The development of a typical new outpatient dialysis center generally requires approximately $2.4$2 million for leasehold improvements and other capital expenditures. Based on our experience, a new outpatient dialysis center typically opens within a year after the property lease is signed, normally achieves operating profitability in the second year after Medicare certification, and normally reaches maturity within three to five years. Acquiring an existing outpatient dialysis center requires a substantially greater initial investment, but profitability and cash flows are generally accelerated and more predictable. To a limited extent, we enter into agreements to provide management and administrative services to outpatient dialysis centers in which we own a noncontrolling interest or which are wholly-owned by third parties in return for management fees.
The table below shows the growth in our dialysis operations by number of dialysis centers owned or operated:
| | U.S. | | International |
| U.S. | | | U.S. | | International |
| | | 2020 | | 2019 | | 2020 | | 2019 | | 2023 | | 2022 | | 2023 | | 2022 |
| Number of centers operated at beginning of year | Number of centers operated at beginning of year | 2,753 | | | 2,664 | | | 259 | | | 241 | |
| Acquired centers | Acquired centers | 8 | | | 7 | | | 66 | | | 16 | |
| Developed centers | Developed centers | 81 | | | 115 | | | 5 | | | 2 | |
Net change in non-owned managed or administered centers(1) | Net change in non-owned managed or administered centers(1) | — | | | (1) | | | (6) | | | 1 | |
Sold and closed centers(2) | Sold and closed centers(2) | (6) | | | (10) | | | — | | | (1) | |
Closed centers(3) | Closed centers(3) | (20) | | | (22) | | | (3) | | | — | |
| Number of centers operated at end of year | Number of centers operated at end of year | 2,816 | | | 2,753 | | | 321 | | | 259 | |
(1)Represents dialysis centers which we manage or provide administrative services to but in which we own a noncontrolling equity interest or which are wholly-owned by third parties, including our Asia Pacific joint venture centers.
(2)Represents dialysis centers that were sold and/or closed for which the majority of patients were not retained.
(3)Represents dialysis centers that were closed for which the majority of patients were retained and transferred to one of our other existing outpatient dialysis centers.
Stock repurchases
The following table summarizes our common stock repurchases during the years ended December 31, 20202023 and 2019:2022:
| | Year ended December 31, | | | Year ended December 31, |
| 2023 | | | 2023 | | 2022 |
| (dollars in millions and shares in thousands, except per share data) | | | (dollars in millions and shares in thousands, except per share data) |
| | | Year ended December 31, |
| | 2020 | | 2019 |
| | (dollars in millions and shares in thousands, except per share data) |
| Open market repurchases | |
| | Shares | |
| | Shares | |
| | Shares | Shares | 8,495 | | | 19,218 | |
| Amounts paid | Amounts paid | $ | 742 | | | $ | 1,168 | |
| Average paid per share | $ | 87.32 | | | $ | 60.79 | |
| Tender offers(1) | |
| Shares | 7,982 | | | 21,802 | |
| Amounts paid | $ | 705 | | | $ | 1,234 | |
| Average paid per share | $ | 88.32 | | | $ | 56.61 | |
| | Total | |
| Shares | 16,477 | | | 41,020 | |
| Amounts paid | $ | 1,447 | | | $ | 2,402 | |
| Average paid per share | $ | 87.80 | | | $ | 58.57 | |
| Average price paid per share | |
(1)The aggregate amounts paid for shares repurchased pursuant to our 2020 and 2019 tender offers for our shares during the years ended December 31, 2020 and 2019, include their clearing prices of $88.00 and $56.50 per share, respectively, plus related fees and expenses of $2.5 million and $2.3 million, respectively.
Subsequent to December 31, 2020, we have repurchased 1,063,000 shares of our common stock for $123 million at an average cost of $115.98 per share from January 1, 2021 through February 10, 2021. We retired all shares of common stock held in treasury effective December 31, 20202023 and 2022. Subsequent to December 31, 2019.2023, we have repurchased 1,507,000 shares of or common stock for $164 million at an average price paid of $107.97 per share through February 12, 2024.
See further discussion of our share repurchase activity and authorizations in Note 1918 to the consolidated financial statements.
Available liquidity
As of December 31, 2020,2023, our cash balance was $325$380 million and we held approximately $20$12 million in short-term investments. At that time we also had $925 million available and $75 million drawnundrawn capacity on our $1.0 billionthe revolving line of credit under our senior secured credit facilities.facilities of $1.5 billion. Credit available under this revolving line of credit is reduced by the amount of any letters of credit outstanding under this facility, but we had no such lettersthereunder, of credit outstandingwhich there were none as of December 31, 2020.2023. As of December 31, 20202023 we also separately had approximately $65$151 million in letters of credit outstanding under a separate bilateral secured letter of credit facility.
See Note 1312 to the consolidated financial statements for components of our long-term debt and their interest rates.
The COVID-19 pandemic and efforts to prevent its spread have dramatically reduced global economic activity and driven increased volatility in the financial markets. We have maintained business process continuity during the COVID-19 pandemic by enabling most back office teammates to work remotely, and as of the date of this report, we have not experienced a material deterioration in our liquidity position as a result of the COVID-19 crisis. In addition, we elected not to accept approximately $250 million in funds available to us through the CARES Act Provider Relief Fund and returned the funds we received in May 2020. There can be no assurance that we will be able to continue to forgo financial or other assistance available under the CARES Act or similar subsequent legislation or that similar assistance will be available from the government if we have a need for such assistance in the future. The ultimate impact of the pandemic will depend on future developments that are highly uncertain and difficult to predict.
We believe that our cash flowflows from operations and other sources of liquidity, including from amounts available under our senior secured credit facilities and our access to the capital markets, will be sufficient to fund our scheduled debt service under the terms of our debt agreements and other obligations for the foreseeable future, including the next 12 months. From time to time, depending on market conditions, our capital requirements and the availability of financing, among other things, we may seek to refinance our existing debt and may incur additional indebtedness. Our primary recurrent sources of liquidity are cash from operations and cash from borrowings, which are subject to general, economic, financial, competitive, regulatory and other factors that are beyond our control, as described in Item 1A1A. Risk Factors under the
heading "The level of our current and future debt could have an adverse impact on our business, and our ability to generate cash to service our indebtedness and for other intended purposes and our ability to maintain compliance with debt covenants depends on many factors beyond our control.debt..."
Reconciliations of non-GAAP measures
The following tables provide reconciliations of adjusted operating income (loss) to operating income (loss) as presented on a U.S. generally accepted accounting principles (GAAP) basis for our U.S. dialysis reportable segment as well as for our U.S. IKC business, our U.S. other ancillary services, our international business, and for our total ancillary services which combines them and is disclosed as our other segments category.category, in addition to our corporate administrative support. These non-GAAP or “adjusted”"adjusted" measures are presented because management believes these measures are useful adjuncts to, but not alternatives for, our GAAP results.
Specifically, management uses adjusted operating income (loss) to compare and evaluate our performance period over period and relative to competitors, to analyze the underlying trends in our business, to establish operational budgets and forecasts and for incentive compensation purposes. We believe this non-GAAP measure is also useful to investors and analysts in evaluating our performance over time and relative to competitors, as well as in analyzing the underlying trends in our business. We also believe this presentation enhances a user's understanding of our normal operating income by excluding certain items which we do not believe are indicative of our ordinary results of operations.
In addition, our effective income tax rate on income from continuing operations attributable to DaVita Inc. excludes noncontrolling owners' income, which primarily relates to non-tax paying entities. We believe this adjusted effective income tax rate is useful to management, investors and analysts in evaluating our performance and establishing expectations for income taxes incurred on our ordinary results attributable to DaVita Inc.
Finally, our free cash flow from continuing operations represents net cash provided by operating activities from continuing operations less distributions to noncontrolling interests and all capital expenditures (including development capital expenditures, routine maintenance and information technology), plus contributions from noncontrolling interests and proceeds from the sale of self-developed properties. Management uses this measure to assess our ability to fund acquisitions and meet our debt service obligations and we believe this measure is equally useful to investors and analysts as an adjunct to cash flows from operating activities from continuing operations and other measures under GAAP.
It is important to bear in mind that these non-GAAP “adjusted”"adjusted" measures are not measures of financial performance under GAAP and should not be considered in isolation from, nor as substitutes for, their most comparable GAAP measures.
| | Year ended December 31, 2020 |
| U.S.
dialysis | | Ancillary services | | Corporate
administration | |
| U.S. | | International | | Total | | Consolidated |
| (dollars in millions) |
| Year ended December 31, 2023 | | | Year ended December 31, 2023 |
| U.S.
dialysis | |
| | U.S. IKC | |
| | U.S. IKC | |
| | U.S. IKC | | | U.S. Other | | International | | Total | | | Consolidated |
| (dollars in millions) | | | (dollars in millions) |
| Operating income (loss) | Operating income (loss) | $ | 1,918 | | | $ | (99) | | | $ | 23 | | | $ | (76) | | | $ | (147) | | | $ | 1,695 | |
| | Loss on changes in ownership interests, net | | 16 | | | 16 | | | 16 | |
| Accruals for legal matters | | 35 | | | 35 | |
| Center closure charges | |
| Severance and other costs | |
| Legal matter | |
| IKC adjustment | |
| Earn-out revaluation | |
| Goodwill impairment | |
| Adjusted operating income (loss) | Adjusted operating income (loss) | $ | 1,918 | | | $ | (83) | | | $ | 23 | | | $ | (60) | | | $ | (112) | | | $ | 1,746 | |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
| | Year ended December 31, 2022 | | | Year ended December 31, 2022 |
| U.S.
dialysis | |
| | U.S. IKC | |
| | U.S. IKC | |
| | U.S. IKC | | | U.S. Other | | International | | Total | | | Consolidated |
| (dollars in millions) | | | (dollars in millions) |
| Operating income (loss) | |
| Center closure charges | |
| | | Year ended December 31, 2019 |
| Severance and other costs | |
| | U.S.
dialysis | | Ancillary services | | Corporate
administration | |
| Severance and other costs | |
| | U.S.
dialysis | | U.S. | | International | | Total | | Corporate
administration | | Consolidated |
| (dollars in millions) |
| Operating income (loss) | $ | 1,925 | | | $ | (66) | | | $ | (123) | | | $ | (189) | | | $ | (92) | | | $ | 1,643 | |
| | Goodwill impairment | | 125 | | | 125 | | | 125 | |
| | Severance and other costs | |
| | Adjusted operating income (loss) | Adjusted operating income (loss) | $ | 1,925 | | | $ | (66) | | | $ | 2 | | | $ | (64) | | | $ | (92) | | | $ | 1,768 | |
| | Adjusted operating income (loss) | |
| | Adjusted operating income (loss) | |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
| | | | | | | | | | | |
| Year ended December 31, |
| 2023 | | 2022 |
| (dollars in millions) |
| Income from continuing operations before income taxes | $ | 1,177 | | | $ | 966 | |
| Less: Noncontrolling owners’ income primarily attributable to non-tax paying entities | (263) | | | (222) | |
| Income from continuing operations before income taxes attributable to DaVita Inc. | $ | 914 | | | $ | 744 | |
| | | |
| Income tax expense for continuing operations | $ | 220 | | | $ | 198 | |
| Income tax attributable to noncontrolling interests | 2 | | | (1) | |
| Income tax expense from continuing operations attributable to DaVita Inc. | $ | 222 | | | $ | 197 | |
| | | |
| Effective income tax rate on income from continuing operations attributable to DaVita Inc. | 24.3 | % | | 26.5 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
| | | | | | | | | | | |
| Year ended December 31, |
| 2020 | | 2019 |
| (dollars in millions) |
| Income from continuing operations before income taxes | $ | 1,318 | | | $ | 1,195 | |
| Less: Noncontrolling owners’ income primarily attributable to non-tax paying entities | (222) | | | (210) | |
| Income from continuing operations before income taxes attributable to DaVita Inc. | $ | 1,097 | | | $ | 986 | |
| | | |
| Income tax expense for continuing operations | $ | 314 | | | $ | 280 | |
| Less: Income tax attributable to noncontrolling interests | (1) | | | (1) | |
| Income tax expense from continuing operations attributable to DaVita Inc. | $ | 313 | | | $ | 279 | |
| | | |
| Effective income tax rate on income from continuing operations attributable to DaVita Inc. | 28.6 | % | | 28.3 | % |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
| | | | | | | | | | | |
| Year ended December 31, |
| 2020 | | 2019 |
| (dollars in millions) |
| Net cash provided by continuing operating activities | $ | 1,979 | | | $ | 1,973 | |
| Less: Distributions to noncontrolling interests | (253) | | | (233) | |
| Plus: Contributions from noncontrolling interests | 43 | | | 57 | |
| Cash provided by continuing operating activities attributable to DaVita Inc. | 1,769 | | | 1,797 | |
| Less: Expenditures for routine maintenance and information technology | (399) | | | (355) | |
| Less: Expenditures for development | (275) | | | (373) | |
| Plus: Proceeds from sale of self-developed properties | 93 | | | 58 | |
| Free cash flow from continuing operations | $ | 1,188 | | | $ | 1,127 | |
| | | | | | | | | | | |
| Year ended December 31, |
| 2023 | | 2022 |
| (dollars in millions) |
| Net cash provided by operating activities | $ | 2,059 | | | $ | 1,565 | |
Adjustments to reconcile net cash provided by continuing operating
activities to free cash flow from continuing operations: | | | |
| Distributions to noncontrolling interests | (281) | | | (268) | |
| Contributions from noncontrolling interests | 15 | | | 15 | |
| Expenditures for routine maintenance and information technology | (406) | | | (431) | |
| Expenditures for developments and relocations | (162) | | | (172) | |
| Proceeds from sale of self-developed properties | 11 | | | 109 | |
| Free cash flow | $ | 1,236 | | | $ | 817 | |
Certain columns or rows may not sum or recalculate due to the presentation of rounded numbers.
Off-balance sheet arrangements and aggregate contractual obligations
In addition to the debt obligations and operating lease liabilities reflected on our balance sheet, we have commitments associated with letters of credit as well as certain working capital funding obligations associated with our equity investments in nonconsolidated dialysis ventures that we manage and some we manage that are wholly-owned by third parties.
We also have potential obligations to purchase the noncontrolling interests held by third parties in many of our majority-owned dialysis partnerships and other nonconsolidated entities. These obligations are in the form of put provisions that are exercisable at the third-party owners’ discretion within specified periods as outlined in each specific put provision. For additional information see Note 1716 to the consolidated financial statements.
The following is a summary of these cash contractual obligations and commitments as of December 31, 2020:2023:
| | | | 2021 | | 2022-2023 | | 2024-2025 | | Thereafter | | Total | | 2024 | | 2025-2026 | | 2027-2028 | | Thereafter | | Total |
| (dollars in millions) |
| Scheduled payments under contractual obligations: | | | | | | | | | |
| (dollars in millions) | | | (dollars in millions) |
| Debt and leases: | | Debt and leases: | | | |
Long-term debt(1): | Long-term debt(1): | |
| Principal payments | |
| Principal payments | |
| Principal payments | Principal payments | $ | 147 | | | $ | 349 | | | $ | 1,512 | | | $ | 5,882 | | | $ | 7,890 | |
| Interest payments on credit facilities and senior notes | Interest payments on credit facilities and senior notes | 219 | | | 429 | | | 389 | | | 704 | | | 1,741 | |
Financing leases(2) | Financing leases(2) | 22 | | | 48 | | | 54 | | | 150 | | | 274 | |
Operating leases, including imputed interest(2) | Operating leases, including imputed interest(2) | 480 | | | 969 | | | 774 | | | 1,438 | | | 3,661 | |
| | | $ | 868 | | | $ | 1,795 | | | $ | 2,729 | | | $ | 8,174 | | | $ | 13,566 | |
| Potential cash requirements under other commitments: | | | | | | | | | |
| Letters of credit | $ | 65 | | | $ | — | | | $ | — | | | $ | — | | | $ | 65 | |
Partnership interests subject to put provisions:(3) | | Partnership interests subject to put provisions:(3) | | | |
| On-balance sheet: | |
| Noncontrolling interests subject to put provisions | Noncontrolling interests subject to put provisions | 1,023 | | | 145 | | | 97 | | | 65 | | | 1,330 | |
| Noncontrolling interests subject to put provisions | |
| Noncontrolling interests subject to put provisions | |
| Off-balance sheet: | |
| Non-owned and minority owned put provisions | Non-owned and minority owned put provisions | 110 | | | 6 | | | — | | | — | | | 116 | |
| Operating capital advances | 1 | | | 2 | | | 2 | | | 4 | | | 9 | |
| Purchase commitments | 542 | | | 721 | | | 92 | | | — | | | 1,355 | |
| Non-owned and minority owned put provisions | |
| Non-owned and minority owned put provisions | |
| | | $ | 1,741 | | | $ | 874 | | | $ | 191 | | | $ | 69 | | | $ | 2,875 | |
(1)See Note 1312 to the consolidated financial statements for components of our long-term debt and related interest rates.
(2)See Note 1413 to the consolidated financial statements for components of our leases and related interest rates.
In 2017,(3)Represents amounts for which we entered into a Sourcing and Supply Agreement with Amgen USA Inc. (Amgen) that expires onare contractually committed, should the outside partner exercise its put option.
As of December 31, 2022. Under2023 we had outstanding letters of credit in the terms of the agreement, the Company will purchase EPO from Amgen in amounts necessary to meet no less than 90% of its requirements for erythropoiesis-stimulating agents (ESAs) through the expiration of the contract. The actualaggregate amount of EPO thatapproximately $151 million under a separate bilateral secured letter of credit facility.
As of December 31, 2023 we willhave outstanding purchase will depend upon the amount of EPO administered during dialysis as prescribed by physicians and the overall number of patients that we serve.
The purchase commitments in the table above represent our agreements with various suppliers to purchase set amounts of dialysis equipment, parts, pharmaceuticals, and supplies. If we fail to meet the minimum purchase commitments under these contracts during any year, it iswe are required to pay the difference to the supplier. For additional information see Note 16 to the consolidated financial statements.
We also have certain potential commitments to provide working capital funding, if necessary, to certain nonconsolidated dialysis businesses that we manage and in which we own a noncontrolling equity interest or which are wholly-owned by third parties. For additional information see Note 16 to the consolidated financial statements.
Additionally, we expect our 2024 capital expenditures to be consistent with our 2023 capital expenditures.
In addition, we have approximately $88$45 million of existing long-term income tax liabilities for unrecognized tax benefits, including interest and penalties, and other long-term tax liabilities,which are excluded from the table above as reasonably reliable estimates of their timing cannot be made.
Finally, on May 25, 2022, we entered into an agreement with Medtronic, Inc. and one of its subsidiaries (collectively, Medtronic) to form a new, independent kidney care-focused medical device company (Mozarc). The transaction closed on April 1, 2023. As a part of this transaction we agreed to pay Medtronic additional consideration of up to $300 million if certain regulatory and commercial milestones are achieved between 2024 and 2028. As of December 31, 2023 we have contingent consideration of $86 million recorded for this obligation which represents its estimated fair value.
Contingencies
The information in Note 1615 to the consolidated financial statements included in this report is incorporated by reference in response to this item.
Critical accounting policies, estimates and judgments
Our consolidated financial statements and accompanying notes are prepared in accordance with United States generally accepted accounting principles. These accounting principles require us to make estimates, judgments and assumptions that affect the reported amounts of revenues, expenses, assets, liabilities, contingencies and noncontrolling interests subject to put provisions (redeemable equity interests). All significant estimates, judgments and assumptions are developed based on the best information available to us at the time made and are regularly reviewed and updated when necessary. Actual results will generally differ from these estimates, and such differences may be material. Changes in estimates are reflected in our financial statements in the period of change based upon on-going actual experience trends or subsequent settlements and realizations depending on the nature and predictability of the estimates and contingencies. Certain accounting estimates, including those concerning revenue recognition and accounts receivable, impairments offair value estimates for goodwill and noncontrolling interests, accounting for income taxes, fair value estimates, and loss contingencies are considered to be critical to evaluating and understanding our financial results because they involve inherently uncertain matters and their application requires the most difficult and complex judgments and estimates. For additional information, see Part IIIV Item 15, "Exhibits, Financial Statement Schedules" – Note 1 – "Organization and summary of significant accounting policies" as referred from Part II Item 8, "Financial Statements and Supplementary Data."
U.S. dialysis revenueRevenue recognition and accounts receivable for our U.S. dialysis patient services. There are significant estimating risks associated with the amount of U.S. dialysis patient service revenue that we recognize in a given reporting period. Payment rates are often subject to significant uncertainties related to wide variations in the coverage terms of the commercial healthcare plans under which we receive payments. In addition, ongoing insurance coverage changes, geographic coverage differences, differing interpretations of contract coverage, and other payor issues complicate the billing and collection process. NetThe measurement and recognition of revenue recognition and allowances for uncollectible billings requirerequires the use of estimates of the amounts that will ultimately be realized considering, among other items, retroactive adjustments that may be associated with regulatory reviews, audits, billing reviews and other matters.
Revenues associated with Medicare and Medicaid programs are recognized based on (a) the payment rates that are established by statute or regulation for the portion of the payment rates paid by the government payor (e.g., 80% for Medicare patients) and (b) for the portion not paid by the primary government payor, the estimated amounts that will ultimately be collectible from other government programs providing secondary coverage (e.g., Medicaid secondary coverage), the patient’s commercial health plan secondary coverage, or the patient. Our dialysis relateddialysis-related reimbursements from Medicare are subject to certain variations under Medicare’s single bundled payment rate system whereby our reimbursements can be adjusted for certain patient characteristics and other variable factors. Our revenue recognition depends upon our ability to effectively capture, document and bill for Medicare’s base payment rate and these other factors. In addition, as a result of the potential range of variations that can occur in our dialysis-related reimbursements from Medicare under the single bundled payment rate system, our revenue recognition is subject to a greater degree of estimating risk.
Commercial healthcare plans, including contracted managed-care payors, are billed at our usual and customary rates; however, revenue is recognized based on estimated net realizable revenue for the services provided. Net realizable revenue is estimated based on contractual terms for the patients covered under commercial healthcare plans with which we have formal agreements, non-contracted commercial healthcare plan coverage terms if known, estimated secondary collections, historical
collection experience, historical trends of refunds and payor payment adjustments (retractions), inefficiencies in our billing and collection processes that can result in denied claims for payments, the estimated timing of collections, changes in our expectations of the amounts that we expect to collect and regulatory compliance matters. Determining applicable primary and secondary coverage for our approximately 204,200200,800 U.S. dialysis patients at any given point in time, together with the changes in patient coverages that occur each month, requires complex, resource-intensive processes. Collections, refunds and payor retractions typically continue to occur for up to three years or longer after services are provided.
We generally expect the range of our U.S. dialysis revenue estimating risk to be within 1% of revenue, which can represent as much as approximately 5%6% of our U.S. dialysis business’s adjusted operating income. Changes in estimates are reflected in the then-current financial statements based on on-going actual experience trends, or subsequent settlements and realizations depending on the nature and predictability of the estimates and contingencies. Changes in revenue estimates for prior periods are separately disclosed and reported if material to the current reporting period and longer term trend analyses, and have not been significant.
Revenues for laboratory services, which are integrally related to our dialysis services, are recognized in the period services are provided at the estimated net realizable amounts to be received.
ImpairmentsCertain fair value estimates. Fair value measurements and estimates affect, or potentially affect, a variety of goodwill. We account for impairmentselements in the Company's financial statements. Two of the elements most significantly impacted by fair value estimates are the Company's goodwill in accordance with theimpairment assessments and remeasurements of its noncontrolling interests subject to put provisions of applicable accounting guidance. balance.
Goodwill is not amortized, but is assessed for impairment at least annually, or when changes in circumstances warrant and at least annually.warrant. An impairment charge is recorded when and to the extent a reporting unit's carrying amount is determined to exceed its estimated fair value.
Changes in circumstance that may trigger a goodwill impairment assessment for one of our business units can include, among others, changes in the legal environment, addressable market, business strategy, development or business plans, reimbursement structure or rates, operating performance, future prospects, relationships with partners, interest rates and/or market value indications for the subject business. We use a variety of factors to assess changes in the financial condition, future prospects and other circumstances concerning thefor businesses subject businesses and to estimate their fair value when applicable. Any change in the factors, assessments or assumptions involved could affect a determination of whether and when to assess goodwill for impairment as well as the outcome of such an assessment. TheseHowever, these assessments and the related valuations can involve significant uncertainties and require significant judgment on various matters, some of which could bematters.
The Company is also required to remeasure its noncontrolling interests subject to reasonable disagreement.put provisions to estimated fair value each reporting period. These estimates also require substantive judgment on meaningful uncertainties concerning this significant balance. See Notes 16 and 23 to the consolidated financial statements for a summary of the Company's approach to these valuations, the variables and uncertainties involved, and the sensitivity of these valuations to changes in a primary aggregate valuation metric.
Accounting for income taxes. Our income tax expense, deferred tax assets and liabilities, and liabilities for unrecognized tax benefits reflect management’s best assessment of estimated current and future taxes to be paid. We are subject to income taxes in the United States and numerous state and foreign jurisdictions, and changes in tax laws or regulations may be proposed or enacted that could adversely affect our overall tax liability. The actual impact of any such laws or regulations could be materially different from our current estimates.
Significant judgments and estimates are required in determining our consolidated income tax expense. Deferred income taxes arise from temporary differences between the tax basis of assets and liabilities and their reported amounts in the financial statements, which will result in taxable or deductible amounts in the future. In evaluating our ability to recover our deferred tax assets within the jurisdictions from which they arise, we consider all available positive and negative evidence, including scheduled reversals of deferred tax liabilities, projected future taxable income, tax planning strategies, results of recent operations, and assumptions about the amount of future federal, state, and foreign pre-tax operating income adjusted for items that do not have tax consequences. The assumptions about future taxable income require significant judgments and are consistent with the plans and estimates we use to manage the underlying businesses. To the extent that recovery is not likely, a valuation allowance is established. The allowance is regularly reviewed and updated for changes in circumstances that would cause a change in judgment about the realizability of the related deferred tax assets.
Fair value estimates. The FASB defines fair value generally as the amount at which an asset (or liability) could be bought (or assumed) or sold (or settled) in a current transaction between willing parties, that is, other than in a forced or liquidation sale. It also defines fair value more specifically for most purposes as the price that would be received to sell an asset or paid to transfer a liability in an orderly transaction between market participants at the measurement date.
We rely on fair value measurements and estimates for purposes that require the recording, reassessment, or adjustment of the carrying amounts of certain assets, liabilities and noncontrolling interests subject to put provisions (redeemable equity interests). These purposes can include purchase accounting for business combination transactions; impairment assessments for goodwill, other intangible assets, and other long-lived assets; recurrent revaluation of investments in debt and equity securities, contingent earn-out obligations, interest rate cap agreements, and noncontrolling interests subject to put provisions; and the accounting for equity method and other investments and stock-based compensation, among others. The criticality of a particular fair value estimate to our consolidated financial statements depends upon the nature and size of the item being measured, the extent of uncertainties involved and the nature and magnitude or potential effect of assumptions and judgments required. Critical fair value estimates can involve significant uncertainties and require significant judgment on various matters, some of which could be subject to reasonable disagreement.
Loss contingencies. As discussed in Notes 1 and 1615 to the consolidated financial statements, we operate in a highly regulated industry and are party to various lawsuits, claims, qui tam suits, governmental investigations and audits (including, without limitation, investigations or other actions resulting from itsour obligation to self-report suspected violations of law), contract disputes and other legal proceedings. Assessments of such matters can involve a series of complex judgments about future events and can rely heavily on estimates and assumptions. We record accruals for loss contingencies on such matters to the extent that we determine an unfavorable outcome is probable and the amount of the loss can be reasonably estimated. See Note 1615 to the consolidated financial statements included in this report for further discussion.
Significant new accounting standards
See Note 1 to the consolidated financial statements included in this report for information regarding certain recent financial accounting standards that have been issued by the FASB.Financial Accounting Standards Board (FASB).
Item 7A. Quantitative and Qualitative Disclosures about Market Risk.Risk
Interest rate sensitivity
The tables below provide information about our financial instruments that are sensitive to changes in interest rates. The first table below presents scheduled principal repayments and current weighted average interest rates on our debt obligations as of December 31, 2020.2023. The variable rates presented reflect the weighted average LIBORSOFR rates in effect for all debt tranches plus the interest rate margins in effect as of December 31, 2020. The2023. At December 31, 2023, the Term Loan AA-1 interest rate margin in effect at December 31, 2020, was 1.50%. At December 31, 2020,1.75% and the Term Loan B-1 interest rate margin in effect was also 1.75%. At December 31, 2020, we had an outstanding balance on our revolving line of credit bearing interest at an Alternate Base Rate (the Prime Rate) plus 0.50%. On January 6, 2021 our revolving line of credit rate was converted to a LIBOR-based rate of LIBOR plus 1.50%. The interest rates in effect on our Term Loan AA-1 and new revolving line of credit are subject to adjustment depending upon changes in our leverage ratio.
| | | | | Expected maturity date | | | | Average
interest
rate | | Estimated fair value(1) |
| | | | Expected maturity date | | Average
interest
rate | | Fair value(1) |
| | | 2021 | | 2022 | | 2023 | | 2024 | | 2025 | | Thereafter | | Total | |
| | | (dollars in millions) | (dollars in millions) |
| Long term debt: | Long term debt: | | | | | | | | | | | | | | | | | | Long term debt: | | | |
| Fixed rate | Fixed rate | $ | 31 | | | $ | 34 | | | $ | 48 | | | $ | 29 | | | $ | 33 | | | $ | 3,448 | | | $ | 3,623 | | | 4.32 | % | | $ | 3,481 | |
| Variable rate | Variable rate | $ | 138 | | | $ | 136 | | | $ | 179 | | | $ | 1,468 | | | $ | 36 | | | $ | 2,584 | | | $ | 4,541 | | | 2.05 | % | | $ | 4,518 | |
(1)Represents the estimated fair value of our long-term debt excluding financing leases.
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | Notional amount | | Contract maturity date | | Receive variable | | Fair value |
| | | 2021 | | 2022 | | 2023 | | 2024 | | 2025 | | |
| | (dollars in millions) |
| 2019 cap agreements | $ | 3,500 | | | $ | — | | | $ | — | | | $ | — | | | $ | 3,500 | | | $ | — | | | LIBOR above 2.0% | | $ | 2.7 | |
However, principal amounts of $2,604 million for Term Loan B-1 and $896 million of Term Loan A-1 (the capped debt) are effectively hedged by our 2019 interest rate cap agreements through June 30, 2024, with additional caps from our 2023 interest rate cap agreements extending for further periods. As of December 31, 2023, applicable SOFR rates were above the 2.00% threshold of our cap agreements making the interest rates on this capped debt “economically fixed", unless or until applicable SOFR rates were to fall back below 2.00% during the remaining term of the caps. As a result, as of December 31, 2023, total fixed and economically fixed debt was $8,078 million, with an average interest rate of 4.28%, while total variable rate debt not subject to caps was $368 million with an average interest rate of 7.51%.
For a further discussion of our debt and interest rate cap agreements, see Note 1312 to our consolidated financial statements at Part IIIV Item 15, "Exhibits, Financial Statement Schedules" – Note 13 – "Long-term debt12" as referred from Part II Item 8, "Financial Statements and Supplementary Data."
We believe that our cash flowflows from operations and other sources of liquidity, including from amounts available under our current credit facilities and our access to the capital markets, will be sufficient to fund our scheduled debt service under the terms of our debt agreements and other obligations for the foreseeable future, including the next 12 months. Our primary recurrent sources of liquidity are cash from operations and cash from borrowings.
One means of assessing exposure to debt-related interest rate changes is a duration-based analysis that measures the potential loss in net income resulting from a hypothetical increase in interest rates of 100 basis points across all variable rate maturities (referred to as a parallel shift in the yield curve). Under this model, with all else held constant, it is estimated that such an increase would have reduced net income by approximately $34.8$4.8 million, $32.4$21.4 million, and $37.8$33.8 million, net of tax and the effect of our interest rate caps, for the years ended December 31, 2020, 2019,2023, 2022, and 2018,2021, respectively.
Exchange rate sensitivity
While our business is predominantly conducted in the U.S., we have developing operations in ten11 other countries as well. For financial reporting purposes, the U.S. dollar is our reporting currency. However, the functional currencies of our operating businesses in other countries are typically those of the countries in which they operate. Therefore, changes in the rate of exchange between the U.S. dollar and the local currencies in which our international operations are conducted affect our results of operations and financial position as reported in our consolidated financial statements.
We have consolidated the balance sheets of our non-U.S. dollar denominated operations into U.S. dollars at the exchange rates prevailing at the balance sheet dates and have translated their revenues and expenseexpenses at average exchange rates during each period. Additionally, our individual subsidiaries are exposed to transactional risks mainly resulting from intercompany transactions between and among subsidiaries with different functional currencies. This exposes the subsidiaries to fluctuations in the rate of exchange between the invoicing or obligation currencies and the currency in which their local operations are conducted.
We evaluate our exposure to foreign exchange risk through the judgment of our international and corporate management teams. Through 2020,2023, our international operations have remained fairly small relative to the size of our consolidated financial statements, constitutingconstitute approximately 9%12% of our consolidated assets as of December 31, 2020, with no single country constituting more than 3% of consolidated assets, and approximately 5%6% of our consolidated revenues for the year ended December 31, 2020.2023, with no single country constituting more than 5% of consolidated assets. In addition, our unrealized foreign currency translation gains (losses) gains were approximately (0.4)%5.5%, (1)%2.2%, and (3)%4.7% of our consolidated operating income for the years ended December 31, 2020, 20192023, 2022 and 2018.2021, respectively.
Given the relatively small size of our international operations, management does not consider our exposure to foreign exchange risk to be significant to the consolidated enterprise. As such, through December 31, 2020,2023, we have not engaged in transactions to hedge the exposure of our international transactions or net investments to foreign currency risk.
Item 8. Financial Statements and Supplementary Data.Data
See the Index to Financial Statements and Index to Financial Statement Schedules included at Part IV Item 15, "Exhibits, Financial Statement Schedules.”"
Item 9. Changes in and Disagreements with Accountants on Accounting and Financial Disclosure.Disclosure
None.
Item 9A. Controls and Procedures.Procedures
Management has established and maintains disclosure controls and procedures designed to ensure that information required to be disclosed in the reports that it files or submits pursuant to the Securities Exchange Act of 1934 (Exchange Act) as amended is recorded, processed, summarized and reported within the time periods specified in the SEC’s rules and forms, and that such information is accumulated and communicated to our management including our Chief Executive Officer ("CEO")(CEO) and Chief Financial Officer ("CFO")(CFO) as appropriate to allow for timely decisions regarding required disclosures.
At the end of the period covered by this report, we carried out an evaluation, under the supervision and with the participation of our CEO and CFO, of the effectiveness of the design and operation of the Company's disclosure controls and procedures in accordance with the Exchange Act requirements as of December 31, 2020.2023. Based upon that evaluation, the CEO and CFO concluded that the Company's disclosure controls and procedures were effective as required by the Exchange Act as of such date for our Exchange Act reports, including this report. Management recognizes that these controls and procedures can provide only reasonable assurance of desired outcomes, and that estimates and judgments are still inherent in the process of maintaining effective controls and procedures.
There was no change in the Company's internal control over financial reporting that was identified during the evaluation that occurred during the fourth fiscal quarter of 20202023 that has materially affected, or is reasonably likely to materially affect, the Company's internal control over financial reporting.
Item 9B. Other Information.Information
None.None of our directors or executive officers adopted or terminated a Rule 10b5-1 trading arrangement or adopted or terminated a non-Rule 10b5-1 trading arrangement (as defined in Item 408(c) of Regulation S-K) during the quarter ended December 31, 2023.
Item 9C. Disclosure Regarding Foreign Jurisdictions that Prevent Inspections
Not applicable.
PART III
Item 10. Directors, Executive Officers and Corporate Governance.Governance
We intend to disclose any amendments or waivers to the Code of Ethics applicable to our principal executive officer, principal financial officer, principal accounting officer or controller or persons performing similar functions, on our website located at http://www.davita.com. In 2002, we adopted a Corporate Governance Code of Ethics that applies to our principal executive officer, principal financial officer, principal accounting officer or controller, and to all of our financial accounting and legal professionals who are directly or indirectly involved in the preparation, reporting and fair presentation of our financial statements and Exchange Act reports. The Code of Ethics is posted on our website, located at http://www.davita.com. We also maintain a Corporate Code of Conduct that applies to all of our employees, officers and directors, which is posted on our website.
Under our Corporate Governance Guidelines all Board Committees including the Audit Committee, Nominating and Governance Committee and the Compensation Committee, which are comprisedcomposed solely of independent directors as defined within the listing standards of the New York Stock Exchange, have written charters that outline the committee’s purpose, goals, membership requirements and responsibilities. These charters are regularly reviewed and updated as necessary by our Board of Directors. All Board Committee charters as well as the Corporate Governance Guidelines are posted on our website located at http://www.davita.com.
The other information required to be disclosed by this item will appear in, and is incorporated by reference from, the sections entitled “"Proposal 1 Election of DirectorsDirectors"”, “"Corporate GovernanceGovernance"”, and “"Security Ownership of Certain Beneficial Owners and ManagementManagement"” to be included in our definitive proxy statement relating to our 20212024 annual stockholder meeting.
Item 11. Executive Compensation.Compensation
The information required by this item will appear in, and is incorporated by reference from, the sections entitled "Executive Compensation", "Pay Ratio Disclosure", "Compensation of Directors" and "Compensation Committee Interlocks and Insider Participation" included in our definitive proxy statement relating to our 20212024 annual stockholder meeting. The information required by Item 407(e)(5) of Regulation S-K will appear in and is incorporated by reference from the section entitled “"Compensation Committee ReportReport"” to be included in our definitive proxy statement relating to our 20212024 annual stockholder meeting; however, this information shall not be deemed to be filed.
Item 12. Security Ownership of Certain Beneficial Owners and Management and Related Stockholder Matters.Matters
The following table provides information about our common stock that may be issued upon the exercise of stock-settled stock appreciation rights, restricted stock units, performance stock units and other rights under all of our existing equity compensation plans as of December 31, 2020,2023, which consist of our DaVita Inc. 2020 Incentive Award Plan, DaVita Healthcare Partners Inc. 2011 Incentive Award Plan and our DaVita Inc. Employee Stock Purchase Plan. The material terms of these plans are described in Note 1817 to the consolidated financial statements.
| | Plan category (shares in thousands) | Plan category (shares in thousands) | | Number of shares to be issued upon exercise of outstanding options, warrants and rights(1) | | Weighted average exercise price of outstanding options, warrants and rights(2) | | Number of shares remaining
available for future issuance under equity
compensation plans (excluding securities reflected in
column (a)) | | Total of shares reflected in columns (a) and (c) | Plan category (shares in thousands) | | Number of shares to be issued upon exercise of outstanding options, warrants and rights(1) | | Weighted average exercise price of outstanding options, warrants and rights(2) | | Number of shares remaining
available for future issuance under equity
compensation plans (excluding securities reflected in
column (a)) | | Total of shares reflected in columns (a) and (c) |
| | | | (a) | | (b) | | (c) | | (d) | | | (a) | | (b) | | (c) | | (d) |
| Equity compensation plans approved by shareholders | Equity compensation plans approved by shareholders | | 12,167 | | | $ | 63.64 | | | 14,263 | | | 26,430 | |
Equity compensation plans not requiring shareholder
approval | Equity compensation plans not requiring shareholder
approval | | — | | | — | | | — | | | — | |
| Total | Total | | 12,167 | | | $ | 63.64 | | | 14,263 | | | 26,430 | |
1.(1) Includes 1,092588 shares of common stock reserved for issuance in connection with performance share units at the maximum number of shares issuable thereunder.
2.(2) This weighted average excludes full value awards such as restricted stock units and performance share units.
Other information required to be disclosed by Item 12 will appear in, and is incorporated by reference from, the section entitled “"Security Ownership of Certain Beneficial Owners and ManagementManagement"” to be included in our definitive proxy statement relating to our 20212024 annual stockholder meeting.
Item 13. Certain Relationships and Related Transactions, and Director Independence.Independence
The information required by this item will appear in, and is incorporated by reference from, the section entitled “"Certain Relationships and Related TransactionsTransactions"” and the section entitled “"Corporate GovernanceGovernance"” to be included in our definitive proxy statement relating to our 20212024 annual stockholder meeting.
Item 14. Principal Accounting Fees and Services.Services
The information required by this item will appear in, and is incorporated by reference from, the section entitled “"Proposal 2 Ratification of the Appointment of our Independent Registered Public Accounting FirmFirm"” to be included in our definitive proxy statement relating to our 20212024 annual stockholder meeting. Our independent registered public accounting firm is KPMG LLP, Seattle, WA, USA PCAOB ID: 185.
PART IV
Item 15. Exhibits, Financial Statement Schedules.Schedules
(a) Documents filed as part of this Report:
(1) Index to Financial Statements: (2) Index to Financial Statement Schedules: (3) Exhibits
The information required by this Item is set forth in the Exhibit Index that precedes the signature pages of this Annual Report on Form 10-K.
Item 16. Form 10-K Summary.Summary
None.
DAVITA INC.
MANAGEMENT’S REPORT ON INTERNAL CONTROL OVER FINANCIAL REPORTING
Management is responsible for establishing and maintaining an adequate system of internal control over financial reporting designed to provide reasonable assurance regarding the reliability of financial reporting and the preparation of financial statements for external purposes in accordance with U.S. generally accepted accounting principles and which includes those policies and procedures that (i) pertain to the maintenance of records that, in reasonable detail, accurately and fairly reflect the transactions and dispositions of the assets of the Company; (ii) provide reasonable assurance that transactions are recorded as necessary to permit preparation of financial statements in accordance with U.S. generally accepted accounting principles, and that receipts and expenditures of the Company are being made only in accordance with authorizations of management and directors of the Company; and (iii) provide reasonable assurance regarding prevention or timely detection of unauthorized acquisition, use, or disposition of the Company’s assets that could have a material effect on the financial statements.
During the last fiscal year, the Company conducted an evaluation, under the oversight of the Chief Executive Officer and Chief Financial Officer, of the effectiveness of the design and operation of the Company’s internal control over financial reporting. This evaluation was completed based on the criteria established in the report titled “"Internal Control—Integrated Framework (2013)"” issued by the Committee of Sponsoring Organizations of the Treadway Commission (COSO).
Based upon our evaluation under the COSO framework, we have concluded that the Company’s internal control over financial reporting was effective as of December 31, 2020.2023.
The Company’s independent registered public accounting firm, KPMG LLP, has issued an attestation report on the Company’s internal control over financial reporting, which report is included in this Annual Report.
Report of Independent Registered Public Accounting Firm
To the Stockholders and Board of Directors
DaVita Inc.:
Opinion on the ConsolidatedFinancial Statements
We have audited the accompanying consolidated balance sheets of DaVita Inc. and subsidiaries (the Company) as of December 31, 20202023 and 2019,2022, the related consolidated statements of income, comprehensive income, equity, and cash flowflows for each of the years in the three-year period ended December 31, 2020,2023, and the related notes and financial statement Schedule II – Valuation and Qualifying Accounts (collectively, the consolidated financial statements). In our opinion, the consolidated financial statements present fairly, in all material respects, the financial position of the Company as of December 31, 20202023 and 2019,2022, and the results of its operations and its cash flows for each of the years in the three-year period ended December 31, 2020,2023, in conformity with U.S. generally accepted accounting principles.
We also have audited, in accordance with the standards of the Public Company Accounting Oversight Board (United States) (PCAOB), the Company’s internal control over financial reporting as of December 31, 2020,2023, based on criteria established in Internal Control – Integrated Framework (2013) issued by the Committee of Sponsoring Organizations of the Treadway Commission, and our report dated February 12, 202114, 2024 expressed an unqualified opinion on the effectiveness of the Company’s internal control over financial reporting.
Change in Accounting Principle
As discussed in Note 14 to the consolidated financial statements, the Company has changed its method of accounting for leases as of January 1, 2019 due to the adoption of the Financial Accounting Standards Board’s Accounting Standards Codification Topic 842 Leases.
Basis for Opinion
These consolidated financial statements are the responsibility of the Company’s management. Our responsibility is to express an opinion on these consolidated financial statements based on our audits. We are a public accounting firm registered with the PCAOB and are required to be independent with respect to the Company in accordance with the U.S. federal securities laws and the applicable rules and regulations of the Securities and Exchange Commission and the PCAOB.
We conducted our audits in accordance with the standards of the PCAOB. Those standards require that we plan and perform the audit to obtain reasonable assurance about whether the consolidated financial statements are free of material misstatement, whether due to error or fraud. Our audits included performing procedures to assess the risks of material misstatement of the consolidated financial statements, whether due to error or fraud, and performing procedures that respond to those risks. Such procedures included examining, on a test basis, evidence regarding the amounts and disclosures in the consolidated financial statements. Our audits also included evaluating the accounting principles used and significant estimates made by management, as well as evaluating the overall presentation of the consolidated financial statements. We believe that our audits provide a reasonable basis for our opinion.
Critical Audit Matters
The critical audit matters communicated below are matters arising from the current period audit of the consolidated financial statements that were communicated or required to be communicated to the audit committee and that: (1) relate to accounts or disclosures that are material to the consolidated financial statements and (2) involved our especially challenging, subjective, or complex judgments. The communication of critical audit matters does not alter in any way our opinion on the consolidated financial statements, taken as a whole, and we are not, by communicating the critical audit matters below, providing separate opinions on the critical audit matters or on the accounts or disclosures to which they relate.
U.S. dialysis patient service revenue recognition
As discussed in Notes 1 and 2 to the consolidated financial statements, the Company recognized $10,619$10,912 million in U.S. dialysis patient service revenue for the year ended December 31, 2020.2023. There are uncertainties associated with estimating U.S. dialysis patient service revenue, which generally take several years to resolve. As these estimates are refined over time, both positive and negative adjustments are recognized in the current period.
We identified the evaluation of the recognition of the transaction price the Company expects to collect as a result of satisfying its performance obligations related to U.S. dialysis patient service revenue as a critical audit matter because it involves estimation that requires complex auditor judgment. The key assumptions and inputs used to estimate the transaction price relate to ongoing insurance coverage changes, differing interpretations of contract coverage, determination of applicable primary and secondary coverage, coordination of benefits, and varying patient characteristics impacting Medicare reimbursements. Changes to the key assumptions and inputs used in the application of the methodology may have a significant effect on the Company’s determination of the estimate.
The following are the primary procedures we performed to address this critical audit matter. We evaluated the design and tested the operating effectiveness of certain internal controls over the Company’s U.S. dialysis patient service revenue recognition process, including controls related to the application of the methodology used to estimate the transaction price, and the key assumptions and inputs. We evaluated the Company’s key assumptions and inputs to estimate the transaction price the Company expects to collect as a result of satisfying its performance obligationsobligation by comparing key assumptions to historical collection experience, trends of refunds and payor payment adjustments, delays in the Company’s billing and collection process and regulatory compliance matters. Additionally, we compared U.S. dialysis patient service revenue related to the transaction price estimates recognized in prior periods to actual cash collections related to performance obligations satisfied in prior periods to analyze the Company’s ability to estimate the transaction price the Company expects to collect as a result of satisfying its performance obligations. We developed an estimate of U.S. dialysis patient service revenue based on actual and expected cash collections and compared to U.S. dialysis patient service revenue recorded by the Company for the year-endedyear ended December 31, 2020.
Evaluation of the goodwill impairment analyses for the Germany kidney care reporting unit
As discussed in Note 10 to the consolidated financial statements, the Company performed annual and other impairment assessments for their reporting units throughout 2020. As a result of these assessments, the Company has not recognized any goodwill impairment charges in the current year. The goodwill balance for the Germany kidney care reporting unit as of December 31, 2020 was $323 million.
We have identified the evaluation of the goodwill impairment analyses for the Germany kidney care reporting unit as a critical audit matter. The evaluations involved assessing the key assumptions used in estimating the fair value of the reporting unit, including non-acquired patient growth rate, projected number of treatments, projected revenue growth rate, discount rates, and revenue and clinical earnings before interest, taxes, depreciation, and amortization (EBITDA) multiples. Evaluation of these key assumptions involved a high degree of subjectivity and auditor judgment as changes to these assumptions could have a significant impact on any goodwill impairment charges recognized.
The following are the primary procedures we performed to address this critical audit matter. We evaluated the design and tested the operating effectiveness of certain internal controls over the Company’s goodwill impairment assessment process, including controls over the development of key assumptions as described above. We assessed the Company’s ability to forecast by comparing prior year actual results of the reporting unit to previously forecasted amounts for the reporting unit. We evaluated the Company’s non-acquired patient growth rate, projected number of treatments, and projected revenue growth rate, for the reporting unit by comparing the projections to the Company’s underlying business strategies and operating plans for the reporting unit, and other industry and market data. In addition, we involved valuation professionals with specialized skills and knowledge, who assisted in:
•evaluating the projected revenue growth rate for the reporting unit by comparing projected rates with comparable companies
•evaluating the discount rate for the reporting unit, by comparing the inputs used to develop the discount rate to publicly available market data for comparable companies to assess whether the inputs used in the development of the discount rate are reasonable
•evaluating the revenue and clinical EBITDA multiples utilized in the Company’s valuation of the reporting unit by comparing the multiples selected to a range of multiples from comparable transactions.2023.
Evaluation of legal proceedings and regulatory matters
As discussed in Notes 1 and 16Note 15 to the consolidated financial statements, the Company operates in a highly regulated industry and is a party to various lawsuits, demands, claims, qui tam suits, governmental investigations and audits (including, without limitation, investigations or other actions resulting from its obligation to self-report suspected violationsviolation of law) and other legal proceedings. The Company records accruals for certain legal proceedings and regulatory matters to the extent an unfavorable outcome is probable, and the amount of the loss can be reasonably estimated.
We identified the evaluation of legal proceedings and regulatory matters as a critical audit matter. Due to the nature of the legal proceedings and regulatory matters, a high degree of subjectivity was required in evaluating the completeness of the Company’s population of legal proceedings and regulatory matters. Additionally, complex auditor judgment was required in evaluating the Company’s probability of outcome assessment, and related disclosures.
The following are the primary procedures we performed to address this critical audit matter. We evaluated the design and tested the operating effectiveness of certain internal controls over the Company’s legal proceedings and regulatory matters process. This includes controls over the Company’s determination of the completeness of the population of legal proceedings and regulatory matters, as well as controls over the Company’s probability of outcome assessment, and related disclosures. We tested existing legal proceedings and regulatory matters by reading certain written correspondence received from outside parties as well as reading certain written responses provided to outside parties. We read letters received directly from the Company’s external and internal legal counsel that described certain legal proceedings and regulatory matters. We involved forensic professionals with specialized skills and knowledge who inspected the Company’s compliance case log. Additionally, we assessed the completeness of the population of legal proceedings and regulatory matters and related disclosures by 1) inquiring of certain key executives and directors and 2) evaluating information received through procedures described above and through publicly available information about the Company, its competitors, and the industry.
/s/ KPMG LLP
We have served as the Company’s auditor since 2000.
Seattle, Washington
February 12, 202114, 2024
Report of Independent Registered Public Accounting Firm
To the Stockholders and the Board of Directors
DaVita Inc.:
Opinion on Internal Control Over Financial Reporting
We have audited DaVita Inc. andsubsidiaries’ subsidiaries' (the Company) internal control over financial reporting as of December 31, 2020,2023, based on criteria established in Internal Control – Integrated Framework (2013) issued by the Committee of Sponsoring Organizations of the Treadway Commission. In our opinion, the Company maintained, in all material respects, effective internal control over financial reporting as of December 31, 2020,2023, based on criteria established in Internal Control – Integrated Framework (2013) issued by the Committee of Sponsoring Organizations of the Treadway Commission.
We also have audited, in accordance with the standards of the Public Company Accounting Oversight Board (United States) (PCAOB), the consolidated balance sheets of the Company as of December 31, 20202023 and 2019,2022, the related consolidated statements of income, comprehensive income, equity, and cash flowflows for each of the years in the three-year period ended December 31, 2020,2023, and the related notes andfinancial statementScheduleII – Valuation and Qualifying Accounts(collectively,(collectively, the consolidated financial statements), and our report dated February 12, 202114, 2024 expressed an unqualified opinion on those consolidated financial statements.
Basis for Opinion
The Company’s management is responsible for maintaining effective internal control over financial reporting and for its assessment of the effectiveness of internal control over financial reporting, included in the accompanying Management’sManagement's Report on Internal Control Over Financial Reporting. Our responsibility is to express an opinion on the Company’s internal control over financial reporting based on our audit. We are a public accounting firm registered with the PCAOB and are required to be independent with respect to the Company in accordance with the U.S. federal securities laws and the applicable rules and regulations of the Securities and Exchange Commission and the PCAOB.
We conducted our audit in accordance with the standards of the PCAOB. Those standards require that we plan and perform the audit to obtain reasonable assurance about whether effective internal control over financial reporting was maintained in all material respects. Our audit of internal control over financial reporting included obtaining an understanding of internal control over financial reporting, assessing the risk that a material weakness exists, and testing and evaluating the design and operating effectiveness of internal control based on the assessed risk. Our audit also included performing such other procedures as we considered necessary in the circumstances. We believe that our audit provides a reasonable basis for our opinion.
Definition and Limitations of Internal Control Over Financial Reporting
A company’s internal control over financial reporting is a process designed to provide reasonable assurance regarding the reliability of financial reporting and the preparation of financial statements for external purposes in accordance with generally accepted accounting principles. A company’s internal control over financial reporting includes those policies and procedures that (1) pertain to the maintenance of records that, in reasonable detail, accurately and fairly reflect the transactions and dispositions of the assets of the company; (2) provide reasonable assurance that transactions are recorded as necessary to permit preparation of financial statements in accordance with generally accepted accounting principles, and that receipts and expenditures of the company are being made only in accordance with authorizations of management and directors of the company; and (3) provide reasonable assurance regarding prevention or timely detection of unauthorized acquisition, use, or disposition of the company’s assets that could have a material effect on the financial statements.
Because of its inherent limitations, internal control over financial reporting may not prevent or detect misstatements. Also, projections of any evaluation of effectiveness to future periods are subject to the risk that controls may become inadequate because of changes in conditions, or that the degree of compliance with the policies or procedures may deteriorate.
/s/ KPMG LLP
Seattle, Washington
February 12, 202114, 2024
DAVITA INC.
CONSOLIDATED STATEMENTS OF INCOME
(dollars and shares in thousands, except per share data)
| | | | Year ended December 31, | | Year ended December 31, |
| | | 2020 | | 2019 | | 2018 | | 2023 | | 2022 | | 2021 |
| Dialysis patient service revenues before provision | $ | 11,039,709 | | | $ | 10,918,421 | | | $ | 10,709,981 | |
| Provision for uncollectible accounts | (13,458) | | | (21,715) | | | (49,587) | |
| | Dialysis patient service revenues | |
| | Dialysis patient service revenues | |
| | Dialysis patient service revenues | Dialysis patient service revenues | 11,026,251 | | | 10,896,706 | | | 10,660,394 | |
| Other revenues | Other revenues | 524,353 | | | 491,773 | | | 744,457 | |
| Total revenues | Total revenues | 11,550,604 | | | 11,388,479 | | | 11,404,851 | |
| Operating expenses and charges: | | | | | |
| Operating expenses: | |
| Patient care costs | |
| Patient care costs | |
| Patient care costs | Patient care costs | 7,988,613 | | | 7,914,485 | | | 8,195,513 | |
| General and administrative | General and administrative | 1,247,584 | | | 1,103,312 | | | 1,135,454 | |
| Depreciation and amortization | Depreciation and amortization | 630,435 | | | 615,152 | | | 591,035 | |
| Provision for uncollectible accounts | 0 | | | 0 | | | (7,300) | |
| Equity investment (income) loss | (26,916) | | | (12,679) | | | 4,484 | |
| Other asset impairments | 0 | | | 0 | | | 17,338 | |
| | Equity investment income, net | |
| Equity investment income, net | |
| Equity investment income, net | |
| | Goodwill impairment charges | Goodwill impairment charges | 0 | | | 124,892 | | | 3,106 | |
| Loss (gain) on changes in ownership interest, net | 16,252 | | | 0 | | | (60,603) | |
| Goodwill impairment charges | |
| Goodwill impairment charges | |
| | Total operating expenses and charges | 9,855,968 | | | 9,745,162 | | | 9,879,027 | |
| | Total operating expenses | |
| | Total operating expenses | |
| | Total operating expenses | |
| Operating income | Operating income | 1,694,636 | | | 1,643,317 | | | 1,525,824 | |
| Debt expense | Debt expense | (304,111) | | | (443,824) | | | (487,435) | |
| Debt prepayment, refinancing and redemption charges | (89,022) | | | (33,402) | | | 0 | |
| Other income, net | 16,759 | | | 29,348 | | | 10,089 | |
| Debt extinguishment and modification costs | |
| Other (loss) income, net | |
| Income from continuing operations before income taxes | Income from continuing operations before income taxes | 1,318,262 | | | 1,195,439 | | | 1,048,478 | |
| Income tax expense | Income tax expense | 313,932 | | | 279,628 | | | 258,400 | |
| Net income from continuing operations | Net income from continuing operations | 1,004,330 | | | 915,811 | | | 790,078 | |
| Net (loss) income from discontinued operations, net of tax | (9,653) | | | 105,483 | | | (457,038) | |
| Net income from discontinued operations, net of tax | |
| Net income | Net income | 994,677 | | | 1,021,294 | | | 333,040 | |
| Less: Net income attributable to noncontrolling interests | Less: Net income attributable to noncontrolling interests | (221,035) | | | (210,313) | | | (173,646) | |
| Net income attributable to DaVita Inc. | Net income attributable to DaVita Inc. | $ | 773,642 | | | $ | 810,981 | | | $ | 159,394 | |
| | Earnings per share attributable to DaVita Inc.: | Earnings per share attributable to DaVita Inc.: | | | | |
| Earnings per share attributable to DaVita Inc.: | |
| Earnings per share attributable to DaVita Inc.: | |
| Basic net income from continuing operations | |
| Basic net income from continuing operations | |
| Basic net income from continuing operations | Basic net income from continuing operations | $ | 6.54 | | | $ | 4.61 | | | $ | 3.66 | |
| Basic net income | Basic net income | $ | 6.46 | | | $ | 5.29 | | | $ | 0.93 | |
| Diluted net income from continuing operations | Diluted net income from continuing operations | $ | 6.39 | | | $ | 4.60 | | | $ | 3.62 | |
| Diluted net income | Diluted net income | $ | 6.31 | | | $ | 5.27 | | | $ | 0.92 | |
| | Weighted average shares for earnings per share: | Weighted average shares for earnings per share: | | | | |
| Weighted average shares for earnings per share: | |
| Weighted average shares for earnings per share: | |
| Basic shares | |
| Basic shares | |
| Basic shares | Basic shares | 119,797 | | | 153,181 | | | 170,786 | |
| Diluted shares | Diluted shares | 122,623 | | | 153,812 | | | 172,365 | |
| | Amounts attributable to DaVita Inc.: | Amounts attributable to DaVita Inc.: | |
| Amounts attributable to DaVita Inc.: | |
| Amounts attributable to DaVita Inc.: | |
| Net income from continuing operations | Net income from continuing operations | $ | 783,295 | | | $ | 706,832 | | | $ | 624,321 | |
| Net (loss) income from discontinued operations | (9,653) | | | 104,149 | | | (464,927) | |
| Net income from continuing operations | |
| Net income from continuing operations | |
| Net income from discontinued operations | |
| Net income attributable to DaVita Inc. | Net income attributable to DaVita Inc. | $ | 773,642 | | | $ | 810,981 | | | $ | 159,394 | |
See notes to consolidated financial statements.
DAVITA INC.
CONSOLIDATED STATEMENTS OF COMPREHENSIVE INCOME
(dollars in thousands)
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 |
| Net income | $ | 994,677 | | | $ | 1,021,294 | | | $ | 333,040 | |
| Other comprehensive (loss) income, net of tax: | | | | | |
| Unrealized (losses) gains on interest rate cap agreements: | | | | | |
| Unrealized (losses) gains | (16,346) | | | 1,151 | | | (133) | |
| Reclassification into net income | 5,313 | | | 6,377 | | | 6,286 | |
| Unrealized losses on foreign currency translation | (7,623) | | | (20,102) | | | (45,944) | |
| Other comprehensive loss | (18,656) | | | (12,574) | | | (39,791) | |
| Total comprehensive income | 976,021 | | | 1,008,720 | | | 293,249 | |
| Less: Comprehensive income attributable to noncontrolling interests | (221,035) | | | (210,313) | | | (173,646) | |
| Comprehensive income attributable to DaVita Inc. | $ | 754,986 | | | $ | 798,407 | | | $ | 119,603 | |
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2023 | | 2022 | | 2021 |
| Net income | $ | 956,978 | | | $ | 781,643 | | | $ | 1,211,762 | |
| Other comprehensive income, net of tax: | | | | | |
| Unrealized gains on interest rate cap agreements: | | | | | |
| Unrealized gains | 6,895 | | | 108,669 | | | 7,155 | |
| Reclassification of net realized (gains) losses into net income | (77,727) | | | (8,806) | | | 4,133 | |
| Unrealized gains (losses) on foreign currency translation | 87,934 | | | (29,802) | | | (84,381) | |
| Other comprehensive income (loss) | 17,102 | | | 70,061 | | | (73,093) | |
| Total comprehensive income | 974,080 | | | 851,704 | | | 1,138,669 | |
| Less: Comprehensive income attributable to noncontrolling interests | (265,443) | | | (221,243) | | | (233,312) | |
| Comprehensive income attributable to DaVita Inc. | $ | 708,637 | | | $ | 630,461 | | | $ | 905,357 | |
See notes to consolidated financial statements.
DAVITA INC.
CONSOLIDATED BALANCE SHEETS
(dollars and shares in thousands, except per share data)
| | | | December 31, 2020 | | December 31, 2019 | | December 31, 2023 | | December 31, 2022 |
| ASSETS | ASSETS | | | | ASSETS | | | |
| Cash and cash equivalents | Cash and cash equivalents | $ | 324,958 | | | $ | 1,102,372 | |
| Restricted cash and equivalents | Restricted cash and equivalents | 176,832 | | | 106,346 | |
| Short-term investments | Short-term investments | 20,101 | | | 11,572 | |
| Accounts receivable | Accounts receivable | 1,824,282 | | | 1,795,598 | |
| Inventories | Inventories | 111,625 | | | 97,949 | |
| Other receivables | Other receivables | 544,376 | | | 489,695 | |
| Prepaid and other current assets | Prepaid and other current assets | 76,387 | | | 66,866 | |
| Income tax receivable | Income tax receivable | 70,163 | | | 19,772 | |
| Total current assets | Total current assets | 3,148,724 | | | 3,690,170 | |
| Property and equipment, net of accumulated depreciation | Property and equipment, net of accumulated depreciation | 3,521,824 | | | 3,473,384 | |
| Operating lease right-of-use assets | Operating lease right-of-use assets | 2,863,089 | | | 2,830,047 | |
| Intangible assets, net of accumulated amortization | Intangible assets, net of accumulated amortization | 166,585 | | | 135,684 | |
| Equity method and other investments | Equity method and other investments | 257,491 | | | 241,983 | |
| Long-term investments | Long-term investments | 32,193 | | | 36,519 | |
| Other long-term assets | Other long-term assets | 79,501 | | | 115,972 | |
| Goodwill | Goodwill | 6,919,109 | | | 6,787,635 | |
| | | $ | 16,988,516 | | | $ | 17,311,394 | |
| LIABILITIES AND EQUITY | LIABILITIES AND EQUITY | | | | LIABILITIES AND EQUITY | | | |
| Accounts payable | Accounts payable | $ | 434,253 | | | $ | 403,840 | |
| Other liabilities | Other liabilities | 810,529 | | | 756,174 | |
| Accrued compensation and benefits | Accrued compensation and benefits | 685,555 | | | 695,052 | |
| Current portion of operating lease liabilities | Current portion of operating lease liabilities | 369,497 | | | 343,912 | |
| Current portion of long-term debt | Current portion of long-term debt | 168,541 | | | 130,708 | |
| Income tax payable | Income tax payable | 7,768 | | | 42,412 | |
| Total current liabilities | Total current liabilities | 2,476,143 | | | 2,372,098 | |
| Long-term operating lease liabilities | Long-term operating lease liabilities | 2,738,670 | | | 2,723,800 | |
| Long-term debt | Long-term debt | 7,917,263 | | | 7,977,526 | |
| Other long-term liabilities | Other long-term liabilities | 150,060 | | | 160,809 | |
| Deferred income taxes | Deferred income taxes | 809,600 | | | 577,543 | |
| Total liabilities | Total liabilities | 14,091,736 | | | 13,811,776 | |
| Commitments and contingencies | Commitments and contingencies | |
| Noncontrolling interests subject to put provisions | Noncontrolling interests subject to put provisions | 1,330,028 | | | 1,180,376 | |
| Noncontrolling interests subject to put provisions | |
| Noncontrolling interests subject to put provisions | |
| Equity: | Equity: | | | | Equity: | | | |
| Preferred stock ($0.001 par value, 5,000 shares authorized; none issued) | Preferred stock ($0.001 par value, 5,000 shares authorized; none issued) | 0 | | | 0 | |
Common stock ($0.001 par value, 450,000 shares authorized; 109,933 and
125,843 shares issued and outstanding at December 31, 2020 and 2019, respectively) | 110 | | | 126 | |
Common stock ($0.001 par value, 450,000 shares authorized; 88,824 and 90,411 shares issued and outstanding at December 31, 2023, and 2022, respectively) | |
| Additional paid-in capital | Additional paid-in capital | 597,073 | | | 749,043 | |
| Retained earnings | Retained earnings | 852,537 | | | 1,431,738 | |
| Accumulated other comprehensive loss | Accumulated other comprehensive loss | (66,154) | | | (47,498) | |
| Total DaVita Inc. shareholders' equity | Total DaVita Inc. shareholders' equity | 1,383,566 | | | 2,133,409 | |
| Noncontrolling interests not subject to put provisions | Noncontrolling interests not subject to put provisions | 183,186 | | | 185,833 | |
| Total equity | Total equity | 1,566,752 | | | 2,319,242 | |
| | | $ | 16,988,516 | | | $ | 17,311,394 | |
See notes to consolidated financial statements.
DAVITA INC.
CONSOLIDATED STATEMENTS OF CASH FLOWFLOWS
(dollars in thousands)
| | | | Year ended December 31, | | Year ended December 31, |
| | | 2020 | | 2019 | | 2018 | | 2023 | | 2022 | | 2021 |
| Cash flows from operating activities: | Cash flows from operating activities: | | | | | | Cash flows from operating activities: | | | | | |
| Net income | Net income | $ | 994,677 | | | $ | 1,021,294 | | | $ | 333,040 | |
| Adjustments to reconcile net income to net cash provided by operating activities: | Adjustments to reconcile net income to net cash provided by operating activities: | | | Adjustments to reconcile net income to net cash provided by operating activities: | | | | | |
| Depreciation and amortization | Depreciation and amortization | 630,435 | | | 615,152 | | | 591,035 | |
| Impairment charges | Impairment charges | 0 | | | 124,892 | | | 61,981 | |
| Valuation adjustment on disposal group | 0 | | | 0 | | | 316,840 | |
| Debt prepayment, refinancing and redemption charges | 86,957 | | | 33,402 | | | 0 | |
| Loss on extinguishment of debt | |
| Stock-based compensation expense | Stock-based compensation expense | 91,458 | | | 67,850 | | | 73,061 | |
| Deferred income taxes | Deferred income taxes | 240,848 | | | 41,723 | | | 273,660 | |
| Equity investment income, net | 13,830 | | | 8,582 | | | 26,449 | |
| Loss (gain) on sales of business interests, net | 24,248 | | | 23,022 | | | (85,699) | |
| Equity investment loss, net | |
| | Other non-cash charges, net | |
| Other non-cash charges, net | |
| Other non-cash charges, net | Other non-cash charges, net | 747 | | | 49,579 | | | 82,374 | |
| Changes in operating assets and liabilities, net of effect of acquisitions and divestitures: | Changes in operating assets and liabilities, net of effect of acquisitions and divestitures: | |
| Accounts receivable | Accounts receivable | (21,087) | | | (79,957) | | | (81,176) | |
| Accounts receivable | |
| Accounts receivable | |
| Inventories | Inventories | (12,349) | | | 10,158 | | | 73,505 | |
| Other receivables and other current assets | (79,277) | | | 2,790 | | | 236,995 | |
| Other current assets | |
| Other long-term assets | Other long-term assets | (6,123) | | | 6,965 | | | 3,497 | |
| Accounts payable | Accounts payable | 37,200 | | | (84,539) | | | (35,959) | |
| Accrued compensation and benefits | Accrued compensation and benefits | (20,931) | | | (14,697) | | | 84,165 | |
| Other current liabilities | Other current liabilities | 105,637 | | | 181,940 | | | (157,462) | |
| Income taxes | Income taxes | (87,391) | | | 95,645 | | | (23,635) | |
| Other long-term liabilities | Other long-term liabilities | (19,851) | | | (31,446) | | | (1,031) | |
| Net cash provided by operating activities | Net cash provided by operating activities | 1,979,028 | | | 2,072,355 | | | 1,771,640 | |
| Cash flows from investing activities: | Cash flows from investing activities: | | | | | | Cash flows from investing activities: | | | | | |
| Additions of property and equipment | Additions of property and equipment | (674,541) | | | (766,546) | | | (987,138) | |
| Acquisitions | Acquisitions | (182,013) | | | (100,861) | | | (183,156) | |
| Proceeds from asset and business sales | Proceeds from asset and business sales | 50,139 | | | 3,877,392 | | | 150,205 | |
| Purchase of debt investments held-to-maturity | Purchase of debt investments held-to-maturity | (150,701) | | | (101,462) | | | (5,963) | |
| Purchase of other debt and equity investments | Purchase of other debt and equity investments | (3,757) | | | (5,458) | | | (8,448) | |
| Proceeds from debt investments held-to-maturity | Proceeds from debt investments held-to-maturity | 151,213 | | | 95,376 | | | 34,862 | |
| Proceeds from sale of other debt and equity investments | Proceeds from sale of other debt and equity investments | 3,491 | | | 3,676 | | | 9,526 | |
| Purchase of equity method investments | Purchase of equity method investments | (22,341) | | | (9,366) | | | (19,177) | |
| Distributions from equity method investments | Distributions from equity method investments | 3,139 | | | 2,589 | | | 3,646 | |
| Net cash (used in) provided by investing activities | (825,371) | | | 2,995,340 | | | (1,005,643) | |
| Other | |
| Net cash used in investing activities | |
| Cash flows from financing activities: | Cash flows from financing activities: | | | | | |
| Borrowings | Borrowings | 4,046,775 | | | 38,525,850 | | | 59,934,750 | |
| Borrowings | |
| Borrowings | |
| Payments on long-term debt | Payments on long-term debt | (4,110,304) | | | (40,520,722) | | | (59,234,946) | |
| Deferred financing and debt redemption costs | (105,848) | | | (85,319) | | | (5,027) | |
| Deferred and debt related financing costs | |
| Purchase of treasury stock | Purchase of treasury stock | (1,458,442) | | | (2,383,816) | | | (1,161,511) | |
| Distributions to noncontrolling interests | Distributions to noncontrolling interests | (253,118) | | | (233,123) | | | (196,441) | |
| Net (payments) receipts related to stock purchases and awards | (975) | | | 11,382 | | | 13,577 | |
| Net payments related to stock purchases and awards | |
| Contributions from noncontrolling interests | Contributions from noncontrolling interests | 42,966 | | | 57,317 | | | 52,311 | |
| Proceeds from sales of additional noncontrolling interest | 0 | | | 0 | | | 15 | |
| Proceeds from sales of additional noncontrolling interests | |
| Purchases of noncontrolling interests | Purchases of noncontrolling interests | (7,831) | | | (68,019) | | | (28,082) | |
| Net cash used in financing activities | Net cash used in financing activities | (1,846,777) | | | (4,696,450) | | | (625,354) | |
| Effect of exchange rate changes on cash, cash equivalents and restricted cash | Effect of exchange rate changes on cash, cash equivalents and restricted cash | (13,808) | | | (1,760) | | | (3,350) | |
| Net (decrease) increase in cash, cash equivalents and restricted cash | (706,928) | | | 369,485 | | | 137,293 | |
| Less: Net (decrease) increase in cash, cash equivalents and restricted cash from discontinued operations | 0 | | | (423,813) | | | 240,793 | |
| Net (decrease) increase in cash, cash equivalents and restricted cash from continuing operations | (706,928) | | | 793,298 | | | (103,500) | |
| Cash, cash equivalents and restricted cash of continuing operations at beginning of the year | 1,208,718 | | | 415,420 | | | 518,920 | |
| Cash, cash equivalents and restricted cash of continuing operations at end of the year | $ | 501,790 | | | $ | 1,208,718 | | | $ | 415,420 | |
| Net increase (decrease) in cash, cash equivalents and restricted cash | |
| | Cash, cash equivalents and restricted cash at beginning of the year | |
| | Cash, cash equivalents and restricted cash at beginning of the year | |
| | Cash, cash equivalents and restricted cash at beginning of the year | |
| Cash, cash equivalents and restricted cash at end of the year | |
See notes to consolidated financial statements.
DAVITA INC.
CONSOLIDATED STATEMENTS OF EQUITY
(dollars and shares in thousands)
| | Non-controlling
interests
subject to put
provisions | | | Non-controlling
interests
subject to put
provisions | | DaVita Inc. Shareholders' Equity | | Non-controlling interests not
subject to
put provisions |
| | | | Additional
paid-in
capital | |
| | Common stock | |
| | Common stock | |
| | Common stock | |
| | Shares | |
| | Shares | |
| | Shares | |
| Balance at December 31, 2020 | |
| Balance at December 31, 2020 | |
| Balance at December 31, 2020 | |
| | Non-controlling
interests
subject to put
provisions | | DaVita Inc. Shareholders' Equity | | Non-controlling interests not
subject to
put provisions |
| | | Additional
paid-in
capital | | Retained
earnings | | | | Accumulated
other
comprehensive
income (loss) | | |
| Common stock | | Treasury stock | |
| Shares | | Amount | | Shares | | Amount | | Total | |
| Balance at December 31, 2017 | $ | 1,011,360 | | | 182,462 | | | $ | 182 | | | $ | 1,042,899 | | | $ | 3,633,713 | | | 0 | | | $ | 0 | | | $ | 13,235 | | | $ | 4,690,029 | | | $ | 196,037 | |
Cumulative effect of change
in accounting principle | | 8,368 | | | (8,368) | | | 0 | | |
| Comprehensive income: | |
| Comprehensive income: | |
| Comprehensive income: | Comprehensive income: | | | | | | | | | | | | | | | | | | | |
| Net income | Net income | 105,531 | | | 159,394 | | | 159,394 | | | 68,115 | |
| Other comprehensive income | | | (39,791) | | | (39,791) | | |
| Net income | |
| Net income | |
| Other comprehensive loss | |
| Stock purchase plan | |
| Stock purchase plan | |
| Stock purchase plan | Stock purchase plan | | 398 | | | 0 | | | 17,398 | | | 17,398 | | |
| Stock award plan | Stock award plan | | 371 | | | 1 | | (5,335) | | | (5,334) | | |
| Stock award plan | |
| Stock award plan | |
Stock-settled stock-based
compensation expense | |
Stock-settled stock-based
compensation expense | |
Stock-settled stock-based
compensation expense | Stock-settled stock-based
compensation expense | | 73,081 | | | 73,081 | | |
Changes in noncontrolling
interest from: | Changes in noncontrolling
interest from: | |
Changes in noncontrolling
interest from: | |
Changes in noncontrolling
interest from: | |
| Distributions | |
| Distributions | |
| Distributions | Distributions | (119,173) | | | (77,268) | |
| Contributions | Contributions | 32,918 | | | 19,393 | |
| Acquisitions and divestitures | Acquisitions and divestitures | 79,078 | | | 3,546 | | | 3,546 | | | 318 | |
| Partial purchases | Partial purchases | (8,546) | | | (17,897) | | | (17,897) | | | (1,639) | |
| Fair value remeasurements | Fair value remeasurements | 23,473 | | | (23,473) | | | (23,473) | | | | Fair value remeasurements | 75,717 | | | | | | | (75,717) | | | | | | (75,717) | | | | | | | | | | | (75,717) | | | | | | | | | | (75,717) | | | | | |
| Purchase of treasury stock | Purchase of treasury stock | | (16,844) | | | (1,153,511) | | | (1,153,511) | | |
| Retirement of treasury stock | Retirement of treasury stock | | (16,844) | | | (17) | | | (95,213) | | | (1,058,281) | | | 16,844 | | | 1,153,511 | | | 0 | | |
| Balance at December 31, 2018 | $ | 1,124,641 | | | 166,387 | | | $ | 166 | | | $ | 995,006 | | | $ | 2,743,194 | | | 0 | | | $ | 0 | | | $ | (34,924) | | | $ | 3,703,442 | | | $ | 204,956 | |
Cumulative effect of change
in accounting principle | (38) | | | 39,876 | | | 0 | | 39,876 | | | (6) | |
| Retirement of treasury stock | |
| Retirement of treasury stock | |
Deferred taxes from
partnership buyouts | |
Deferred taxes from
partnership buyouts | |
Deferred taxes from
partnership buyouts | |
| Balance at December 31, 2021 | |
| Balance at December 31, 2021 | |
| Balance at December 31, 2021 | |
| | Comprehensive income: | Comprehensive income: | | |
| Comprehensive income: | |
| Comprehensive income: | |
| Net income | |
| Net income | |
| Net income | Net income | 143,413 | | | 810,981 | | | 810,981 | | | 66,900 | |
| Other comprehensive income | Other comprehensive income | | (12,574) | | | (12,574) | | |
| Stock purchase plan | Stock purchase plan | | 315 | | | 1 | | | 16,569 | | | 16,570 | | |
| Stock award plan | | 161 | | | 0 | | | (3,290) | | | (3,290) | | |
| Stock purchase plan | |
| Stock purchase plan | |
| Stock award plans | |
| Stock award plans | |
| Stock award plans | |
Stock-settled stock-based
compensation expense | |
Stock-settled stock-based
compensation expense | |
Stock-settled stock-based
compensation expense | Stock-settled stock-based
compensation expense | | 67,549 | | | 67,549 | | |
Changes in noncontrolling
interest from: | Changes in noncontrolling
interest from: | |
Changes in noncontrolling
interest from: | |
Changes in noncontrolling
interest from: | |
| Distributions | |
| Distributions | |
| Distributions | Distributions | (155,011) | | | (78,112) | |
| Contributions | Contributions | 35,572 | | | 21,745 | |
| Acquisitions and divestitures | Acquisitions and divestitures | (6,332) | | | (10,170) | |
| Partial purchases | Partial purchases | (11,394) | | | (37,145) | | | (37,145) | | | (19,480) | |
| Fair value remeasurements | Fair value remeasurements | 49,525 | | | (49,525) | | | (49,525) | | |
| Other | |
| Other | |
| Other | |
| Purchase of treasury stock | Purchase of treasury stock | | (41,020) | | | (2,402,475) | | | (2,402,475) | | |
| Retirement of treasury stock | Retirement of treasury stock | | (41,020) | | | (41) | | | (240,121) | | | (2,162,313) | | | 41,020 | | | 2,402,475 | | | 0 | | |
| Balance at December 31, 2019 | $ | 1,180,376 | | | 125,843 | | | $ | 126 | | | $ | 749,043 | | | $ | 1,431,738 | | | 0 | | | $ | 0 | | | $ | (47,498) | | | $ | 2,133,409 | | | $ | 185,833 | |
| Retirement of treasury stock | |
| Retirement of treasury stock | |
| Balance at December 31, 2022 | |
| Balance at December 31, 2022 | |
| Balance at December 31, 2022 | |
DAVITA INC.
CONSOLIDATED STATEMENTS OF EQUITY - continued
(dollars and shares in thousands)
| | | | Non-controlling
interests
subject to put
provisions | | DaVita Inc. Shareholders' Equity | | Non-controlling interests not
subject to
put provisions | | Non-controlling
interests
subject to put
provisions | | DaVita Inc. Shareholders' Equity | | Non-controlling interests not
subject to
put provisions |
| | | Additional
paid-in
capital | | Retained
earnings | | | | Accumulated
other
comprehensive
income (loss) | | | |
| Common stock | | Treasury stock | |
| Shares | | Amount | | Shares | | Amount | | Total | |
| Balance at December 31, 2019 | $ | 1,180,376 | | | 125,843 | | | $ | 126 | | | $ | 749,043 | | | $ | 1,431,738 | | | 0 | | | $ | 0 | | | $ | (47,498) | | | $ | 2,133,409 | | | $ | 185,833 | |
| Common stock | |
| Shares | |
| Shares | |
| Shares | |
| Balance at December 31, 2022 | |
| Balance at December 31, 2022 | |
| Balance at December 31, 2022 | |
| Comprehensive income: | Comprehensive income: | | |
| Net income | |
| Net income | |
| Net income | Net income | 141,879 | | | 773,642 | | | 773,642 | | | 79,156 | |
| Other comprehensive income | Other comprehensive income | | (18,656) | | | (18,656) | | |
| Stock purchase plan | Stock purchase plan | | 222 | | | 0 | | | 17,148 | | | 17,148 | | |
| Stock purchase plan | |
| Stock purchase plan | |
| Stock award plans | |
| Stock award plans | |
| Stock award plans | Stock award plans | | 345 | | | 0 | | | (17,801) | | | (17,801) | | |
Stock-settled stock-based
compensation expense | Stock-settled stock-based
compensation expense | | 90,007 | | | 90,007 | | |
Stock-settled stock-based
compensation expense | |
Stock-settled stock-based
compensation expense | |
Changes in noncontrolling
interest from: | Changes in noncontrolling
interest from: | |
Changes in noncontrolling
interest from: | |
Changes in noncontrolling
interest from: | |
| Distributions | |
| Distributions | |
| Distributions | Distributions | (163,175) | | | (89,943) | |
| Contributions | Contributions | 30,154 | | | 12,812 | |
| Acquisitions and divestitures | Acquisitions and divestitures | (3,215) | | | (248) | |
| Partial purchases | Partial purchases | (7,771) | | | 4,364 | | | 4,364 | | | (4,424) | |
| Fair value remeasurements | Fair value remeasurements | 151,780 | | | (151,780) | | | (151,780) | | |
| | Purchase of treasury stock | |
| | Purchase of treasury stock | |
| | Purchase of treasury stock | Purchase of treasury stock | | (16,477) | | | (1,446,767) | | | (1,446,767) | | |
| Retirement of treasury stock | Retirement of treasury stock | | (16,477) | | | (16) | | | (93,908) | | | (1,352,843) | | | 16,477 | | | 1,446,767 | | | 0 | | |
| Balance at December 31, 2020 | $ | 1,330,028 | | | 109,933 | | | $ | 110 | | | $ | 597,073 | | | $ | 852,537 | | | 0 | | | $ | 0 | | | $ | (66,154) | | | $ | 1,383,566 | | | $ | 183,186 | |
| Retirement of treasury stock | |
| Retirement of treasury stock | |
| | Balance at December 31, 2023 | |
| | Balance at December 31, 2023 | |
| | Balance at December 31, 2023 | |
See notes to consolidated financial statements.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
(dollars in thousands, except per share data)
1. Organization and summary of significant accounting policies
Organization
The Company's operations are comprisedcomposed of its dialysis and related lab services to patients in the United States (its U.S. dialysis business), its U.S. integrated kidney care (IKC) business, its U.S. other ancillary services and strategic initiatives including its international operations (collectively, its ancillary services), andas well as its corporate administrative support.
The Company’s largest line of business is its U.S. dialysis business, which operates kidney dialysis centers in the U.S. for patients suffering from chronic kidney failure, also known as end stage renal disease (ESRD)or end stage kidney disease (ESRD or ESKD). As of December 31, 2020,2023, the Company operated or provided administrative services through a network of 2,8162,675 U.S. outpatient dialysis centers in 46 states and the District of Columbia, serving a total of approximately 204,200200,800 patients. In addition, as of December 31, 2020,2023, the Company operated or provided administrative services to a total of 321367 outpatient dialysis centers serving approximately 36,20049,400 patients located in 1011 countries outside of the U.S.
On June 19, 2019, the Company completed the sale of its DaVita Medical Group (DMG) business to Collaborative Care Holdings, LLC (Optum), a subsidiary of UnitedHealth Group Inc. As a result of this transaction, DMG's results of operations have been reported as discontinued operations for all periods presented in these consolidated financial statements. For financial information about the DMG business, see Note 22.
The Company’s U.S. dialysis and related lab services business qualifies as a separately reportable segment, and the Company’s ancillary services, including its international operations,all other operating segments have been combined and disclosed in the other segments category.
Basis of presentation
These consolidated financial statements are prepared in accordance with United States generally accepted accounting principles (U.S. GAAP). The financial statements include DaVita Inc. and its subsidiaries, partnerships and other entities in which it maintains a majority voting or other controlling financial interest (collectively, the Company). All significant intercompany transactions and balances have been eliminated. Equity investments in investees over which the Company only has significant influence are recorded on the equity method, while investments in other equity securities are recorded at fair value or on the adjusted cost method, as applicable. For the Company’s international subsidiaries, local currencies are considered their functional currencies. Translation adjustments result from translating the financial statements of the Company’s international subsidiaries from their functional currencies into the Company’s reporting currency (the U.S. dollar, or USD). Prior year classifications have been conformed to the current year presentation.
The Company has evaluated subsequent events through the date these consolidated financial statements were issued and has included all necessary adjustments and disclosures.
Use of estimates
The preparation of financial statements in conformity with U.S. GAAP requires the use of estimates and assumptions that affect the reported amounts of revenues, expenses, assets, liabilities, contingencies and noncontrolling interests subject to put provisions. Although actual results in subsequent periods will differ from these estimates, such estimates are developed based on the best information available to management and management’s best judgments at the time. All significant assumptions and estimates underlying the amounts reported in the financial statements and accompanying notes are regularly reviewed and updated when necessary. Changes in estimates are reflected in the financial statements based upon on-going actual experience trends or subsequent settlements and realizations depending on the nature and predictability of the estimates and contingencies.
The most significant assumptions and estimates underlying these consolidated financial statements and accompanying notes involve revenue recognition and accounts receivable, impairments of goodwill, accounting for income taxes, certain fair value estimates and loss contingencies. Specific estimating risks and contingencies are further addressed within these notes to the consolidated financial statements.
Revenues
On January 1, 2018, the Company adopted Financial Accounting Standards Board (FASB) Accounting Standards Codification Topic 606 Revenue from Contracts with Customers (Topic 606) using the cumulative effect method for those contracts that were not substantially completed as of January 1, 2018. Results for reporting periods beginning on and after January 1, 2018 are presented under Topic 606.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
The adoption of this new standard primarily changed the Company’s presentation of revenues, provision for uncollectible accounts and allowance for doubtful accounts. Topic 606 requires revenue to be recognized based on the Company’s estimate of the transaction price the Company expects to collect as a result of satisfying its performance obligations. Accordingly, for performance obligations satisfied after the adoption of Topic 606, the Company no longer separately presents a provision for uncollectible accounts on the consolidated income statement and no longer presents the related allowance for doubtful accounts on the consolidated balance sheet. However, as a result of the Company’s election to apply Topic 606 only to contracts not substantially completed as of January 1, 2018, the Company continued to maintain an allowance for doubtful accounts related to performance obligations satisfied prior to the adoption of Topic 606. Net collections or write-offs of accounts receivable generated prior to January 1, 2018, beyond amounts previously reserved thereon, are presented in the provision for uncollectible accounts on the consolidated income statement in accordance with Topic 605.
Dialysis patient service revenues
Revenues are recognized based on the Company’s estimate of the transaction price the Company expects to collect as a result of satisfying its performance obligations. Dialysis patient service revenues are recognized in the period services are provided based on these estimates. Revenues consist primarily of payments from government and commercial health plans for dialysis services provided to patients. AThe Company maintains a usual and customary fee schedule is maintained for the Company’sits dialysis treatments and related lab services; however, actual collectible revenue is normally recognized at a discount from thethis fee schedule.
Revenues associated with Medicare and Medicaid programs are estimated based on: (a) the payment rates that are established by statute or regulation for the portion of payment rates paid by the government payor (e.g., 80% for Medicare
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
patients) and (b) for the portion not paid by the primary government payor, estimates of the amounts ultimately collectible from other government programs providing secondary coverage (e.g., Medicaid secondary coverage), the patient’s commercial health plan secondary coverage, or the patient.
Under Medicare’s bundled payment rate system, services covered by Medicare are subject to estimating risk, whereby reimbursements from Medicare can vary significantly depending upon certain patient characteristics and other variable factors. Even with the bundled payment rate system, Medicare payments for bad debt claims as established by cost reports require evidence of collection efforts. As a result, billing and collection of Medicare bad debt claims can be delayed significantly and final payment is subject to audit. The Company’s revenue recognition is estimated based on its judgment regarding its ability to collect, which depends upon its ability to effectively capture, document and bill for Medicare’s base payment rate as well as these other variable factors.
Medicare Advantage revenues are reimbursed at negotiated contract rates that are generally higher than Medicare fee-for-service rates, but which generally have a slower payment cycle than Medicare fee-for-service payments, and some of which are subject to certain quality or performance adjustments. Medicare Advantage revenues are subject to meaningful estimating risk based on factors similar to those described for commercial health plans below.
Medicaid payments, when Medicaid coverage is secondary, can also be difficult to estimate. For many states, Medicaid payment terms and methods differ from Medicare, and may prevent accurate estimation of individual payment amounts prior to billing.
Revenues associated with commercial health plans are estimated based on contractual terms for the patients under healthcare plans with which the Company has formal agreements, non-contracted health plan coverage terms if known, estimated secondary collections, historical collection experience, historical trends of refunds and payor payment adjustments (retractions), inefficiencies in the Company’s billing and collection processes that can result in denied claims for payments, delays in collections due to payor payment inefficiencies, and regulatory compliance matters.
Commercial revenue recognition also involves significant estimating risks. With many larger commercial insurers, the Company has several different contracts and payment arrangements, and these contracts often include only a subset of the Company’s centers. Some of the Company's commercial revenue contracts are also subject to certain quality or performance adjustments. In certain circumstances, it may not be possible to determine which contract, if any, should be applied prior to billing. In addition, for services provided by non-contracted centers, final collection may require specific negotiation of a payment amount, typically at a significant discount from the Company’s usual and customary rates.
As described above, there are significant risks associated with estimating dialysis patient service revenue, many of which take several years to resolve. As these estimates are refined over time, both positive and negative adjustments to revenue are recognized in the current period.
Other revenues
Other revenues consist of revenues earned by the Company's non-dialysis ancillary services as well as fees for management and administrative support services provided to outpatient dialysis businesses that the Company does not ownconsolidate. Other revenues are estimated and recognized in the period the Company's performance obligations are met, subject to applicable measurement constraints.
The Company's IKC revenues include revenues earned under risk-based arrangements, including value-based care (VBC) arrangements. Under its VBC arrangements, the Company assumes full or inshared financial risk for the total medical cost of care for patients below or above a benchmark. The benchmarks against which the Company owns a noncontrolling interest as well as revenues associatedincurs profit or loss on these contracts are typically based on the underlying premiums paid to the insuring entity (the Company's counterparty), with adjustments where applicable, or on trended and adjusted medical cost targets.
For some of the Company's non-dialysis ancillaryrisk-based arrangements (such as its special needs plans), the Company acts as a principal with respect to all medical services provided to the patient by effectively hosting or sponsoring the entire arrangement, and strategic initiatives. Revenues associatedas a result recognizes revenue and expense for all medical services provided to covered patients. However, under its VBC arrangements (including VBC contracts with dialysis managementhealth plans and via direct government programs), the Company provides health monitoring and care coordination services integrated careto patients but does not control or direct the medical services clinical research programs, physician services,that patients receive from third party providers. As a result, the Company does not include third party medical costs in its reported revenues and ESRD seamless care organizationsexpenses for its VBC arrangements, but rather recognizes revenue only for the estimated amount of shared savings or shared losses or related revenues that are estimated indirectly earned or incurred by the period services are provided. Revenues associated with pharmacy services until that business was closed in 2018 were estimated as prescriptions were filledCompany, and shippedultimately paid to patients. Revenues associated with direct primary care until that business was sold in 2018 were estimated overor by the membership period.Company, under the arrangement.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Other incomeMeasurements of revenue for the Company's IKC risk-based arrangements are complex, sensitive to a number of key inputs, and require meaningful estimates for a number of factors, including but not limited to member alignment data, third-party medical claims expense, outcomes on various quality metrics, and ultimate risk adjustment factor (RAF) scores. Information and other measurement limitations on these factors may constrain revenue recognition for a risk-based arrangement until a period after the Company's performance obligations have been met.
Other (loss) income, net
Other (loss) income includes interest income on cash and cash equivalents and short- and long-term investments, equity investment (loss) income on equity method investments other than dialysis partnerships, realized and unrealized gains and losses recognized on other investments, impairments on investments, and foreign currency transaction gains and losses.
Cash and cash equivalents
Cash equivalents are short-term highly liquid investments readily convertible to known amounts of cash that typically mature within three months or less at date of purchase.
Restricted cash and equivalents
Restricted cash and cash equivalents include funds held in trust to satisfy insurer and state regulatory requirements related to wholly-owned captive insurance companies that bear professional and general liability and workers' compensation risks for the Company as well as funds held in escrow for certain legal settlements pending finalization.escrow.
Investments in debt and equity securities
The Company classifies certain debt securities as held-to-maturity and records them at amortized cost based on the Company’s intentions and strategies concerning those investments. Equity securities that have readily determinable fair values or redemption values are recorded at estimated fair value with changes in fair value recognized in current earnings within "Otherother (loss) income, net".net. These debt and equity investments are classified as "short-term investments"short-term investments or "long-term investments"long-term investments on the Company's consolidated balance sheet. See Note 54 for further details.
Inventories
Inventories are stated at the lower of cost (first-in, first-out) or net realizable value and consist principally of pharmaceuticals and dialysis-related supplies. Rebates related to inventory purchases are recorded when earned and are based on certain qualification requirements which are dependent on a variety of factors including future pricing levels and purchase volume levels from the manufacturer and related data submission.
Property and equipment
Property and equipment is stated at cost less accumulated depreciation and amortization and is further reduced by any impairments. Maintenance and repairs are charged to expense as incurred. Disposition gains and losses are included in current operating expenses. Property and equipment assets are reviewed for possible impairment whenever significant events or changes in circumstances indicate that an impairment may have occurred. Property and equipment impairment assessments are performed at a location or market level, as applicable, based on the specific cash flows they support or protect. If the Company commits to a plan to dispose of a long-lived asset before the end of its previously estimated useful life, cash flow estimates are revised accordingly, and the Company records an asset impairment, if applicable, or accelerates depreciation over the revised estimated useful life. Upon sale or retirement of long-lived assets, the cost and related accumulated depreciation or amortization are removed from the balance sheet and any resulting gain or loss is included in current operating expenses.
Leases
The Company leases substantially all of its U.S. dialysis facilities. The majority of the Company’s facilities are leased under non-cancellable operating leases which contain renewal options. These renewal options are included in the Company's determination of thelease right-of-use assets and related lease liabilities when renewal is considered reasonably certain at the commencement date. Certain of theThe Company's leases are generally subject to periodicfixed escalation clauses or contain consumer price increases or contain fixed escalation clauses.index increases.
The Company categorizes leases with contractual terms longer than twelve months as either operating or finance leases. Finance leases are generally those leases that allow the Company to substantially utilize or pay for the entire asset over its estimated life. All other leases are categorized as operating leases. The Company has elected the practical expedient to not
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
separate lease components from non-lease components for its financing and operating leases. The Company has also elected theFor short-term lease recognition exemption and does not recognize right-of-use assets or lease liabilities for leases with a term of less than 12 months.months, the Company does not recognize lease right-of-use assets or lease liabilities and instead recognizes short-term lease costs as rent expense directly as incurred.
Financing and operating right-of-use assetslease liabilities are recognized based onmeasured at the net present value of lease payments over the lease term plus expected renewals as of the commencement date. Since most of the Company's leases do not provide an implicit rate of return, the Company uses its incremental borrowing rate based on information available at the commencement date or remeasurement date in determining the present value of lease payments.
Assets acquired under finance leases are recorded on the balance sheet within property and equipment, net and liabilities for finance lease obligations are recorded within long-term debt. Finance lease assets are amortized to depreciation expense on a straight-line basis over the shorter of their estimated useful lives or the expected lease term.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares Accretion of interest on finance lease liabilities is included in thousands, except per share data)debt expense.
Rights to use assets under operating leases are recorded on the balance sheet as operating lease right-of-use assets and liabilities for operating lease obligations are recorded as operating lease liabilities. Reductions in the carrying amountBoth amortization of operating lease right-of-use assets and interest accretion on operating lease liabilities are recorded to rent expense over the lease term. Rent expenses are included in patient care costs or general and administrative expense, as applicable, based on the business unit or corporate function for which the space is leased. The Company evaluates its lease right-of-use assets for impairments in a similar manner to long-lived assets, as described above in Property and equipment.
Amortizable intangibles
Amortizable intangible assets include noncompetition agreements, hospital service contracts, and customer relationships arising from other service contracts, each of which have finite useful lives. Amortization expense is computed using the straight-line method over the useful lives of the assets estimated as follows: non-competitionnoncompetition agreements and hospital acute service contracts over the contract term, and customer relationships from other service contracts over the remaining contract term plus expected renewal periods. Amortizable intangible assets are reviewed for possible impairment whenever significant events or changes in circumstances indicate that an impairment may have occurred. Amortizable intangible asset impairment assessments are performed on a location, market or business unit basis, as applicable, based on the specific cash flows they support or protect.
Indefinite-lived intangibles
Indefinite-lived intangible assets include international licenses and accreditations that allow the Company to be reimbursed for providing dialysis services to patients, each of which has an indefinite useful life. Indefinite-lived intangibles are not amortized, but are assessed for impairment at least annually and whenever significant events or changes in circumstances indicate that an impairment may have occurred. Costs to renew indefinite-lived intangible assets are expensed as incurred.
Equity method and other investments
Equity investments that do not have readily determinable fair values are carried on the equity method if the Company maintains significant influence over the investee.investee unless the fair value option is elected. Equity investments without readily determinable fair values for which the Company does not maintain significant influence over the investee are carried either at estimated fair value or on the adjusted cost method or at estimated fair value, as determined on an investment-specific basis. The adjusted cost method represents the Company's cost for an investment, net of any other-than-temporary impairments, as adjusted for any subsequent observation of the investment's fair value.observable price changes. These equity method and adjusted cost method investments are classified as “Equityequity method and other investments”investments on the Company's consolidated balance sheet. See Note 98 for further details.
Equity method and other investments are assessed for other-than-temporary impairment when significant events or changes in circumstances indicate that an other-than-temporary impairment may have occurred. An other-than-temporary impairment charge is recorded when the fair value of an investment has fallen below its carrying amount and the shortfall is expected to be indefinitely or permanently unrecoverable.
Income and expense from nonconsolidated dialysis partnerships accounted for as equity method investments are recorded within equity investment income, net. For ownership interests accounted for as equity method investments other than dialysis partnerships, income and expense are included on up to a one quarter lag in other (loss) income, net.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Goodwill
Goodwill represents the difference between the fair value of businesses acquired and the fair value of the identifiable tangible and intangible net assets acquired. Goodwill is not amortized, but is assessed by individual reporting unit for impairment as circumstances warrant and at least annually. An impairment charge is recognized when and to the extent a reporting unit's carrying amount is determined to exceed its fair value. The Company operates multiple reporting units. See Note 109 for further details.
Self-insurance
The Company predominantly self-insures its professional and general liability, and workers' compensation and automobile risks, and a portion of its employment liability practice risks, through its wholly-owned captive insurance companies, with excess or reinsurance coverage for additional protection. The Company is also predominantly self-insured with respect to employee medical and other health benefits. The Company records insurance liabilities for the professional and general liability, workers’ compensation, andautomobile, employee health benefit and portion of employment liability practice risks that it retains and estimates its liability for those risks using third party actuarial calculations that are based upon historical claims experience and expectations for future claims.
Income taxes
Federal, state and stateforeign income taxes are computed at currently enacted tax rates less tax credits using the asset and liability method. Deferred taxes are adjusted both for items that do not currently have tax consequences and for the cumulative effect of any changes in tax rates from those previously used to determine deferred tax assets or liabilities. Tax provisions include amounts that are currently payable, changes in deferred tax assets and liabilities that arise because of temporary differences between the timing of when items of income and expense are recognized for financial reporting and income tax purposes, changes in the recognition of tax positions and any changes in the valuation allowance caused by a change in judgment about
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
the realizability of the related deferred tax assets. A valuation allowance is established when necessary to reduce deferred tax assets to amounts expected to be realized.
The Company uses a recognition threshold of more-likely-than-not and a measurement attribute on all tax positions taken or expected to be taken in a tax return in order to be recognized in the financial statements. Once the recognition threshold is met, the tax position is then measured to determine the actual amount of benefit to recognize in the financial statements.
Stock-based compensation
The Company’s stock-based compensation expense for stock-settled awards is measured at the estimated fair value of awards on the date of grant and recognized on a cumulative straight-line basis over the vesting terms of the awards, unless the stock awards are based on non-market basednon-market-based performance metrics, in which case expense is adjusted for the ultimate number of shares expected to be issued as of the end of each reporting period. Stock-based compensation expense for cash-settled awards is based on their estimated fair values as of the end of each reporting period. The expense for all stock-based awards is recognized net of expected forfeitures.
Stock-based compensation to be settled in shares is recorded to the Company’s shareholders’ contributed capital, while stock-based compensation to be settled in cash is recorded as a liability. Shares issued upon exercise or, when applicable, vesting of stock awards, are issued from authorized but unissued shares.
Interest rate cap agreements
The Company often carries a combination of current or forward interest rate caps on portions of its variable rate debt as a means of hedging its exposure to changes in LIBORSecured Overnight Financing Rate (SOFR) interest rates as part of its overall interest rate risk management strategy. These interest rate caps are not held for trading or speculative purposes and are designated as qualifying cash flow hedges. See Note 1312 for further details.
Noncontrolling interests
Noncontrolling interests represent third-party equity ownership interests in entities which are consolidated by the Company for financial statement reporting purposes. As of December 31, 2020,2023, third parties held noncontrolling equity interests in 688696 consolidated legal entities.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Fair value estimates
Fair value is defined as the price that would be received to sell an asset or paid to transfer a liability in an orderly transaction between market participants at the measurement date. Fair value measurements are determined based on the principal or most advantageous market for the item being measured, assume that buyers and sellers are independent, willing and able to transact, and knowledgeable, with access to all information customarily available in such a transaction, and are based on assumptions that market participants would use in pricing the item, not assumptions specific to the reporting entity. The criticality of a particular fair value estimate to the Company's consolidated financial statements depends upon the nature and size of the item being measured, the extent of uncertainties involved and the nature and magnitude or potential effect of assumptions and judgments required. Certain fair value estimates can involve significant uncertainties and require significant judgment on various matters, some of which could be subject to reasonable disagreement.
The Company relies on fair value measurements and estimates for purposes that require the recording, reassessment, or adjustment of the carrying amounts of certain assets, liabilities, and noncontrolling interests subject to put provisions (redeemable equity interests classified as temporary equity). These purposes can include the accounting for business combination transactions; impairment assessments for goodwill, other intangible assets, or other long-lived assets; recurrent revaluation of investments in debt and equity securities, contingent earn-out obligations, interest rate cap agreements, and noncontrolling interests subject to put provisions; and the accounting for equity method and other investments and stock-based compensation, as applicable. The Company has also classified its assets, liabilities and temporary equity into the appropriate fair value hierarchy levels as defined by the FASB.Financial Accounting Standards Board (FASB) reflecting their differing degrees of uncertainty. See Note 2423 for further details.
New accounting standards
New standards recently adopted
In June 2016, the FASB issued ASU No. 2016-13, Financial Instruments - Credit Losses (Topic 326): Measurement of Credit Losses on Financial Instruments. The amendments in this ASU amend the impairment model to utilize an expected loss methodology in place of the incurred loss methodology for financial instruments and off-balance sheet credit exposures. The amendment requires entities to consider a broader range of information to estimate expected credit losses, which may result in earlier recognition of losses. The amendments in this ASU became effective for the Company beginning on January 1, 2020 and were applied using a modified retrospective basis. The adoption of ASU No. 2016-13 did not have a material impact on the Company's consolidated financial statements.
In August 2018, the FASB issued ASU No. 2018-13, Fair Value Measurement (Topic 820): Disclosure Framework -Changes to the Disclosure Requirements for Fair Value Measurement. The applicable amendments in this ASU remove requirements for disclosures concerning transfers between fair value measurement levels 1, 2 and 3 and disclosures concerning
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
valuation processes for level 3 fair value measurements. The applicable amendments in this ASU also add a requirement to separately disclose the changes in unrealized gains and losses included in other comprehensive income for the reporting period for level 3 items measured at fair value on a recurring basis, and require disclosure of the range and weighted average of significant unobservable inputs used to develop level 3 fair value measurements. The amendments in this ASU became effective for the Company beginning on January 1, 2020 and were applied on a prospective basis. The adoption of this ASU did not have a material impact on the Company’s consolidated financial statements.
In August 2018, the FASB issued ASU No. 2018-15, Intangibles-Goodwill and Other-Internal Use Software (Subtopic 350-40): Customer’s Accounting for Implementation Costs Incurred in a Cloud Computing Arrangement That Is a Service Contract. ASU No. 2018-15 aligns the requirements for capitalizing implementation costs incurred in a cloud computing arrangement that is a service contract with the requirements for capitalizing implementation costs incurred to develop or obtain internal-use software. The Company adopted this ASU as of January 1, 2020, using the prospective transition approach, which allows the Company to change the accounting method without restating prior periods or booking cumulative adjustments. The adoption of ASU No. 2018-15 did not have a material impact on the Company's consolidated financial statements.
New standards not yet adopted
In December 2019, the FASB issued ASU 2019-12, Income Taxes (Topic 740): Simplifying the Accounting for Income Taxes. ASU 2019-12 attempts to simplify aspects of accounting for franchise taxes and enacted changes in tax laws or rates, and clarifies the accounting for transactions that result in a step-up in the tax basis of goodwill. ASU 2019-12 is effective for public business entities for fiscal years beginning after December 15, 2020, including interim periods within that fiscal year. Early adoption is permitted for all entities. The Company has evaluated the impact of this standard on its consolidated financial statements, including accounting policies, processes, and systems, and does not expect the impact to be material.
In March 2020, the FASB issued ASUAccounting Standards Update (ASU) No. 2020-04, Reference Rate Reform (Topic 848): Facilitation of the Effects of Reference Rate Reform on Financial Reporting. ASU No. 2020-04 provides optional expedients and exceptions for applying U.S. GAAP to contract modifications and hedging relationships, subject to meeting certain criteria, that reference LIBOR or another rate that is expected to be discontinued. The amendments in this ASU were effective beginning on March 12, 2020, and the Company maycould elect to apply the amendments prospectively through December 31, 2022. In December 2022, the FASB issued ASU No. 2022-06, Reference Rate Reform (Topic 848): Deferral of the Sunset Date of Topic 848, which extended the election date to December 31, 2024. Effective January 1, 2022 certain LIBOR tenors that do not affect the Company, including the one-week and two-month U.S. dollar LIBOR rate, ceased or became non-representative. The remaining U.S. dollar LIBOR tenors ceased or became non-representative effective July 1, 2023. The application of this ASU did not have a material impact on the Company's consolidated financial statements. See Note 12 for further discussion of the Company's debt.
In October 2021, the FASB issued ASU No. 2021-08, Business Combinations (Topic 805): Accounting for Acquired Contract Assets and Contract Liabilities (ASU 2021-08). ASU 2021-08 requires application of ASC 606, Revenue from Contracts with Customers, to recognize and measure assets and liabilities from contracts with customers acquired in a business combination. This ASU created an exception to the general recognition and measurement principle in ASC 805 which results in recognition of contract assets and contract liabilities consistent with those recorded by the acquiree immediately before the acquisition date. The ASU was effective beginning January 1, 2023 and application of this ASU did not have a material impact on the Company's consolidated financial statements.
New standards not yet adopted
In November 2023, the FASB issued ASU 2023-07, Segment Reporting (Topic 280): Improvements to Reportable Segment Disclosures (ASU 2023-07), which improves reportable segment disclosure requirements, primarily through enhanced disclosures about significant segment expenses. The guidance also requires disclosure of the chief operating decision maker's (CODM) position for each segment and detail of how the CODM uses financial reporting to assess their segment’s performance. ASU 2023-07 is effective for all public entities for fiscal years beginning after December 15, 2023, with early adoption permitted. The Company is currently assessing the effect this guidance may have on its consolidated financial statements.
In December 2023, the Financial Accounting Standards Board issued ASU 2023-09, Income Taxes (Topic 740): Improvements to Income Tax Disclosures, which expands income tax disclosure requirements to include additional information related to the rate reconciliation of effective tax rates to statutory rates, as well as additional disaggregation of taxes paid in both
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
U.S. and foreign jurisdictions. The amendments in the ASU also remove disclosures related to certain unrecognized tax benefits and deferred taxes. ASU 2023-09 is effective for fiscal years beginning after December 15, 2024. The amendments may be applied prospectively or retrospectively, and early adoption is permitted. The Company is currently assessing the effect this guidance may have on its consolidated financial statements.
2. Revenue recognition and accounts receivable
The Company's revenues by segment and primary payor source were as follows:
| | Year ended December 31, 2020 |
| U.S. dialysis | | Other - Ancillary services | | Consolidated |
| Year ended December 31, 2023 | | | Year ended December 31, 2023 |
| U.S. dialysis | | | U.S. dialysis | | Other - Ancillary services | | Consolidated |
| Patient service revenues: | Patient service revenues: | | | | | |
| Medicare and Medicare Advantage | |
| Medicare and Medicare Advantage | |
| Medicare and Medicare Advantage | Medicare and Medicare Advantage | $ | 6,048,043 | | | $ | | $ | 6,048,043 | |
| Medicaid and Managed Medicaid | Medicaid and Managed Medicaid | 744,862 | | | 744,862 | |
| Other government | Other government | 455,897 | | | 380,584 | | | 836,481 | |
| Commercial | Commercial | 3,370,562 | | | 170,394 | | | 3,540,956 | |
| Other revenues: | Other revenues: | |
| Medicare and Medicare Advantage | Medicare and Medicare Advantage | | 419,662 | | | 419,662 | |
| Medicare and Medicare Advantage | |
| Medicare and Medicare Advantage | |
| Medicaid and Managed Medicaid | Medicaid and Managed Medicaid | | 1,227 | | | 1,227 | |
| Commercial | Commercial | | 33,246 | | | 33,246 | |
Other(1) | Other(1) | 40,571 | | | 47,585 | | | 88,156 | |
| Eliminations of intersegment revenues | Eliminations of intersegment revenues | (145,286) | | | (16,743) | | | (162,029) | |
| Total | Total | $ | 10,514,649 | | | $ | 1,035,955 | | | $ | 11,550,604 | |
(1)Other consistsConsists primarily of management service fees earned in the respective Company lineCompany's U.S. dialysis business and research fees, management fees, and other non-patient service revenues in the Other - ancillary services businesses.
| | | | | | | | | | | | | | | | | |
| Year ended December 31, 2022 |
| U.S. dialysis | | Other - Ancillary services | | Consolidated |
| Patient service revenues: | | | | | |
| Medicare and Medicare Advantage | $ | 6,041,496 | | | $ | | $ | 6,041,496 | |
| Medicaid and Managed Medicaid | 759,579 | | | | | 759,579 | |
| Other government | 336,991 | | | 464,921 | | | 801,912 | |
| Commercial | 3,437,306 | | | 223,216 | | | 3,660,522 | |
| Other revenues: | | | | | |
| Medicare and Medicare Advantage | | | 345,340 | | | 345,340 | |
| Medicaid and Managed Medicaid | | | 1,546 | | | 1,546 | |
| Commercial | | | 22,211 | | | 22,211 | |
Other(1) | 24,437 | | | 44,092 | | | 68,529 | |
| Eliminations of intersegment revenues | (87,035) | | | (4,206) | | | (91,241) | |
| Total | $ | 10,512,774 | | | $ | 1,097,120 | | | $ | 11,609,894 | |
(1)Consists primarily of business as well as other revenue frommanagement service fees in the Company's U.S. dialysis business and research fees, management fees, and other non-patient service revenues in the Other - ancillary services.services businesses.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
| | Year ended December 31, 2019 |
| U.S. dialysis | | Other - Ancillary services | | Consolidated |
| Year ended December 31, 2021 | | | Year ended December 31, 2021 |
| U.S. dialysis | | | U.S. dialysis | | Other - Ancillary services | | Consolidated |
| Patient service revenues: | Patient service revenues: | | | | | |
| Medicare and Medicare Advantage | |
| Medicare and Medicare Advantage | |
| Medicare and Medicare Advantage | Medicare and Medicare Advantage | $ | 6,129,697 | | | $ | | $ | 6,129,697 | |
| Medicaid and Managed Medicaid | Medicaid and Managed Medicaid | 669,089 | | | 669,089 | |
| Other government | Other government | 446,010 | | | 352,765 | | | 798,775 | |
| Commercial | Commercial | 3,286,089 | | | 144,256 | | | 3,430,345 | |
| Other revenues: | Other revenues: | |
| Medicare and Medicare Advantage | Medicare and Medicare Advantage | | 264,538 | | | 264,538 | |
| Medicare and Medicare Advantage | |
| Medicare and Medicare Advantage | |
| Medicaid and Managed Medicaid | Medicaid and Managed Medicaid | | 606 | | | 606 | |
| Commercial | Commercial | | 130,823 | | | 130,823 | |
Other(1) | Other(1) | 32,021 | | | 78,940 | | | 110,961 | |
| Eliminations of intersegment revenues | Eliminations of intersegment revenues | (132,325) | | | (14,030) | | | (146,355) | |
| Total | Total | $ | 10,430,581 | | | $ | 957,898 | | | $ | 11,388,479 | |
(1)Other consistsConsists primarily of management service fees earned in the respective Company line ofCompany's U.S. dialysis business as well asand research fees, management fees, and other revenue from the Company's ancillary services.
| | | | | | | | | | | | | | | | | |
| Year ended December 31, 2018 |
| U.S. dialysis | | Other - Ancillary services | | Consolidated |
| Patient service revenues: | | | | | |
| Medicare and Medicare Advantage | $ | 6,063,891 | | | $ | | $ | 6,063,891 | |
| Medicaid and Managed Medicaid | 628,766 | | | | | 628,766 | |
| Other government | 446,999 | | | 335,594 | | | 782,593 | |
| Commercial | 3,176,413 | | | 101,681 | | | 3,278,094 | |
| Other revenues: | | | | | |
| Medicare and Medicare Advantage | | | 492,812 | | | 492,812 | |
| Medicaid and Managed Medicaid | | | 44,246 | | | 44,246 | |
| Commercial | | | 90,890 | | | 90,890 | |
Other(1) | 19,880 | | | 130,865 | | | 150,745 | |
| Eliminations of intersegment revenues | (92,950) | | | (34,236) | | | (127,186) | |
| Total | $ | 10,242,999 | | | $ | 1,161,852 | | | $ | 11,404,851 | |
(1)Other consists of managementnon-patient service fees earnedrevenues in the respective Company line of business as well as other revenue from the Company'sOther - ancillary services.services businesses.
The majority of the Company's non-patient service revenues from Medicare and Medicare Advantage, Medicaid and Managed Medicaid, and commercial sources represent risk-based revenues earned by the Company's U.S. IKC business.
For its IKC business, the Company had 0 allowancerecognized revenues for doubtful accounts related to performance obligations satisfied in previous years prior to January 1, 2018 as of $94,361, $34,600, and $11,312 during the years ended December 31, 20202023, 2022 and such allowance was $8,328 as2021, respectively. The delay in recognition of December 31, 2019.
As described in Note 1, there are significant risks associatedthese amounts resulted predominantly from measurement limitations and recognition constraints on our VBC contracts with estimating revenue,health plans, many of which take severalare complex and relatively new arrangements. The Company's revenue recognition for its government Comprehensive Kidney Care Contracting (CKCC) program also remains heavily constrained for plan years to resolve. These estimates are subject to ongoing insurance coverage changes, geographic coverage differences, differing interpretations2023 and 2022. See Note 1 "Other revenues" for a description of contract coverage and other payor issues, as well as patient issues including determining applicable primary and secondary coverage, changes in patient coverage and coordination of benefits. Asthe Company's accounting for these estimates are refined over time, both positive and negative adjustments to revenue are recognized in the current period. As a result of these changes in estimates, 0 additional revenue was recognized during the year ended December 31, 2020 associated with performance obligations satisfied prior to January 1, 2018 and additional revenue of $37,274 was recognized during the year ended December 31, 2019 associated with performance obligations satisfied in years prior to January 1, 2018.value-based care arrangements.
There is 0No single commercial payor that accounted for more than 10% of totalconsolidated revenues or consolidated accounts receivable or consolidated revenues at or for the years ended December 31, 2020periods presented in these consolidated financial statements or 2019.at their period-ends, respectively.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Net dialysisDialysis services accounts receivable and other receivables from Medicare, including Medicare Advantage plans, and Medicaid, including managed Medicaid plans, were approximately $1,101,837$817,045 and $1,038,248$1,113,499 as of December 31, 20202023 and 2019,2022, respectively. Approximately 17%19% and 18% of the Company’s net patient services accounts receivable balances as of December 31, 20202023 and 2019,2022, respectively, were more than six months old. There were 0no significant balances over one year old at December 31, 2020.2023. The Company's accounts receivable are principally due from Medicare and Medicaid programs and commercial insurance plans.
3. Earnings per share
Basic earnings per share is calculated by dividing net income attributable to the Company by the weighted average number of common shares outstanding, reduced for 2018 by the weighted average shares held in escrow that under certain circumstances may have been returned to the Company.outstanding. Weighted average common shares outstanding include restricted stock unit awards that are no longer subject to forfeiture because the recipients have satisfied either their explicit vesting terms or retirement eligibility requirements.
Diluted earnings per share includes the dilutive effect of outstanding stock-settled stock appreciation rights and unvested stock units (under the treasury stock method) and, for 2018, the weighted average contingently returnable shares held in escrow that were outstanding during the period.
The reconciliations of the numerators and denominators used to calculate basic and diluted earnings per share were as follows:
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 |
| Net income (loss) attributable to DaVita Inc.: | | | | | |
| Continuing operations | $ | 783,295 | | | $ | 706,832 | | | $ | 624,321 | |
| Discontinued operations | (9,653) | | | 104,149 | | | (464,927) | |
| Net income attributable to DaVita Inc. | $ | 773,642 | | | $ | 810,981 | | | $ | 159,394 | |
| | | | | |
| Weighted average shares outstanding: | | | | | |
| During the period | 119,797 | | | 153,181 | | | 171,886 | |
Contingently returnable(1) | 0 | | | 0 | | | (1,100) | |
| Basic shares | 119,797 | | | 153,181 | | | 170,786 | |
Contingently returnable(1) | 0 | | | 0 | | | 1,100 | |
| Assumed incremental from stock plans | 2,826 | | | 631 | | | 479 | |
| Diluted shares | 122,623 | | | 153,812 | | | 172,365 | |
| | | | | |
| Basic net income (loss) attributable to DaVita Inc.: | | | | | |
| Continuing operations per share | $ | 6.54 | | | $ | 4.61 | | | $ | 3.66 | |
| Discontinued operations per share | (0.08) | | | 0.68 | | | (2.73) | |
| Basic net income per share attributable to DaVita Inc. | $ | 6.46 | | | $ | 5.29 | | | $ | 0.93 | |
| | | | | |
| Diluted net income (loss) attributable to DaVita Inc.: | | | | | |
| Continuing operations per share | $ | 6.39 | | | $ | 4.60 | | | $ | 3.62 | |
| Discontinued operations per share | (0.08) | | | 0.67 | | | (2.70) | |
| Diluted net income per share attributable to DaVita Inc. | $ | 6.31 | | | $ | 5.27 | | | $ | 0.92 | |
| | | | | |
Anti-dilutive stock-settled awards excluded from calculation(2) | 2,301 | | | 5,936 | | | 5,295 | |
(1)Shares previously held in escrow for the DaVita HealthCare Partners merger.
(2)Shares associated with stock awards excluded from the diluted denominator calculation because they were anti-dilutivecomputed under the treasury stock method.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
4. Restricted cash and equivalents
The Company had restricted cash and cash equivalents of $176,832 and $106,346 at December 31, 2020 and 2019, respectively. Approximately $92,286reconciliations of the balance at December 31, 2020 represents restricted cash equivalents held in trustnumerators and denominators used to satisfy insurercalculate basic and state regulatory requirements related todiluted earnings per share were as follows:
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2023 | | 2022 | | 2021 |
| Net income attributable to DaVita Inc.: | | | | | |
| Continuing operations | $ | 691,535 | | | $ | 546,948 | | | $ | 978,450 | |
| Discontinued operations | — | | | 13,452 | | | — | |
| Net income attributable to DaVita Inc. | $ | 691,535 | | | $ | 560,400 | | | $ | 978,450 | |
| | | | | |
| Weighted average shares outstanding: | | | | | |
| Basic shares | 90,790 | | | 92,992 | | | 105,230 | |
| Assumed incremental from stock plans | 2,392 | | | 2,842 | | | 4,718 | |
| Diluted shares | 93,182 | | | 95,834 | | | 109,948 | |
| | | | | |
| Basic net income attributable to DaVita Inc.: | | | | | |
| Continuing operations per share | $ | 7.62 | | | $ | 5.88 | | | $ | 9.30 | |
| Discontinued operations per share | — | | | 0.15 | | | — | |
| Basic net income per share attributable to DaVita Inc. | $ | 7.62 | | | $ | 6.03 | | | $ | 9.30 | |
| | | | | |
| Diluted net income attributable to DaVita Inc.: | | | | | |
| Continuing operations per share | $ | 7.42 | | | $ | 5.71 | | | $ | 8.90 | |
| Discontinued operations per share | — | | | 0.14 | | | — | |
| Diluted net income per share attributable to DaVita Inc. | $ | 7.42 | | | $ | 5.85 | | | $ | 8.90 | |
| | | | | |
Anti-dilutive stock-settled awards excluded from calculation(1) | 531 | | | 1,058 | | | 116 | |
(1)Shares associated with stock awards excluded from the wholly-owned captive insurance companies that bear professional and general liability and workers' compensation risks fordiluted denominator calculation because they were anti-dilutive under the Company and $70,000 represents cash held in escrow to fund a previously announced legal settlement pending finalization. The remaining restricted cash and cash equivalents held at December 31, 2020 primarily represents cash pledged to third parties in connection with 1 of the Company's ancillary services.treasury stock method.
5.4. Short-term and long-term investments
The Company’s short-term and long-term investments, consisting of debt instruments classified as held-to-maturity and equity investments with readily determinable fair values or redemption values, were as follows:
| | | | December 31, 2020 | | December 31, 2019 | | December 31, 2023 | | December 31, 2022 |
| | | Debt
securities | | Equity
securities | | Total | | Debt
securities | | Equity
securities | | Total | | Debt
securities | | Equity
securities | | Total | | Debt
securities | | Equity
securities | | Total |
| Certificates of deposit and other time deposits | Certificates of deposit and other time deposits | $ | 8,217 | | | $ | 0 | | | $ | 8,217 | | | $ | 8,140 | | | $ | 0 | | | $ | 8,140 | |
| Investments in mutual funds and common stock | Investments in mutual funds and common stock | 0 | | | 44,077 | | | 44,077 | | | 0 | | | 39,951 | | | 39,951 | |
| | | $ | 8,217 | | | $ | 44,077 | | | $ | 52,294 | | | $ | 8,140 | | | $ | 39,951 | | | $ | 48,091 | |
| Short-term investments | Short-term investments | $ | 8,217 | | | $ | 11,884 | | | $ | 20,101 | | | $ | 8,140 | | | $ | 3,432 | | | $ | 11,572 | |
| Long-term investments | Long-term investments | 0 | | | 32,193 | | | 32,193 | | | 0 | | | 36,519 | | | 36,519 | |
| | | $ | 8,217 | | | $ | 44,077 | | | $ | 52,294 | | | $ | 8,140 | | | $ | 39,951 | | | $ | 48,091 | |
Debt securities: The Company's short-term debt investments are principally bank certificates of deposit with contractual maturities longer than three months but shorter than one year. The Company's long-term debt investments are bank time deposits with contractual maturities longer than one year. These debt securities are accounted for as held-to-maturity and recorded at amortized cost, which approximated their fair values at December 31, 20202023 and 2019.2022.
Equity securities: TheSubstantially all of the Company's short-term and long-term equity investments in mutual funds and common stock are held within a trust to fund existing obligations associated with several of the Company’s non-qualified deferred compensation plans. During 2020, the Company recognized pre-tax net gains of $3,818
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in other income associated with changes in the fair value of these equity securities, comprised of pre-tax realized gains of $1,941 and a net increase in unrealized gains of $1,877. During 2019, the Company recognized pre-tax net gains of $4,383 in other income associated with changes in the fair value of these equity securities, comprised of pre-tax realized gains of $1,459 and a net increase in unrealized gains of $2,924.thousands, except per share data)
6.5. Other receivables
Other receivables were comprised of the following:
| | | | | | | | | | | |
| | December 31, |
| | 2020 | | 2019 |
| Supplier rebates and non-trade receivables | $ | 390,508 | | | $ | 351,650 | |
| Medicare bad debt claims | 153,868 | | | 138,045 | |
| | $ | 544,376 | | | $ | 489,695 | |
| | | | | | | | | | | |
| | December 31, |
| | 2023 | | 2022 |
| Customer contract assets: | | | |
| Medicare bad debt claims | $ | 107,444 | | | $ | 110,751 | |
| IKC VBC arrangements | 127,442 | | | 13,932 | |
| Supplier rebates and non-trade receivables | $ | 187,783 | | | $ | 289,293 | |
| | $ | 422,669 | | | $ | 413,976 | |
7.6. Property and equipment
Property and equipment were comprised of the following:
| | | | December 31, | | December 31, |
| | | 2020 | | 2019 | | 2023 | | 2022 |
| Land | Land | $ | 37,924 | | | $ | 36,480 | |
| Buildings | Buildings | 400,616 | | | 392,256 | |
| Leasehold improvements | Leasehold improvements | 3,865,729 | | | 3,545,224 | |
| Equipment and information systems, including internally developed software | Equipment and information systems, including internally developed software | 3,081,298 | | | 2,880,645 | |
| New center and capital asset projects in progress | New center and capital asset projects in progress | 616,686 | | | 588,345 | |
| | | 8,002,253 | | | 7,442,950 | |
| Less accumulated depreciation | Less accumulated depreciation | (4,480,429) | | | (3,969,566) | |
| | | $ | 3,521,824 | | | $ | 3,473,384 | |
Depreciation and amortization expenses are computed using the straight-line method over the useful lives of the assets estimated as follows: buildings, 25 years to 40 years; leasehold improvements, the shorter of ten years or the expected lease term; and equipment and information systems, including internally developed software, principally three years to 15 years. Depreciation expense on property and equipment was $616,626, $600,905,$736,474, $721,133 and $574,799$667,755 for 2020, 20192023, 2022 and 2018,2021, respectively.
Interest on debt incurred during the development of new centers and other capital asset projects is capitalized as a component of the asset cost based on the respective in-process capital asset balances. Interest capitalized was $17,944, $27,322$9,178, $12,677 and $25,978$15,275 for 2020, 20192023, 2022 and 2018,2021, respectively.
During 2018, the Company recognized asset impairment charges of $17,338 related to the restructuring of its pharmacy business.
8.7. Intangible assets
Intangible assets other than goodwill were comprised of the following:
| | | | December 31, | | December 31, |
| | | 2020 | | 2019 | | 2023 | | 2022 |
| Indefinite-lived licenses | Indefinite-lived licenses | $ | 100,138 | | | $ | 90,209 | |
| Noncompetition agreements | Noncompetition agreements | 84,022 | | | 103,510 | |
| Customer relationships and other | Customer relationships and other | 52,566 | | | 23,887 | |
| | | 236,726 | | | 217,606 | |
| Less accumulated amortization | (70,141) | | | (81,922) | |
| Accumulated amortization: | |
| Noncompetition agreements | |
| Noncompetition agreements | |
| Noncompetition agreements | |
| Customer relationships and other | |
| | | $ | 166,585 | | | $ | 135,684 | |
Noncompetition agreements are generally amortized over threefour years to 10 years and customer relationships are principally amortized over 10 years to 20 years. The weighted average renewal or extension period of customer relationships was two years as of December 31, 2023 and 2022. Amortization expense from amortizable intangible assets was $13,809, $14,247,$8,969, $11,469, and $16,236$12,860 for 2020, 20192023, 2022 and 2018,2021, respectively.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
For the years ended December 31, 2020, 20192023, 2022 and 2018,2021, the Company recognized 0no impairment charges on any intangible assets other than goodwill. See Note 9 for further information regarding goodwill.
Scheduled amortization expenses from amortizable intangible assets as of December 31, 2023 were as follows:
| | | | | | | | | | | |
| | Noncompetition
agreements | | Customer relationships and other |
| 2024 | $ | 3,049 | | | $ | 3,978 | |
| 2025 | 1,921 | | | 3,712 | |
| 2026 | 1,182 | | | 3,642 | |
| 2027 | 730 | | | 3,525 | |
| 2028 | 528 | | | 3,472 | |
| Thereafter | — | | | 23,502 | |
| Total | $ | 7,410 | | | $ | 41,831 | |
8. Equity method and other investments
The Company maintains equity method and other minor investments in the goodwill impairment charges discussedprivate securities of certain other healthcare and healthcare-related businesses as follows:
| | | | | | | | | | | |
| | December 31, |
| | 2023 | | 2022 |
| Mozarc Medical Holding LLC | $ | 324,711 | | | $ | — | |
| APAC joint venture | 98,865 | | | 99,141 | |
| Other equity method partnerships | 107,282 | | | 116,403 | |
| Adjusted cost method and other investments | 14,990 | | | 15,564 | |
| $ | 545,848 | | | $ | 231,108 | |
During 2023, 2022 and 2021, the Company recognized equity investment income of $27,864, $26,520 and $26,937, respectively, from its equity method investments in Note 10.nonconsolidated dialysis partnerships. The Company also recognized equity investment losses from other equity method investments of $59,508, $4,703 and $1,292 in other (loss) income, net during 2023, 2022 and 2021, respectively.
On May 25, 2022, the Company entered into an agreement with Medtronic, Inc. and one of its subsidiaries (collectively, Medtronic) to form a new, independent kidney care-focused medical device company (Mozarc Medical Holding LLC, or Mozarc) via a deconsolidating partial interest sale from Medtronic to the Company which closed effective April 1, 2023. The Company holds a 50% voting equity interest in Mozarc and Medtronic holds the other 50% voting equity interest. The Company does not maintain a controlling financial interest in Mozarc and therefore accounts for this investment on the equity method, with equity method income or loss recognized in other (loss) income, net, on a one-month lag.
At the closing, the Company made an estimated purchase price payment, including certain transaction cost adjustments, to Medtronic of $44,651, subject to certain customary post-closing adjustments, and contributed certain other non-cash assets to Mozarc with an estimated value of $14,539. In addition, the Company agreed to pay Medtronic additional consideration of up to $300,000 if certain regulatory, commercial and financial milestones are achieved between 2024 and 2028. At close, the Company and Medtronic also each contributed an additional $224,415 in cash to Mozarc to fund its development initiatives.
The Company’s investment in Mozarc was recorded at an estimated cost of $375,326, which represents the sum of the cash amounts paid and contributed for the Company’s investment in Mozarc, the estimated fair value of the non-cash assets contributed, the estimated fair value of the Company’s contingent consideration payable to Medtronic for its interest in Mozarc of $86,200, and direct costs incurred to complete this transaction. The foregoing cost estimates are based upon the best information available to management but remain subject to change based on finalization of post-closing purchase price adjustments yet to be completed between the parties and finalization of related third-party valuation reports. As of December 31, 2023, the book value of the Company's contingent consideration payable to Medtronic approximates its estimated fair value, which is based on level 3 inputs.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Scheduled amortization expenses from amortizable intangible assets asThe recorded cost of December 31, 2020 were as follows:
| | | | | | | | | | | |
| | Noncompetition
agreements | | Customer relationships and other |
| 2021 | $ | 10,274 | | | $ | 3,143 | |
| 2022 | 6,680 | | | 3,139 | |
| 2023 | 3,883 | | | 3,102 | |
| 2024 | 1,714 | | | 2,851 | |
| 2025 | 585 | | | 2,660 | |
| Thereafter | 168 | | | 28,248 | |
| Total | $ | 23,304 | | | $ | 43,143 | |
9. Equity method and other investments
The Company maintainsthe Company's equity method and other minor investmentsinvestment in the private securities of certain other healthcareMozarc, and healthcare-related businesses, comprised as follows:
| | | | | | | | | | | |
| | December 31, |
| | 2020 | | 2019 |
| APAC joint venture | $ | 120,787 | | | $ | 116,924 | |
| Other equity method partnerships | 107,599 | | | 114,611 | |
| Adjusted cost method and other investments | 29,105 | | | 10,448 | |
| $ | 257,491 | | | $ | 241,983 | |
During 2020, 2019 and 2018, the Company recognized equity investment income (loss) of $26,916, $12,679 and $(4,484), respectively, from its equity method investments in nonconsolidated businesses. income (loss) from that investment, remain subject to finalization of fair value estimates for the following based on third-party valuation reports: the Company's non-cash assets contributed to Mozarc, the Company's contingent consideration payable to Medtronic, and valuation of Mozarc's underlying net assets, including its intangible assets, fixed assets, leases and certain working capital items, some of which are pending final quantification for certain post-closing purchase price adjustments.
The Company's largest equity method investment is its ownershipCompany also holds a 75%voting and economic interest in DaVita Care Pte. Ltd. (the APAC joint venture, or APAC JV). The Company holds a 75%voting and economic interest in the APAC JV and an unrelated noncontrolling investor holds the other 25% voting and economic interest in the joint venture. During 2019 the continuing third party noncontrolling investor made its final subscribed capital contribution to the joint venture and the other previous third party noncontrolling investor elected to exit the joint venture. The governance structure and voting rights established forCompany does not control or consolidate the APAC JV which remain unchanged since its formation on August 1, 2016, provide thatas a result of substantive participating rights retained by the unrelated investor over certain key operating decisions affectingfor the joint venture’s operations are not subject to the unilateral discretion of the Company but rather are under the joint control of the Company and the APAC JV's unrelated noncontrolling investor. As a result, the Company does not consolidate the APAC JV.venture.
Prior to the transactions described above, the Company held a 60% voting interest and a 73.3% economic interest in the APAC JV, while the other two noncontrolling investors collectively held a 40% voting interest and a 26.7% economic interest in the APAC JV.
The Company's other equity method investments include 2223 legal entities over which the Company has significant influence but in which it does not maintain a controlling financial interest. Almost all of these are U.S. dialysis partnerships in the form of limited liability companies. The Company's ownership interests in these partnerships vary, and are often subject to blocking rights on certain key operating decisions held by outside investors, but typicallymostly range from 30% to 50%65%.
There were 0 significantFor the year ended December 31, 2022, the Company recognized impairments orand other valuation adjustments on the Company's adjusted cost method and other investments during 2020, 2019of $20,154 in other (loss) income, net. There were no significant investment impairments or 2018.
other valuation adjustments for the years ended December 31, 2023 and 2021.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
10.9. Goodwill
Changes in the carrying value of goodwill by reportable segment were as follows:
| | | | | | | | | | | | | | | | | |
| | U.S. dialysis | | Other - Ancillary
services | | Consolidated |
| Balance at December 31, 2018 | $ | 6,275,004 | | | $ | 566,956 | | | $ | 6,841,960 | |
| Acquisitions | 18,089 | | | 72,137 | | | 90,226 | |
| Impairment charges | 0 | | | (124,892) | | | (124,892) | |
| Foreign currency and other adjustments | (5,993) | | | (13,666) | | | (19,659) | |
| Balance at December 31, 2019 | $ | 6,287,100 | | | $ | 500,535 | | | $ | 6,787,635 | |
| Acquisitions | 24,377 | | | 105,680 | | | 130,057 | |
| Divestitures | (1,549) | | | (6,744) | | | (8,293) | |
| Foreign currency and other adjustments | 0 | | | 9,710 | | | 9,710 | |
| Balance at December 31, 2020 | $ | 6,309,928 | | | $ | 609,181 | | | $ | 6,919,109 | |
| | | | | |
| Balance at December 31, 2020: | | | | | |
| Goodwill | $ | 6,309,928 | | | $ | 745,732 | | | $ | 7,055,660 | |
| Accumulated impairment charges | 0 | | | (136,551) | | | (136,551) | |
| $ | 6,309,928 | | | $ | 609,181 | | | $ | 6,919,109 | |
As dialysis treatments are an essential, life-sustaining service for patients who depend on them, the Company's operations have continued and are currently expected to continue throughout the novel coronavirus (COVID-19) pandemic. However, the ultimate impact of the dynamic and evolving COVID-19 pandemic on the Company will depend on future developments that are highly uncertain and difficult to predict, including among other things the severity and duration of the pandemic, further spread or resurgence of the virus, including as a result of the emergence of the new strains of the virus, its impact on the chronic kidney disease (CKD) patient population and the Company's patient population, the availability, acceptance, impact and efficacy of COVID-19 treatments, therapies and vaccines, the pandemic's continuing impact on the U.S. and global economies and unemployment, the responses of the Company's competitors to the pandemic and related changes in the marketplaces, and the timing, scope and effectiveness of governmental responses. While the Company does not currently expect a material adverse impact to its business as a result of this public health crisis, there can be no assurance that the COVID-19 pandemic will not have a material adverse impact on one or more of the Company's businesses. | | | | | | | | | | | | | | | | | |
| | U.S. dialysis | | Other - Ancillary
services | | Consolidated |
| Balance at December 31, 2021 | $ | 6,400,162 | | | $ | 646,079 | | | $ | 7,046,241 | |
| Acquisitions | 16,750 | | | 32,297 | | | 49,047 | |
| Divestitures | (87) | | | (3,263) | | | (3,350) | |
| | | | | |
| Foreign currency and other adjustments | — | | | (15,328) | | | (15,328) | |
| Balance at December 31, 2022 | $ | 6,416,825 | | | $ | 659,785 | | | $ | 7,076,610 | |
| Acquisitions | — | | | 25,723 | | | 25,723 | |
| | | | | |
| Impairment charges | — | | | (26,083) | | | (26,083) | |
| Foreign currency and other adjustments | — | | | 36,310 | | | 36,310 | |
| Balance at December 31, 2023 | $ | 6,416,825 | | | $ | 695,735 | | | $ | 7,112,560 | |
| | | | | |
| Balance at December 31, 2023: | | | | | |
| Goodwill | $ | 6,416,825 | | | $ | 844,836 | | | $ | 7,261,661 | |
| Accumulated impairment charges | — | | | (149,101) | | | (149,101) | |
| $ | 6,416,825 | | | $ | 695,735 | | | $ | 7,112,560 | |
Each of the Company’s operating segments described in Note 2524 to these consolidated financial statements represents an individual reporting unit for goodwill impairment assessment purposes.
Within the U.S. dialysis operating segment, the Company considers each of its dialysis centers to constitute an individual business for which discrete financial information is available. However, since these dialysis centers have similar operating and economic characteristics, and the allocation of resources and significant investment decisions concerning these businesses are highly centralized and the benefits broadly distributed, the Company has aggregated these centers and deemed them to constitute a single reporting unit.
The Company has applied a similar aggregation to the physician practices in its physician services reporting units and to the dialysis centers and other health operations within each international reporting unit, and to the vascular access service centers in its former vascular access services reporting unit. For the Company’s other operating segments, discrete business components below the operating segment level constitute individual reporting units.
When performing quantitative goodwill impairment assessments, the Company estimates fair value using either appraisals developed with an independent third party valuation firm which consider both discounted cash flow estimates for the
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
subject business and observed market multiples for similar businesses, or offer prices received for the subject business that would be acceptable to the Company.
During the year ended December 31, 2019,2023, the Company recognized goodwill impairment charges of $119,476 in its Germany kidney care business. These charges resulted primarily from a decline in then current and expected future patient census and an increase in then current and expected future costs, including due to wage increases expected to result from legislation announced at that time. The changes in the Company's expectations were informed by developments in the business in response to evolving market conditions, including changes in the Company's expected timing and ability to mitigate them,
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
and based on in-depth operating and strategic reviews completed by the Company's new Germany management team. During the year ended December 31, 2019 the Company also recognized a goodwill impairment charge of $5,416$26,083 in its German other health operations.
Based on its most recent assessments, the Company determined that further changes in expected patient census, increases in operating costs, reductions in reimbursement rates, changes in actual or expected growth rates, or other significant adverse changes in expected future cash flows or valuation assumptions could result in goodwill impairment charges in the future for the followingtransplant software reporting unit, which remains at riskor $19,575 net of goodwill impairment as of December 31, 2020:
| | | | | | | | | | | | | | | | | | | | | | | | | | |
| Reporting unit | | Goodwill
balance | | Carrying amount coverage(1) | | Sensitivities |
Operating income(2) | | Discount rate(3) |
| Germany kidney care | | $ | 322,736 | | | 2.3 | % | | (1.5) | % | | (10.1) | % |
| | | | | | | | |
(1)Excess oftax. This charge resulted from a reduction in estimated fair value offor the reporting unit overbusiness driven primarily from the business not achieving its carrying amountrevenue targets, with reduced revenue expectations for future years, as of the latest assessment date.
(2)Potential impact on estimated fair value of a sustained, long-term reduction of 3% in operating incomewell as of the latest assessment date.
(3)Potential impact on estimated fair value of an increase in discount ratesthe risk-free rate. After this impairment charge, the transplant software reporting unit has a goodwill balance of 100 basis points as$14,424 remaining, which could be further impaired if the business fails to meet its revised revenue targets and growth expectations.
None of the latest assessment date.
Except as described above, 0ne of the Company’s other reporting units were considered at risk of significant goodwill impairment as of December 31, 2020.2023. Since the dates of the Company’s last annual goodwill impairment assessments, there have been certain developments, events, changes in operating performance and other changes in key circumstances that have affected the Company’s businesses. However, these have not caused management to believe it is more likely than not that the fair values of any of the Company’s reporting units would be less than their respective carrying amounts as of December 31, 2020.2023.
11.10. Other liabilities
Other liabilities were comprised of the following:
| | | | December 31, | | December 31, |
| | | 2020 | | 2019 | | 2023 | | 2022 |
| Payor refunds and retractions | Payor refunds and retractions | $ | 371,183 | | | $ | 377,044 | |
| Insurance and self-insurance accruals | Insurance and self-insurance accruals | 54,438 | | | 58,941 | |
| Accrued interest | Accrued interest | 30,066 | | | 54,899 | |
| Accrued non-income tax liabilities | Accrued non-income tax liabilities | 39,075 | | | 36,285 | |
| Other | Other | 315,767 | | | 229,005 | |
| | | $ | 810,529 | | | $ | 756,174 | |
12.11. Income taxes
The Company accounts for income taxes under the asset and liability method, which requires the recognition of deferred tax assets and liabilities for the expected future tax consequences of events that have been included in the consolidated financial statements. Under this method, deferred tax assets and liabilities are determined on the basis of the differences between the financial statement and tax basis of assets and liabilities using enacted tax rates in effect for the year in which the differences are expected to reverse.
Income before income taxes from continuing operations consisted of the following:
| | | | Year ended December 31, | | Year ended December 31, |
| | | 2020 | | 2019 | | 2018 | | 2023 | | 2022 | | 2021 |
| Domestic | Domestic | $ | 1,287,976 | | | $ | 1,307,299 | | | $ | 1,083,578 | |
| International | International | 30,286 | | | (111,860) | | | (35,100) | |
| | | $ | 1,318,262 | | | $ | 1,195,439 | | | $ | 1,048,478 | |
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Income tax expense for continuing operations consisted of the following:
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 |
| Current: | | | | | |
| Federal | $ | 47,171 | | | $ | 208,339 | | | $ | 140,064 | |
| State | 21,442 | | | 58,026 | | | 32,990 | |
| International | 17,481 | | | 15,545 | | | 7,557 | |
| Total current income tax | 86,094 | | | 281,910 | | | 180,611 | |
| Deferred: | | | | | |
| Federal | 198,623 | | | 44,263 | | | 52,034 | |
| State | 27,206 | | | (25,836) | | | 21,096 | |
| International | 2,009 | | | (20,709) | | | 4,659 | |
| Total deferred income tax | 227,838 | | | (2,282) | | | 77,789 | |
| | $ | 313,932 | | | $ | 279,628 | | | $ | 258,400 | |
Income taxes are allocated between continuing and discontinued operations as follows:
| | | | | | | | | | | | | | | | | |
| Year ended December 31, |
| 2020 | | 2019 | | 2018 |
| Continuing operations | $ | 313,932 | | | $ | 279,628 | | | $ | 258,400 | |
| Discontinued operations | 1,657 | | | 40,689 | | | 99,768 | |
| $ | 315,589 | | | $ | 320,317 | | | $ | 358,168 | |
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2023 | | 2022 | | 2021 |
| Current: | | | | | |
| Federal | $ | 200,070 | | | $ | 201,932 | | | $ | 216,539 | |
| State | 38,370 | | | 55,593 | | | 15,601 | |
| International | 21,008 | | | 16,253 | | | 14,247 | |
| Total current income tax | 259,448 | | | 273,778 | | | 246,387 | |
| Deferred: | | | | | |
| Federal | (40,234) | | | (66,400) | | | 59,528 | |
| State | 367 | | | (12,289) | | | 5,342 | |
| International | 535 | | | 2,998 | | | (4,525) | |
| Total deferred income tax | (39,332) | | | (75,691) | | | 60,345 | |
| | $ | 220,116 | | | $ | 198,087 | | | $ | 306,732 | |
The reconciliation between the Company’s effective tax rate from continuing operations and the U.S. federal income tax rate is as follows:
| | | | Year ended December 31, | | Year ended December 31, |
| | | 2020 | | 2019 | | 2018 | | 2023 | | 2022 | | 2021 |
| Federal income tax rate | Federal income tax rate | 21.0 | % | | 21.0 | % | | 21.0 | % | Federal income tax rate | 21.0 | % | | 21.0 | % | | 21.0 | % |
| State income taxes, net of federal benefit | State income taxes, net of federal benefit | 3.4 | | | 2.3 | | | 4.1 | |
| Change in International valuation allowance | 1.5 | | | 1.3 | | | 0.9 | |
| | Equity compensation | |
| Federal and international tax rate adjustments | |
| Nondeductible executive compensation | |
| Political advocacy costs | Political advocacy costs | 1.7 | | | 0.2 | | | 2.3 | |
| Nondeductible executive compensation | 1.2 | | | 0.8 | | | 0.7 | |
| Unrecognized tax benefits | Unrecognized tax benefits | 0.4 | | | 2.4 | | | 0.2 | |
| Change in international valuation allowance | |
| Credits | |
| Other | Other | (0.6) | | | 0.3 | | | 0 | |
Impact of noncontrolling interests primarily
attributable to non-tax paying entities | Impact of noncontrolling interests primarily
attributable to non-tax paying entities | (4.8) | | | (4.9) | | | (4.6) | |
| Effective tax rate | Effective tax rate | 23.8 | % | | 23.4 | % | | 24.6 | % | Effective tax rate | 18.7 | % | | 20.5 | % | | 20.2 | % |
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Deferred tax assets and liabilities arising from temporary differences for continuing operations were as follows:
| | | | December 31, | | December 31, |
| | | 2020 | | 2019 | | 2023 | | 2022 |
| Receivables | Receivables | $ | 9,324 | | | $ | 19,095 | |
| Accrued liabilities | Accrued liabilities | 64,982 | | | 64,458 | |
| Operating lease liabilities | Operating lease liabilities | 584,656 | | | 580,110 | |
| Net operating loss carryforwards | Net operating loss carryforwards | 167,398 | | | 139,690 | |
| Other | Other | 62,110 | | | 55,108 | |
| Deferred tax assets | Deferred tax assets | 888,470 | | | 858,461 | |
| Valuation allowance | Valuation allowance | (114,824) | | | (91,925) | |
| Net deferred tax assets | Net deferred tax assets | 773,646 | | | 766,536 | |
| Intangible assets | Intangible assets | (634,736) | | | (563,914) | |
| Property and equipment | Property and equipment | (274,742) | | | (162,628) | |
| Operating lease assets | Operating lease assets | (532,082) | | | (527,056) | |
| Investments in partnerships | Investments in partnerships | (101,996) | | | (64,960) | |
| Other | Other | (39,690) | | | (25,521) | |
| Deferred tax liabilities | Deferred tax liabilities | (1,583,246) | | | (1,344,079) | |
| Net deferred tax liabilities | Net deferred tax liabilities | $ | (809,600) | | | $ | (577,543) | |
| Reported as: | |
| Deferred tax liabilities | |
| Deferred tax liabilities | |
| Deferred tax liabilities | |
| Deferred tax assets (included in Other long-term assets) | |
| $ | |
At December 31, 2020,2023, the Company had federal net operating loss carryforwards of approximately $99,657$57,649 that expire through 2036, although a substantial amount expire by 2029. The Company also had state net operating loss carryforwards of $488,070,$501,405, some of which have an indefinite life, although a substantial amount expire by 20402043 and international net operating loss carryforwards of $296,451,$391,510, some of which will begin to expire in 20212026 though the majority have an indefinite life. The Company has a state capital loss carryover of $297,748,$299,803, the majority of which expires in 2024. The utilization of a portion of these losses may be limited in future years based on the profitability of certain entities. A valuation allowance is recorded to account for the unrealizable balances in the table above. The net increase of $22,899$6,462 in the valuation allowance is primarily due to newly created net operating loss carryforwardslosses generated in state and foreign jurisdictions and from equity investments that the Company does not anticipate being able to utilize.
During the year ended December 31, 2021, the Company recorded a true-up to recognize net deferred tax assets related to historical purchases of noncontrolling interests in consolidated partnerships. The Company's foreign earnings continueeffect of this adjustment was an increase of $46,692 to benet deferred tax assets, a charge of $16,044 to income tax expense, and an increase of $62,736 to additional paid-in capital. The Company’s prior purchases of this type have not generated significant pre-tax adjustments to additional paid-in capital in any single prior year. The majority of the $16,044 recorded to income tax expense was due to the decrease in the corporate tax rate in 2017.
The Company remains indefinitely reinvested in several of the foreign jurisdictions in which it operates as of December 31, 2020.2023. As a result of the passage of the Tax Cuts and Jobs Act (2017 Tax Act), the Company does not expect any significant taxes to be incurred if such earnings to be taxable ifwere remitted.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Unrecognized tax benefits
A reconciliation of the beginning and ending liability for unrecognized tax benefits that do not meet the more-likely-than-not threshold is as follows:
| | | | Year ended December 31, | | Year ended December 31, |
| | | 2020 | | 2019 | | 2023 | | 2022 |
| Beginning balance | Beginning balance | $ | 68,214 | | | $ | 40,382 | |
| Additions for tax positions related to current year | Additions for tax positions related to current year | 2,293 | | | 3,378 | |
| Additions for tax positions related to prior years | 258 | | | 24,722 | |
| Adjustments for tax positions related to prior years | |
| Reductions related to lapse of applicable statute | Reductions related to lapse of applicable statute | (133) | | | (268) | |
| Reductions related to settlements with taxing authorities | Reductions related to settlements with taxing authorities | (430) | | | 0 | |
| Ending balance | Ending balance | $ | 70,202 | | | $ | 68,214 | |
As of December 31, 2020,2023, the Company’s total liability for unrecognized tax benefits relating to tax positions that do not meet the more-likely-than-not threshold is $70,202, of which $66,607$47,379. Of this balance, $31,299 would impact the Company’s effective tax rate if recognized. This balance represents an increase of $1,988 from the December 31, 2019 balance of $68,214.
The Company recognizes accrued interest and penalties related to unrecognized tax benefits in its income tax expense. We recognized a benefit of $138 and an expense of $10,459 related to interest and penalties net of federal tax benefit within tax expense in 2023 and 2022, respectively. At December 31, 20202023 and 2019,December 31, 2022, the Company had approximately $17,864$6,525 and $14,428,$8,208, respectively, accrued for interest and penalties related to unrecognized tax benefits, net of federal tax benefit.
The Company and its subsidiaries are under examination in various state, local and foreign tax jurisdictions. In June 2023 we closed our audit with the IRS for the years 2016 and 2017. In 2022, the Company was able to reach a settlement with the IRS for tax years 2014-2015. Subsequent to the settlement, the Company filed a 2014 refund claim with respect to a contested issue that was included in the IRS examination. During 2023 the IRS denied the refund claim and the Company has until September 2025 to appeal. Except for the 2014 refund claim, the Company is no longer subject to U.S. federal examinations prior to 2020.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
The Company and its subsidiaries file U.S. federal and state income tax returns and various foreign income tax returns. The Company is no longer subject to U.S. federal and state examinations by tax authorities for years before 2014 and 2009, respectively. In addition to being under audit in various state and local tax jurisdictions, the Company’s federal tax returns are under audit by the Internal Revenue Service for the years 2014-2017.
13.12. Long-term debt
Long-term debt was comprised of the following:
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | December 31, | | | | As of December 31, 2020 |
| | 2020 | | 2019 | | Maturity date | | Interest rate | | Estimated fair value(1) |
| Senior Secured Credit Facilities: | | | | | | | | | |
| Term Loan A | $ | 1,684,375 | | | $ | 1,739,063 | | | 8/12/2024 | | LIBOR + 1.50% | | $ | 1,675,953 | |
| Term Loan B-1 | 2,715,694 | | | 0 | | | 8/12/2026 | | LIBOR + 1.75% | | 2,702,115 | |
| Term Loan B | 0 | | | 2,743,125 | | | 8/12/2026 | | | | |
Revolving line of credit(2) | 75,000 | | | 0 | | | 8/12/2024 | | ABR + 0.50% | | $ | 75,000 | |
| Senior Notes: | | | | | | | | | |
| 4.625% Senior Notes | 1,750,000 | | | 0 | | | 6/1/2030 | | 4.625 | % | | $ | 1,859,375 | |
| 3.75% Senior Notes | 1,500,000 | | | 0 | | | 2/15/2031 | | 3.75 | % | | $ | 1,522,500 | |
| 5.125% Senior Notes | 0 | | | 1,750,000 | | | 7/15/2024 | | | | |
| 5.0% Senior Notes | 0 | | | 1,500,000 | | | 5/1/2025 | | | | |
Acquisition obligations and other notes payable(3) | 164,160 | | | 180,352 | | | 2021-2036 | | 4.88 | % | | $ | 164,160 | |
Financing lease obligations(4) | 274,292 | | | 268,534 | | | 2021-2038 | | 5.1 | % | | |
| Total debt principal outstanding | 8,163,521 | | | 8,181,074 | | | | | | | |
Discount and deferred financing costs(5) | (77,717) | | | (72,840) | | | | | | | |
| | 8,085,804 | | | 8,108,234 | | | | | | | |
| Less current portion | (168,541) | | | (130,708) | | | | | | | |
| | $ | 7,917,263 | | | $ | 7,977,526 | | | | | | | |
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | December 31, | | | | As of December 31, 2023 |
| | 2023 | | 2022 | | Maturity date | | Interest rate | | Estimated fair value(1) |
| Senior Secured Credit Facilities: | | | | | | | | | |
| Term Loan A-1 | $ | 1,234,375 | | | $ | | (2) | | SOFR+CSA+1.75% | | $ | 1,209,688 | |
| Term Loan B-1 | 2,603,786 | | | 2,660,831 | | | 8/12/2026 | | SOFR+CSA+1.75% | | $ | 2,600,531 | |
| New Revolving line of credit | — | | | | | (2) | | SOFR+CSA+1.75% | | $ | — | |
| Prior Term Loan A | — | | | 1,498,438 | | | 8/12/2024 | | (3) | | |
| Prior Revolving line of credit | — | | | 165,000 | | | 8/12/2024 | | (3) | | |
| Senior Notes: | | | | | | | | | |
| 4.625% Senior Notes | 2,750,000 | | | 2,750,000 | | | 6/1/2030 | | 4.625 | % | | $ | 2,416,563 | |
| 3.75% Senior Notes | 1,500,000 | | | 1,500,000 | | | 2/15/2031 | | 3.75 | % | | $ | 1,235,625 | |
Acquisition obligations and other notes payable(4) | 102,328 | | | 120,562 | | | 2024-2036 | | 6.69 | % | | $ | 102,328 | |
Financing lease obligations(5) | 255,491 | | | 273,688 | | | 2024-2038 | | 4.58 | % | | |
| Total debt principal outstanding | 8,445,980 | | | 8,968,519 | | | | | | | |
Discount, premium and deferred financing costs(6) | (54,347) | | | (44,498) | | | | | | | |
| | 8,391,633 | | | 8,924,021 | | | | | | | |
| Less current portion | (123,299) | | | (231,404) | | | | | | | |
| | $ | 8,268,334 | | | $ | 8,692,617 | | | | | | | |
(1)For the Company's senior secured credit facilities, and senior notes, fair value estimates are based upon bid and ask quotes, typically a level 2 input. For our senior notes, fair value estimates are based on market level 1 inputs. For acquisition obligations and other notes payable, the carrying values presented here approximate their estimated fair values, based on estimates of their present values typically using level 2 interest rate inputs.
(2)The Company'sOutstanding Term Loan A-1 and the new Revolving line of credit balances are due on April 28, 2028, unless any of Term Loan B-1 remains outstanding 91 days prior to the Term Loan B-1 maturity date, in which case the outstanding Term Loan A-1 and the new Revolving line of credit balances become due at that 91 day date (May 13, 2026).
(3)At March 31, 2023, the interest rate on the Company's then-existing credit facilities was LIBOR plus an interest rate margin in effect of 1.75% for itsthe prior Term Loan A and prior revolving line of credit as of December 31, 2020 was based on an Alternate Base Rate (ABR or Prime Rate) plus 0.50%, or 3.75%. Effective January 6, 2021 this was converted to a LIBOR-based rate of LIBOR plus 1.50%.credit.
(3)(4)The interest rate presented for acquisition obligations and other notes payable is their weighted average interest rate based on the current fixed and LIBORvariable interest rate components in effect as of December 31, 2020.2023.
(4)(5)Financing lease obligations are measured at their approximate present values at inception. The interest rate presented is the weighted average discount rate embedded in financing leases outstanding. The term of one ground lease runs to 2070, in addition to the other lease maturity dates presented in the table above.
(5)(6)As of December 31, 2020,2023, the carrying amount of the Company's senior secured credit facilities includeshave been reduced by a discount of $5,461$2,487 and deferred financing costs of $35,825$32,498 and the carrying amount of the Company's senior notes includeshave been reduced by deferred financing costs of $36,431.$31,491 and increased by a debt premium of $12,129. As of December 31, 2019,2022, the carrying amount of the Company's senior secured credit facilities includedwas reduced by a discount of $6,457$3,497 and deferred financing costs of $45,444,$18,816, and the carrying amountamounts of the Company's senior notes includedwere reduced by deferred financing costs of $20,939.$36,203 and increased by a debt premium of $14,018.
| | | | | |
| 2024 | $ | 123,299 | |
| 2025 | $ | 132,878 | |
| 2026 | $ | 2,663,669 | |
| 2027 | $ | 116,712 | |
| 2028 | $ | 1,017,856 | |
| Thereafter | $ | 4,391,566 | |
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Scheduled maturities of long-term debt at December 31, 2020 were as follows:
| | | | | |
| 2021 | $ | 168,541 | |
| 2022 | $ | 169,782 | |
| 2023 | $ | 227,062 | |
| 2024 | $ | 1,496,892 | |
| 2025 | $ | 69,440 | |
| Thereafter | $ | 6,031,804 | |
On February 13, 2020,April 3, 2023, the Company entered into an amendmentthe Second Amendment (the RepricingSecond Amendment) to refinance and reprice its senior secured Term Loan B with a senior securedcredit agreement (the Credit Agreement). The Second Amendment modifies the Credit Agreement to, among other things, transition the interest pricing on Term Loan B-1 that bears interest atfrom LIBOR + 1.75% to a forward-looking term rate equal to LIBOR(Term SOFR) based on the Secured Overnight Financing Rate (SOFR) +1.75% plus an applicable margin of 1.75% and matures on August 12, 2026. The Repricing Amendment did not changeadditional credit spread adjustment (CSA), provided that this adjusted rate shall never be less than 0.00%, as well as to update the successor interest rate onprovisions in the Credit Agreement with respect to Term Loan A orB-1. As of December 31, 2023, the revolving line of credit. NaN additional debt was incurred, nor any additional proceeds received, by the Company in connection with the Repricing Amendment. The majority ofCSA for all tranches outstanding on the Company's Term Loan B debtB-1 was considered modified0.11%. The Company adopted Accounting Standards Update (ASU) No. 2020-04 and ASU No. 2022-06 regarding reference rate reform during the second quarter and applied one of their practical expedients to treat the amendment of Term Loan B-1 as a non-substantial modification.
On April 28, 2023, the Company entered into the Third Amendment (the Third Amendment, and together with the Second Amendment, the Amendments) to the Credit Agreement. The Third Amendment modifies the Credit Agreement to, among other things, refinance its Term Loan A and revolving line of credit with a secured Term Loan A-1 facility in the aggregate principal amount of $1,250,000 and a secured revolving line of credit in the aggregate principal amount of up to $1,500,000 (the foregoing referred to as the new Term Loan A-1 and new revolving line of credit, respectively).
The new Term Loan A-1 and new revolving line of credit initially bore interest at Term SOFR, plus a CSA of 0.10% and an interest rate margin of 2.00%, which was subject to adjustment depending upon the Company's leverage ratio under the Credit Agreement, as amended, and which can range from 1.25% to 2.25%, provided that this transaction. adjusted rate shall never be less than 0.00%. The new Term Loan A-1 requires amortizing quarterly principal payments that began on September 30, 2023 of $7,813 per quarter for the first four payments, $15,625 per quarter for the fifth through sixteenth payments, $23,438 per quarter for the seventeenth through nineteenth payments, with the balance due on April 28, 2028. The new revolving line of credit has a five-year term. However, under the Third Amendment, Term Loan A-1 and the new revolving line of credit become due if any of Term Loan B-1 remains outstanding 91 days prior to the Term Loan B-1 maturity date, in which case the Term Loan A-1 balance and any outstanding balance on the new revolving line of credit become due at that 91 day date (May 13, 2026).
Borrowings under the Company's senior secured credit facilities are guaranteed and secured by substantially all of DaVita Inc.'s and certain of the Company’s domestic subsidiaries' assets and rank senior to all unsecured indebtedness. Borrowings under the new Term Loan A-1, Term Loan B-1 and new revolving line of credit rank equal in priority for that security and related subsidiary guarantees under the facility's terms. The Credit Agreement, as amended, contains certain customary affirmative and negative covenants such as various restrictions or limitations on permitted amounts of investments (including acquisitions), share repurchases, payment of dividends, and redemptions and incurrence of other indebtedness. Many of these restrictions and limitations will not apply as long as the Company’s leverage ratio calculated in accordance with the Amendments is below 4.00:1.00. In addition, the Amendments require compliance with a maximum leverage ratio covenant, tested quarterly, of 5.00:1.00 through June 30, 2026 and 4.50:1.00 thereafter.
In the second quarter of 2023, the Company used a portion of the proceeds from the new Term Loan A-1 and initial borrowing of $400,000 on the new revolving line of credit to pay off the remaining principal balance outstanding and accrued interest and fees on its prior Term Loan A and prior revolving line of credit in the amount of $1,602,199. The remaining borrowings added cash to the balance sheet for general corporate purposes.
In addition to the prepayments described above, during 2023, the Company made regularly scheduled and other principal payments under its senior secured credit facilities totaling $54,010 on its prior Term Loan A, $15,625 on Term Loan A-1 and $57,046 on Term Loan B-1.
As a result of the transactions described above, the Company recognized debt prepayment and refinancing charges of $2,948$7,962 in the year ended December 31, 2020 comprisedsecond quarter of 2023 composed partially of fees incurred on this transactionfor these transactions and partially of deferred financing costs written off for the portion of debt considered extinguished and reborrowed.reborrowed as a result of the repayment of all principal balances outstanding on the Company's prior Term Loan A and prior revolving line of credit. For the portion of the Term Loan B debt that was considered extinguished and reborrowed, in this refinancing, the Company recognized $68,842 in constructive financing cash outflows and financing cash inflows on the statement of cash flows of $434,393 and $150,000 for the Term Loan A and prior revolving line of credit, respectively, even though no funds were actually paid or received. Another $55,895$715,019 of the debt considered extinguished in this refinancing represented a non-cash financing activity.
During the year endedAs of December 31, 2020,2023, the Company made regularly scheduled mandatory principal paymentshad undrawn capacity on the revolving line of credit under its senior secured credit facilities totaling $54,688 on Term Loan A and $27,431 on Term Loan B-1.
On June 9, 2020,of $1,500,000. Credit available under this revolving line of credit is reduced by the Company issued $1,750,000 aggregate principal amount of 4.625% senior notes due 2030 (the 4.625% Senior Notes) in a private offering pursuant to Rule 144A and Regulation S under the Securities Actany letters of 1933, as amended. The 4.625% Senior Notes pay interest on June 1 and December 1 of each year beginning December 1, 2020. The 4.625% Senior Notes are unsecured senior obligations and rank equally in right of payment with the Company's existing and future unsecured senior indebtedness. The 4.625% Senior Notes are guaranteed by each of the Company’s domestic subsidiaries that guarantee its senior secured credit facilities. The Company may redeem up to 40% of the aggregate principal amount of the 4.625% Senior Notes at any time prior to June 1, 2023 at 104.625% of the aggregate principal amount from the proceeds of one or more equity offerings, plus accrued and unpaid interest. In addition, the Company may redeem the 4.625% Senior Notes at any time prior to June 1, 2025 at a make-whole redemption price plus accrued and unpaid interest or, on and after such date, at certain redemption prices specified in the indenture governing these notes plus accrued and unpaid interest. The 4.625% Senior Notes contain restrictive covenants that limit the ability of the Company and its guarantors to, among other things, create certain liens, enter into certain sale/leaseback transactions, or merge, consolidate or sell all or substantially all of their assets. The 4.625% Senior Notes and related subsidiary guarantees do not have any registration or similar rights and are not expected to be registered for exchange on public markets. During the year ended December 31, 2020, the Company incurred $20,386 in fees, discounts and other professional expenses associated with this transaction that were capitalized and will amortize over the term of the 4.625% Senior Notes.
On July 15, 2020, the Company used the net proceeds from these 4.625% Senior Notes, together with cash on hand, to redeem in full all $1,750,000 aggregate principal amount outstanding of its 5.125% Senior Notes plus accrued interest and redemption premium. The Company incurred debt redemption premium charges of $29,890 and deferred financing cost write-offs of $9,764 in connection with this redemption.
On August 11, 2020, the Company issued $1,500,000 aggregate principal amount of 3.75% senior notes due 2031 (the 3.75% Senior Notes) in a private offering pursuant to Rule 144A and Regulation S under the Securities Act of 1933, as amended. The 3.75% Senior Notes pay interest on February 15 and August 15 of each year beginning February 15, 2021. The 3.75% Senior Notes are unsecured senior obligations and rank equally in right of payment with the Company's existing and future unsecured senior indebtedness. The 3.75% Senior Notes are guaranteed by each of the Company’s domestic subsidiaries that guarantee its senior secured credit facilities. The Company may redeem up to 40% of the aggregate principal amount of the 3.75% Senior Notes at any time prior to August 15, 2023 at 103.75% of the aggregate principal amount from the proceeds of one or more equity offerings, plus accrued and unpaid interest. In addition, the Company may redeem the 3.75% Senior Notes at any time prior to February 15, 2026 at a make-whole redemption price plus accrued and unpaid interest or, on and after such date, at certain redemption prices specified in the indenture governing these notes plus accrued and unpaid interest. The 3.75% Senior Notes contain restrictive covenants that limit the ability of the Company and its guarantors to, among other things, create
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
certain liens, enter into certain sale/leaseback transactions, or merge, consolidate or sell all or substantially allcredit outstanding thereunder, of their assets. The 3.75% Senior Notes and related subsidiary guarantees do not have any registration or similar rights and are not expected to be registered for exchange on public markets. During the year endedwhich there were none as of December 31, 2020, the Company incurred $17,936 in fees, discounts and other professional expenses associated with this transaction that were capitalized and will amortize over the term of the 3.75% Senior Notes.
On August 21, 2020, the Company used the net proceeds from these 3.75% Senior Notes, together with cash on hand, to redeem in full all $1,500,000 aggregate principal amount outstanding of its 5.0% Senior Notes plus accrued interest and redemption premium.2023. The Company incurred debt redemption premium chargesalso had letters of $37,500 and deferred financing cost write-offscredit of $8,866 in connection with this redemption.approximately $151,403 outstanding under a separate bilateral secured letter of credit facility as of December 31, 2023.
TheAs of December 31, 2023, the Company's 20152019 interest rate cap agreements expired on June 30, 2020, at which time the Company's 2019 cap agreements became effective. As of December 31, 2020, the Company maintains several interest rate cap agreements that havedescribed below had the economic effect of capping the Company's maximum exposure to LIBORSOFR variable interest rate changes on specific portionsequivalent amounts of the Company's floating rate debt, including all of the Term Loan B-1 and a portion of the Term Loan A.A-1. The remaining $900,069$338,161 outstanding principal balance of the Term Loan A and the $75,000 outstanding balance of the revolving line of credit areA-1 is subject to LIBOR-basedSOFR-based interest rate volatility. TheThese cap agreements are designated as cash flow hedges and, as a result, changes in their fair values are reported in other comprehensive income. The amortization oforiginal premiums paid for the original cap premium is recognized as a component ofcaps are amortized to debt expense on the interest methoda straight-line basis over the termsterm of theeach cap agreements.agreement starting from its effective date. These cap agreements do not contain credit risk-contingent features.
Senior Notes
The Senior Notes are unsecured obligations, rank equally in right of payment with the Company’s existing and future unsecured senior indebtedness and require semi-annual interest payments. The Company may redeem some or all of the Senior Notes at any time on or after certain specific dates and at certain specific redemption prices as outlined in each senior note agreement. Interest rates on the Senior Notes are fixed by their terms.
Interest rate cap agreements
During 2023 the Company entered into several forward interest rate cap agreements, described below, that have the economic effect of capping the Company's exposure to SOFR variable interest rate changes on specific portions of the Company's floating rate debt (2023 cap agreements). These 2023 cap agreements are designated as cash flow hedges and, as a result, changes in their fair values will be reported in other comprehensive income. These 2023 cap agreements have notional amounts that amortize downward over time, do not contain credit-risk contingent features.features, and become effective and expire as described in the table below.
Additionally, during and as of the end of the second quarter of 2023, the Company transitioned the variable rate base on its senior secured credit facilities and related hedging interest rate caps from LIBOR to SOFR. This transition involved a SOFR-to-LIBOR rate mismatch between this debt and the 2019 interest rate caps for a portion of the second quarter of 2023, but the Company’s interest rate hedges remained highly effective throughout the transition and thereafter.
This transition was accomplished through the Amendments to the Credit Agreement for the Company's senior secured credit facility debt and, for the Company's 2019 interest rate caps outstanding, through the International Swaps and Derivatives Association (ISDA)'s Interbank Offered Rate (IBOR) Fallbacks Supplement and IBOR Fallbacks Protocol which were established in anticipation of the cessation of LIBOR. That ISDA protocol incorporated fallbacks for derivatives linked to LIBOR which facilitated their transition to a replacement reference rate. The Company has adhered to this ISDA protocol and as of June 30, 2023 transitioned all of its LIBOR-based derivative exposure to SOFR.
The following table summarizes the Company’s interest rate cap agreements outstanding as of December 31, 2020 and December 31,2023:
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | | | | | | | Notional reduction or contractual maturity date
At December 31 unless noted |
| Year cap agreements executed | | Notional amount | | SOFR maximum rate | | Approximate effective date | |
| | | | 2024(1) | | 2025 | | 2026 |
| 2019 | | $ | 3,500,000 | | | 2.00% | | 6/30/2020 | | $ | 3,500,000 | | | | | |
| 2023 | | $ | 1,000,000 | | | 3.75% | | 6/30/2024 | | $ | 500,000 | | | $ | 500,000 | | | |
| 2023 | | $ | 1,000,000 | | | 4.00%(2) | | 6/30/2024 | | $ | 250,000 | | | $ | 750,000 | | | |
| 2023 | | $ | 1,000,000 | | | 4.75%(3) | | 6/30/2024 | | $ | 250,000 | | | $ | 750,000 | | | |
| 2023 | | $ | 500,000 | | | 5.00%(4) | | 6/30/2024 | | | | | | $ | 500,000 | |
| 2023 | | $ | 250,000 | | | 4.50% | | 12/31/2024 | | | | $ | 250,000 | | | |
| 2023 | | $ | 750,000 | | | 4.00% | | 12/31/2024 | | | | $ | 250,000 | | | $ | 500,000 | |
(1)The Company's 2019 which are classified in "Other long-term assets"cap agreements mature on its consolidated balance sheet:June 30, 2024.
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | | | | | | | | Year ended | | December 31, |
| | | | | | | | | December 31, 2020 | | 2020 | | 2019 |
| | Notional amount | | LIBOR maximum rate | | Effective date | | Expiration date | | Debt expense | | Recorded OCI loss | | Fair value |
| 2019 cap agreements | $ | 3,500,000 | | | 2.00% | | 6/30/2020 | | 6/30/2024 | | $ | 2,755 | | | $ | (21,781) | | | $ | 2,671 | | | $ | 24,452 | |
| 2015 cap agreements | $ | 3,500,000 | | | 3.50% | | 6/29/2018 | | 6/30/2020 | | $ | 4,326 | | | $ | 0 | | | $ | 0 | | | $ | 0 | |
The following table summarizes(2)Effective January 1, 2025, the effectsmaximum rate of the Company’s4.00% decreases to 3.75% for these interest rate cap agreementscaps.
(3)Effective January 1, 2025, the maximum rate of 4.75% decreases to 4.00% for the years ended December 31, 2020, 2019 and 2018:
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | | Amount of unrealized (losses) gains in OCI on interest rate cap agreements | | Location of losses | | Reclassification from accumulated other comprehensive income into net income |
| | | Year ended December 31, | | | Year ended December 31, |
| Derivatives designated as cash flow hedges | | 2020 | | 2019 | | 2018 | | | 2020 | | 2019 | | 2018 |
| Interest rate cap agreements | | $ | (21,781) | | | $ | 1,566 | | | $ | (181) | | | Debt expense | | $ | 7,081 | | | $ | 8,591 | | | $ | 8,466 | |
| Related income tax | | 5,435 | | | (415) | | | 48 | | | Related income tax | | (1,768) | | | (2,214) | | | (2,180) | |
| Total | | $ | (16,346) | | | $ | 1,151 | | | $ | (133) | | | | | $ | 5,313 | | | $ | 6,377 | | | $ | 6,286 | |
See Note 20 for further details on amounts recorded and reclassified from accumulated other comprehensive (loss) income.
The Company’s weighted average effectivethese interest rate on its senior secured credit facilities atcaps.
(4)Effective January 1, 2025, the endmaximum rate of 2020 was 2.03%, based upon the current margins in effect5.00% decreases to 4.50% for the Term Loan A, Term Loan B-1 and revolving line of credit as of December 31, 2020.
The Company’s weighted average effectivethese interest rate on all debt, including the effect of interest rate caps and amortization of debt discount, was 3.59% for the year ended December 31, 2020 and 3.06% as of December 31, 2020.
As of December 31, 2020, the Company’s interest rates were fixed on approximately 44.4% of its total debt.
As of December 31, 2020, the Company had $925,000 available and $75,000 drawn on its $1,000,000 revolving line of credit under its senior secured credit facilities. Credit available under this revolver is reduced by the amount of any letters of credit outstanding under this facility, but there were no such letters of credit outstanding as of December 31, 2020. Thecaps.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Company also had approximately $64,636The following table summarizes the effects of outstanding lettersthe Company’s interest rate cap agreements for the years ended December 31, 2023, 2022 and 2021:
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | | Amount of unrealized gains (losses) in OCI on interest rate cap agreements | | Location in Consolidated Statements of Income | | Reclassification from accumulated other comprehensive income into net income |
| | | Year ended December 31, | | | Year ended December 31, |
| Derivatives designated as cash flow hedges | | 2023 | | 2022 | | 2021 | | | 2023 | | 2022 | | 2021 |
| Interest rate cap agreements | | $ | 9,186 | | | $ | 144,793 | | | $ | 9,532 | | | Debt expense | | $ | (103,567) | | | $ | (11,732) | | | $ | 5,509 | |
| Related income tax | | (2,291) | | | (36,124) | | | (2,377) | | | Related income tax | | 25,840 | | | 2,926 | | | (1,376) | |
| Total | | $ | 6,895 | | | $ | 108,669 | | | $ | 7,155 | | | | | $ | (77,727) | | | $ | (8,806) | | | $ | 4,133 | |
The fair value of the Company's interest rate cap agreements, which are classified in other long-term assets on its consolidated balance sheet, were $79,805 and $139,755 for the years ended December 31, 2023 and December 31, 2022, respectively.
See Note 19 for further details on amounts recorded and reclassified from accumulated other comprehensive (loss) income and recorded as debt expense (offset) related to the Company’s interest rate cap agreements for the year ended December 31, 2023.
As a result of the variable rate cap from the Company's 2019 interest rate cap agreements, the Company’s weighted average effective interest rate on its senior secured credit under a separate bilateralfacilities at the end of December 31, 2023 was 4.39%, based on the current margins in effect for its senior secured letter of credit facilityfacilities as of December 31, 2020.2023, as detailed in the table above.
The Company’s weighted average effective interest rate on all debt, including the effect of interest rate caps and amortization of debt discount, was 4.52% for the year ended December 31, 2023 and 4.42% as of December 31, 2023.
As of December 31, 2023, the Company’s interest rates were fixed and economically fixed on approximately 54% and 96% of its total debt, respectively.
Debt expense
Debt expense consisted of interest expense of $282,932, $419,639$373,951, $339,247 and $461,897$267,049 and the amortization and accretion of debt discounts and premiums, amortization of deferred financing costs, costs for the undrawn portion of the revolving line of credit and the amortization of interest rate cap agreements of $21,179, $24,185$24,600, $17,772 and $25,538$18,205 for 2020, 20192023, 2022 and 2018,2021, respectively. These interest expense amounts are net of capitalized interest.
14.13. Leases
The Company leases substantially all of its U.S. dialysis facilities. The majority of the Company’s facilities are leased under non-cancellable operating leases which range in terms from five years to 2015 years and which contain renewal options of five years to ten years at the fair rental value at the time of renewal. Certain of theThe Company's leases are generally subject to periodicfixed escalation clauses or contain consumer price increases or contain fixed escalation clauses.index increases. See Note 1 for further information on how the Company accounts for leases.
As of December 31, 20202023 and December 31, 2019,2022, assets recorded under finance leases were $275,389$322,844 and $247,246,$319,546, respectively, and accumulated amortization associated with finance leases was $49,345$122,286 and $27,193,$101,361, respectively, included in property and equipment, net, on the Company's consolidated balance sheet.
In certain markets, the Company acquires and develops dialysis centers. Upon completion, the Company sells the center to a third party and leases the space back with the intent of operating the center on a long termlong-term basis. Both the sale and leaseback terms are generally market terms. TheSubstantially all of the lease terms are consistent with the Company's other operating leases with the majority of the leases under non-cancellable operating leases ranging in terms from fiveten years to 2015 years and which containcontaining renewal options of five years to ten years at the fair rental value at the time of renewal.
The Company adopted Topic 842, Leases beginning on January 1, 2019 through a modified retrospective approach for leases existing at the adoption date with a cumulative effect adjustment. Consequently, financial information was not updated for dates and periods before January 1, 2019.
The components of lease expense were as follows:
| | | | | | | | | | | | | | |
| | Year ended December 31, |
| Lease cost | | 2020 | | 2019 |
Operating lease cost(1): | | | | |
| Fixed lease expense | | $ | 541,090 | | | $ | 526,352 | |
| Variable lease expense | | 122,729 | | | 119,740 | |
| Financing lease cost: | | | | |
| Amortization of leased assets | | 24,720 | | | 23,724 | |
| Interest on lease liabilities | | 14,421 | | | 14,932 | |
| Net lease cost | | $ | 702,960 | | | $ | 684,748 | |
(1) Includes short-term lease expense and sublease income, which are immaterial.
Other information related to leases was as follows:
| | | | | | | | | | | | | | |
| | Year ended December 31, |
| Lease term and discount rate | | 2020 | | 2019 |
| Weighted average remaining lease term (years): | | | | |
| Operating leases | | 8.7 | | 9.0 |
| Finance leases | | 10.5 | | 10.2 |
| Weighted average discount rate: | | | | |
| Operating leases | | 3.8 | % | | 4.1 | % |
| Finance leases | | 5.1 | % | | 5.4 | % |
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
| | | | | | | | | | | | | | |
| | Year ended December 31, |
| Other information | | 2020 | | 2019 |
| Gains on sale leasebacks, net | | $ | 34,301 | | | $ | 20,833 | |
Cash paid for amounts included in the
measurement of lease liabilities: | | | | |
| Operating cash flows for operating leases | | $ | 661,318 | | | $ | 637,655 | |
| Operating cash flows for finance leases | | $ | 20,981 | | | $ | 22,257 | |
| Financing cash flows for finance leases | | $ | 24,780 | | | $ | 25,692 | |
Net operating lease assets obtained in exchange
for new or modified operating lease liabilities | | $ | 401,559 | | | $ | 432,074 | |
| | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| Lease cost | | 2023 | | 2022 | | 2021 |
Operating lease cost(1): | | | | | | |
| Fixed lease expense | | $ | 556,844 | | | $ | 552,194 | | | $ | 547,923 | |
| Variable lease expense | | 135,990 | | | 127,621 | | | 125,981 | |
| Financing lease cost: | | | | | | |
| Amortization of leased assets | | 26,964 | | | 27,079 | | | 26,846 | |
| Interest on lease liabilities | | 11,724 | | | 12,776 | | | 13,988 | |
| Net lease cost | | $ | 731,522 | | | $ | 719,670 | | | $ | 714,738 | |
(1) Includes short-term lease expense and sublease income, which are immaterial.
Other information related to leases was as follows:
| | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| Lease term and discount rate | | 2023 | | 2022 | | 2021 |
| Weighted average remaining lease term (years): | | | | | | |
| Operating leases | | 7.6 | | 8.2 | | 8.3 |
| Finance leases | | 8.5 | | 9.4 | | 10.5 |
| Weighted average discount rate: | | | | | | |
| Operating leases | | 4.0 | % | | 3.6 | % | | 3.5 | % |
| Finance leases | | 4.6 | % | | 4.5 | % | | 4.5 | % |
| | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| Other information | | 2023 | | 2022 | | 2021 |
| Gains on sale leasebacks, net | | $ | 3,387 | | | $ | 28,005 | | | $ | 17,137 | |
Cash paid for amounts included in the
measurement of lease liabilities: | | | | | | |
| Operating cash flows for operating leases | | $ | 708,162 | | | $ | 696,291 | | | $ | 684,186 | |
| Operating cash flows for finance leases | | $ | 19,246 | | | $ | 20,103 | | | $ | 21,343 | |
| Financing cash flows for finance leases | | $ | 26,455 | | | $ | 24,329 | | | $ | 22,445 | |
Net operating lease assets obtained in exchange
for new or modified operating lease liabilities | | $ | 269,564 | | | $ | 278,108 | | | $ | 361,101 | |
Future minimum lease payments under non-cancellable leases as of December 31, 20202023 are as follows:
| | | | | Operating leases | | Finance leases | | | Operating leases | | Finance leases |
| 2021 | | $ | 480,439 | | | $ | 35,039 | |
| 2022 | | 504,789 | | | 35,124 | |
| 2023 | | 464,023 | | | 35,645 | |
| 2024 | 2024 | | 412,419 | | | 35,669 | |
| 2025 | 2025 | | 361,447 | | | 35,539 | |
| 2026 | |
| 2027 | |
| 2028 | |
| Thereafter | Thereafter | | 1,437,965 | | | 174,907 | |
| Total future minimum lease payments | Total future minimum lease payments | | 3,661,082 | | | 351,923 | |
| Less portion representing interest | Less portion representing interest | | (552,915) | | | (77,631) | |
| Present value of lease liabilities | Present value of lease liabilities | | $ | 3,108,167 | | | $ | 274,292 | |
Rent expense under all operating leases for 2020, 2019,2023, 2022 and 20182021 was $663,819, $646,092$692,834, $679,815 and $596,117,$673,904, respectively. Rent expense is recorded on a straight-line basis over the term of the lease, including leases that contain fixed escalation clauses or include abatement provisions. Leasehold improvement incentives reduce the carrying value of right-of-use assets and are deferred and amortized to rent expense over the term of the lease. Finance lease obligations are included in long-term debt. See Note 1312 for further details on long-term debt.
15.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
14. Employee benefit plans
The Company has a 401(k) retirement savings plan for substantially all of its U.S. employees which has been established pursuant to applicable provisions of the Internal Revenue Code (IRC). The plan allows for employees to contribute a percentage of their base annual salaries on a tax-deferred basis not to exceed IRC limitations. The Company maintains a 401(k) matching program under which the Company matches 50% of the employee's contribution up to 6% of the employee's salary, subject to certain limitations. The matching contributions are subject to certain eligibility and vesting conditions. For the years ended December 31, 2020, 20192023, 2022 and 2018,2021, the Company accrued matching contributions totaling approximately $70,180, $64,988$73,725, $70,084 and $67,807,$68,658, respectively. Prior to 2018, the Company did not provide matching contributions for its 401(k) savings plan.
The Company also maintains a voluntary compensation deferral plan, the Deferred Compensation Plan, as well as other legacy deferral plans.Plan. The Deferred Compensation Plan is non-qualified and permits certain employees whose annualized base salary equals or exceeds a minimum annual threshold amount as set by the Company to elect to defer all or a portion of their annual bonus payment and up to 50% of their base salary into a deferral account maintained by the Company. Total contributions to this plan in 2020, 20192023, 2022 and 20182021 were $3,637, $1,751$2,695, $3,573 and $3,090,$2,962, respectively. Deferred amounts are generally paid out in cash at the participant’s election either in the first or second year following retirement or in a specified future period at least three to four years after the deferral election was effective. During 2020, 20192023, 2022 and 20182021 the Company distributed $3,139, $2,730$3,899, $3,731 and $4,652,$11,887, respectively, to participants from its deferred compensation plans. Participants are credited with their proportional amount of annual earnings from the plans. The assets of these plans are held in rabbi trusts subject to the claims of the Company’s general creditors in the event of its bankruptcy. As of December 31, 20202023 and 2019,2022, the total fair value of assets held in these plans' trusts was $43,844$36,936 and $39,527,$32,944, respectively. The assets of these plans are recorded at fair value with changes in fair value recorded in "Otherother (loss) income, net".net. See Note 4 for further details. Any fair value changes to the corresponding liability balance are recorded as compensation expense. See Note 5 for further details.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
16.15. Contingencies
The majority of the Company’s revenues are from government programs and may be subject to adjustment as a result of: (i) examination by government agencies or contractors, for which the resolution of any matters raised may take extended periods of time to finalize; (ii) differing interpretations of government regulations by different Medicare contractors or regulatory authorities; (iii) differing opinions regarding a patient’s medical diagnosis or the medical necessity of services provided; and (iv) retroactive applications or interpretations of governmental requirements. In addition, the Company’s revenues from commercial payors may be subject to adjustment as a result of potential claims for refunds, as a result of government actions or as a result of other claims by commercial payors.
The Company operates in a highly regulated industry and is a party to various lawsuits, demands, claims, qui tam suits, governmental investigations (which frequently arise from qui tam suits) and audits (including, without limitation, investigations or other actions resulting from its obligation to self-report suspected violations of law) and other legal proceedings, including, without limitation, those described below. The Company records accruals for certain legal proceedings and regulatory matters to the extent that the Company determines an unfavorable outcome is probable and the amount of the loss can be reasonably estimated. AsExcluding amounts stated below, as of December 31, 20202023 and December 31, 2019,2022, the Company’s total recorded accruals with respect to legal proceedings and regulatory matters, net of anticipated third party recoveries, were immaterial. While these accruals reflect the Company’s best estimate of the probable loss for those matters as of the dates of those accruals, the recorded amounts may differ materially from the actual amount of the losses for those matters, and any anticipated third party recoveries for any such losses may not ultimately be recoverable. Additionally, in some cases, no estimate of the possible loss or range of loss in excess of amounts accrued, if any, can be made because of the inherently unpredictable nature of legal proceedings and regulatory matters, which also may be impacted by various factors, including, without limitation, that they may involve indeterminate claims for monetary damages or may involve fines, penalties or non-monetary remedies; present novel legal theories or legal uncertainties; involve disputed facts; represent a shift in regulatory policy; are in the early stages of the proceedings; or may result in a change of business practices. Further, there may be various levels of judicial review available to the Company in connection with any such proceeding.
The following is a description of certain lawsuits, claims, governmental investigations and audits and other legal proceedings to which the Company is subject.
Certain Governmental Inquiries and Related Proceedings
2016 U.S. Attorney Texas Investigation: In February 2016, DaVita Rx, LLC (DaVita Rx), a wholly-owned subsidiary of the Company, received a Civil Investigative Demand (CID) from the U.S. Attorney’s Office, Northern District of Texas. The government is conducting a federal False Claims Act (FCA) investigation concerning allegations that DaVita Rx presented or caused to be presented false claims for payment to the government for prescription medications, as well as an investigation into the Company’s relationships with pharmaceutical manufacturers. The government's investigation covers the period from January 1, 2006 through December 31, 2018. In December 2017, the Company finalized and executed a settlement agreement that resolved certain of the issues in the government's investigation and that included total monetary consideration of $63,700, as previously disclosed, of which $41,500 was an incremental cash payment and $22,200 was for amounts previously refunded, and all of which was previously accrued. The government’s investigation is ongoing with respect to issues related to DaVita Rx's historic relationships with certain pharmaceutical manufacturers, and in July 2018 the OIG served the Company with a subpoena seeking additional documents and information relating to those relationships. The Company is continuing to cooperate with the government in this investigation.
2017 U.S. Attorney Colorado Investigation: In November 2017, the U.S. Attorney’s Office, District of Colorado informed the Company of an investigation it was conducting into possible federal healthcare offenses involving DaVita Kidney Care, as well as several of the Company’s wholly-owned subsidiaries. In addition to DaVita Kidney Care, the matter currently
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
includes an investigation into DaVita Rx, DaVita Laboratory Services, Inc. (DaVita Labs), and RMS Lifeline Inc. (Lifeline). In each of August 2018, and May 2019, and July 2021, the Company received a CID pursuant to the FCA from the U.S. Attorney's Office relating to this investigation. In May 2020, the Company sold its interest in Lifeline, but the Company retained certain liabilities of the Lifeline business, including those related to this investigation. The Company is continuing to cooperateengaged in discussions with the government in this investigation.
2018 U.S. Attorney Florida Investigation: In March 2018, DaVita Labs received two CIDs from the U.S. Attorney’s Office, Middle District of Florida that were identical in nature but directed to the two different labs. According to the face of the CIDs, the U.S. Attorney’s Office is conducting an investigation as to whether the Company’s subsidiary submitted claims for blood, urine, and fecal testing, where there were insufficient test validation or stability studies to ensure accurate results, in violation of the FCA. In October 2018, DaVita Labs received a subpoena from the OIG in connection with this matter
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
requesting certain patient records linked to clinical laboratory tests. On September 30, 2019, the U.S. Attorney's Office notifiedand the U.S. District Court, Middle District of Florida, of its decision not to elect to intervene at this time in the matter of U.S. ex rel. Lorne Holland, et al. v. DaVita Healthcare Partners, Inc. et al. The court then unsealed the complaint, which alleges violationsCivil Division of the FCA, by order dated the same day. In January 2020, the private party relators served the Company and DaVita Labs with an amended complaint. On February 24, 2020, the Company and DaVita Labs filed a motionUnited States Department of Justice to dismiss the amended complaint. On June 25, 2020, the court denied the motion to dismiss.resolve this matter. The Company and DaVita Labs answeredcan make no assurance as to the complaint on July 23, 2020.final outcome. The Company and DaVita Labs dispute these allegations and intend to defendhas reserved $40 million for this action accordingly.matter, which includes any potential payment of attorneys' fees.
2020 U.S. Attorney New Jersey Investigation: In March 2020, the U.S. Attorney’s Office, District of New Jersey served the Company with a subpoena and a CID relating to an investigation being conducted by that office and the U.S. Attorney’s Office, Eastern District of Pennsylvania. The subpoena and CID request information on several topics, including certain of the Company’s joint venture arrangements with physicians and physician groups, medical director agreements, and compliance with its five-year Corporate Integrity Agreement, the term of which expired October 22, 2019. In November 2022, the Company learned that, on April 1, 2022, the U.S. Attorney’s Office for the District of New Jersey notified the U.S. District Court for the District of New Jersey of its decision not to elect to intervene in the matter of U.S. ex rel. Doe v. DaVita Inc. and filed a Stipulation of Dismissal. On April 13, 2022, the U.S. District Court for the District of New Jersey dismissed the case without prejudice. On October 12, 2022, the U.S. Attorney’s Office for the Eastern District of Pennsylvania notified the U.S. District Court, Eastern District of Pennsylvania, of its decision not to elect to intervene at this time in the matter of U.S. ex rel. Bayne v. DaVita Inc., et al.The court then unsealed an amended complaint, which alleges violations of federal and state False Claims Acts, by order dated October 14, 2022. On November 8, 2023, the private party relator filed a fourth amended complaint. On November 29, 2023, the Company is cooperating withfiled a motion to dismiss the government in this investigation.fourth amended complaint.
2020 California Department of Insurance Investigation: In April 2020, the California Department of Insurance (CDI) sent the Company an Investigative Subpoena relating to an investigation being conducted by that office. CDI issued a superseding subpoena in September 2020. The2020 and an additional subpoena as revised, requestsin September 2021. Those subpoenas request information on a number of topics, including but not limited to the Company’s communications with patients about insurance plans and financial assistance from the American Kidney Fund (AKF), analyses of the potential impact of patients’ decisions to change insurance providers, and documents relating to donations or contributions to the AKF. The Company is cooperatingcontinuing to cooperate with CDI in this investigation.
2020 Department2023 District of JusticeColumbia Office of Attorney General Investigation: In October 2020,January 2023, the Company receivedOffice of the Attorney General for the District of Columbia issued a CID fromto the Department of Justice pursuant to a False Claims Act investigation concerning allegations that DaVita Medical Group (DMG) may have submitted undocumented or unsupported diagnosis codesCompany in connection with Medicare Advantage beneficiaries.an antitrust investigation into the AKF. The CID covers the period from January 1, 2015 through June 19, 2019,2016 to the datepresent. The CID requests information on a number of topics, including but not limited to the Company completedCompany’s communications with AKF, documents relating to donations to the divestiture of DMG to Collaborative Care Holdings, LLC.AKF, and communications with patients, providers, and insurers regarding the AKF. The Company is cooperating with the government in this investigation.
* * *
Although the Company cannot predict whether or when proceedings might be initiated or when these matters may be resolved (other than as may be described above), it is not unusual for inquiries such as these to continue for a considerable period of time through the various phases of document and witness requests and on-goingongoing discussions with regulators and to develop over the course of time. In addition to the inquiries and proceedings specifically identified above, the Company frequently is subject to other inquiries by state or federal government agencies, many of which relate to qui tam complaints filed by relators. Negative findings or terms and conditions that the Company might agree to accept as part of a negotiated resolution of pending or future government inquiries or relator proceedings could result in, among other things, substantial financial penalties or awards against the Company, substantial payments made by the Company, harm to the Company’s reputation, required changes to the Company’s business practices, an impact on the Company's various relationships and/or contracts related to the Company's business, exclusion from future participation in the Medicare, Medicaid and other federal health care programs and, if criminal proceedings were initiated against the Company, members of its board of directors or management, possible criminal penalties, any of which could have a material adverse effect on the Company.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Shareholder and Derivative Claims
Peace Officers’ Annuity and Benefit Fund of Georgia Securities Class Action Civil Suit: On February 1, 2017, the Peace Officers’ Annuity and Benefit Fund of Georgia filed a putative federal securities class action complaint in the U.S. District Court for the District of Colorado against the Company and certain executives. The complaint covers the time period of August 2015 to October 2016 and alleges, generally, that the Company and its executives violatedfederal securities laws concerning the Company’s financial results and revenue derived from patients who received charitable premium assistance from an industry-funded non-profit organization. The complaint further alleges that the process by which patients obtained commercial insurance and received charitable premium assistance was improper and "created a false impression of DaVita’s business and operational status and future growth prospects." In November 2017, the court appointed the lead plaintiff and an amended complaint was filed on January 12, 2018. On March 27, 2018, the Company and various individual defendants filed a motion to dismiss. On March 28, 2019, the court denied the motion to dismiss. The Company answered the complaint on May 28, 2019. On January 31, 2020, the plaintiffs filed a motion for class certification and the Company filed its opposition on June 29, 2020.
While the Company continues to dispute the allegations, in July 2020, it reached an agreement in principle to resolve this matter without admitting to any liability. Settlement of this matter on the agreed terms is expected to be covered primarily with insurance proceeds, with the Company contributing an amount that would not have a material impact on the Company’s consolidated financial position, results of operations or cash flows. A motion for preliminary approval of the settlement was granted by the court on October 27, 2020. The settlement is subject to, among other things, final approval by the court.
In re DaVita Inc. Stockholder Derivative Litigation: On August 15, 2017, the U.S. District Court for the District of Delaware consolidated three previously disclosed shareholder derivative lawsuits: the Blackburn Shareholder action filed on February 10, 2017, the Gabilondo Shareholder action filed on May 30, 2017, and the City of Warren Police and Fire Retirement System Shareholder action filed on June 9, 2017. The complaint covers the time period from 2015 to present and alleges, generally, breach of fiduciary duty, unjust enrichment, abuse of control, gross mismanagement, corporate waste, and misrepresentations and/or failures to disclose certain information in violation of the federal securities laws in connection with an alleged practice to direct patients with government-subsidized health insurance into private health insurance plans to maximize the Company’s profits. An amended complaint was filed in September 2017, and on December 18, 2017, the Company filed a motion to dismiss and a motion to stay proceedings in the alternative. On April 25, 2019, the court denied the Company's motion to dismiss. The Company answered the complaint on May 28, 2019.
While the defendants continue to dispute the allegations, in July 2020, an agreement in principle was reached to resolve this matter without admitting to any liability. The Company’s Board of Directors (Board) approved the settlement on October 20, 2020. The court granted a motion for final approval of the settlement on January 27, 2021 and approved the settlement on January 29, 2021. As part of the settlement, the Company agreed to certain corporate governance policies, but will not make any financial contribution towards the settlement.
Other Proceedings
2021 Antitrust Indictment and Putative Class Action Suit: On July 14, 2021, an indictment was returned by a grand jury in the U.S. District Court, District of Colorado against the Company and its former chief executive officer in the matter of U.S. v. DaVita Inc., et al. alleging that purported agreements entered into by DaVita's former chief executive officer not to solicit senior-level employees violated Section 1 of the Sherman Act. On April 15, 2022, a jury returned a verdict in the Company’s favor, acquitting both the Company and its former chief executive officer on all counts. On April 20, 2022, the court entered judgments of acquittal and closed the case. On August 9, 2021, DaVita Inc. and its former chief executive officer were added as
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
defendants in a consolidated putative class action complaint in the matter of In additionre Outpatient Medical Center Employee Antitrust Litigation in the U.S. District Court, Northern District of Illinois. This class action complaint asserts that the defendants violated Section 1 of the Sherman Act and seeks to bring an action on behalf of certain groups of individuals employed by the foregoing,Company between February 1, 2012 and January 5, 2021. On September 26, 2022, the court denied the Company's motion to dismiss. The Company disputes the allegations in the class action complaint, as well as the asserted violations of the Sherman Act, and intends to defend this action accordingly.
Additionally, from time to time the Company is subject to other lawsuits, demands, claims, governmental investigations and audits and legal proceedings that arise due to the nature of its business, including, without limitation, contractual disputes, such as with payors, suppliers and others, employee-related matters and professional and general liability claims. From time to time, the Company also initiates litigation or other legal proceedings as a plaintiff arising out of contracts or other matters.
* * *
Other than as may be described above, the Company cannot predict the ultimate outcomes of the various legal proceedings and regulatory matters to which the Company is or may be subject from time to time, including those described in this Note 16 to these consolidated financial statements,15, or the timing of their resolution or the ultimate losses or impact of developments in those matters, which could have a material adverse effect on the Company’s revenues, earnings and cash flows. Further, any legal proceedings or regulatory matters involving the Company, whether meritorious or not, are time consuming, and often require management’s attention and result in significant legal expense, and may result in the diversion of significant operational resources, may impact the Company's various relationships and/or contracts related to the Company's business or otherwise harm the Company’s business, results of operations, financial condition, cash flows or reputation.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
17.16. Noncontrolling interests subject to put provisions and other commitments
Noncontrolling interests subject to put provisions
The Company has potential obligations to purchase the equity interests held by third parties in many of its majority-owned dialysis partnerships and other nonconsolidated entities. These noncontrolling interests subject to put provisions constitute redeemable equity interests and are therefore classified as temporary equity and carried at estimated fair value on the Company's balance sheet.
Specifically, these obligations are in the form of put provisions that are exercisable at the third-party owners’ discretion within specified periods outlined in each specific put provision. If these put provisions were exercised, the Company would be required to purchase the third-party owners’ equity interests, generally at the appraised fair market value of the equity interests or in certain cases at a predetermined multiple of earnings or cash flows attributable to the equity interests put to the Company, intended to approximate fair value. The methodology the Company uses to estimate the fair values of noncontrolling interests subject to put provisions assumes the higher of either a liquidation value of net assets or an average multiple of earnings, based on historical earnings, patient mix and other performance indicators that can affect future results, as well as other factors. The estimated fair values of noncontrolling interests subject to put provisions are a critical accounting estimate that involves significant judgments and assumptions and may not be indicative of the actual values at which the noncontrolling interests may ultimately be settled, which could vary significantly from the Company’s current estimates. The estimated fair values of noncontrolling interests subject to put provisions can fluctuate and the implicit multiple of earnings at which these noncontrolling interests obligations may be settled will vary significantly depending upon market conditions including potential purchasers’ access to the capital markets, which can impact the level of competition for dialysis and non-dialysis related businesses, the economic performance of these businesses and the restricted marketability of the third-party owners’ equity interests. The amount of noncontrolling interests subject to put provisions that employ a contractually predetermined multiple of earnings rather than fair value is immaterial.
The Company also has certain potential commitments to provide working capital funding, if necessary, to certain nonconsolidated dialysis businesses that the Company manages and in which the Company owns a noncontrolling equity interest or which are wholly-owned by third parties of approximately $8,663.
Certain consolidated dialysis partnerships are originally contractually scheduled to dissolve after terms ranging from ten years to 50 years. While noncontrolling interests in these limited life entities qualify as mandatorily redeemable financial instruments, they are subject to a classification and measurement scope exception from the accounting guidance generally applicable to other mandatorily redeemable financial instruments. Future distributions upon dissolution of these entities would be valued below the related noncontrolling interest carrying balances in the consolidated balance sheet.
Other commitments
In 2017, the Company entered into a Sourcing and Supply Agreement with Amgen USA Inc. (Amgen) that expires on December 31, 2022. Under the terms of the agreement, the Company will purchase EPO from Amgen in amounts necessary to meet no less than 90% of its requirements for erythropoiesis-stimulating agents (ESAs) through the expiration of the contract. The actual amount of EPO that the Company will purchase will depend upon the amount of EPO administered during dialysis as prescribed by physicians and the overall number of patients that the Company serves.
The Company has agreements with various suppliers to purchase established amounts of dialysis equipment, parts, pharmaceuticals and supplies. As of December 31, 2020,2023, the remaining minimum purchase commitments under these arrangements were approximately $542,061, $540,715, $179,869,$663,498, $541,683, $551,187, $175,707 and $92,075$178,559 for the years 2021, 2022, 2023,2024, 2025, 2026, 2027
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and 2024,shares in thousands, except per share data)
and 2028, respectively. If the Company fails to meet the minimum purchase commitments under these contracts during any year, it is required to pay the difference to the supplier.
The Company also has certain potential commitments to provide working capital funding, if necessary, to certain nonconsolidated dialysis businesses that the Company manages and in which the Company owns a noncontrolling equity interest or which are wholly-owned by third parties of approximately $8,852.
Other than the letters of credit disclosed in Note 1312 to these consolidated financial statements, and the arrangements as described above, the Company has 0no off balance sheet financing arrangements as of December 31, 2020.2023.
18. Long-term incentive17. Stock-based compensation
Long-term incentiveStock-based compensation
Long-term incentive program (LTIP)Stock-based compensation includes both stock-based awards (principallyconsists primarily of stock-settled stock appreciation rights, restricted stock units and performance stock units) as well as long-term performance-based cash awards.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Long-term incentiveunits. Stock-based compensation, expense, which is primarily general and administrative in nature, is attributed to the Company’s U.S. dialysis business, its corporate administrative support, and its ancillary services.
The Company’s See Note 1 "Organization and summary of significant accounting policies" for more information on how the Company measures and recognizes stock-based compensation expense for stock-settled awards is measured at the estimated fair value of awards on the date of grant and recognized on a cumulative straight-line basis over the vesting terms of the awards, unless the stock awards are based on non-market-based performance metrics, in which case expense is adjusted for the ultimate number of shares expected to be issued as of the end of each reporting period. Stock-based compensation expense for cash-settled awards is based on their estimated fair values as of the end of each reporting period. The expense for all LTIP awards is recognized net of expected forfeitures.
Stock-based compensation to be settled in shares is recorded to the Company’s shareholders’ contributed capital, while stock-based compensation to be settled in cash is recorded as a liability. Shares issued upon exercise or, when applicable, vesting of stock awards, are issued from authorized but unissued shares.expense.
Long-term incentive compensation plans
On June 11, 2020, the Company’s stockholders approved theThe DaVita Inc. 2020 Incentive Award Plan (the 2020 Plan). Prior to June 11, 2020 stock-based awards were granted under the DaVita Healthcare Partners Inc. 2011 Incentive Award Plan (the 2011 Plan). The 2011 Plan was terminated with respect to any new awards upon stockholder approval of the 2020 Plan. At the time the 2020 Plan was approved there were 8,730 shares of common stock available for issuance under the 2020 Plan, consisting of 5,000 newly authorized shares and 3,730 shares that were available for issuance under the 2011 Plan as of the effective date of the 2020 Plan and which became available for grant under the 2020 Plan, pursuant to the terms of the 2020 Plan.
The 2020 Plan is the Company’s current omnibus equity compensation plan and provides for grants of stock-based awards to employees, directors and other individuals providing services to the Company, except that incentive stock options may only be awarded to employees. The 2020 Plan provides for the grant of stock appreciation rights, nonqualified stock options, incentive stock options, restricted stock units, restricted stock, performance stock awards, dividend equivalents, stock payments, deferred stock unit awards, deferred stock awards and performance cash awards. The 2020 Plan mandates a maximum award term of 10 years for stock appreciation rights and stock options and stipulates that awards of these types be granted with a base or exercise price per share of not less than the fair market value of the Company's common stock on the date of grant. Shares available under the 2020 Plan are also stated on a full value share basis rather than on an option-equivalent basis. The 2020 Plan therefore provides that shares available for issuance under the plan are reduced by 1one share available for every 4four shares underlying stock appreciation rights and stock options, and are reduced by 1one share available for every 1one share underlying stock-based awards other than stock appreciation rights and stock options. At December 31, 2020,2023, there were 8,0745,570 shares available for future grants under the 2020 Plan. The Company’s stock units awardedawards granted under the 2020 Plan generally vest over 36 months to 48 months from the date of grant. As
A summary of December 31, 2020, 0the status of the Company’s stock-settled awards, including base shares for stock-settled stock appreciation rights have been awarded under the 2020 Plan.(SSARs) and stock-settled stock unit awards is as follows:
The 2011 Plan was the Company’s prior omnibus equity compensation plan and authorized the Company to award stock options, stock appreciation rights, restricted stock units, restricted stock, and other stock-based or performance-based awards. The 2011 Plan mandated a maximum award term of five years and stipulated that stock appreciation rights and stock options be granted with prices not less than fair market value on the date of grant. The 2011 Plan also required that full value share awards such as restricted stock units reduce shares available under the 2011 Plan at a ratio of 3.5:1. The Company’s stock appreciation rights and stock units awarded under the 2011 Plan generally vest over 36 months to 48 months from the date of grant. | | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, 2023 |
| | Stock appreciation rights | | Stock units |
| Awards | | Weighted
average
exercise
price | | Weighted
average
remaining
contractual life | | Awards | | Weighted
average
remaining
contractual life |
| Outstanding at beginning of year | 5,390 | | | $ | 66.00 | | | | | 3,072 | | | |
| Granted | — | | | | | | | 1,383 | | | |
| Added by performance factor | | | | | | | 66 | | | |
| Exercised/Vested | (1,872) | | | $ | 63.75 | | | | | (1,067) | | | |
| Canceled | (47) | | | $ | 52.41 | | | | | (231) | | | |
| Outstanding at end of period | 3,471 | | | $ | 67.40 | | | 0.91 | | 3,223 | | | 2.21 |
| Exercisable at end of period | 3,076 | | | $ | 63.42 | | | 0.75 | | — | | | — | |
| Weighted-average fair value of grants: | | | | | | | | | |
| 2023 | | | | | | | $ | 77.61 | | | |
| 2022 | $ | 35.13 | | | | | | | $ | 107.60 | | | |
| 2021 | $ | 32.15 | | | | | | | $ | 109.50 | | | |
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
A combined summary of the status of the Company’s stock-settled awards under both the 2020 Plan and 2011 Plan, including base shares for stock-settled stock appreciation rights (SSARs) and stock-settled stock unit awards is as follows:
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | Year ended December 31, 2020 |
| | Stock appreciation rights | | Stock units |
| Awards | | Weighted
average
exercise
price | | Weighted
average
remaining
contractual life | | Awards | | Weighted
average
remaining
contractual life |
| Outstanding at beginning of year | 6,953 | | | $ | 64.10 | | | | | 3,160 | | | |
| Granted | 2,765 | | | $ | 68.58 | | | | | 1,027 | | | |
| Added by performance factor | | | | | | | 19 | | | |
| Exercised/Vested | (894) | | | $ | 72.13 | | | | | (351) | | | |
| Expired | (494) | | | $ | 83.61 | | | | | 0 | | | |
| Canceled | (246) | | | $ | 61.36 | | | | | (318) | | | |
| Outstanding at end of period | 8,084 | | | $ | 63.64 | | | 3.0 | | 3,537 | | | 1.8 |
| Exercisable at end of period | 987 | | | $ | 69.56 | | | 1.0 | | 0 | | | — | |
| Weighted-average fair value of grants: | | | | | | | | | |
| 2020 | $ | 26.70 | | | | | | | $ | 77.83 | | | |
| 2019 | $ | 14.04 | | | | | | | $ | 50.58 | | | |
| 2018 | $ | 16.24 | | | | | | | $ | 66.23 | | | |
| | | | | Awards Outstanding | | Weighted average exercise price | | Awards exercisable | | Weighted average exercise price | | | Awards Outstanding | | Weighted average exercise price | | Awards exercisable | | Weighted average exercise price |
| Range of SSARs base prices | Range of SSARs base prices | |
| $50.01–$60.00 | $50.01–$60.00 | | 2,263 | | | $ | 52.53 | | | 2 | | | $ | 57.88 | |
| $50.01–$60.00 | |
| $50.01–$60.00 | |
| $60.01–$70.00 | $60.01–$70.00 | | 5,165 | | | $ | 66.99 | | | 610 | | | $ | 65.95 | |
| $70.01–$80.00 | $70.01–$80.00 | | 656 | | | $ | 75.60 | | | 375 | | | $ | 75.50 | |
| $100.01–$110.00 | | $100.01–$110.00 | | 132 | | | $ | 108.93 | | | |
| $110.01–$120.00 | | $110.01–$120.00 | | 130 | | | $ | 110.63 | | | |
| Total | Total | | 8,084 | | | $ | 63.64 | | | 987 | | | $ | 69.56 | |
For the years ended December 31, 2020, 2019,2023, 2022 and 2018,2021, the aggregate intrinsic value of stock-based awards exercised was $49,258, $11,475$168,500, $149,442 and $31,045,$208,585, respectively. At December 31, 2020,2023, the aggregate intrinsic value of stock-based awards outstanding was $853,803$475,918 and the aggregate intrinsic value of stock awards exercisable was $47,208.$128,229.
Estimated fair value of stock-based compensation awards
The Company has estimated the grant-date fair value of stock-settled stock appreciation rights awards using the Black-Scholes-Merton valuation model and stock-settled stock unit awards at intrinsic value on the date of grant, except for portions of the Company’s performance stock unit awards for which a Monte Carlo simulation was used to estimate the grant-date fair value. The following assumptions were used in estimating these values and determining the related stock-based compensation expense attributable to the current period:
Expected term of the awards: The expected term of awards granted represents the period of time that they are expected to remain outstanding from the date of grant. The Company determines the expected term of its stock awards based on its historical experience with similar awards, considering the Company’s historical exercise and post-vesting termination patterns.
Expected volatility: Expected volatility represents the volatility anticipated over the expected term of the award. The Company determines the expected volatility for its awards based on the volatility of the price of its common stock over the most recent retrospective period commensurate with the expected term of the award, considering the volatilities expected by peer companies in near industries.
Expected dividend yield: The Company has not paid dividends on its common stock and does not currently expect to pay dividends during the term of stock awards granted.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Risk-free interest rate: The Company bases the expected risk-free interest rate on the implied yield currently available on stripped interest coupons of U.S. Treasury issues with a remaining term equivalent to the expected term of the award.
A summary of the weighted average valuation inputs described above used for estimating the grant-date fair value of SSAR awards granted in the periods indicated is as follows:
| | | |
| | |
| | |
| | |
| | |
| | |
| | |
| | | | Year ended December 31, |
| | | 2020 | | 2019 | | 2018 | 2022 | | 2021 |
| Expected term | Expected term | 4.8 | | 4.0 | | 4.2 | Expected term | 4.5 | | 4.5 |
| Expected volatility | Expected volatility | 28.2 | % | | 29.5 | % | | 23.8 | % | Expected volatility | 34.3 | % | | 34.3 | % |
| Expected dividend yield | Expected dividend yield | 0 | % | | 0 | % | | 0 | % | Expected dividend yield | — | % | | — | % |
| Risk-free interest rate | Risk-free interest rate | 1.5 | % | | 2.2 | % | | 2.9 | % | Risk-free interest rate | 2.1 | % | | 0.7 | % |
The Company estimates expected forfeitures based upon historical experience with separate groups of employees that have exhibited similar forfeiture behavior in the past. Stock-based compensation expense is recorded only for awards that are expected to vest.
On November 4, 2019, the independent members of the Company’s Board of Directors (Board) approved an award of 2,500 premium-priced stock-settled stock appreciation rights (Premium-Priced Award) to the Company’s Chief Executive Officer (CEO), which award was subject to stockholder approval of a related amendment to the 2011 Plan. Stockholders approved such amendment to the 2011 Plan on January 23, 2020, authorizing the grant to the Company's CEO. Since stockholder approval occurred in 2020, this award was treated as granted in 2020 for accounting purposes.
The base price of the Premium-Priced Award was $67.80 per share, which was a 20% premium to the clearing price of the Company's modified Dutch auction tender offer for its shares in 2019 (2019 Tender Offer). The award vests 50% on each of November 4, 2022 and November 4, 2023 and expires on November 4, 2024. The award includes a requirement that the CEO hold any shares acquired upon exercise of this award, net of shares used to cover related taxes, until November 4, 2024 (that is, for the full term of the award), subject to lapse of the holding period upon a change in control of the Company or due to the CEO's death or termination due to disability.
Employee stock purchase plan
The Employee Stock Purchase Plan entitles qualifying employees to purchase up to $25 of the Company’s common stock during each calendar year. The amounts used to purchase stock are accumulated through payroll withholdings or through optional lump sum payments made in advance of the first day of the purchase right period. This compensatory plan allows employees to purchase stock for the lesser of 100% of its fair market value on the first day of the purchase right period or 85% of its fair market value on the last day of the purchase right period. Purchase right periods begin on January 1 and July 1, and end on December 31. Contributions used to purchase the Company’s common stock under this plan for the 2020, 20192023, 2022 and 2018
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
2021 purchase periods were $17,148, $16,569$18,213, $18,061 and $17,398,$19,626, respectively. Shares purchased pursuant to the plan’s 2020, 20192023, 2022 and 20182021 purchase periods were 222, 315231, 285 and 398,203, respectively. At December 31, 2020,2023, there were 6,1895,471 shares remaining available for future grants under this plan.
The fair value of participants’ purchase rights was estimated as of the beginning dates of the purchase right periods using the Black-Scholes-Merton valuation model with the following weighted average assumptions for purchase right periods in 2020, 20192023, 2022 and 2018,2021, respectively: expected volatility of 40.4%41.3%, 28.8%31.7% and 24.2%39.0%; risk-free interest rates of 1.0%4.9%, 2.6%1.3% and 1.9%,0.1%; and 0no dividends. Using these assumptions, the weighted average estimated per share fair value of each purchase right was $22.06, $13.80$25.25, $26.50 and $17.45$34.94 for 2020, 20192023, 2022 and 2018,2021, respectively.
Long-term incentiveStock-based compensation expense and proceeds
For the years ended December 31, 2020, 20192023, 2022 and 2018,2021, the Company recognized $99,643, $118,513$112,375, $95,427 and $85,759, respectively,$102,209 in total LTIP expense, of which $91,458, $63,705 and $73,582, respectively, was stock-based compensation expense for stock appreciation rights, stock units and discounted employee stock purchase plan purchases, which are primarily included in general and administrative expenses. The estimated tax benefits recorded for stock-based compensation in 2020, 20192023, 2022 and 20182021 were $11,775, $9,186$16,536, $14,723 and $13,591,$13,853, respectively. As of December 31, 2020,2023, there was $189,713$134,720 of total estimated but unrecognized stock-based compensation expense under the Company’s equity compensation and employee stock purchase plans. The Company expects to recognize this expense over a weighted average remaining period of 1.41.3 years. The Company 0 longer has outstanding long-term performance-based cash awards in its principal U.S. dialysis business as the performance and accrual period for these awards ended December 31, 2019 with a final payout of $66,302 in 2020.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
During the year ended December 31, 2018, the Company adopted a retirement policy (Rule of 65 policy). The Rule of 65 policy generally provides that Section 16 officers that are a minimum age of 55 with five years of continuous service with the Company receive certain benefits with respect to their outstanding equity awards upon a qualifying retirement if the sum of their age plus years of service is greater than or equal to 65. These benefits generally include accelerated vesting of restricted stock unit awards, continued vesting of stock-settled stock appreciation rights and performance stock unit awards and an exercise window for stock-settled stock appreciation rights from the original vest date through the original expiration date regardless of continued employment, with pro rata vesting for a Rule of 65 retirement within one year of the award grant date. The adoption of the Rule of 65 policy resulted in a $14,704 modification charge and a net acceleration of expense of $9,727 during the year ended December 31, 2018 that is included in the expense amounts reported above.
For the years ended December 31, 2020, 20192023, 2022 and 2018,2021, the Company received $8,957, $2,251$25,629, $24,805 and $7,988,$46,990, respectively, in actual tax benefits upon the exercise or vesting of stock awards. Since the Company issues stock-settled stock appreciation rights rather than stock options, there were 0no cash proceeds from stock option exercises.
19.18. Shareholders’ equity
Stock repurchases
The following table summarizes the Company's repurchases of its common stock during the years ended December 31, 2020, 20192023, 2022 and 2018:2021:
| | | | | | | | | | | | | | | | | |
| 2020 | | 2019 | | 2018 |
| Open market repurchases | | | | | |
| Shares | 8,495 | | | 19,218 | | | 16,844 | |
| Amounts paid | $ | 741,850 | | | $ | 1,168,321 | | | $ | 1,153,511 | |
| Average paid per share | $ | 87.32 | | | $ | 60.79 | | | $ | 68.48 | |
| | | | | |
Tender offers (1) | | | | | |
| Shares | 7,982 | | | 21,802 | | | 0 |
| Amounts paid | $ | 704,917 | | | $ | 1,234,154 | | | 0 |
| Average paid per share | $ | 88.32 | | | $ | 56.61 | | | 0 |
| | | | | |
| Total | | | | | |
| Shares | 16,477 | | | 41,020 | | | 16,844 | |
| Amounts paid | $ | 1,446,767 | | | $ | 2,402,475 | | | $ | 1,153,511 | |
| Average paid per share | $ | 87.80 | | | $ | 58.57 | | | $ | 68.48 | |
| | | | | | | | | | | | | | | | | |
| 2023 | | 2022 | | 2021 |
| Open market repurchases | | | | | |
| Shares | 2,904 | | | 8,095 | | | 13,877 | |
Amounts paid(1) | $ | 285,710 | | | $ | 787,854 | | | $ | 1,546,016 | |
Average price paid per share(2) | $ | 97.82 | | | $ | 97.30 | | | $ | 111.38 | |
| | | | | |
| | | | | |
| | | | | |
| | | | | |
| | | | | |
| | | | | |
| | | | | |
| | | | | |
| | | | | |
| | | | | |
(1)The aggregate amounts paid for shares repurchased pursuant toIncludes commissions and the Company's 2020 and 2019 tender offers for its shares during the years ended1% excise tax imposed on certain stock repurchases made after December 31, 20202022 by the Inflation Reduction Act of 2022. The excise tax is recorded as part of the cost basis of treasury stock repurchased and, 2019, include their clearing prices of $88.00as such, is included in stockholders’ equity.
(2)Excludes commissions and $56.50 per share, respectively, plus related fees and expenses of $2,529 and $2,343, respectively.the excise tax described above.
Subsequent to December 31, 2020 through February 10, 2021, theThe Company has repurchased 1,0631,507 shares of its common stock for $123,282$164,366 at an average costprice paid of $115.98$107.97 per share.share subsequent to December 31, 2023 through February 12, 2024.
Effective asAs of the close of business on November 4, 2019, the Board terminated all remaining prior share repurchase authorizations available toDecember 31, 2023, the Company and approvedis authorized to make share repurchases pursuant to a new shareDecember 17, 2021 Board authorized repurchase authorization of $2,000,000.
Effective on December 10, 2020, the Board terminated all remaining prior share repurchase authorizations available to the Company under the aforementioned November 4, 2019 authorization and approved a new share repurchase authorizationplan of $2,000,000. TheThis authorization allows the Company is authorized to make purchases from time to time in the open market or in privately negotiated transactions, including without limitation, through accelerated share repurchase transactions, derivative transactions, tender offers, Rule 10b5-1 plans or any combination of the foregoing, depending upon market conditions and other considerations.
As of February 10, 2021,12, 2024, the Company has a total of $1,806,674$1,149,192, excluding excise taxes, available under the current repurchase authorization for additional share repurchases. Although this share repurchase authorization does not have an expiration date, the Company
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
remains subject to share repurchase limitations, including under the terms of the currentits senior secured credit facilities and the indentures governing the Company's senior notes.facilities.
The Company retired all shares held in its treasury effective as of December 31, 20202023 and December 31, 2019.2022.
Charter documents & Delaware law
The Company’s charter documents include provisions that may deter hostile takeovers, delay or prevent changes of control or changes in management, or limit the ability of stockholders to approve transactions that they may otherwise
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
determine to be in their best interests. These include provisions prohibiting stockholders from acting by written consent, requiring 90 days advance notice for director nominations and stockholder proposals and granting the Company's Board of Directors the authority to issue up to 5,000 shares of preferred stock and to determine the rights and preferences of the preferred stock without the need for further stockholder approval.
The Company is also subject to Section 203 of the Delaware General Corporation Law which, subject to exceptions, prohibits the Company from engaging in any business combinations with any interested stockholder, as defined in that section, for a period of three years following the date on which that stockholder became an interested stockholder. The provisions described above may discourage, delay or prevent an acquisition of the Company at a price that stockholders may find attractive.
Changes in DaVita Inc.’s ownership interests in consolidated subsidiaries
The effects of changes in DaVita Inc.’s ownership interests in consolidated subsidiaries on the Company’s consolidated equity were as follows:
| | | | Year ended December 31, | | Year ended December 31, |
| | | 2020 | | 2019 | | 2018 | | 2023 | | 2022 | | 2021 |
| Net income attributable to DaVita Inc. | Net income attributable to DaVita Inc. | $ | 773,642 | | | $ | 810,981 | | | $ | 159,394 | |
| Changes in paid-in capital for: | Changes in paid-in capital for: | |
| Purchases of noncontrolling interests | Purchases of noncontrolling interests | 4,364 | | | (37,145) | | | (17,897) | |
| Purchases of noncontrolling interests | |
| Purchases of noncontrolling interests | |
| Sales of noncontrolling interest | Sales of noncontrolling interest | 0 | | | 0 | | | 79 | |
| Net transfers in noncontrolling interests | Net transfers in noncontrolling interests | 4,364 | | | (37,145) | | | (17,818) | |
Net income attributable to DaVita Inc. net of transfers in
noncontrolling interests | Net income attributable to DaVita Inc. net of transfers in
noncontrolling interests | $ | 778,006 | | | $ | 773,836 | | | $ | 141,576 | |
The Company acquired additional ownership interests in several existing majority-owned partnerships for $7,831, $68,019,$12,555, $20,775 and $28,082$20,104 in 2020, 2019,2023, 2022 and 2018,2021, respectively.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
20.19. Accumulated other comprehensive (loss) incomeloss
Charges and credits to other comprehensive (loss) income have been as follows:
| | | | | | | | | | | | | | | | | | | | | | | |
| | Interest rate
cap agreements | | Investment
securities | | Foreign currency
translation
adjustments | | Accumulated other
comprehensive
(loss) income |
| Balance at December 31, 2017 | $ | (12,408) | | | $ | 5,662 | | | $ | 19,981 | | | $ | 13,235 | |
Cumulative effect of change in accounting principle(1) | (2,706) | | | (5,662) | | | 0 | | | (8,368) | |
| Unrealized losses | (181) | | | 0 | | | (45,944) | | | (46,125) | |
| Related income tax | 48 | | | 0 | | | 0 | | | 48 | |
| | (133) | | | 0 | | | (45,944) | | | (46,077) | |
| Reclassification of income (loss) into net income | 8,466 | | | 0 | | | 0 | | | 8,466 | |
| Related income tax | (2,180) | | | 0 | | | 0 | | | (2,180) | |
| | 6,286 | | | 0 | | | 0 | | | 6,286 | |
| Balance at December 31, 2018 | $ | (8,961) | | | $ | 0 | | | $ | (25,963) | | | $ | (34,924) | |
| Unrealized gains (losses) | 1,566 | | | 0 | | | (20,102) | | | (18,536) | |
| Related income tax | (415) | | | 0 | | | 0 | | | (415) | |
| | 1,151 | | | 0 | | | (20,102) | | | (18,951) | |
| Reclassification of income into net income | 8,591 | | | 0 | | | 0 | | | 8,591 | |
| Related income tax | (2,214) | | | 0 | | | 0 | | | (2,214) | |
| | 6,377 | | | 0 | | | 0 | | | 6,377 | |
| Balance at December 31, 2019 | $ | (1,433) | | | $ | 0 | | | $ | (46,065) | | | $ | (47,498) | |
| Unrealized losses | (21,781) | | | 0 | | | (7,080) | | | (28,861) | |
| Related income tax | 5,435 | | | 0 | | | (543) | | | 4,892 | |
| | (16,346) | | | 0 | | | (7,623) | | | (23,969) | |
| Reclassification of income into net income | 7,081 | | | 0 | | | 0 | | | 7,081 | |
| Related income tax | (1,768) | | | 0 | | | 0 | | | (1,768) | |
| | 5,313 | | | 0 | | | 0 | | | 5,313 | |
| Balance at December 31, 2020 | $ | (12,466) | | | $ | 0 | | | $ | (53,688) | | | $ | (66,154) | |
(1)Reflects the cumulative effect of a change in accounting principle for ASUs 2016-01 and 2018-03 on classification and measurement of financial instruments and ASU 2018-02 on remeasurement and reclassification of deferred tax effects in accumulated other comprehensive income associated with the 2017 Tax Act. | | | | | | | | | | | | | | | | | |
| | Interest rate
cap agreements | | Foreign currency
translation
adjustments | | Accumulated other
comprehensive
(loss) income |
| Balance at December 31, 2020 | $ | (12,466) | | | $ | (53,688) | | | $ | (66,154) | |
| Unrealized gains (losses) | 9,532 | | | (83,375) | | | (73,843) | |
| Related income tax | (2,377) | | | (1,006) | | | (3,383) | |
| | 7,155 | | | (84,381) | | | (77,226) | |
| Reclassification of loss into net income | 5,509 | | | — | | | 5,509 | |
| Related income tax | (1,376) | | | — | | | (1,376) | |
| | 4,133 | | | — | | | 4,133 | |
| Balance at December 31, 2021 | $ | (1,178) | | | $ | (138,069) | | | $ | (139,247) | |
| Unrealized gains (losses) | 144,793 | | | (30,554) | | | 114,239 | |
| Related income tax | (36,124) | | | 752 | | | (35,372) | |
| | 108,669 | | | (29,802) | | | 78,867 | |
| Reclassification of income into net income | (11,732) | | | — | | | (11,732) | |
| Related income tax | 2,926 | | | — | | | 2,926 | |
| | (8,806) | | | — | | | (8,806) | |
| Balance at December 31, 2022 | $ | 98,685 | | | $ | (167,871) | | | $ | (69,186) | |
| Unrealized gains | 9,186 | | | 89,055 | | | 98,241 | |
| Related income tax | (2,291) | | | (1,121) | | | (3,412) | |
| | 6,895 | | | 87,934 | | | 94,829 | |
| Reclassification of income into net income | (103,567) | | | — | | | (103,567) | |
| Related income tax | 25,840 | | | — | | | 25,840 | |
| | (77,727) | | | — | | | (77,727) | |
| Balance at December 31, 2023 | $ | 27,853 | | | $ | (79,937) | | | $ | (52,084) | |
The reclassification of net interest rate cap realized losses into income are recorded as debt expense in the corresponding consolidated statements of income. See Note 1312 for further details.
21.20. Acquisitions and divestitures
Routine acquisitions
During 2020,2023, 2022 and 2021, the Company acquired 8 dialysis centers in the U.S.businesses and 66 dialysis centers outside the U.S. for a total of $182,013 in net cash, earn-outs of $14,042 and deferred purchase price and liabilities assumed of $20,415. The Company also recognized a non-cash gain of $1,821. During 2019, the Company acquired 7 dialysis centers in the U.S. and 16 dialysis centers outside the U.S. for a total of $98,836 in net cash, earn-outs of $23,536, and deferred purchase price and liabilities assumed of $4,326. During 2018, the Company acquired 18 dialysis centers in the U.S. and 28 dialysis centers outside the U.S. for a total of $176,161 in net cash, earn-outs of $1,246 and deferred purchase price of $34,394. In one of these 2018 transactions the Company acquired a controlling interest in a previously nonconsolidated U.S. dialysis partnership for which the Company recognized a non-cash gain of $28,152 on its prior interest upon consolidation. other businesses, as follows:
| | | | | | | | | | | | | | | | | |
| Year ended Year ended December 31, |
| 2023 | | 2022 | | 2021 |
| Cash paid, net of cash acquired | $ | 26,394 | | | $ | 57,308 | | | $ | 187,050 | |
| Contingent earn-out obligations | 11,065 | | | 4,261 | | | 14,854 | |
| Deferred purchase price and liabilities assumed | 8,736 | | | 15,076 | | | 10,226 | |
| Aggregate consideration | $ | 46,195 | | | $ | 76,645 | | | $ | 212,130 | |
| Number of dialysis centers acquired — U.S. | — | | | 5 | | 19 |
| Number of dialysis centers acquired — International | 12 | | 11 | | 17 |
The assets and liabilities for allthese acquisitions were recorded at their estimated fair values at the dates of the acquisitions and are included in the Company’s consolidated financial statements, as are their operating results, from the designated effective dates of the acquisitions.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
The initial purchase price allocations for these transactions have been recorded at estimated fair values based on information available to management and will be finalized when certain information arranged to be obtained has been received. For several of the 20202023 acquisitions, certain income tax amounts are pending final evaluation and quantification of any pre-acquisitionpre-
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
acquisition tax contingencies. In addition, valuation of contingent earn-outs, intangibles, fixed assets, leases and certain other working capital items relating to several of these acquisitions are pending final quantification.
The following table summarizes the assets acquired and liabilities assumed in these transactions and recognized at their acquisition dates at estimated fair values, as well as the estimated fair value of noncontrolling interests assumed in these transactions:
| | | | Year ended December 31, | | Year ended December 31, |
| | | 2020 | | 2019 | | 2018 | | 2023 | | 2022 | | 2021 |
| Current assets | Current assets | $ | 23,607 | | | $ | 6,713 | | | $ | 23,686 | |
| Property and equipment | Property and equipment | 37,457 | | | 4,842 | | | 11,421 | |
| Customer relationships | Customer relationships | 34,625 | | | 0 | | | 0 | |
| Noncompetition agreements and other long-term assets | Noncompetition agreements and other long-term assets | 10,168 | | | 1,980 | | | 3,079 | |
| Indefinite-lived licenses | Indefinite-lived licenses | 22,136 | | | 31,858 | | | 23,656 | |
| Goodwill | Goodwill | 130,057 | | | 90,226 | | | 278,348 | |
| Deferred income taxes | (3,962) | | | 0 | | | 0 | |
| | Liabilities assumed | |
| Liabilities assumed | |
| Liabilities assumed | Liabilities assumed | (34,068) | | | (7,159) | | | (19,946) | |
| Noncontrolling interests assumed | Noncontrolling interests assumed | (1,729) | | | (1,762) | | | (80,291) | |
| $ | 218,291 | | | $ | 126,698 | | | $ | 239,953 | |
| $ | |
The following summarizes weighted-average estimated useful lives of amortizable intangible assets acquired during 2020, 20192023, 2022 and 2018,2021, as well as goodwill deductible for tax purposes associated with these acquisitions:
| | Year ended December 31, |
| 2020 | | 2019 | | 2018 |
| Weighted-average estimated useful lives: | | | | | |
| Year ended December 31, | | | Year ended December 31, |
| 2023 | | | 2023 | | 2022 | | 2021 |
| Weighted-average estimated useful lives (in years): | |
| Customer relationships | |
| Customer relationships | |
| Customer relationships | Customer relationships | 18 | | 0 | | 0 | — | | | — | | — | | | 10 | | 10 |
| Noncompetition agreements | Noncompetition agreements | 5 | | 6 | | 6 | Noncompetition agreements | 3 | | 4 | | 6 |
| | Goodwill deductible for tax purposes | Goodwill deductible for tax purposes | $ | 94,318 | | | $ | 88,517 | | | $ | 165,013 | |
| Goodwill deductible for tax purposes | |
| Goodwill deductible for tax purposes | |
Pro forma financial information (unaudited)
The following summary, prepared on a pro forma basis, combines the results of operations as if all acquisitions within continuing operations in 20202023 and 20192022 had been consummated as of the beginning of 2019,2022, including the impact of certain adjustments such as amortization of intangibles, interest expense on acquisition financing and income tax effects.
| | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 |
| | (unaudited) |
| Pro forma total revenues | $ | 11,636,416 | | | $ | 11,570,086 | |
Pro forma net income from continuing operations attributable to
DaVita Inc. | $ | 789,473 | | | $ | 718,928 | |
Pro forma basic net income per share from continuing operations
attributable to DaVita Inc. | $ | 6.59 | | | $ | 4.69 | |
Pro forma diluted net income per share from continuing operations
attributable to DaVita Inc. | $ | 6.44 | | | $ | 4.67 | |
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Sale of RMS Lifeline
The Company divested its vascular access business, RMS Lifeline, Inc., effective May 1, 2020 and recognized a loss on sale of approximately $16,252. | | | | | | | | | | | |
| | Year ended December 31, |
| | 2023 | | 2022 |
| | (unaudited) |
| Pro forma total revenues | $ | 12,160,466 | | | $ | 11,651,311 | |
Pro forma net income from continuing operations attributable to
DaVita Inc. | $ | 694,854 | | | $ | 550,245 | |
Pro forma basic net income per share from continuing operations
attributable to DaVita Inc. | $ | 7.65 | | | $ | 5.92 | |
Pro forma diluted net income per share from continuing operations
attributable to DaVita Inc. | $ | 7.46 | | | $ | 5.74 | |
Contingent earn-out obligations
The Company has several contingent earn-out obligations associated with acquisitions that could result in the Company paying the former owners of acquired companiesbusinesses a total of up to approximately $42,378$66,299 if certain performance targets or quality margins are met over the next one year to five years.
Contingent earn-out obligations are remeasured to fair value at each reporting date until the contingencies are resolved with changes in the liability due to the remeasurement recognized in earnings. See Note 2423 for further details. As of December 31, 2020,2023, the Company estimated the fair value of these contingent earn-out obligations to be $30,248,$23,088, of which a
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
total of $13,025$6,431 is included in other current liabilities, and the remaining $17,223$16,657 is included in other long-term liabilities in the Company’s consolidated balance sheet.
The following is a reconciliation of changes in contingent earn-out liabilities for the years ended December 31, 20202023 and 2019:2022:
| | Year ended December 31, |
| 2020 | | 2019 |
| Year ended December 31, | | | Year ended December 31, |
| 2023 | | | 2023 | | 2022 |
| Beginning balance | Beginning balance | $ | 24,586 | | | $ | 2,608 | |
| Acquisitions | Acquisitions | 14,042 | | | 23,536 | |
| Foreign currency translation | Foreign currency translation | (3,688) | | | (905) | |
| Fair value remeasurements | Fair value remeasurements | (2,630) | | | 121 | |
| Payments or other settlements | Payments or other settlements | (2,062) | | | (774) | |
| Ending balance | Ending balance | $ | 30,248 | | | $ | 24,586 | |
22.21. Discontinued operations previously held for sale
DaVita Medical Group (DMG)
On June 19, 2019, the Company completed the sale of its prior DMG business to Optum, a subsidiary of UnitedHealth Group Inc., for an aggregate purchase price of $4,340,000, prior to certain closing and post-closing adjustments specified in the related equity purchase agreement dated as of December 5, 2017, as amended as of September 20, 2018 and as of December 11, 2018 (as amended, the equity purchase agreement).
The Company recorded a preliminary estimated pre-tax net loss of approximately $23,022 on the sale of its DMG business in 2019. This preliminary net loss was based on initial estimates of the Company's expected aggregate proceeds from the sale, net of transaction costs and obligations, as well as the estimated values of DMG net assets sold as of the closing date. Those estimated net proceeds included $4,465,476 in cash received from Optum at closing, or $3,824,509 net of cash and restricted cash included in the DMG net assets sold.
At close, of the DMG sale, the Company's ultimate net proceeds from this sale proceeds remained subject to resolution of certain post-closing adjustments.
Shortly after December 31, 2022, Optum made an additional purchase price adjustments described inpayment of $13,452 to the equity purchase agreement. InCompany after resolution of one such post-closing matter, which represented a contingent gain to the Company for the fourth quarter of 2020, the2022.
The Company and Optum reached agreement on the final purchase pricerecognized no DMG operating, financing or investing cash flows for the DMG sale, which resulted in an additional payment by the Company to Optum of $47,000years ended December 31, 2023, 2022 and an additional loss on sale of $17,976. In the first quarter of 2020, the Company recognized $9,980 in additional tax benefits under the Coronavirus Aid, Relief and Economic Security Act related to its period of DMG ownership, which were also recognized as an adjustment to the Company's loss on sale of the DMG business.2021.
Under the equity purchase agreement, the Company also has certain continuing indemnification obligations that could require payments to the buyer relating to the Company's previous ownership and operation of the DMG business. Potential payments under these provisions, if any, remain subject to continuing uncertainties and the amounts of such payments could be significant to the Company.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
The following table presents the financial results of discontinued operations related to DMG:
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 |
| Net revenues | $ | 0 | | | $ | 2,713,059 | | | $ | 4,963,792 | |
| Expenses | 0 | | | 2,543,865 | | | 4,962,686 | |
| Goodwill and other asset impairment charges | 0 | | | 0 | | | 41,537 | |
| Valuation adjustment on disposal group | 0 | | | 0 | | | 316,840 | |
| Income (loss) from discontinued operations before taxes | 0 | | | 169,194 | | | (357,271) | |
| Loss on sale of discontinued operations before taxes | (7,996) | | | (23,022) | | | 0 | |
| Income tax expense | 1,657 | | | 40,689 | | | 99,768 | |
| Net (loss) income from discontinued operations, net of tax | $ | (9,653) | | | $ | 105,483 | | | $ | (457,038) | |
The following table presents cash flows of discontinued operations related to DMG:
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 |
| Net cash provided by operating activities from discontinued operations | $ | 0 | | | $ | 99,634 | | | $ | 290,684 | |
| Net cash used in investing activities from discontinued operations | $ | 0 | | | $ | (43,442) | | | $ | (57,382) | |
DMG acquisitions
During the period from January 1, 2019 to June 18, 2019 immediately prior to the sale, the DMG business acquired 2 medical businesses for a total of $2,025 in net cash and deferred purchase price of $212. During 2018, the DMG business acquired other medical businesses for a total of $6,995 in net cash and deferred purchase price of $1,142.
23.22. Variable interest entities
The Company manages or maintains an ownership interest in certain legal entities subject to the consolidation guidance applicable to variable interest entities (VIEs). Almost all of these legal entitiesthe VIEs the Company consolidates are either U.S. dialysis partnerships encumbered by guaranteed debt, U.S. dialysis limited partnerships, U.S. integrated kidney care subsidiaries, or other legal entities subject to nominee ownership arrangements.
Under U.S. GAAP, VIEs typically include entities for which (i) the entity’s equity is not sufficient to finance its activities without additional subordinated financial support; (ii) the equity holders as a group lack the power to direct the activities that most significantly influence the entity’s economic performance, the obligation to absorb the entity’s expected losses, or the right to receive the entity’s expected returns; or (iii) the voting rights of some investors are not proportional to their obligations to absorb the entity’s losses.
The substantial majority of VIEs the Company is associated with are U.S. dialysis partnerships which the Company manages and in which it maintains a controlling majority ownership interest. These U.S. dialysis partnerships are considered VIEs either because they are (i) encumbered by debt guaranteed proportionately by the partners that is considered necessary to finance the partnership's activities, or (ii) in the form of limited partnerships for which the limited partners are not considered to have substantive kick-out or participating rights. The Company consolidates virtually all such U.S. dialysis partnerships.
Also, certain wholly-owned entities employed in the Company's integrated kidney care business constitute VIEs since by design these entities require additional subordinated financial support. The Company also reliesbelieves it has the most power over these entities' most significant activities and the Company is fully exposed to all or almost all of their expected losses. The Company therefore consolidates these wholly-owned entities as its subsidiaries.
Finally, some of the Company's business units rely on the operating activities of certain nominee-owned legal entities in which it does not maintain a controlling ownership interest but over which it has indirect influence and of which it is considered
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
the primary beneficiary. These entities are typically subject to nominee ownershiptransfer restriction, management and transfer restrictionother agreements that effectively transfer the majority of the economic risks and rewards of their ownership to the Company. The Company’s management, restriction and other agreements concerning such nominee-owned entities typically include both financial terms and protective and participating rights to the entities’ operating, strategic and non-clinical governance decisions which transfer substantial ultimate powers over, and economic responsibility for, these entities to the Company. The Company consolidates all of the nominee-owned entities with which it is most closely associated.
At December 31, 2020,In addition to the consolidated entities described above, the Company maintains minor equity method or other venture capital investments in certain development-stage investees which qualify as VIEs based on their capitalization. The Company has concluded that it is not the primary beneficiary of any of these investees.
For the VIEs described above, these consolidated financial statements include total assets of VIEs above of $310,190$256,542 and total liabilities and noncontrolling interests of these VIEs to third parties of $216,632.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
$139,443 at December 31, 2023.The Company also sponsors certain non-qualified deferred compensation plans whose trusts qualify as VIEs and the Company consolidates these plans as their primary beneficiary. The assets of these plans are recorded in short-term or long-term investments with related liabilities recorded in accrued compensation and benefits and other long-term liabilities. See Note 15Notes 4 and 14 for disclosures concerning the assets of these consolidated non-qualified deferred compensation plans.
24.23. Fair values of financial instruments
The Company measures the fair value of certain assets, liabilities, and noncontrolling interests subject to put provisions (redeemable equity interests classified as temporary equity) based upon certain valuation techniques that include observable or unobservable inputs and assumptions that market participants would use in pricing these assets, liabilities, temporary equity and commitments. The Company has also classified assets, liabilities and temporary equity that are measured at fair value on a recurring basis into the appropriate fair value hierarchy levels as defined by the FASB.
The following table summarizes the Company’s assets, liabilities and temporary equity measured at fair value on a recurring basis as of December 31, 20202023 and 2019:2022:
| | | | | | | | | | | | | | | | | | | | | | | |
| December 31, 2020 | Total | | Quoted prices in
active markets for
identical assets
(Level 1) | | Significant other
observable inputs
(Level 2) | | Significant
unobservable
inputs
(Level 3) |
| Assets | | | | | | | |
| Investments in equity securities | $ | 44,077 | | | $ | 44,077 | | | $ | 0 | | | $ | 0 | |
| Interest rate cap agreements | $ | 2,671 | | | $ | 0 | | | $ | 2,671 | | | $ | 0 | |
| Liabilities | | | | | | | |
| Contingent earn-out obligations | $ | 30,248 | | | $ | 0 | | | $ | 0 | | | $ | 30,248 | |
| Temporary equity | | | | | | | |
| Noncontrolling interests subject to put provisions | $ | 1,330,028 | | | $ | 0 | | | $ | 0 | | | $ | 1,330,028 | |
| December 31, 2019 | | | | | | | |
| Assets | | | | | | | |
| Investments in equity securities | $ | 39,951 | | | $ | 39,951 | | | $ | 0 | | | $ | 0 | |
| Interest rate cap agreements | $ | 24,452 | | | $ | 0 | | | $ | 24,452 | | | $ | 0 | |
| Liabilities | | | | | | | |
| Contingent earn-out obligations | $ | 24,586 | | | $ | 0 | | | $ | 0 | | | $ | 24,586 | |
| Temporary equity | | | | | | | |
| Noncontrolling interests subject to put provisions | $ | 1,180,376 | | | $ | 0 | | | $ | 0 | | | $ | 1,180,376 | |
For reconciliations of changes in contingent earn-out obligations and noncontrolling interests subject to put provisions during the year ended at December 31, 2020 and 2019, see Note 21 and the consolidated statement of equity, respectively. | | | | | | | | | | | | | | | | | | | | | | | |
| December 31, 2023 | Total | | Quoted prices in
active markets for
identical assets
(Level 1) | | Significant other
observable inputs
(Level 2) | | Significant
unobservable
inputs
(Level 3) |
| Assets | | | | | | | |
| Investments in equity securities | $ | 37,391 | | | $ | 37,391 | | | | | |
| Interest rate cap agreements | $ | 79,805 | | | | | $ | 79,805 | | | |
| Liabilities | | | | | | | |
| Contingent earn-out obligations for acquisitions | $ | 23,088 | | | | | | | $ | 23,088 | |
| Temporary equity | | | | | | | |
| Noncontrolling interests subject to put provisions | $ | 1,499,288 | | | | | | | $ | 1,499,288 | |
| December 31, 2022 | | | | | | | |
| Assets | | | | | | | |
| Investments in equity securities | $ | 39,143 | | | $ | 39,143 | | | | | |
| Interest rate cap agreements | $ | 139,755 | | | | | $ | 139,755 | | | |
| Liabilities | | | | | | | |
| Contingent earn-out obligations for acquisitions | $ | 25,422 | | | | | | | $ | 25,422 | |
| Temporary equity | | | | | | | |
| Noncontrolling interests subject to put provisions | $ | 1,348,908 | | | | | | | $ | 1,348,908 | |
Investments in equity securities represent investments in various open-ended registered investment companies (mutual funds) and common stockstocks and are recorded at fair value estimated based on reported market prices or redemption prices, as applicable. See Note 54 for further discussion.
Interest rate cap agreements are recorded at fair value estimated from valuation models utilizing the income approach and commonly accepted valuation techniques that use inputs from closing prices for similar assets and liabilities in active markets as well as other relevant observable market inputs at quoted intervals such as current interest rates, forward yield curves, implied volatility and credit default swap pricing. The Company does not believe the ultimate amount that could be realized upon settlement of these interest rate cap agreements would be materially different from the fair value estimates currently reported. See Note 1312 for further discussion.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
The estimated fair value measurements of these contingent earn-out obligations are primarily based on unobservable inputs, including projected earnings before interest, taxes, depreciation, and amortization (EBITDA), revenue and revenue.key performance indicators. The estimated fair value of these contingent earn-out obligations is remeasured as of each reporting date and could fluctuate based upon any significant changes in key assumptions, such as changes in the Company credit risk adjusted rate that is used to discount obligations to present value. See Note 2120 for further discussion.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollarsdiscussion and shares in thousands, except per share data)
a reconciliation of changes.The estimated fair value of noncontrolling interests subject to put provisions is based principally on the higher of either estimated liquidation value of net assets or a multiple of earnings for each subject dialysis partnership, based on historical earnings, revenue mix, and other performance indicators that can affect future results. The multiples used for these valuations are derived from observed ownership transactions for dialysis businesses between unrelated parties in the U.S. in recent years, and the specific valuation multiple applied to each dialysis partnership is principally determined by its recent and expected revenue mix and contribution margin. As of December 31, 2020,2023, an increase or decrease in the weighted average multiple used in these valuations of one times EBITDA would change the estimated fair value of these noncontrolling interests by approximately $160,000.$190,000. See Note 1716 for a discussion of the Company’s methodology for estimating the fair values of noncontrolling interests subject to put obligations.obligations and the reconciliation of changes on the consolidated statements of equity.
The Company's fair value estimates for its senior secured credit facilities and senior notes are based upon quoted bid and ask prices for these instruments, typically a level 2 input. See Note 1312 for further discussion of the Company's debt.
Other financial instruments consist primarily of cash and cash equivalents, restricted cash and cash equivalents, accounts receivable, accounts payable, other accrued liabilities, lease liabilities and debt. The balances of financial instruments other than debt and lease liabilities are presented in the consolidated financial statements at December 31, 20202023 and 20192022 at their approximate fair values due to the short-term nature of their settlements.
25.24. Segment reporting
The Company's operationsoperating divisions are comprisedcomposed of its U.S. dialysis and related lab services business (its U.S. dialysis business), its variousU.S. integrated kidney care business, its U.S. other ancillary services and strategic initiatives, including its international operations (collectively, its ancillary services), andas well as its corporate administrative support. See Note 1 "Organization" for a summary description of the Company's businesses.
On June 19, 2019, the Company completed the sale of its DMG business to Optum. As a result of this transaction, DMG's results of operations have been reported as discontinued operations for all periods presented.
The Company’s operating segments have been defined based on the separate financial information that is regularly produced and reviewed by the Company’s chief operating decision maker in making decisions about allocating resources to and assessing the financial performance of the Company’s various operating lines of business. The chief operating decision maker for the Company is its Chief Executive Officer.
The Company’s separate operating segments include its U.S. dialysis and related lab services business, each of its U.S. integrated kidney care business, its U.S. other ancillary services, and strategic initiatives, its kidney care operations in each foreign sovereign jurisdiction, its other health operations in each foreign sovereign jurisdiction, and its equity method investment in the APACits Asia Pacific joint venture.venture (APAC JV). The U.S. dialysis and related lab services business qualifies as a separately reportable segment, and all other ancillary services and strategic initiatives operating segments, including the international operating segments have been combined and disclosed in the other segments category.
The Company’s operating segment financial information included in this report is prepared on the internal management reporting basis that the chief operating decision maker uses to allocate resources and assess the financial performance of and allocate resources among the Company's operating segments. For internal management reporting, segment operations include direct segment operating expenses but generally exclude corporate administrative support costs, which consist primarily of indirect labor, benefits and long-term incentive compensation expenses of certain departments which provide support to allmore than one of the Company’s various operating lines of business, exceptbusiness. The chief operating decision maker uses segment operating margin to assess segment profitability. The chief operating decision maker does not use total assets by segment to make decisions regarding resources; therefore, the extent that such costs are charged to and bornetotal assets by certain ancillary services and strategic initiatives via internal management fees. These corporate administrative support costs are reduced by internal management fees received from the Company’s ancillary lines of business.segment disclosure has not been included.
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
The following is a summary of segment revenues, segment operating margin (loss), and a reconciliation of segment operating margin to consolidated income from continuing operations before income taxes:
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 |
| Segment revenues: | | | | | |
| U.S. dialysis | | | | | |
| Patient service revenues: | | | | | |
| External sources | $ | 10,488,731 | | | $ | 10,421,401 | | | $ | 10,274,046 | |
| Intersegment revenues | 144,091 | | | 131,199 | | | 92,950 | |
| U.S. dialysis revenues before provision | 10,632,822 | | | 10,552,600 | | | 10,366,996 | |
| Provision for uncollectible accounts | (13,458) | | | (21,715) | | | (50,927) | |
| U.S. dialysis patient service revenues | 10,619,364 | | | 10,530,885 | | | 10,316,069 | |
Other revenues(1) | | | | | |
| External sources | 39,376 | | | 30,895 | | | 19,880 | |
| Intersegment revenues | 1,195 | | | 1,126 | | | 0 | |
| Total U.S. dialysis revenues | $ | 10,659,935 | | | $ | 10,562,906 | | | $ | 10,335,949 | |
| Other - Ancillary services | | | | | |
| Net patient service revenues | 550,978 | | | 497,021 | | | 437,275 | |
| Other external sources | 484,977 | | | 460,877 | | | 724,577 | |
| Intersegment revenues | 16,743 | | | 14,030 | | | 34,236 | |
| Total ancillary services | 1,052,698 | | | 971,928 | | | 1,196,088 | |
| Total net segment revenues | 11,712,633 | | | 11,534,834 | | | 11,532,037 | |
| Elimination of intersegment revenues | (162,029) | | | (146,355) | | | (127,186) | |
| Consolidated revenues | $ | 11,550,604 | | | $ | 11,388,479 | | | $ | 11,404,851 | |
| Segment operating margin (loss): | | | | | |
| U.S. dialysis | $ | 1,917,604 | | | $ | 1,924,826 | | | $ | 1,709,721 | |
Other - Ancillary services(2) | (76,261) | | | (189,174) | | | (93,789) | |
| Total segment margin | 1,841,343 | | | 1,735,652 | | | 1,615,932 | |
Reconciliation of segment operating margin to consolidated income from
continuing operations before income taxes: | | | | | |
| Corporate administrative support | (146,707) | | | (92,335) | | | (90,108) | |
| Consolidated operating income | 1,694,636 | | | 1,643,317 | | | 1,525,824 | |
| Debt expense | (304,111) | | | (443,824) | | | (487,435) | |
| Debt prepayment, refinancing and redemption charges | (89,022) | | | (33,402) | | | 0 | |
| Other income | 16,759 | | | 29,348 | | | 10,089 | |
| Income from continuing operations before income taxes | $ | 1,318,262 | | | $ | 1,195,439 | | | $ | 1,048,478 | |
- | | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2023 | | 2022 | | 2021 |
| Segment revenues: | | | | | |
| U.S. dialysis | | | | | |
| Patient service revenues: | | | | | |
| External sources | $ | 10,823,525 | | | $ | 10,488,327 | | | $ | 10,551,106 | |
| Intersegment revenues | 88,222 | | | 87,045 | | | 90,512 | |
| U.S. dialysis patient service revenues | 10,911,747 | | | 10,575,372 | | | 10,641,618 | |
| Other revenues | | | | | |
| External sources | 25,251 | | | 24,447 | | | 25,061 | |
| Intersegment revenues | — | | | (10) | | | 284 | |
| Total U.S. dialysis revenues | 10,936,998 | | | 10,599,809 | | | 10,666,963 | |
| Other - Ancillary services | | | | | |
| Patient service revenues | 751,416 | | | 688,137 | | | 662,409 | |
| Other external sources | 539,955 | | | 408,983 | | | 380,221 | |
| Intersegment revenues | 7,852 | | | 4,206 | | | 4,294 | |
| Total ancillary services | 1,299,223 | | | 1,101,326 | | | 1,046,924 | |
| Total net segment revenues | 12,236,221 | | | 11,701,135 | | | 11,713,887 | |
| Elimination of intersegment revenues | (96,074) | | | (91,241) | | | (95,090) | |
| Consolidated revenues | $ | 12,140,147 | | | $ | 11,609,894 | | | $ | 11,618,797 | |
| Segment operating margin (loss): | | | | | |
| U.S. dialysis | $ | 1,774,578 | | | $ | 1,565,310 | | | $ | 1,974,988 | |
Other - Ancillary services(1) | (8,747) | | | (96,579) | | | (66,003) | |
| Total segment margin | 1,765,831 | | | 1,468,731 | | | 1,908,985 | |
Reconciliation of segment operating margin to consolidated income from
continuing operations before income taxes: | | | | | |
| Corporate administrative support | (163,047) | | | (129,669) | | | (111,615) | |
| Consolidated operating income | 1,602,784 | | | 1,339,062 | | | 1,797,370 | |
| Debt expense | (398,551) | | | (357,019) | | | (285,254) | |
| Debt extinguishment and modification costs | (7,962) | | | — | | | — | |
| Other (loss) income, net | (19,177) | | | (15,765) | | | 6,378 | |
| Income from continuing operations before income taxes | $ | 1,177,094 | | | $ | 966,278 | | | $ | 1,518,494 | |
(1)Includes management fee revenues from providing management and administrativeSegment operating loss for Other - Ancillary services to dialysis ventures in which the Company owns a noncontrolling interest or which are wholly-owned by third parties.
(2)Includesincludes equity investment incomeloss of $5,866, $9,366,$2,103, $1,898 and $24,866$3,177 in 2020, 20192023, 2022 and 2018,2021, respectively.
Depreciation and amortization expense by reportable segment was as follows:
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2023 | | 2022 | | 2021 |
| U.S. dialysis | $ | 695,674 | | | $ | 690,949 | | | $ | 642,711 | |
| Other - Ancillary services | 49,769 | | | 41,653 | | | 37,904 | |
| | $ | 745,443 | | | $ | 732,602 | | | $ | 680,615 | |
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
Depreciation and amortization expense by reportable segment was as follows:
| | | | | | | | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 | | 2018 |
| U.S. dialysis | $ | 594,552 | | | $ | 583,454 | | | $ | 558,810 | |
| Other - Ancillary services | 35,883 | | | 31,698 | | | 32,225 | |
| | $ | 630,435 | | | $ | 615,152 | | | $ | 591,035 | |
Summary of assets by reportable segment was as follows:
| | | | | | | | | | | |
| | Year ended December 31, |
| | 2020 | | 2019 |
| Segment assets | | | |
U.S. dialysis(1) | $ | 15,344,647 | | | $ | 15,778,880 | |
Other - Ancillary services(2) | 1,643,869 | | | 1,532,514 | |
| Consolidated assets | $ | 16,988,516 | | | $ | 17,311,394 | |
(1)Includes equity method and other investments of $122,974 and $124,188 in 2020 and 2019, respectively.
(2)Includes equity method and other investments of $134,517 and 117,795 in 2020 and 2019, respectively and includes approximately $181,137 and $154,572 in 2020 and 2019, respectively, of net property and equipment related to the Company’s international operations.
Expenditures for property and equipment by reportable segment were as follows:
| | | | Year ended December 31, | | Year ended December 31, |
| | | 2020 | | 2019 | | 2018 | | 2023 | | 2022 | | 2021 |
| U.S. dialysis | U.S. dialysis | 646,870 | | | $ | 681,339 | | | $ | 856,108 | |
| Other - Ancillary services | Other - Ancillary services | 27,671 | | | 46,741 | | | 45,806 | |
| DMG - Discontinued operations | 0 | | | 38,466 | | | 85,224 | |
| | | $ | 674,541 | | | $ | 766,546 | | | $ | 987,138 | |
| | |
| | |
| | |
The Company's international operations include approximately $240,742 and $207,162 in 2023 and 2022, respectively, of net property and equipment.
26.25. Supplemental cash flow information
The table below provides supplemental cash flow information:
| | | | Year ended December 31, | | Year ended December 31, |
| | | 2020 | | 2019 | | 2018 | | 2023 | | 2022 | | 2021 |
| Cash paid: | Cash paid: | | | | | | Cash paid: | | | |
| Income taxes, net | Income taxes, net | $ | 154,850 | | | $ | 157,983 | | | $ | 92,526 | |
| Interest | $ | 326,165 | | | $ | 473,176 | | | $ | 488,974 | |
| Interest, net | |
| Non-cash investing and financing activities: | Non-cash investing and financing activities: | | | | | | Non-cash investing and financing activities: | | | |
| Fixed assets under financing lease obligations | Fixed assets under financing lease obligations | $ | 22,042 | | | $ | 18,953 | | | $ | 8,828 | |
DAVITA INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS - (continued)
(dollars and shares in thousands, except per share data)
27. Selected quarterly financial data (unaudited)
| | | | | | | | | | | | | | | | | | | | | | | |
| December 31, | | September 30, | | June 30, | | March 31, |
| 2020 | | | | | | | |
| Total revenues | $ | 2,905,322 | | | $ | 2,924,066 | | | $ | 2,879,979 | | | $ | 2,841,237 | |
| Operating income | $ | 381,671 | | | $ | 437,669 | | | $ | 409,920 | | | $ | 465,376 | |
| Attributable to DaVita Inc.: | | | | | | | |
Net income from continuing operations(1) | $ | 193,406 | | | $ | 158,674 | | | $ | 201,602 | | | $ | 229,613 | |
| Net (loss) income from discontinued operations | (19,633) | | | 0 | | | 0 | | | 9,980 | |
| Net income | $ | 173,773 | | | $ | 158,674 | | | $ | 201,602 | | | $ | 239,593 | |
| Per share attributable to DaVita Inc.: | | | | | | | |
| Basic net income from continuing operations | $ | 1.73 | | | $ | 1.31 | | | $ | 1.65 | | | $ | 1.84 | |
| Basic net (loss) income from discontinued operations | (0.17) | | | 0 | | | 0 | | | 0.08 | |
| Basic net income | $ | 1.56 | | | $ | 1.31 | | | $ | 1.65 | | | $ | 1.92 | |
| Diluted net income from continuing operations | $ | 1.67 | | | $ | 1.28 | | | $ | 1.62 | | | $ | 1.81 | |
| Diluted net (loss) income from discontinued operations | (0.17) | | | 0 | | | 0 | | | 0.08 | |
| Diluted net income | $ | 1.50 | | | $ | 1.28 | | | $ | 1.62 | | | $ | 1.89 | |
| 2019 | | | | | | | |
| Total revenues | $ | 2,898,584 | | | $ | 2,904,078 | | | $ | 2,842,705 | | | $ | 2,743,112 | |
| Operating income | $ | 462,588 | | | $ | 378,336 | | | $ | 461,886 | | | $ | 340,507 | |
| Attributable to DaVita Inc.: | | | | | | | |
Net income from continuing operations(1) | $ | 242,242 | | | $ | 150,113 | | | $ | 194,223 | | | $ | 120,254 | |
| Net (loss) income from discontinued operations | 2,629 | | | (6,843) | | | 79,328 | | | 29,035 | |
| Net income | $ | 244,871 | | | $ | 143,270 | | | $ | 273,551 | | | $ | 149,289 | |
| Per share attributable to DaVita Inc.: | | | | | | | |
| Basic net income from continuing operations | $ | 1.87 | | | $ | 1.00 | | | $ | 1.17 | | | $ | 0.72 | |
| Basic net income (loss) from discontinued operations | 0.02 | | | (0.05) | | | 0.47 | | | 0.18 | |
| Basic net income | $ | 1.89 | | | $ | 0.95 | | | $ | 1.64 | | | $ | 0.90 | |
| Diluted net income from continuing operations | $ | 1.86 | | | $ | 0.99 | | | $ | 1.16 | | | $ | 0.72 | |
| Diluted net income (loss) from discontinued operations | 0.02 | | | (0.04) | | | 0.48 | | | 0.18 | |
| Diluted net income | $ | 1.88 | | | $ | 0.95 | | | $ | 1.64 | | | $ | 0.90 | |
(1)The following table summarizes impairment charges, loss on changes in ownership interest, and a legal settlement included in operating expenses and charges in 2020 and 2019 by quarter:
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| Quarter ended | | Quarter ended |
| December 31,
2020 | | September 30,
2020 | | June 30,
2020 | | March 31,
2020 | | December 31,
2019 | | September 30,
2019 | | June 30,
2019 | | March 31,
2019 |
Certain operating expenses
and charges: | | | | | | | | | | | | | | | |
| Impairment charges | | | | | | | | | | | $ | 83,855 | | | | | $ | 41,037 | |
Loss on changes in
ownership interest, net | | | | | $ | 16,252 | | | | | | | | | | | |
| Accruals for legal matters | | | | | $ | 35,000 | | | | | | | | | | | |
| | | | | | | | | | | | | | | |
| | | | | | | | | | | | | | | |
EXHIBIT INDEX
| | | | | | | | |
| | Equity Purchase Agreement, dated as of December 5, 2017, by and among DaVita Inc., Collaborative Care Holdings, LLC, and solely with respect to Section 9.3 and Section 9.18 thereto, UnitedHealth Group Incorporated.(2) |
| | |
| | Amendment No. 1 dated as of September 20, 2018, to that certain Equity Purchase Agreement, dated as of December 5, 2017, by and among DaVita Inc., a Delaware corporation, Collaborative Care Holdings, LLC, a Delaware limited liability company and a wholly owned subsidiary of Optum, Inc., and solely with respect to Section 9.3 and Section 9.18 thereto, UnitedHealth Group Incorporated, a Delaware corporation.(22)(14) |
| | |
| | Second Amendment to Equity Purchase Agreement by and between DaVita Inc., a Delaware corporation, and Collaborative Care Holdings, LLC, a Delaware limited liability company, dated as of December 11, 2018, amending that certain Equity Purchase Agreement, dated as of December 5, 2017, by and among DaVita Inc., Collaborative Care Holdings, LLC, and, solely with respect to Section 9.3 and Section 9.18 thereto, UnitedHealth Group Incorporated (as previously amended).(11)(9) |
| | |
| | Amended and Restated Certificate of Incorporation of DaVita Inc., as filed with the Secretary of State of Delaware on November 1, 2016.(1) |
| | |
| | Amended and Restated Bylaws for DaVita Inc. dated as of December 10, 2020.(33)adopted on October 14, 2022.(23) |
| | |
| | Indenture for the 4.625% Senior Notes due 2030, dated as of June 9, 2020, by and among DaVita Inc., the subsidiary guarantors party thereto and The Bank of New York Mellon Trust Company, N.A., as Trustee.(20)(13) |
| | |
| | Form of 4.625% Senior Notes due 2030 and related Guarantee (included in Exhibit 4.1).(20)(13) |
| | |
| | Indenture for the 3.750% Senior Notes due 2031, dated August 11, 2020, by and among DaVita Inc., the subsidiary guarantors party thereto and The Bank of New York Mellon Trust Company, N.A., as Trustee.(17)(11) |
| | | |
| | Form of 3.750% Senior Notes due 2031 and related Guarantee (included in Exhibit 4.3).(17)(11) |
| | |
| | Description of Securities.(28)(20) |
| | |
| | Sourcing and Supply Agreement between DaVita Inc. and Amgen USA Inc. effective as of January 6, 2017.(5)** |
| | |
| | Credit Agreement, dated August 12, 2019, by and among DaVita Inc., certain subsidiary guarantors party thereto, the lenders party thereto, Credit Agricole Corporate and Investment Bank, JPMorgan Chase Bank, N.A. and MUFG Bank Ltd., as co-syndication agents, Bank of America, N.A., Barclays Bank PLC, Credit Suisse Loan Funding LLC, Goldman Sachs Bank USA, Morgan Stanley Senior Funding, Inc. and Suntrust Bank, as co-documentation agents, and Wells Fargo Bank, National Association, as administrative agent, collateral agent and swingline lender.(24)(16) |
| | |
| | First Amendment, dated as of February 13, 2020, to that certain Credit Agreement, dated as of August 12, 2019, by and among DaVita Inc., certain subsidiary guarantors party thereto, the lenders party thereto, and Wells Fargo Bank, National Association, as administrative agent, collateral agent and swingline lender.(28)(20) |
| | |
| | Second Amendment, dated as of April 3, 2023, to that certain Credit Agreement, dated as of August 12, 2019, by and among DaVita Inc., certain subsidiary guarantors party thereto, the lenders party thereto, and Wells Fargo Bank, National Association, as administrative agent, collateral agent and swingline lender.(25) |
| | |
| | EmploymentThird Amendment, dated as of April 28, 2023, to that certain Credit Agreement, effective July 25, 2008, betweendated as of August 12, 2019, by and among DaVita Inc., certain subsidiary guarantors party thereto, the lenders party thereto, and Kent J. Thiry.(12)*Wells Fargo Bank, National Association, as administrative agent, collateral agent and swingline lender.(24) |
| | |
| | Amendment to Employment Agreement, effective December 31, 2014, by and between DaVita Inc. and Kent. J. Thiry.(3)* |
| | |
| | Amendment Number Two to Employment Agreement, effective August 20, 2018, by and between DaVita Inc. and Kent J. Thiry.(23)* |
| | |
| | | | | | | | |
| | Executive Chairman Agreement between Kent J. Thiry and DaVita, Inc., dated as of April 29, 2019.(13)* |
| | |
| | Restricted Stock Units Agreement, effective as of May 15, 2019, by and between DaVita Inc. and Kent Thiry.(25)* |
| | |
| | Performance Stock Units Agreement, effective as of May 15, 2019, by and between DaVita Inc. and Kent Thiry.(25)* |
| | |
| | Employment Agreement, dated as of April 29, 2019, by and between Javier J. Rodriguez and DaVita Inc.(13)(10)* |
| | |
| | | | | | | | |
| | Stock Appreciation Rights Agreement, effective November 4, 2019, by and between Javier J. Rodriguez and DaVita Inc.(27)(19)* |
| | |
| | Employment Agreement, effective February 21, 2017, by and between DaVita Inc. and Joel Ackerman.(8)(6)* |
| | |
| | Employment Agreement, effective April 27, 2016, by and between DaVita HealthCare Partners Inc. and Kathleen A. Waters.(5)(4)* |
| | |
| | Employment Agreement, effective September 22, 2005, by and between DaVita Inc. and James Hilger.(7)* |
| | |
| | Amendment to Mr. Hilger’s Employment Agreement, effective December 12, 2008.(15)* |
| | |
| | Second Amendment to Mr. Hilger’s Employment Agreement, effective December 27, 2012.(18)* |
| | |
| | Third Amendment to Employment Agreement, effective December 31, 2014, by and between DaVita Inc. and James Hilger.(3)* |
| | |
| | Transition Agreement, dated as of July 31, 2018, by and between DaVita Inc. and James Hilger.(21)* |
| | |
| | Employment Agreement, effective April 29, 2015, by and between DaVita HealthCare Partners Inc. and Michael Staffieri.(28)(20)* |
| | |
| | Amendment to Stock Appreciation Rights Agreements, effective June 11, 2020, by and between DaVita Inc. and William L. Roper, M.D.(30)* |
| | |
| | Transition Agreement, dated October 1, 2020, by and between DaVita Inc. and LeAnne Zumwalt.(32)* |
| | |
| | Form of Indemnity Agreement.(10)(8)* |
| | |
| | Form of Indemnity Agreement.(6)(5)* |
| | |
| | DaVita Inc. Deferred Compensation Plan.(8)(6)* |
| | |
| | DaVita Voluntary Deferral Plan.(4)* |
| | |
| | Deferred Bonus Plan (Prosperity Plan).(14)* |
| | |
| | Amendment No. 1 to Deferred Bonus Plan (Prosperity Plan).(15)* |
| | |
| | Amended and Restated Employee Stock Purchase Plan.(26)(18)* |
| | |
| | DaVita Inc. Severance Plan for Directors and Above.(3)* |
| | |
| | | | | | | | |
| | DaVita Inc. Non-Employee Director Compensation Policy.(16)(15)* |
| | |
| | Amended and Restated DaVita Inc. 2011 Incentive Award Plan.(9)(7)* |
| | |
| | Amendment No. 1 to the Amended and Restated DaVita Inc. 2011 Incentive Award Plan.(27)(19)* |
| | |
| | DaVita Inc. 2020 Incentive Award Plan.(29)* |
| | |
| | DaVita Inc. Rule of 65 Policy, adopted on August 19, 2018.(23)* |
| | |
| | Form of Stock Appreciation Rights Agreement-Board members (DaVita Inc. 2011 Incentive Award Plan).(21)* |
| | |
| | Form of Stock Appreciation Rights Agreement-Executives (DaVita Inc. 2011 Incentive Award Plan).(18)(12)* |
| | |
| | Form of Restricted Stock Units Agreement-Executives (DaVita Inc. 2011 Incentive Award Plan).(19)(17)* |
| | |
| | Form of Long-Term Incentive Program Award Agreement (For 162(m) designated teammates)Stock Appreciation Rights Agreement-Executives (DaVita Inc. 2011 Incentive Award Plan).(18)(17)* |
| | |
| | Form of Long-Term Incentive Program Award Agreement (DaVita Inc. 2011 Incentive Award Plan).(18)* |
| | |
| | Form of Restricted Stock Units Agreement-Executives (DaVita Inc. 2011 Incentive Award Plan).(25)(17)* |
| | |
| | Form of Performance Stock Units Agreement-Executives (DaVita Inc. 2011 Incentive Award Plan).(25)* |
| | |
| | Form of Stock Appreciation Rights Agreement-Executives (DaVita Inc. 2011 Incentive Award Plan).(25)(17)* |
| | |
| | Form of Restricted Stock Units Agreement-Executives (DaVita Inc. 2011 Incentive Award Plan).(25)* |
| | |
| | Form of Performance Stock Units Agreement-Executives (DaVita Inc. 2011 Incentive Award Plan).(25)* |
| | |
| | Form of Stock Appreciation Rights Agreement-Executives (DaVita Inc. 2011 Incentive Award Plan).(25)* |
| | |
| | Form of Stock Appreciation Rights Agreement (DaVita Inc. 2020 Incentive Award Plan).(31)(22)* |
| | |
| | Form of Performance-Based Restricted Stock Unit Agreement (DaVita Inc. 2020 Incentive Award Plan).(31)(22)* |
| | |
| | Form of Restricted Stock Unit Agreement (DaVita Inc. 2020 Incentive Award Plan).(31)(22)* |
| | |
| | Form of Performance Award Agreement (DaVita Inc. 2020 Incentive Award Plan).(15)* |
| | |
| | Form of Stock Appreciation Rights Agreement (DaVita Inc. 2020 Incentive Award Plan).(25)* |
| | |
| | Form of Performance-Based Restricted Stock Unit Agreement (DaVita Inc. 2020 Incentive Award Plan).(25)* |
| | |
| | Form of Restricted Stock Unit Agreement (DaVita Inc. 2020 Incentive Award Plan).(25)* |
| | | | | | | | |
| | |
| | List of our subsidiaries.ü |
| | |
| | Consent of KPMG LLP, independent registered public accounting firm.ü |
| | |
| | Powers of Attorney with respect to DaVita.DaVita Inc. (Included on Page S-1). |
| | |
| | Certification of the Chief Executive Officer, dated February 12, 2021,14, 2024, pursuant to Rule 13a-14(a) or 15d-14(a), as adopted pursuant to Section 302 of the Sarbanes-Oxley Act of 2002.ü |
| | |
| | Certification of the Chief Financial Officer, dated February 12, 2021,14, 2024, pursuant to Rule 13a-14(a) or 15d-14(a), as adopted pursuant to Section 302 of the Sarbanes-Oxley Act of 2002.ü |
| | |
| | | | | | | | |
| | Certification of the Chief Executive Officer, dated February 12, 2021,14, 2024, pursuant to 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002.ü |
| | | |
| | Certification of the Chief Financial Officer, dated February 12, 2021,14, 2024, pursuant to 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002.ü |
| | |
| | DaVita Inc. Dodd-Frank Policy on Recoupment of Incentive Compensation.ü* |
| | |
| 101.INS | | XBRL Instance Document - the Instance Document does not appear in the Interactive Data File because its XBRL tags are embedded within the Inline XBRL document.ü |
| | | |
| 101.SCH | | Inline XBRL Taxonomy Extension Schema Document.ü |
| | |
| 101.CAL | | Inline XBRL Taxonomy Extension Calculation Linkbase Document.ü |
| | | |
| 101.DEF | | Inline XBRL Taxonomy Extension Definition Linkbase Document.ü |
| | | |
| 101.LAB | | Inline XBRL Taxonomy Extension Label Linkbase Document.ü |
| | | |
| 101.PRE | | Inline XBRL Taxonomy Extension Presentation Linkbase Document.ü |
| | |
| 104 | | Cover Page Interactive Data File (formatted as Inline XBRL and contained in Exhibit 101).ü |
| | | | | |
| ü | Included in this filing. |
| * | Management contract or executive compensation plan or arrangement. |
** | Portions of this exhibit are subject to a request for confidential treatment and have been redacted and filed separately with the SEC. |
(1)Filed on November 2, 2016June 8, 2023 as an exhibit to the Company’s QuarterlyCompany's Current Report on Form 10-Q for the quarter ended September 30, 2016.8-K.
(2)Filed on December 6, 2017 as an exhibit to the Company’s Current Report on Form 8-K.
(3)Filed on February 22, 2019 as an exhibit to the Company’s Annual Report on Form 10-K for the year ended December 31, 2018.
(4)Filed on November 8, 2005October 28, 2021 as an exhibit to the Company’s Quarterly Report on Form 10-Q for the quarter ended September 30, 2005.2021.
(5)(4)Filed on May 2, 2017 as an exhibit to the Company’s Quarterly Report on 10-Q for the quarter ended March 31, 2017.
(6)(5)Filed on March 3, 2005 as an exhibit to the Company’s Annual Report on Form 10-K for the year ended December 31, 2004.
(7)Filed on August 7, 2006 as an exhibit to the Company’s Quarterly Report on Form 10-Q for the quarter ending June 30, 2006.
(8)(6)Filed on February 24, 2017 as an exhibit to the Company’s Annual Report on Form 10-K for the year ended December 31, 2016.
(9)(7)Filed on April 28, 2014 as Appendix Aan appendix to the Company's Definitive Proxy Statement on Schedule 14A.
(10)(8)Filed on December 20, 2006 as an exhibit to the Company’s Current Report on Form 8-K.
(11)(9)Filed on December 17, 2018 as an exhibit to the Company’s Current Report on Form 8-K.
(12)Filed on July 31, 2008 as an exhibit to the Company’s Current Report on Form 8-K.
(13)(10)Filed on April 29, 2019 as an exhibit to the Company's Current Report on Form 8-K.
(14)Filed on February 29, 2008 as an exhibit to the Company’s Annual Report on Form 10-K for the year ended December 31, 2007.
(15)Filed on February 27, 2009 as an exhibit to the Company’s Annual Report on Form 10-K for the year ended December 31, 2008.
(16)Filed on May 5, 2020 as an exhibit to the Company's Quarterly Report on Form 10-Q for the quarter ended March 31, 2020.
(17)(11)Filed on August 11, 2020 as an exhibit to the Company’s Current Report on Form 8-K.
(12)Filed on March 1, 2013 as an exhibit to the Company’s Annual Report on Form 10-K for the year ended December 31, 2012.
(19)Filed on August 4, 2011 as an exhibit to the Company's Quarterly Report on Form 10-Q for the quarter ended June 30, 2011.
(20)(13)Filed on June 9, 2020 as an exhibit to the Company's Current Report on Form 8-K.
(21)Filed on August 1, 2018 as an exhibit to the Company’s Quarterly Report on Form 10-Q for the quarter ended June 30, 2018.
(22)(14)Filed on September 24, 2018 as an exhibit to the Company’s Current Report on Form 8-K.
(23)(15)Filed on August 23, 2018February 22, 2023 as an exhibit to the Company’s CurrentCompany's Annual Report on Form 8-K.10-K for the year ended December 31, 2022.
(24)(16)Filed on August 14, 2019 as an exhibit to the Company’s Current Report on Form 8-K.
(25)(17)Filed on July 22, 2019 as an exhibit to the Company’s Tender Offer Statement on Schedule TO-I.
(26)(18)Filed on May 10, 2016 as an appendix to the Company's Proxy Statement on DEF 14A.
(27)(19)Filed on December 6, 2019 as an appendix to the Company's Proxy Statement on DEF 14A.
(28)(20)Filed on February 21, 2020 as an exhibit to the Company’s Annual Report on Form 10-K for the year ended December 31, 2019.
(29)(21)Filed on April 27, 2020 as an appendix to the Company's Proxy Statement on DEF 14A.
(30)Filed on July 30, 2020 as an exhibit to the Company’s Quarterly Report on Form 10-Q for the quarter ended June 30, 2020.
(31)(22)Filed on August 17, 2020 as an exhibit to the Company’s Tender Offer Statement on Schedule TO-I.
(32)(23)Filed on October 29, 2020 as an exhibit to the Company’s Quarterly Report on Form 10-Q for the quarter ended September 30, 2020.
(33)Filed on December 10, 202018, 2022 as an exhibit to the Company’s Current Report on Form 8-K.
(24)Filed on May 1, 2023 as an exhibit to the Company's Current Report on Form 8-K.
(25)Filed on May 8, 2023 as an exhibit to the Company's Quarterly Report on Form 10-Q for the quarter ended March 31, 2023.
SIGNATURES
Pursuant to the requirements of Section 13 or 15(d) of the Securities Exchange Act of 1934, we have duly caused this Annual Report on Form 10-K to be signed on our behalf by the undersigned, thereunto duly authorized, in the City of Denver, State of Colorado, on February 12, 2021.14, 2024.
| | | | | | | | |
| DAVITA INC. |
| | | |
| By: | | /S/ JAVIER J. RODRIGUEZ |
| | | Javier J. Rodriguez
Chief Executive Officer |
KNOW ALL MEN BY THESE PRESENT, that each person whose signature appears below constitutes and appoints Javier J. Rodriguez, Joel Ackerman, and Kathleen Waters, and each of them his or her true and lawful attorneys-in-fact and agents with full power of substitution and resubstitution, for him or her and in his or her name, place and stead, in any and all capacities, to sign any and all amendments to this Annual Report on Form 10-K, and to file the same, with all exhibits thereto, and other documents in connection therewith, with the Securities and Exchange Commission, granting unto said attorneys-in-fact and agents, and each of them, full power and authority to do and perform each and every act and thing requisite or necessary to be done in and about the premises, as fully to all intents and purposes as he or she might or could do in person, hereby ratifying and confirming all that said attorneys-in-fact and agents or any of them, or their or his or her substitute or substitutes, may lawfully do or cause to be done by virtue hereof.
Pursuant to the requirements of the Securities Exchange Act of 1934, this Annual Report on Form 10-K has been signed by the following persons on behalf of the registrant and in the capacities and on the dates indicated.
| | | | | | | | | | | | | | |
| Signature | | Title | | Date |
| | | |
/S/ JAVIER J. RODRIGUEZ | | Chief Executive Officer and Director | | February 12, 202114, 2024 |
| Javier J. Rodriguez | | (Principal Executive Officer) | | |
| | | |
/S/ JOEL ACKERMAN | | Chief Financial Officer and Treasurer | | February 12, 202114, 2024 |
| Joel Ackerman | | (Principal Financial Officer) | | |
| | | |
/S/ JCOHNHRISTOPHER D. WM. BINSTELERRY | | Chief Accounting Officer | | February 12, 202114, 2024 |
John D. WinstelChristopher M. Berry | | (Principal Accounting Officer) | | |
| | | | | |
/S/ PAMELA M. ARWAY | | Director | | February 12, 202114, 2024 |
| Pamela M. Arway | | | | |
| | | |
/S/ CHARLES G. BERG | | Director | | February 12, 202114, 2024 |
| Charles G. Berg | | | | |
| | | |
/S/ BARBARA J. DESOER | | Director | | February 12, 202114, 2024 |
| Barbara J. Desoer | | | | |
| | | |
/S/ PJAULASON M. HOLLAR | | Director | | February 14, 2024 |
| Jason M. Hollar | | | | |
| | | | |
/S/ GREGORY J. DMIAZOORE | | Director | | February 12, 202114, 2024 |
PaulGregory J. Diaz | | | | |
| | |
/S/ SHAWN M. GUERTIN
| | Director | | February 12, 2021 |
Shawn M. GuertinMoore | | | | |
| | | |
/S/ JOHN M. NEHRA | | Director | | February 12, 202114, 2024 |
| John M. Nehra | | | | |
| | | | | |
/S/ PAAULADAM A. PH. SRICECHECHTER | | Director | | February 12, 202114, 2024 |
Paula A. PriceAdam H. Schechter | | | | |
| | | | |
/S/ WENDY L. SCHOPPERT | | Director | | February 14, 2024 |
| Wendy L. Schoppert | | | | |
| | | | |
/S/ PHYLLIS R. YALE | | Director | | February 12, 202114, 2024 |
| Phyllis R. Yale | | | | |
DAVITA INC.
SCHEDULE II—VALUATION AND QUALIFYING ACCOUNTS
��
| | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | | |
| | Balance at
beginning of year | | Acquisitions | | Amounts
charged to income | | Amounts written off | | Balance
at end of year |
| Description | | | | | |
| | | (dollars in thousands) |
| Allowance for uncollectible accounts: | | | | | | | | | | |
| Year ended December 31, 2020 | | $ | 8,328 | | | $ | 0 | | | $ | 13,458 | | | $ | 21,786 | | | $ | 0 | |
| Year ended December 31, 2019 | | $ | 52,924 | | | $ | 0 | | | $ | 21,715 | | | $ | 66,311 | | | $ | 8,328 | |
| Year ended December 31, 2018 | | $ | 218,399 | | | $ | 0 | | | $ | 42,287 | | | $ | 207,762 | | | $ | 52,924 | |