
Corporate Overview December 2016 Exhibit 99.1

This presentation contains certain forward-looking statements about Curis, Inc. (“we,” “us,” or the “Company”) that are intended to be covered by the safe harbor for “forward-looking statements” provided by the Private Securities Litigation Reform Act of 1995, as amended. Words such as “expect(s),” “feel(s),” “believe(s),” “will,” “may,” “anticipate(s)” and similar expressions are intended to identify forward-looking statements. Forward-looking statements are statements that are not historical facts, reflect management’s expectations as of the date of this presentation, and involve certain risks and uncertainties. Forward-looking statements include, but are not limited to, statements herein with respect to the timing and results of future clinical and pre-clinical milestones; the timing of future preclinical studies and clinical trials and results of these studies and trials; the clinical and therapeutic potential of our drug candidates; our ability to successfully develop and commercialize our drug candidates; the sufficiency of our current cash position to fund our operations; our expectations regarding the need for additional capital; and management’s ability to successfully achieve its goals. These forward-looking statements are based on our current expectations and may differ materially from actual results due to a variety of factors including, without limitation, whether any of our drug candidates will advance further in the clinical development process and whether and when, if at all, they will receive approval from the U.S. Food and Drug Administration or equivalent foreign regulatory agencies; whether historical preclinical results will be predictive of future clinical trial results; whether historical clinical trial results will be predictive of future trial results; whether any of our drug candidate discovery and development efforts will be successful; whether any of our drug candidates will be successfully marketed if approved; our ability to achieve the benefits contemplated by our collaboration agreements; management’s ability to successfully achieve its goals; our ability to raise additional capital to fund our operations on terms acceptable to us; general economic conditions; competition; and the other risk factors contained in our periodic and interim reports filed with the Securities and Exchange Commission which are available on the SEC website at www.sec.gov. You are cautioned not to place undue reliance on these forward-looking statements that speak only as of the date hereof, and we do not undertake any obligation to revise and disseminate forward-looking statements to reflect events or circumstances after the date hereof, or to reflect the occurrence of or non-occurrence of any events, except as required by law. Forward Looking Statements

Mission: Innovative Medicines to Treat Cancer Effectively Precision Oncology Oncology-Focused Biotech Publicly traded (NASDAQ: CRIS) based in Lexington, MA 62 full-time employees, expertise in clinical development and translational research Pipeline of differentiated small molecule cancer drug candidates Partnerships: Aurigene, Genentech/Roche Immuno-oncology
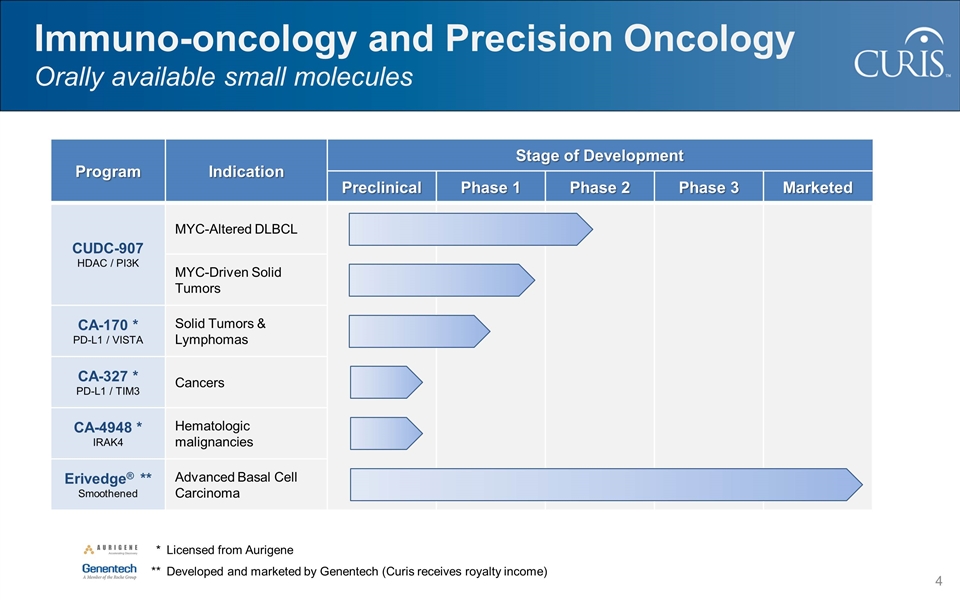
Program Indication Stage of Development Preclinical Phase 1 Phase 2 Phase 3 Marketed CUDC-907 HDAC / PI3K MYC-Altered DLBCL MYC-Driven Solid Tumors CA-170 * PD-L1 / VISTA Solid Tumors & Lymphomas CA-327 * PD-L1 / TIM3 Cancers CA-4948 * IRAK4 Hematologic malignancies Erivedge® ** Smoothened Advanced Basal Cell Carcinoma Immuno-oncology and Precision Oncology Orally available small molecules * Licensed from Aurigene **Developed and marketed by Genentech (Curis receives royalty income)

Curis Immuno-oncology Small molecule design to target interactions between B7 Ig family Majority of inhibitory immune checkpoint proteins belong to this subfamily Shared common folding structure in the extracellular domain Sufficient sites for design and docking of small molecules Multi-year, exclusive collaboration with Aurigene Curis option to royalty-bearing license for multiple programs Current Targets of interest PD-L1Expressed on immune and tumor cells – binds PD-1 and inhibits T cell activation VISTAExpressed on myeloid cells, including MDSCs TIM3Co-expressed along with PD-1 and marks the most exhausted CD8+ T cells Canonical Ig family 3D structure
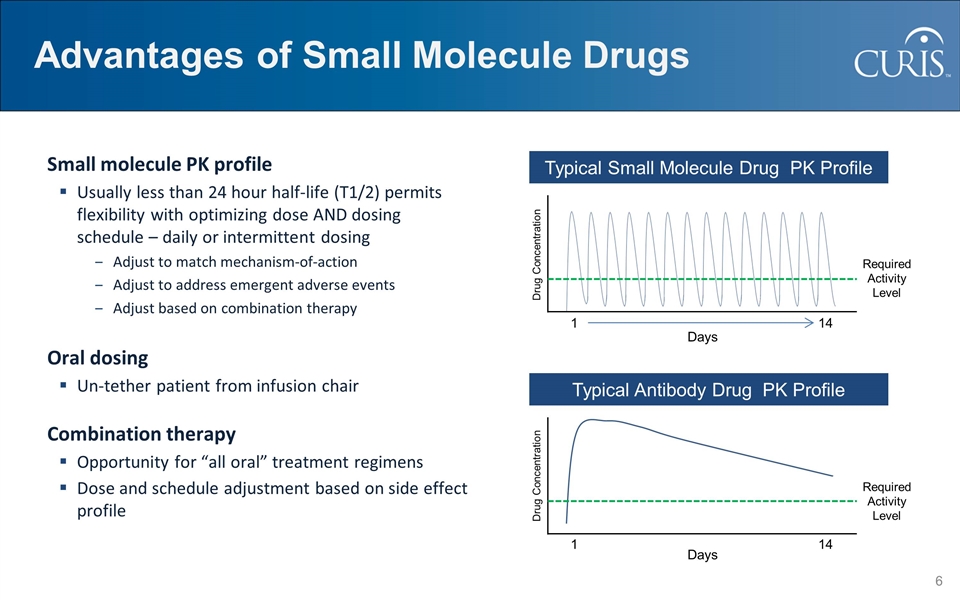
Advantages of Small Molecule Drugs Drug Concentration Required Activity Level Required Activity Level Days Drug Concentration Days Small molecule PK profile Usually less than 24 hour half-life (T1/2) permits flexibility with optimizing dose AND dosing schedule – daily or intermittent dosing Adjust to match mechanism-of-action Adjust to address emergent adverse events Adjust based on combination therapy Oral dosing Un-tether patient from infusion chair Combination therapy Opportunity for “all oral” treatment regimens Dose and schedule adjustment based on side effect profile Typical Small Molecule Drug PK Profile Typical Antibody Drug PK Profile 1 14 1 14
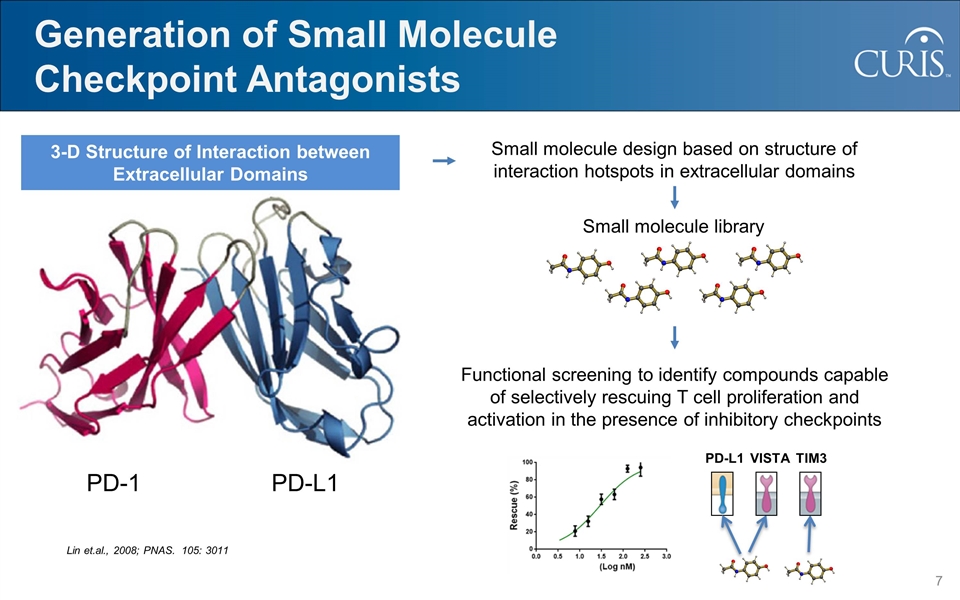
Generation of Small Molecule Checkpoint Antagonists Small molecule design based on structure of interaction hotspots in extracellular domains Small molecule library Functional screening to identify compounds capable of selectively rescuing T cell proliferation and activation in the presence of inhibitory checkpoints VISTA TIM3 PD-L1 PD-1 PD-L1 Lin et.al., 2008; PNAS. 105: 3011 3-D Structure of Interaction between Extracellular Domains

CA-170 is a first-in-class oral small molecule immune checkpoint inhibitor In Phase 1 clinical development CA-170 Oral, small molecule checkpoint inhibitor – PDL1 and VISTA Program Indication Stage of Development Preclinical Phase 1 Phase 2 Phase 3 Marketed CA-170 * PD-L1 / VISTA Solid Tumors & Lymphomas
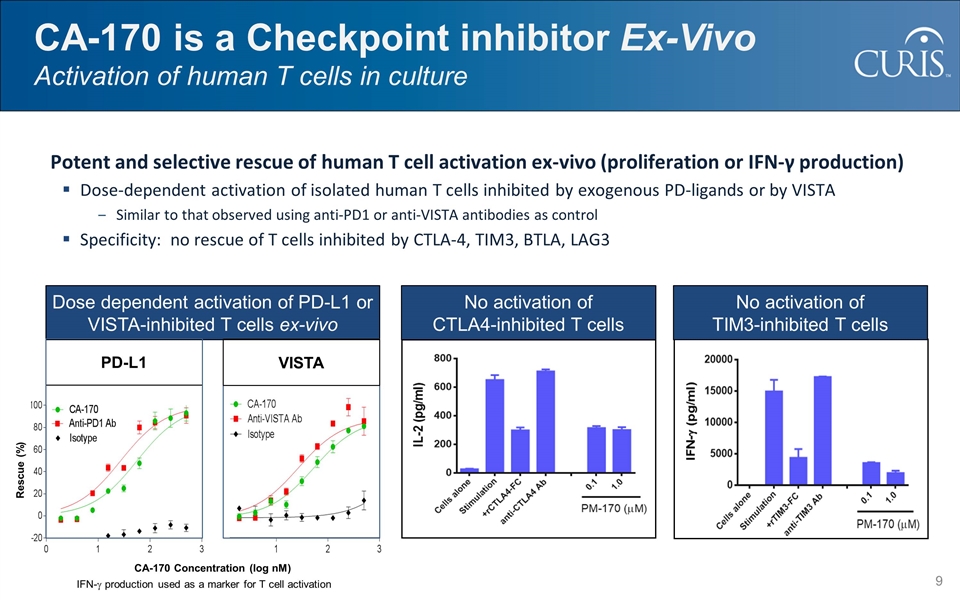
CA-170 is a Checkpoint inhibitor Ex-Vivo Activation of human T cells in culture Dose dependent activation of PD-L1 or VISTA-inhibited T cells ex-vivo PD-L1 Rescue (%) IFN-g production used as a marker for T cell activation CA-170 Concentration (log nM) VISTA No activation of CTLA4-inhibited T cells No activation of TIM3-inhibited T cells Potent and selective rescue of human T cell activation ex-vivo (proliferation or IFN-γ production) Dose-dependent activation of isolated human T cells inhibited by exogenous PD-ligands or by VISTA Similar to that observed using anti-PD1 or anti-VISTA antibodies as control Specificity: no rescue of T cells inhibited by CTLA-4, TIM3, BTLA, LAG3
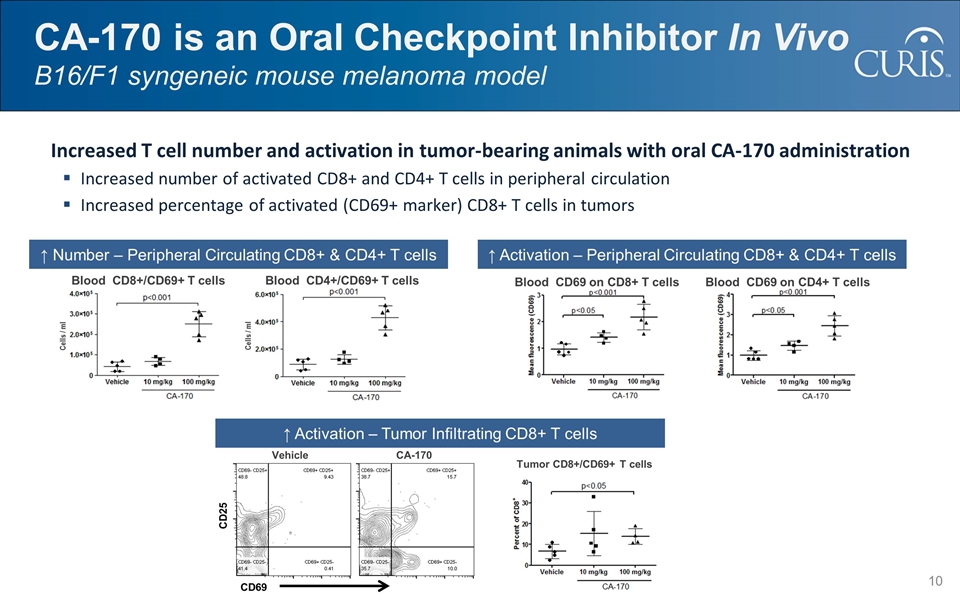
CA-170 is an Oral Checkpoint Inhibitor In Vivo B16/F1 syngeneic mouse melanoma model Increased T cell number and activation in tumor-bearing animals with oral CA-170 administration Increased number of activated CD8+ and CD4+ T cells in peripheral circulation Increased percentage of activated (CD69+ marker) CD8+ T cells in tumors ↑ Activation – Tumor Infiltrating CD8+ T cells Tumor CD8+/CD69+ T cells ↑ Number – Peripheral Circulating CD8+ & CD4+ T cells Cells / ml Blood CD8+/CD69+ T cells Cells / ml Blood CD4+/CD69+ T cells ↑ Activation – Peripheral Circulating CD8+ & CD4+ T cells Blood CD69 on CD4+ T cells Blood CD69 on CD8+ T cells CD25 CD69 Vehicle CA-170
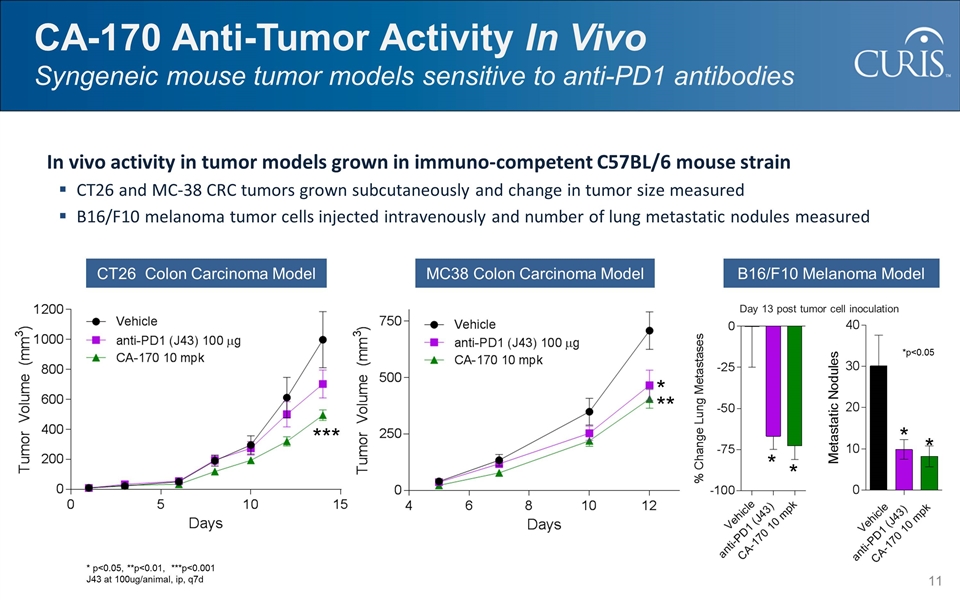
CA-170 Anti-Tumor Activity In Vivo Syngeneic mouse tumor models sensitive to anti-PD1 antibodies CT26 Colon Carcinoma Model B16/F10 Melanoma Model MC38 Colon Carcinoma Model * ** *** * * * * In vivo activity in tumor models grown in immuno-competent C57BL/6 mouse strain CT26 and MC-38 CRC tumors grown subcutaneously and change in tumor size measured B16/F10 melanoma tumor cells injected intravenously and number of lung metastatic nodules measured Day 13 post tumor cell inoculation *p<0.05 * p<0.05, **p<0.01, ***p<0.001 J43 at 100ug/animal, ip, q7d
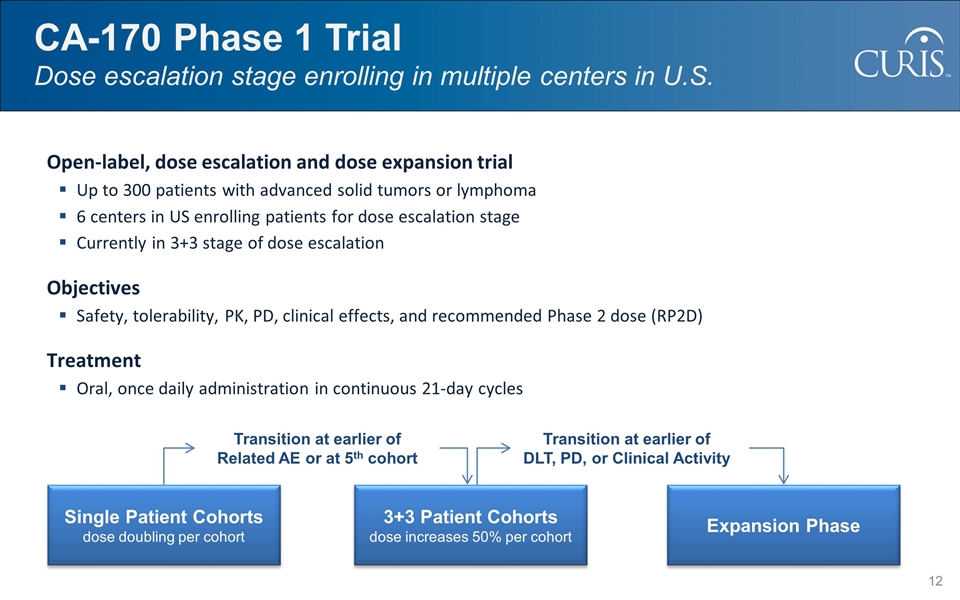
CA-170 Phase 1 Trial Dose escalation stage enrolling in multiple centers in U.S. Open-label, dose escalation and dose expansion trial Up to 300 patients with advanced solid tumors or lymphoma 6 centers in US enrolling patients for dose escalation stage Currently in 3+3 stage of dose escalation Objectives Safety, tolerability, PK, PD, clinical effects, and recommended Phase 2 dose (RP2D) Treatment Oral, once daily administration in continuous 21-day cycles Transition at earlier of Related AE or at 5th cohort Single Patient Cohorts dose doubling per cohort 3+3 Patient Cohorts dose increases 50% per cohort Expansion Phase Transition at earlier of DLT, PD, or Clinical Activity
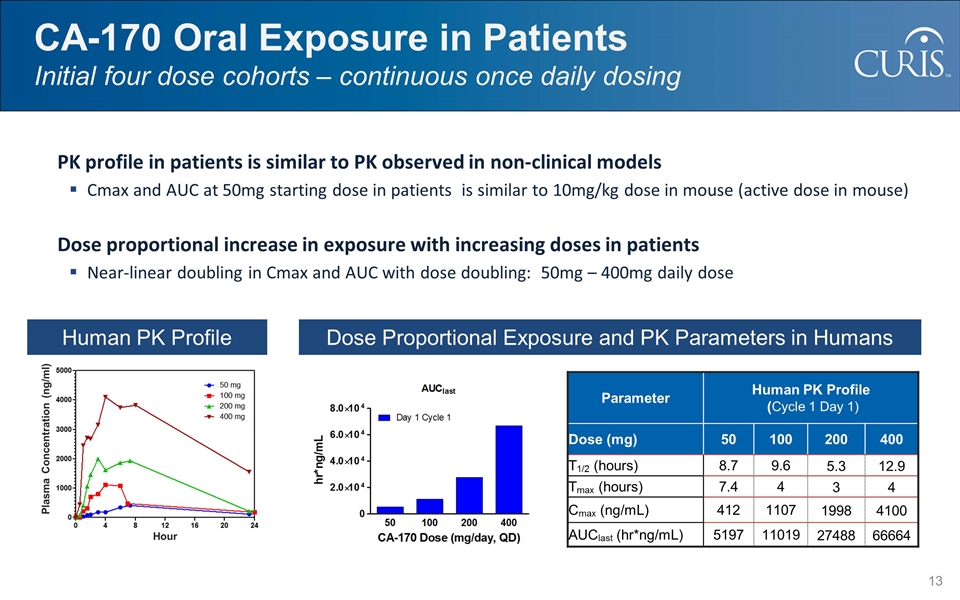
CA-170 Oral Exposure in Patients Initial four dose cohorts – continuous once daily dosing PK profile in patients is similar to PK observed in non-clinical models Cmax and AUC at 50mg starting dose in patients is similar to 10mg/kg dose in mouse (active dose in mouse) Dose proportional increase in exposure with increasing doses in patients Near-linear doubling in Cmax and AUC with dose doubling: 50mg – 400mg daily dose Parameter Human PK Profile (Cycle 1 Day 1) Dose (mg) 50 100 200 400 T1/2 (hours) 8.7 9.6 5.3 12.9 Tmax (hours) 7.4 4 3 4 Cmax (ng/mL) 412 1107 1998 4100 AUClast (hr*ng/mL) 5197 11019 27488 66664 Human PK Profile Dose Proportional Exposure and PK Parameters in Humans Plasma Concentration (ng/ml) Hour
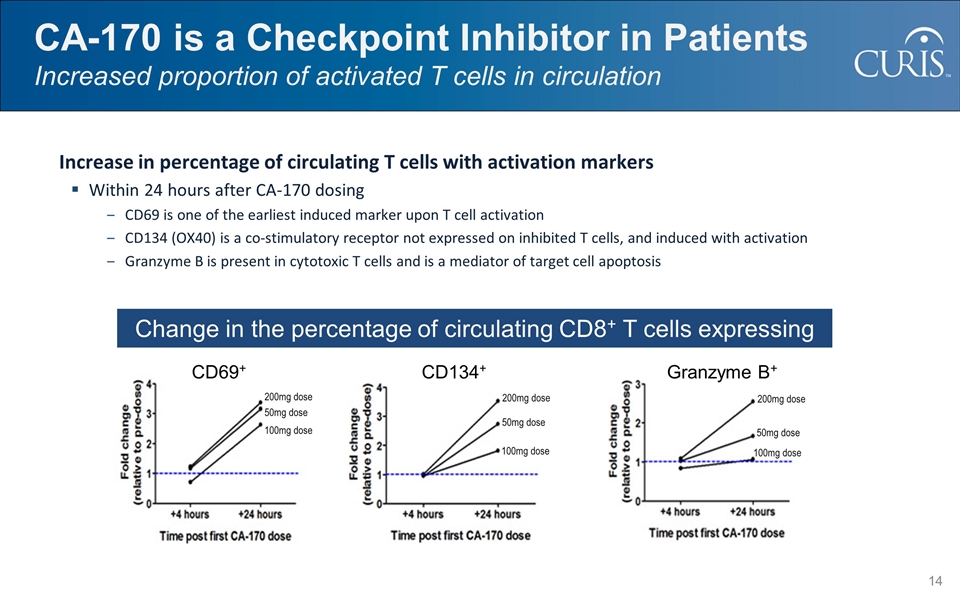
CA-170 is a Checkpoint Inhibitor in Patients Increased proportion of activated T cells in circulation Increase in percentage of circulating T cells with activation markers Within 24 hours after CA-170 dosing CD69 is one of the earliest induced marker upon T cell activation CD134 (OX40) is a co-stimulatory receptor not expressed on inhibited T cells, and induced with activation Granzyme B is present in cytotoxic T cells and is a mediator of target cell apoptosis Change in the percentage of circulating CD8+ T cells expressing 200mg dose 50mg dose 100mg dose 200mg dose 50mg dose 100mg dose 200mg dose 50mg dose 100mg dose CD69+ CD134+ Granzyme B+

CA-170 Development Plan Objective: registration in subpopulations of cancer patients Ongoing Phase 1 Trial Objectives Confirm safety, tolerability and PK/PD relationship with increasing doses of CA-170 Proof-of-concept: Demonstrate objective response with small molecule checkpoint inhibitor Identify potentially responsive patient populations during expansion stage: Immunotherapy-naïve patients: indications with PD1/PDL1 approvals in US – trial centers in Europe and Asia Immunotherapy-naïve patients: indications without anti-PD1/PDL1 approvals – trial centers in US, Europe and Asia Prior immunotherapy-treated patients: trial centers in US Expanded assessment of biomarkers for patient/sub-population selection Strategy/Potential Opportunities for Registration Subpopulations of immunotherapy-naïve patients in multiple indications Prior immunotherapy-treated patients in multiple indications

CA-170 Summary Potent and selective, oral small molecule immune checkpoint inhibitor ex-vivo Targets PDL1 and VISTA immune checkpoints Activates isolated T cells that are inhibited by PDL1 or VISTA in culture Potent immune checkpoint inhibitor in vivo in mouse tumor models with oral dosing Biologically active in mouse: Oral administration results in T cell activation in circulation and in tumor tissue Significant anti-tumor activity in multiple syngeneic tumor models Immune checkpoint inhibitor in cancer patients with oral dosing Biologically active in patients: T cell activation in circulation after oral dosing Planned continued development in Phase 1 In patients that are immunotherapy-naïve, or prior-treated Assessment of biomarkers of activity and opportunities for patient selection

CA-327 is an oral, small molecule immune checkpoint inhibitor Expected to enter clinical development in 2017 CA-327 Oral, small molecule checkpoint inhibitor – PDL1 and TIM3 Program Indication Stage of Development Preclinical Phase 1 Phase 2 Phase 3 Marketed CA-327 * PD-L1 / TIM3 Cancers
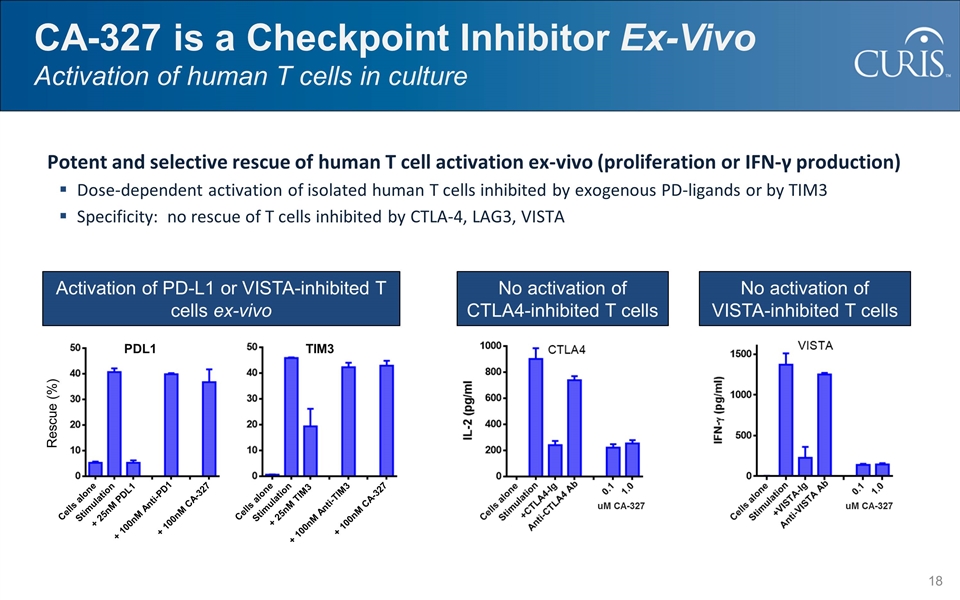
CA-327 is a Checkpoint Inhibitor Ex-Vivo Activation of human T cells in culture Activation of PD-L1 or VISTA-inhibited T cells ex-vivo No activation of CTLA4-inhibited T cells No activation of VISTA-inhibited T cells Potent and selective rescue of human T cell activation ex-vivo (proliferation or IFN-γ production) Dose-dependent activation of isolated human T cells inhibited by exogenous PD-ligands or by TIM3 Specificity: no rescue of T cells inhibited by CTLA-4, LAG3, VISTA Rescue (%) PDL1 Cells alone Stimulation + 25nM PDL1 + 100nM Anti-PD1 + 100nM CA-327 TIM3 Cells alone Stimulation + 25nM TIM3 + 100nM Anti-TIM3 + 100nM CA-327 uM CA-327 uM CA-327
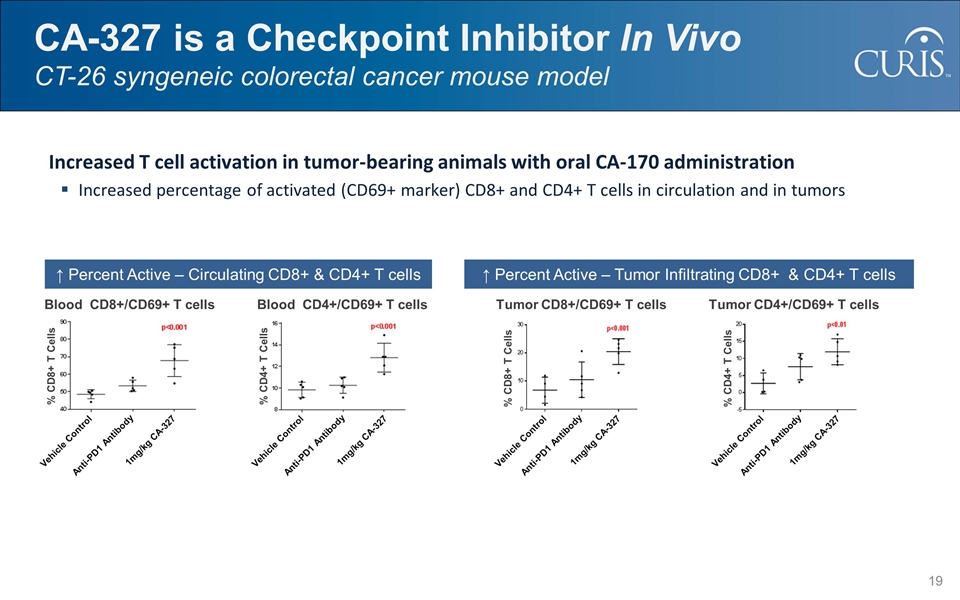
CA-327 is a Checkpoint Inhibitor In Vivo CT-26 syngeneic colorectal cancer mouse model Increased T cell activation in tumor-bearing animals with oral CA-170 administration Increased percentage of activated (CD69+ marker) CD8+ and CD4+ T cells in circulation and in tumors ↑ Percent Active – Tumor Infiltrating CD8+ & CD4+ T cells ↑ Percent Active – Circulating CD8+ & CD4+ T cells Blood CD8+/CD69+ T cells Vehicle Control Anti-PD1 Antibody 1mg/kg CA-327 Blood CD4+/CD69+ T cells Vehicle Control Anti-PD1 Antibody 1mg/kg CA-327 Tumor CD8+/CD69+ T cells Vehicle Control Anti-PD1 Antibody 1mg/kg CA-327 Tumor CD4+/CD69+ T cells Vehicle Control Anti-PD1 Antibody 1mg/kg CA-327 % CD8+ T Cells % CD8+ T Cells % CD4+ T Cells % CD4+ T Cells
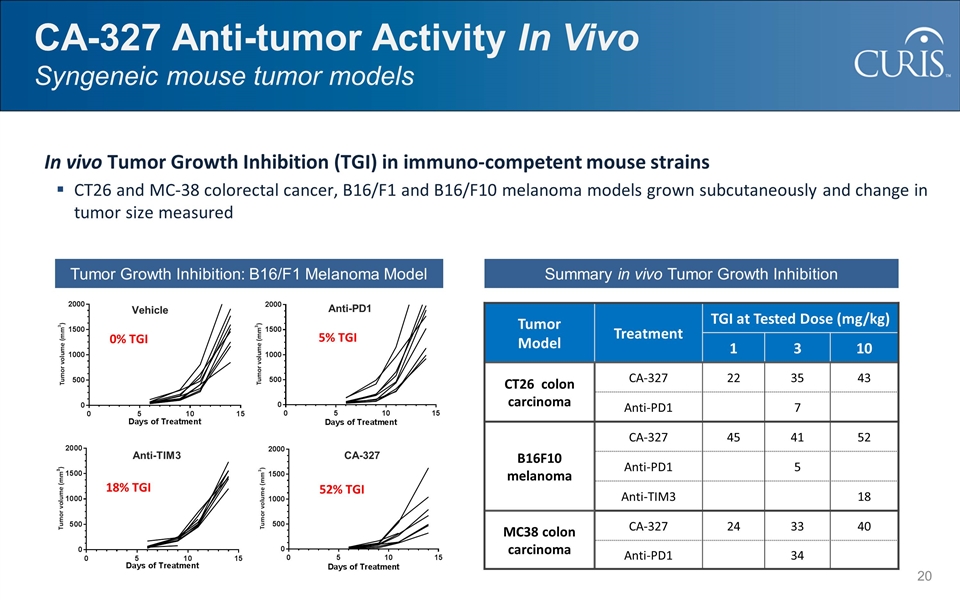
CA-327 Anti-tumor Activity In Vivo Syngeneic mouse tumor models In vivo Tumor Growth Inhibition (TGI) in immuno-competent mouse strains CT26 and MC-38 colorectal cancer, B16/F1 and B16/F10 melanoma models grown subcutaneously and change in tumor size measured 5% TGI Anti-PD1 18% TGI Anti-TIM3 52% TGI CA-327 0% TGI Vehicle Tumor Growth Inhibition: B16/F1 Melanoma Model Tumor Model Treatment TGI at Tested Dose (mg/kg) 1 3 10 CT26 colon carcinoma CA-327 22 35 43 Anti-PD1 7 B16F10 melanoma CA-327 45 41 52 Anti-PD1 5 Anti-TIM3 18 MC38 colon carcinoma CA-327 24 33 40 Anti-PD1 34 Summary in vivo Tumor Growth Inhibition

CA-327 Summary Potent and selective, oral small molecule immune checkpoint inhibitor ex-vivo Targets PDL1 and TIM3 immune checkpoints Activates isolated T cells that are inhibited by PDL1 or TIM3 in culture Potent immune checkpoint inhibitor in vivo in mouse tumor models with oral dosing Biologically active in mouse: Oral administration results in T cell activation in circulation and in tumor tissue Significant anti-tumor activity in multiple syngeneic tumor models IND-enabling studies ongoing Non-GLP preclinical safety profile similar to CA-170 Manufacturing underway in preparation for IND filing

CUDC-907 has the potential to become a treatment for MYC-altered cancers CUDC-907 Phase 2 drug candidate to treat MYC-driven cancers Program Indication Stage of Development Preclinical Phase 1 Phase 2 Phase 3 Marketed CUDC-907 HDAC / PI3K MYC-Altered DLBCL MYC-Driven Solid Tumors
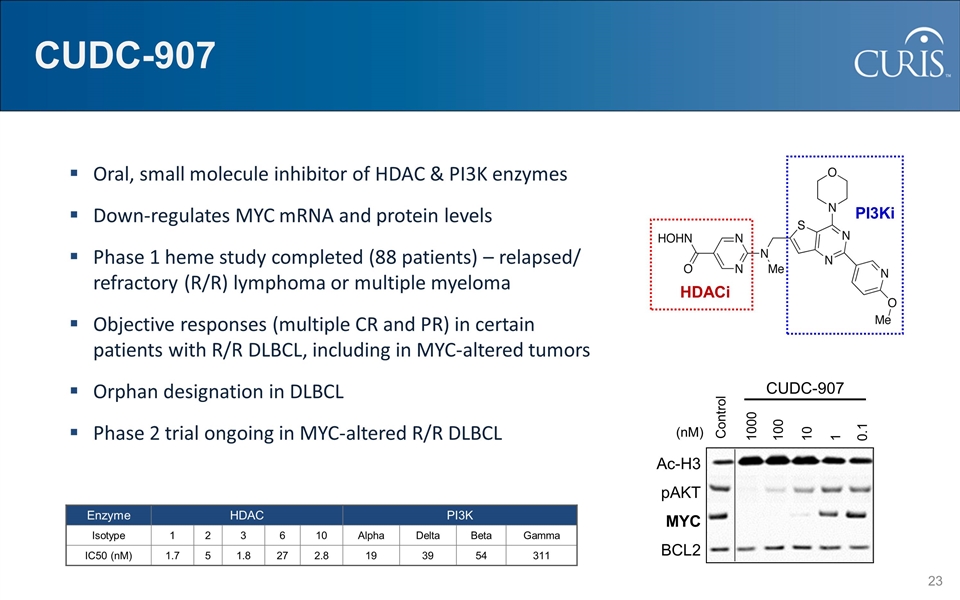
HDACi PI3Ki CUDC-907 Oral, small molecule inhibitor of HDAC & PI3K enzymes Down-regulates MYC mRNA and protein levels Phase 1 heme study completed (88 patients) – relapsed/ refractory (R/R) lymphoma or multiple myeloma Objective responses (multiple CR and PR) in certain patients with R/R DLBCL, including in MYC-altered tumors Orphan designation in DLBCL Phase 2 trial ongoing in MYC-altered R/R DLBCL Enzyme HDAC PI3K Isotype 1 2 3 6 10 Alpha Delta Beta Gamma IC50 (nM) 1.7 5 1.8 27 2.8 19 39 54 311 CUDC-907 Control 1000 100 10 1 0.1 Ac-H3 pAKT MYC BCL2 (nM)

CUDC-907 Phase 1 Trial Completed Study Population Patients with relapsed/refractory lymphoma or multiple myeloma after ≥ 2 prior regimens 76 patients treated with monotherapy: 41 in dose escalation, 35 in dose expansion stage 12 patients treated with combination of CUDC-907 + rituximab Treatment Dose escalation: oral, once daily administration in continuous 21-day cycles Multiple schedules of administration examined: QD (30mg, 60mg) 5 days on/2 off (60mg) 2x/week (60mg – 150mg) 3x/week (60mg – 120mg) RP2D: 60mg, oral, once daily, continuous dosing using 5 days on / 2 days off schedule in 21-day cycles Expansion cohorts at RP2D Monotherapy in cohorts of patients with DLBCL, HL, and multiple myeloma Combination therapy CUDC-907 + rituximab in patients with DLBCL
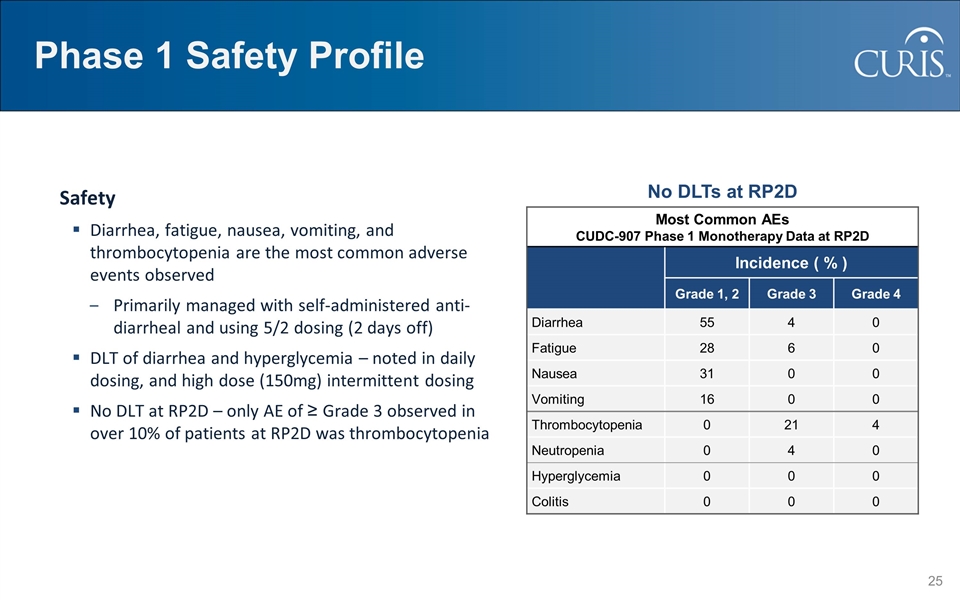
Phase 1 Safety Profile Most Common AEs CUDC-907 Phase 1 Monotherapy Data at RP2D Incidence ( % ) Grade 1, 2 Grade 3 Grade 4 Diarrhea 55 4 0 Fatigue 28 6 0 Nausea 31 0 0 Vomiting 16 0 0 Thrombocytopenia 0 21 4 Neutropenia 0 4 0 Hyperglycemia 0 0 0 Colitis 0 0 0 No DLTs at RP2D Safety Diarrhea, fatigue, nausea, vomiting, and thrombocytopenia are the most common adverse events observed Primarily managed with self-administered anti-diarrheal and using 5/2 dosing (2 days off) DLT of diarrhea and hyperglycemia – noted in daily dosing, and high dose (150mg) intermittent dosing No DLT at RP2D – only AE of ≥ Grade 3 observed in over 10% of patients at RP2D was thrombocytopenia
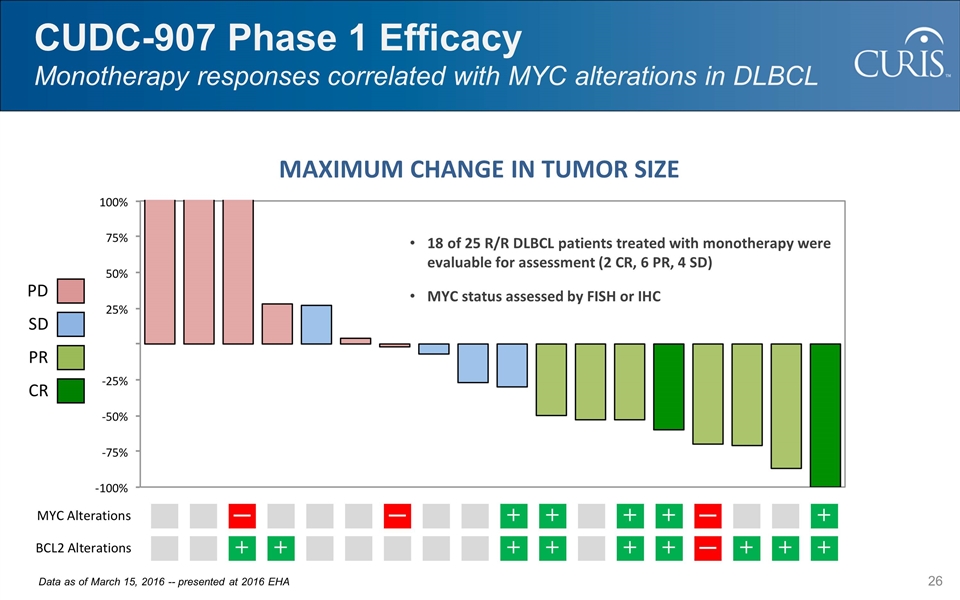
CUDC-907 Phase 1 Efficacy Monotherapy responses correlated with MYC alterations in DLBCL Data as of March 15, 2016 -- presented at 2016 EHA 18 of 25 R/R DLBCL patients treated with monotherapy were evaluable for assessment (2 CR, 6 PR, 4 SD) MYC status assessed by FISH or IHC MAXIMUM CHANGE IN TUMOR SIZE

CUDC-907 Phase 2 Trial Monotherapy in MYC-altered relapsed/refractory DLBCL Open label study to evaluate the efficacy and safety of CUDC-907 monotherapy in patients with relapsed/refractory (R/R) DLBCL – after 2 prior treatments Analysis of primary (ORR) and secondary (PFS, OS, DoR & safety) endpoints based on 60 MYC-altered R/R DLBCL patients MYC alterations detected by FISH or IHC Based on results, potential for discussion with FDA for accelerated registration path Study Ongoing Enrolling in multiple centers in the US and ex-US (currently active sites: 22) Objective responses have been observed (full analysis to be presented at a medical meeting) Study includes patients with and without MYC alterations, but endpoint analysis only for MYC-altered patients (N=60) Includes patients with 2-4 prior lines of therapy, including HSCT (and ECOG status <2) Excludes patients with active CNS disease, GVHD, serious bacterial or viral infections (HIV, HBV, HCV, CMV)

CUDC-907 DLBCL Development Plan Objective: registration for treatment of MYC-altered DLBCL Ongoing Phase 2 monotherapy trial Treatment of patients with MYC-altered R/R DLBCL with 2 prior treatments Based on results, expect to discuss with FDA in 2017 potential for accelerated registration path Planned Phase 3 randomized trial In accelerated approval path scenario, Phase 3 trial will still be required for full approval Potential for use in earlier lines of treatment, likely as combination therapy Manufacturing and CMC Commercial drug substance and drug product manufacturing process ongoing with selected vendors Intellectual property Composition of matter patent issued in multiple countries – protection through 2032
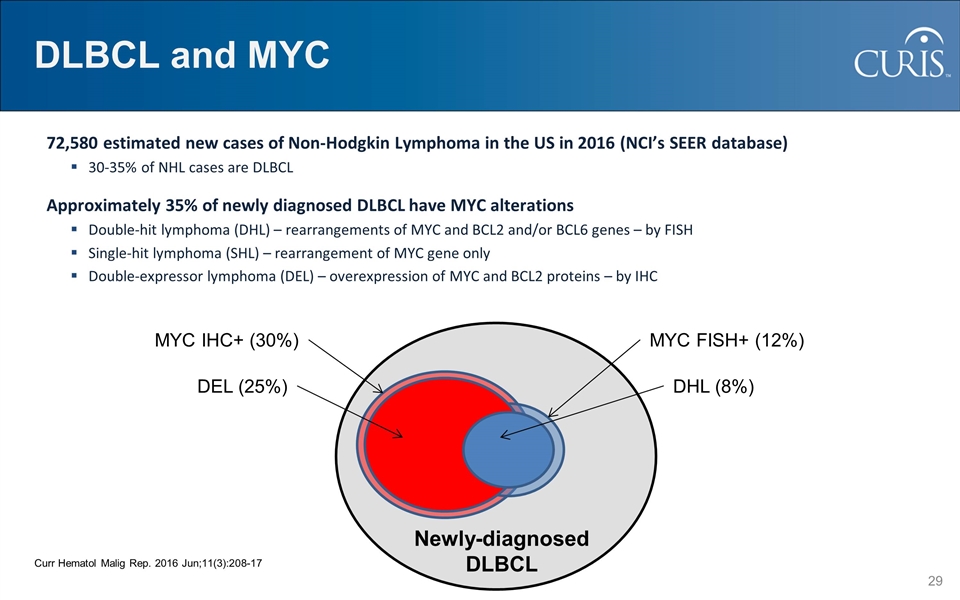
DLBCL and MYC 72,580 estimated new cases of Non-Hodgkin Lymphoma in the US in 2016 (NCI’s SEER database) 30-35% of NHL cases are DLBCL Approximately 35% of newly diagnosed DLBCL have MYC alterations Double-hit lymphoma (DHL) – rearrangements of MYC and BCL2 and/or BCL6 genes – by FISH Single-hit lymphoma (SHL) – rearrangement of MYC gene only Double-expressor lymphoma (DEL) – overexpression of MYC and BCL2 proteins – by IHC Newly-diagnosed DLBCL MYC IHC+ (30%) DEL (25%) MYC FISH+ (12%) DHL (8%) Curr Hematol Malig Rep. 2016 Jun;11(3):208-17
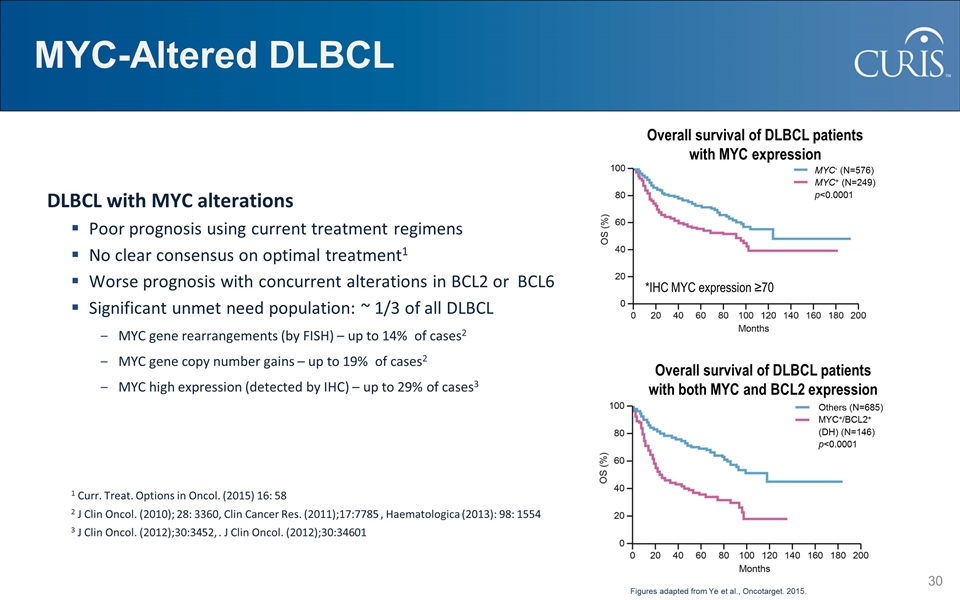
MYC-Altered DLBCL DLBCL with MYC alterations Poor prognosis using current treatment regimens No clear consensus on optimal treatment1 Worse prognosis with concurrent alterations in BCL2 or BCL6 Significant unmet need population: ~ 1/3 of all DLBCL MYC gene rearrangements (by FISH) – up to 14% of cases2 MYC gene copy number gains – up to 19% of cases2 MYC high expression (detected by IHC) – up to 29% of cases3 1 Curr. Treat. Options in Oncol. (2015) 16: 58 2 J Clin Oncol. (2010); 28: 3360, Clin Cancer Res. (2011);17:7785 , Haematologica (2013): 98: 1554 3 J Clin Oncol. (2012);30:3452, . J Clin Oncol. (2012);30:34601 Overall survival of DLBCL patients with MYC expression *IHC MYC expression ≥70 Overall survival of DLBCL patients with both MYC and BCL2 expression Figures adapted from Ye et al., Oncotarget. 2015. Others (N=685) MYC+/BCL2+ (DH) (N=146) p<0.0001 MYC- (N=576) MYC+ (N=249) p<0.0001
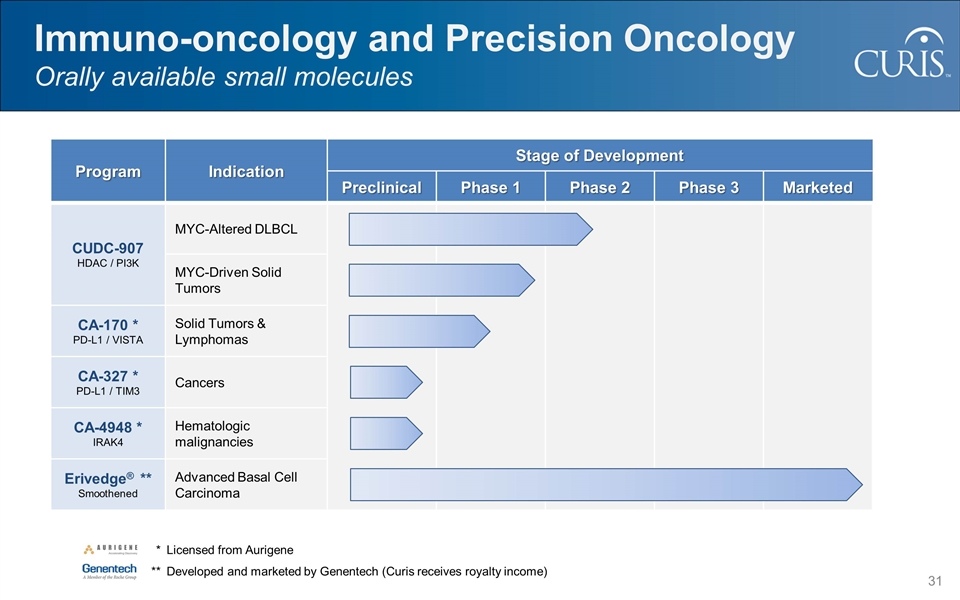
Immuno-oncology and Precision Oncology Orally available small molecules * Licensed from Aurigene **Developed and marketed by Genentech (Curis receives royalty income) Program Indication Stage of Development Preclinical Phase 1 Phase 2 Phase 3 Marketed CUDC-907 HDAC / PI3K MYC-Altered DLBCL MYC-Driven Solid Tumors CA-170 * PD-L1 / VISTA Solid Tumors & Lymphomas CA-327 * PD-L1 / TIM3 Cancers CA-4948 * IRAK4 Hematologic malignancies Erivedge® ** Smoothened Advanced Basal Cell Carcinoma

$53.4MCash & Marketable Securities $20.9MErivedge® secured debt (non-recourse to Curis) 140.0MShares Outstanding - Basic 155.5MShares Outstanding - Fully Diluted* *Diluted Shares= 140.0M basic shares + 15.5M options Summary of Financial Data As of September 30, 2016

CA-170 Phase 1 Dose Escalationn Ongoing Phase 1 Expansionn Begin Enrollment in 1H 2017 CA-327 INDn Mid-2017 filing CUDC-907 Phase 2 in DLBCLn Initial Results in 1H 2017 Phase 1 in Solid Tumorsn Initial Results in 2H 2017 CA-4948 INDn Mid-2017 filing Projected Milestones

END