
Commitment to a Cure Cellectis Clinical Update December 2022 NASDAQ: CLLS EURONEXT GROWTH: ALCLS.PA Exhibit 99.1

This presentation (together with the corresponding webcast, this “Presentation”) contains “forward-looking” statements within the meaning of applicable securities laws, including the Private Securities Litigation Reform Act of 1995. This Presentation shall not constitute an offer to sell, or the solicitation of an offer to buy, securities of Cellectis S.A. (“Cellectis,” “we,” “us,” or “our”) . All statements other than statements of present and historical facts regarding Cellectis contained in this Presentation are forward-looking statements. You can identify certain forward-looking statements by words such as “anticipate,” “believe,” “can,” “could,” “estimate,” “expect,” “intend,” “is designed to,” “may,” “might,” “plan,” “potential,” “predict,” “objective,” “scheduled,” “should,” and “will,” or similar expressions (or the negative of these). Such forward-looking statements include, but are not limited to, statements regarding: the preliminary results for the AMELI-01 and BALLI-01 trials and the objectives of such trials, which remain ongoing; Cellectis’ manufacturing capabilities and the scalability and cost thereof; the potential for profitable market access; Cellectis’ expected cash runway and the projections taken into account therein; Cellectis’ near term milestones and ability to achieve such expectations. These forward-looking statements are subject to numerous risks and uncertainties, including with respect to the risk that initial, interim and preliminary data from clinical trials may change as more data becomes available, and that subsequent data may not bear out promising early results; the risk of disruptions or delays in our clinical trials as a result of failures by third-parties on whom we rely or arising out of regulatory inquiries or delays; the risk of manufacturing delays or problems; the risk associated with increased competition and/or adequate enrollment to support our clinical trials; and the various other risks associated with biopharmaceutical product candidate development, including those described under “Risk Factors” and “Special Note Regarding Forward-Looking Statements” in our Annual Report on Form 20-F filed with the Securities and Exchange Commission (the “SEC”) on March 3, 2022 and under “Risk Factors” in the subsequent reports that we file with the SEC. Actual results, performance or events may differ materially from those projected in any forward-looking statement. Except as required by law, we assume no obligation to update these forward-looking statements. Legal Notices

References in this Presentation to Cellectis’ product candidates as “off-the-shelf” refers to the fact that our CAR T-cells are allogeneic, meaning they are derived from healthy donors rather than the patients themselves, which we believe allows for the development of cost-effective product candidates capable of being stored and distributed worldwide. Caution should be exercised when interpreting preliminary results and results relating to a small number of patients or individually presented case studies — such results should not be viewed as predictive of future results. Legal Notices

Cellectis at a Glance 4 Ongoing Clinical Trials Operational since 2021 End-to-end manufacturing autonomy Near-Term Clinical Catalyst 200+ patients dosed to date Potential revenues > $4B in milestones + royalties 6 trials sponsored by Cellectis’ licensed partners Diversified Partnerships with Industry Leaders $103M as of Sept 30, 2022 Expected Cash Runway into 2024* Global GMP Facilities 40+ patients dosed in Cellectis-sponsored trials UCART clinical data updates Cash position, includes cash, cash equivalent, financial assets and restricted cash Cash runway takes into account projected cash flow from operations, including payments Cellectis expects to receive pursuant to strategic licensing agreements
UCARTs are “Off-The-Shelf” Reduced cost Scalable manufacturing: 1 batch = 100s of doses The goal is to provide potency and consistency to each patient Immediately available to eligible patients Market Access Robustness Scalable Manufacturing
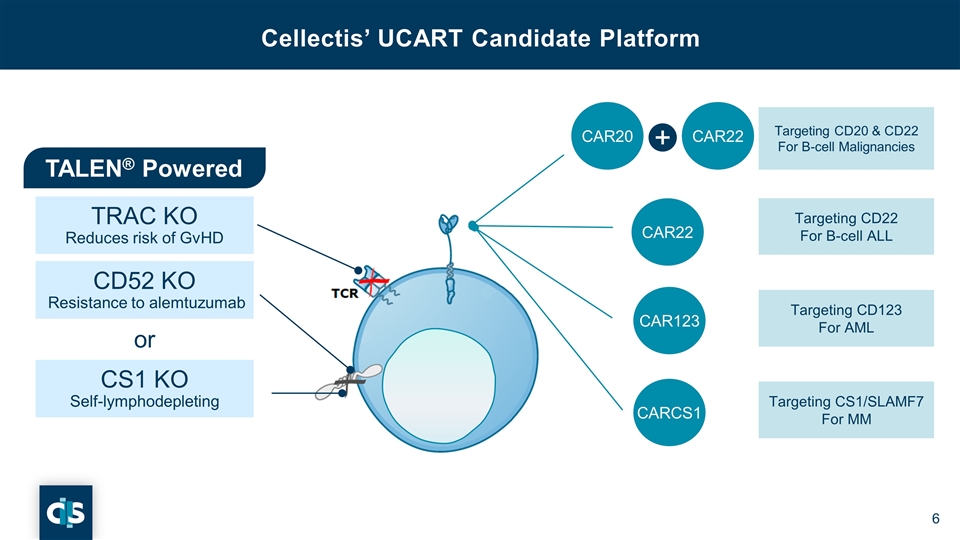
TALEN® Powered TRAC KO Reduces risk of GvHD CS1 KO Self-lymphodepleting CD52 KO Resistance to alemtuzumab or Cellectis’ UCART Candidate Platform CAR20 CAR22 CAR123 CARCS1 Targeting CD20 & CD22 For B-cell Malignancies Targeting CD22 For B-cell ALL Targeting CD123 For AML Targeting CS1/SLAMF7 For MM CAR22

AMELI-01: UCART123

AMELI-01:Preliminary Results from A Phase I Trial of UCART123v1.2, an Anti-CD123 Allogeneic CAR-T Cell Product, in Adult Patients with Relapsed or Refractory (R/R) CD123+ Acute Myeloid Leukemia David A. Sallman1, Daniel J. DeAngelo2, Naveen Pemmaraju3, Shira Dinner4, Saar Gill5, Rebecca Olin6, Eunice S. Wang7, Marina Konopleva3, Eileen Stark8, Ana Korngold8, Asifa Haider8, Kate Backhouse8, Carolyn Figliola8, Daniel J. Lee8, Kathryn Newhall8, Mark G. Frattini8, Carrie Brownstein8, Gail J. Roboz9 1H. Lee Moffitt Cancer Center, 2Dana-Farber Cancer Institute, 3MD Anderson Cancer Center, 4Northwestern Medical Center, 5University of Pennsylvania Perelman School of Medicine, 6University of California San Francisco, 7Roswell Park Comprehensive Cancer Center, 8Cellectis, Inc., and 9Weill Cornell Medical College Publication Number 981 ASH 2022

Background and Introduction It is estimated that 20,050 new cases and 11,540 deaths related to AML will occur in the US in 20221 Outcomes for patients with R/R AML remain poor, with response rates <30% and an expected 5-year overall survival of <15%2,3 AMELI-01 (NCT03190278) is a phase I, open-label, dose-escalation trial evaluating the safety, tolerability, expansion, and preliminary activity of UCART123v1.2 given at escalating doses after LD with fludarabine and cyclophosphamide (FC) or FC with alemtuzumab (FCA) in patients with R/R CD123+ AML 1 https://www.cancer.org/cancer/acute-myeloid-leukemia/about/key-statistics.html; 2Ganzel, C, et al. Am J Hematol. 2018; 93: 1074-1081; 3Döhner, H, et al. Blood 2017; 129 (4): 424–447.
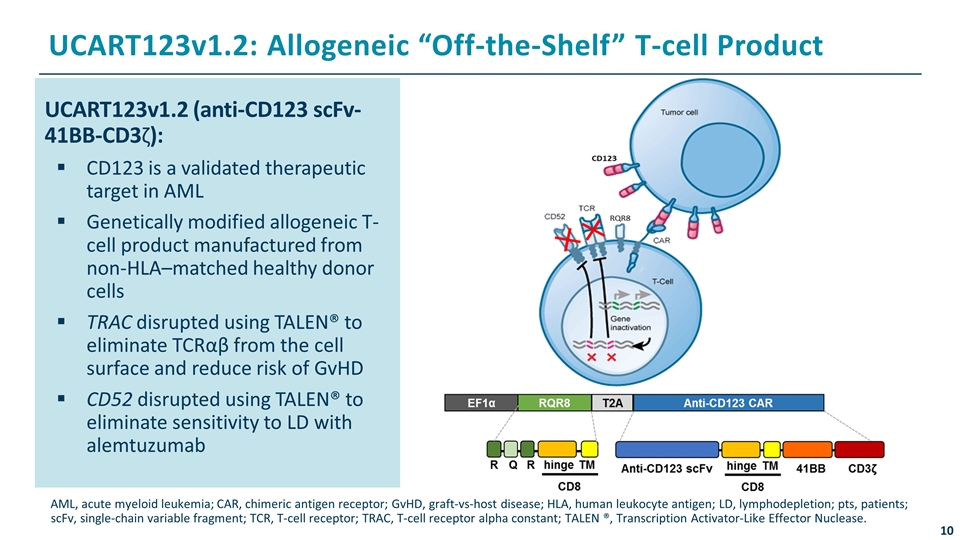
UCART123v1.2 (anti-CD123 scFv-41BB-CD3ζ): CD123 is a validated therapeutic target in AML Genetically modified allogeneic T-cell product manufactured from non-HLA–matched healthy donor cells TRAC disrupted using TALEN® to eliminate TCRαβ from the cell surface and reduce risk of GvHD CD52 disrupted using TALEN® to eliminate sensitivity to LD with alemtuzumab AML, acute myeloid leukemia; CAR, chimeric antigen receptor; GvHD, graft-vs-host disease; HLA, human leukocyte antigen; LD, lymphodepletion; pts, patients; scFv, single-chain variable fragment; TCR, T-cell receptor; TRAC, T-cell receptor alpha constant; TALEN ®, Transcription Activator-Like Effector Nuclease. UCART123v1.2: Allogeneic “Off-the-Shelf” T-cell Product
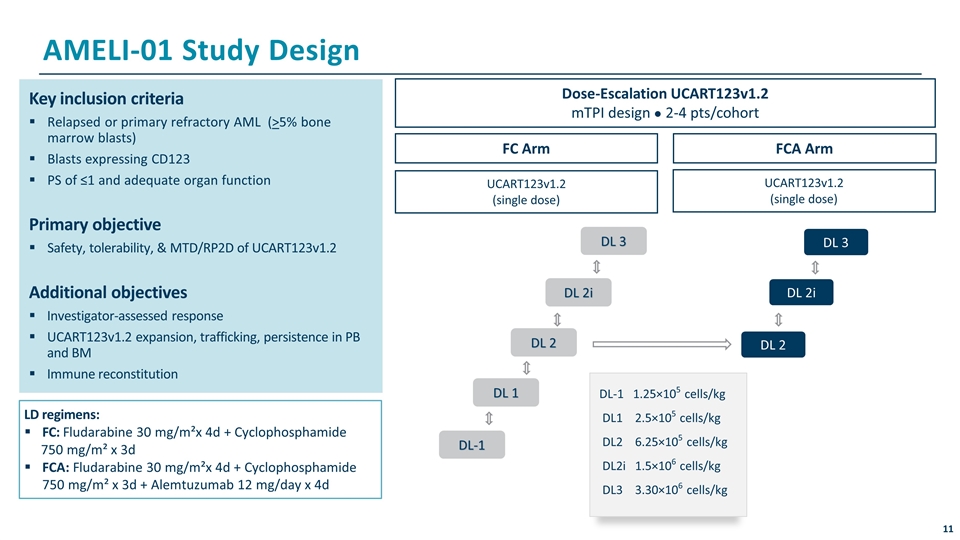
AMELI-01 Study Design Key inclusion criteria Relapsed or primary refractory AML (>5% bone marrow blasts) Blasts expressing CD123 PS of ≤1 and adequate organ function Primary objective Safety, tolerability, & MTD/RP2D of UCART123v1.2 Additional objectives Investigator-assessed response UCART123v1.2 expansion, trafficking, persistence in PB and BM Immune reconstitution LD regimens: FC: Fludarabine 30 mg/m²x 4d + Cyclophosphamide 750 mg/m² x 3d FCA: Fludarabine 30 mg/m²x 4d + Cyclophosphamide 750 mg/m² x 3d + Alemtuzumab 12 mg/day x 4d Dose-Escalation UCART123v1.2 mTPI design ● 2-4 pts/cohort FC Arm UCART123v1.2 (single dose) FCA Arm UCART123v1.2 (single dose) DL-1 DL 1 DL 2 DL 2i DL 2 DL 2i DL 3 DL-1 1.25×105 cells/kg DL1 2.5×105 cells/kg DL2 6.25×105 cells/kg DL2i 1.5×106 cells/kg DL3 3.30×106 cells/kg DL 3
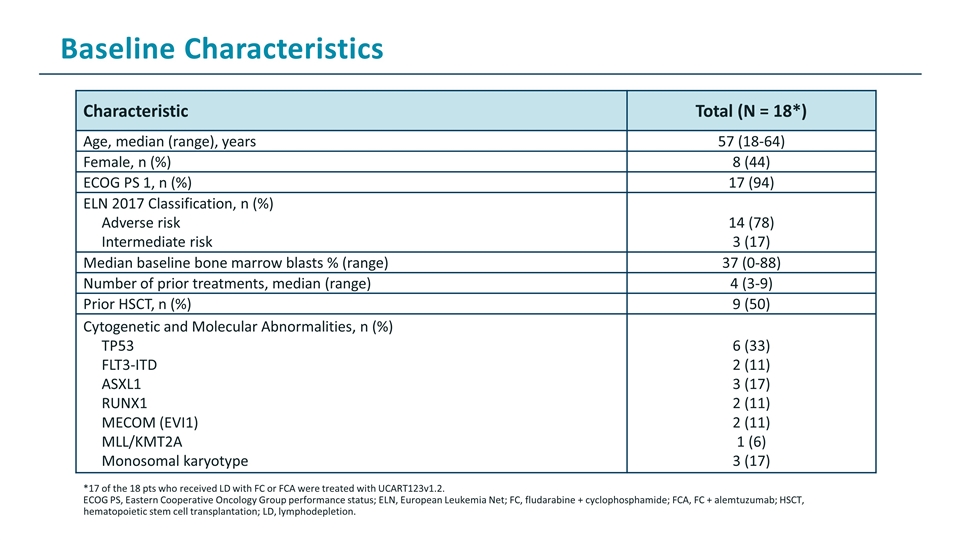
Characteristic Total (N = 18*) Age, median (range), years 57 (18-64) Female, n (%) 8 (44) ECOG PS 1, n (%) 17 (94) ELN 2017 Classification, n (%) Adverse risk Intermediate risk 14 (78) 3 (17) Median baseline bone marrow blasts % (range) 37 (0-88) Number of prior treatments, median (range) 4 (3-9) Prior HSCT, n (%) 9 (50) Cytogenetic and Molecular Abnormalities, n (%) TP53 FLT3-ITD ASXL1 RUNX1 MECOM (EVI1) MLL/KMT2A Monosomal karyotype 6 (33) 2 (11) 3 (17) 2 (11) 2 (11) 1 (6) 3 (17) *17 of the 18 pts who received LD with FC or FCA were treated with UCART123v1.2. ECOG PS, Eastern Cooperative Oncology Group performance status; ELN, European Leukemia Net; FC, fludarabine + cyclophosphamide; FCA, FC + alemtuzumab; HSCT, hematopoietic stem cell transplantation; LD, lymphodepletion. Baseline Characteristics
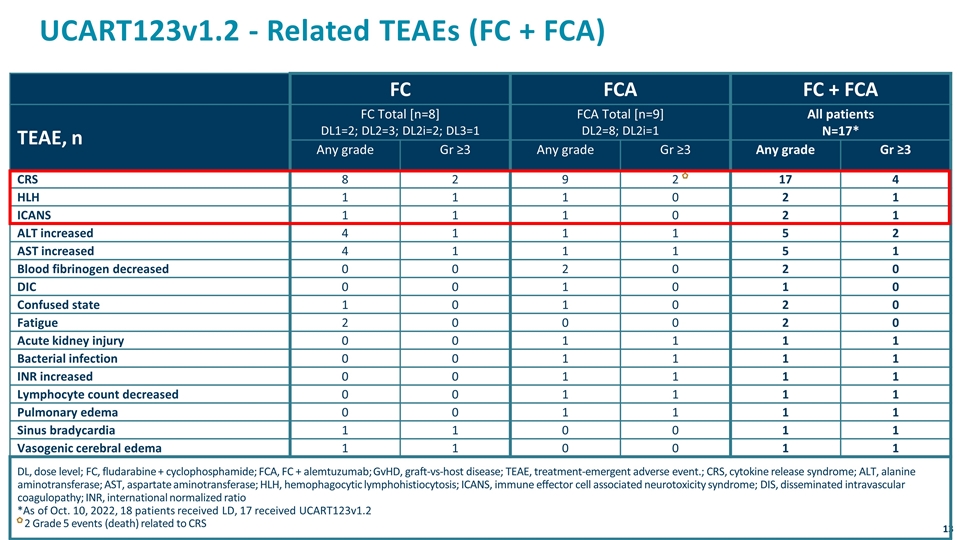
UCART123v1.2 - Related TEAEs (FC + FCA) FC FCA FC + FCA TEAE, n FC Total [n=8] DL1=2; DL2=3; DL2i=2; DL3=1 FCA Total [n=9] DL2=8; DL2i=1 All patients N=17* Any grade Gr ≥3 Any grade Gr ≥3 Any grade Gr ≥3 CRS 8 2 9 2 17 4 HLH 1 1 1 0 2 1 ICANS 1 1 1 0 2 1 ALT increased 4 1 1 1 5 2 AST increased 4 1 1 1 5 1 Blood fibrinogen decreased 0 0 2 0 2 0 DIC 0 0 1 0 1 0 Confused state 1 0 1 0 2 0 Fatigue 2 0 0 0 2 0 Acute kidney injury 0 0 1 1 1 1 Bacterial infection 0 0 1 1 1 1 INR increased 0 0 1 1 1 1 Lymphocyte count decreased 0 0 1 1 1 1 Pulmonary edema 0 0 1 1 1 1 Sinus bradycardia 1 1 0 0 1 1 Vasogenic cerebral edema 1 1 0 0 1 1 DL, dose level; FC, fludarabine + cyclophosphamide; FCA, FC + alemtuzumab; GvHD, graft-vs-host disease; TEAE, treatment-emergent adverse event.; CRS, cytokine release syndrome; ALT, alanine aminotransferase; AST, aspartate aminotransferase; HLH, hemophagocytic lymphohistiocytosis; ICANS, immune effector cell associated neurotoxicity syndrome; DIS, disseminated intravascular coagulopathy; INR, international normalized ratio *As of Oct. 10, 2022, 18 patients received LD, 17 received UCART123v1.2 2 Grade 5 events (death) related to CRS
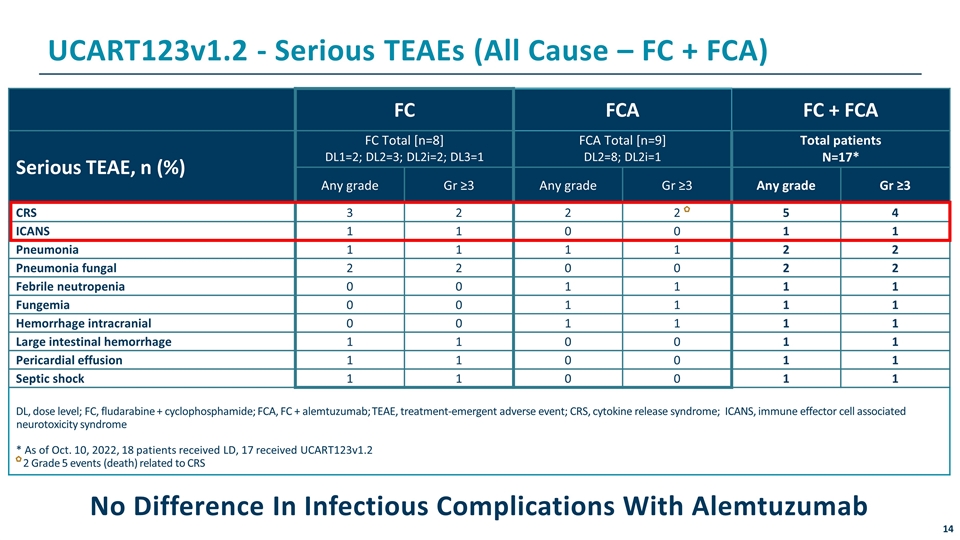
UCART123v1.2 - Serious TEAEs (All Cause – FC + FCA) FC FCA FC + FCA Serious TEAE, n (%) FC Total [n=8] DL1=2; DL2=3; DL2i=2; DL3=1 FCA Total [n=9] DL2=8; DL2i=1 Total patients N=17* Any grade Gr ≥3 Any grade Gr ≥3 Any grade Gr ≥3 CRS 3 2 2 2 5 4 ICANS 1 1 0 0 1 1 Pneumonia 1 1 1 1 2 2 Pneumonia fungal 2 2 0 0 2 2 Febrile neutropenia 0 0 1 1 1 1 Fungemia 0 0 1 1 1 1 Hemorrhage intracranial 0 0 1 1 1 1 Large intestinal hemorrhage 1 1 0 0 1 1 Pericardial effusion 1 1 0 0 1 1 Septic shock 1 1 0 0 1 1 DL, dose level; FC, fludarabine + cyclophosphamide; FCA, FC + alemtuzumab; TEAE, treatment-emergent adverse event; CRS, cytokine release syndrome; ICANS, immune effector cell associated neurotoxicity syndrome * As of Oct. 10, 2022, 18 patients received LD, 17 received UCART123v1.2 2 Grade 5 events (death) related to CRS No Difference In Infectious Complications With Alemtuzumab
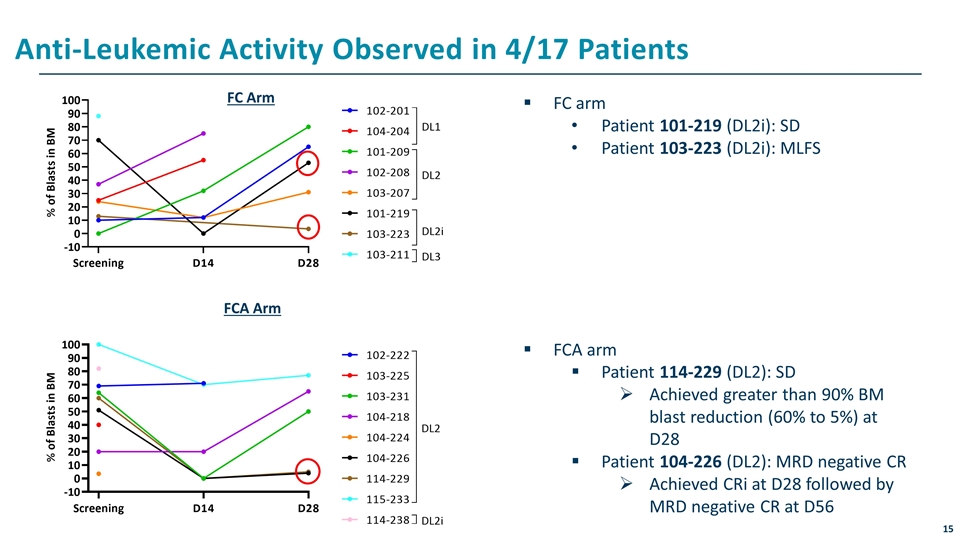
Anti-Leukemic Activity Observed in 4/17 Patients FC arm Patient 101-219 (DL2i): SD Patient 103-223 (DL2i): MLFS FCA arm Patient 114-229 (DL2): SD Achieved greater than 90% BM blast reduction (60% to 5%) at D28 Patient 104-226 (DL2): MRD negative CR Achieved CRi at D28 followed by MRD negative CR at D56 FC Arm FCA Arm
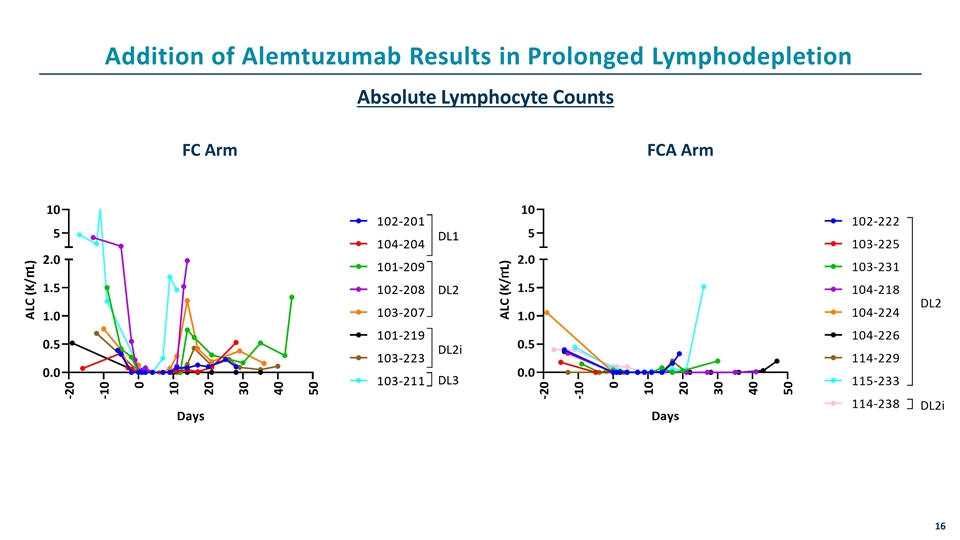
Absolute Lymphocyte Counts FC Arm FCA Arm Addition of Alemtuzumab Results in Prolonged Lymphodepletion

Addition of Alemtuzumab Results in Increased UCART123v1.2 Expansion UCART123 Cell Expansion in WB by VCN VCN AUC(0-28days) FC Arm FCA Arm p=0.04
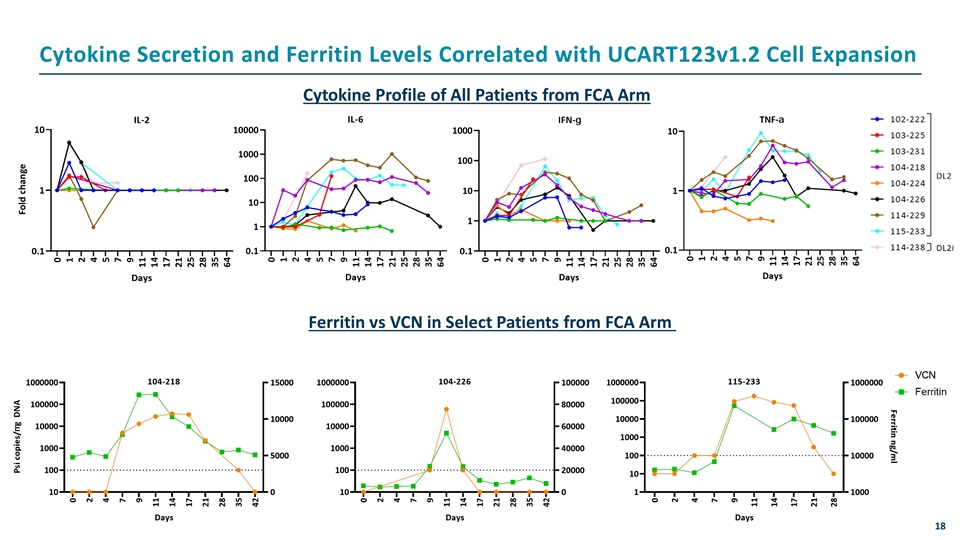
Cytokine Profile of All Patients from FCA Arm Ferritin vs VCN in Select Patients from FCA Arm Cytokine Secretion and Ferritin Levels Correlated with UCART123v1.2 Cell Expansion
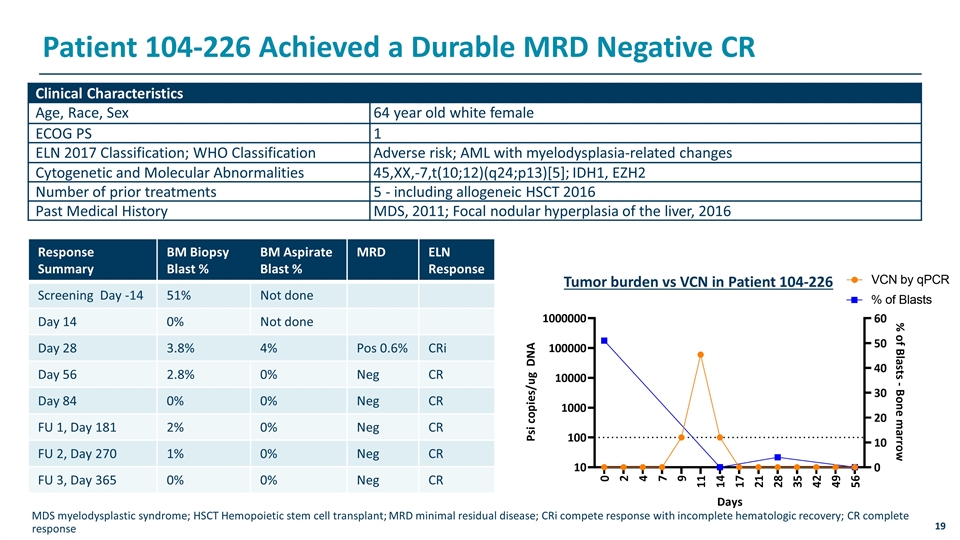
Patient 104-226 Achieved a Durable MRD Negative CR Clinical Characteristics Age, Race, Sex 64 year old white female ECOG PS 1 ELN 2017 Classification; WHO Classification Adverse risk; AML with myelodysplasia-related changes Cytogenetic and Molecular Abnormalities 45,XX,-7,t(10;12)(q24;p13)[5]; IDH1, EZH2 Number of prior treatments 5 - including allogeneic HSCT 2016 Past Medical History MDS, 2011; Focal nodular hyperplasia of the liver, 2016 MDS myelodysplastic syndrome; HSCT Hemopoietic stem cell transplant; MRD minimal residual disease; CRi compete response with incomplete hematologic recovery; CR complete response Response Summary BM Biopsy Blast % BM Aspirate Blast % MRD ELN Response Screening Day -14 51% Not done Day 14 0% Not done Day 28 3.8% 4% Pos 0.6% CRi Day 56 2.8% 0% Neg CR Day 84 0% 0% Neg CR FU 1, Day 181 2% 0% Neg CR FU 2, Day 270 1% 0% Neg CR FU 3, Day 365 0% 0% Neg CR Tumor burden vs VCN in Patient 104-226

Translational Data From Patient 104-226 and Others Supports Use of a Two-Dose Regimen of UCART123v1.2 UCART123v1.2 expansion correlates with reduction in tumor burden at DL2 (6.25 x 105 cells/kg) but at this dose, UCART123v1.2 cell function is not sufficient for sustained anti-leukemic activity in all patients A second dose would then be given to allow for additional UCART123v1.2 expansion and clinical activity after 10-14 days without the use of additional lymphodepletion The second peak of expansion in the setting of reduced disease burden should be safe and allow for clearance of residual disease The 2-dose regimen will initiate at DL2, a dose that has already been administered and cleared for safety as a single dose, and incorporate the use of prophylactic tocilizumab
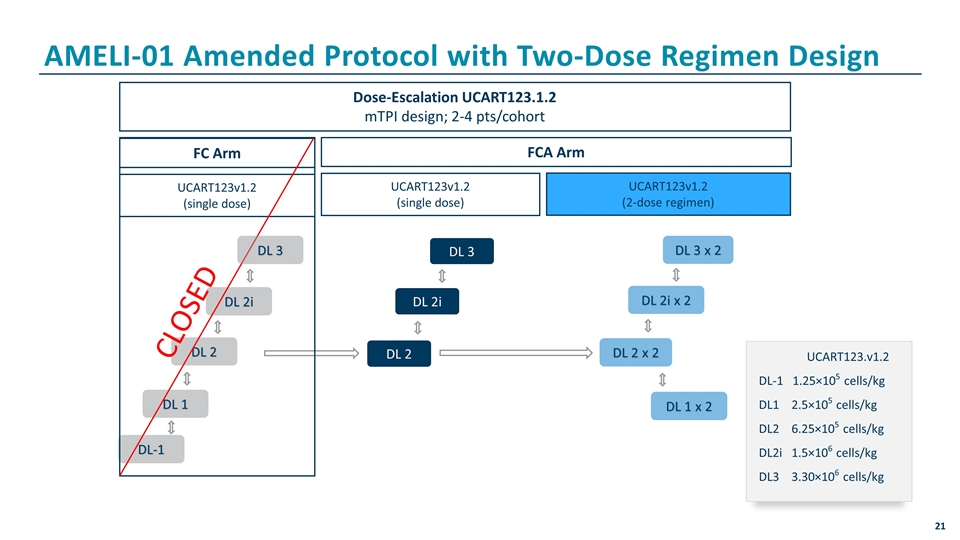
AMELI-01 Amended Protocol with Two-Dose Regimen Design Dose-Escalation UCART123.1.2 mTPI design; 2-4 pts/cohort FC Arm UCART123v1.2 (single dose) FCA Arm UCART123v1.2 (single dose) UCART123v1.2 (2-dose regimen) DL-1 DL 1 DL 2 DL 2i DL 2 DL 2i DL 3 DL 2 x 2 DL 2i x 2 DL 3 x 2 DL 1 x 2 UCART123.v1.2 DL-1 1.25×105 cells/kg DL1 2.5×105 cells/kg DL2 6.25×105 cells/kg DL2i 1.5×106 cells/kg DL3 3.30×106 cells/kg CLOSED DL 3

Conclusions Adding alemtuzumab to the FC regimen was associated with improved LD and significantly higher UCART123v1.2 cell expansion, which correlated with improved activity and cytokine profiles One patient in the DL2 FCA arm achieved >90% blast reduction at Day 28 One patient in the DL2 FCA arm achieved a long term durable MRD negative CR (now past 12 months) Overall, these data support further study of UCART123v1.2 after FCA LD in pts with R/R AML Based on observed UCART123v1.2 expansion patterns and cytokine profiles, the study is enrolling patients in the FCA 2-dose regimen arm

BALLI-01: UCART22
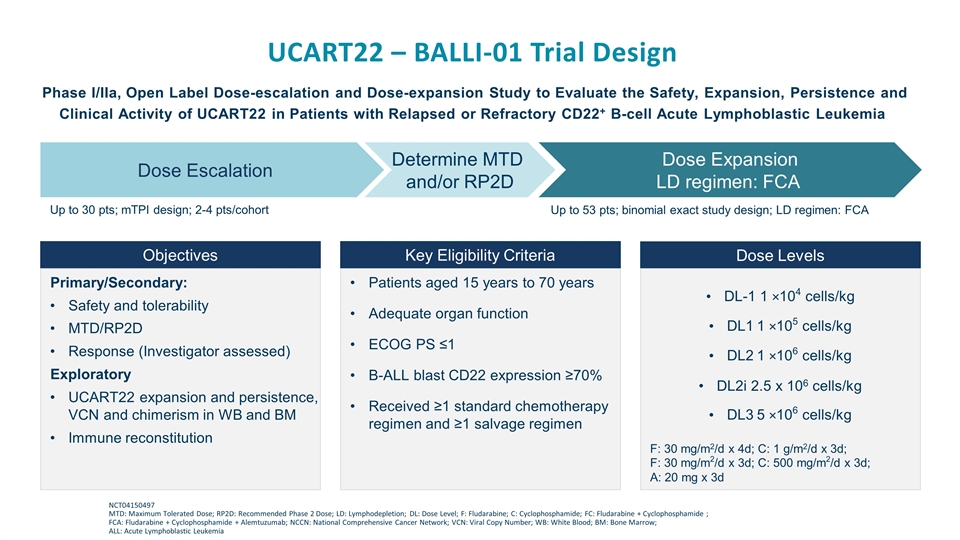
UCART22 – BALLI-01 Trial Design NCT04150497 MTD: Maximum Tolerated Dose; RP2D: Recommended Phase 2 Dose; LD: Lymphodepletion; DL: Dose Level; F: Fludarabine; C: Cyclophosphamide; FC: Fludarabine + Cyclophosphamide ; FCA: Fludarabine + Cyclophosphamide + Alemtuzumab; NCCN: National Comprehensive Cancer Network; VCN: Viral Copy Number; WB: White Blood; BM: Bone Marrow; ALL: Acute Lymphoblastic Leukemia Phase I/IIa, Open Label Dose-escalation and Dose-expansion Study to Evaluate the Safety, Expansion, Persistence and Clinical Activity of UCART22 in Patients with Relapsed or Refractory CD22+ B-cell Acute Lymphoblastic Leukemia Dose Escalation Determine MTD and/or RP2D Dose Expansion LD regimen: FCA Up to 30 pts; mTPI design; 2-4 pts/cohort Up to 53 pts; binomial exact study design; LD regimen: FCA Objectives Key Eligibility Criteria Dose Levels Primary/Secondary: Safety and tolerability MTD/RP2D Response (Investigator assessed) Exploratory UCART22 expansion and persistence, VCN and chimerism in WB and BM Immune reconstitution Patients aged 15 years to 70 years Adequate organ function ECOG PS ≤1 B-ALL blast CD22 expression ≥70% Received ≥1 standard chemotherapy regimen and ≥1 salvage regimen DL-1 1 ×104 cells/kg DL1 1 ×105 cells/kg DL2 1 ×106 cells/kg DL2i 2.5 x 106 cells/kg DL3 5 ×106 cells/kg F: 30 mg/m2/d x 4d; C: 1 g/m2/d x 3d; F: 30 mg/m2/d x 3d; C: 500 mg/m2/d x 3d; A: 20 mg x 3d

UCART22 Administration Shows Promising Safety Profile Data Source: ASH 2021 Conference Presentation CRFL2: Cytokine Receptor-Like Factor 2 ; FCA: Fludarabine, Cyclophosphamide, Alemtuzumab ; ICANS: Immune effector Cell-Associated Neurotoxicity Syndrome ; TEAE: Treatment Emergent Adverse Event CRS: Cytokine Release Syndrome ; GvHD: Graft versus Host Disease N=11 for calculating patients with prior therapy *not confirmed by biopsy; in context of re-activation of prior allogeneic bone marrow donor stem cells Median age: 30 (20-61) WHO classification: B-ALL with recurrent genetic abnormalities: 7 (58%); CRFL2 rearrangement: 4 (33%) Median prior lines of therapy: 3 (2-6) Prior blinatumomab: 8 (73%) Prior inotuzumab: 5 (45%) Prior CD19 CART: 3 (27%) Prior HSCT: 3 (25%) 0 dose limiting toxicity 0 ICANS (immune effector cell associated neurotoxicity) 0 severe UCART22-related TEAEs (treatment emergent adverse events) 3 patients with mild to moderate CRS (cytokine release syndrome), Grade 1/2 1 patient with GII GvHD; skin only* Patient Characteristics (N=12) Safety: FCA Cohorts (N=6)
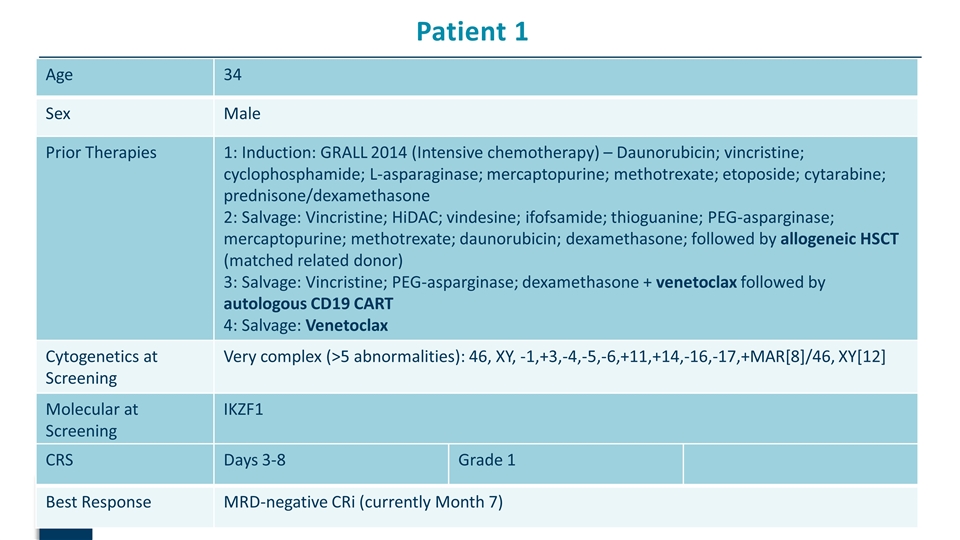
Patient 1 P Age 34 Sex Male Prior Therapies 1: Induction: GRALL 2014 (Intensive chemotherapy) – Daunorubicin; vincristine; cyclophosphamide; L-asparaginase; mercaptopurine; methotrexate; etoposide; cytarabine; prednisone/dexamethasone 2: Salvage: Vincristine; HiDAC; vindesine; ifofsamide; thioguanine; PEG-asparginase; mercaptopurine; methotrexate; daunorubicin; dexamethasone; followed by allogeneic HSCT (matched related donor) 3: Salvage: Vincristine; PEG-asparginase; dexamethasone + venetoclax followed by autologous CD19 CART 4: Salvage: Venetoclax Cytogenetics at Screening Very complex (>5 abnormalities): 46, XY, -1,+3,-4,-5,-6,+11,+14,-16,-17,+MAR[8]/46, XY[12] Molecular at Screening IKZF1 CRS Days 3-8 Grade 1 Best Response MRD-negative CRi (currently Month 7)
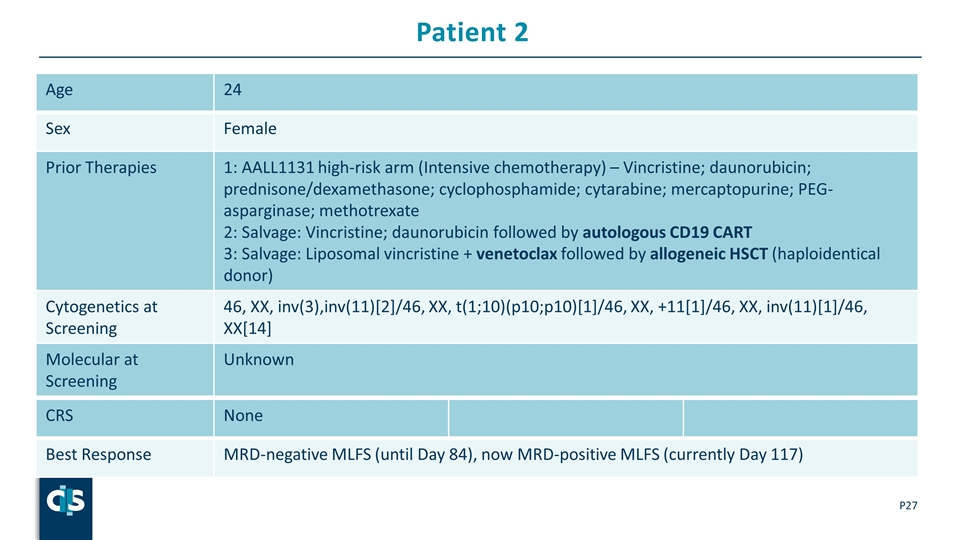
Patient 2 P Age 24 Sex Female Prior Therapies 1: AALL1131 high-risk arm (Intensive chemotherapy) – Vincristine; daunorubicin; prednisone/dexamethasone; cyclophosphamide; cytarabine; mercaptopurine; PEG-asparginase; methotrexate 2: Salvage: Vincristine; daunorubicin followed by autologous CD19 CART 3: Salvage: Liposomal vincristine + venetoclax followed by allogeneic HSCT (haploidentical donor) Cytogenetics at Screening 46, XX, inv(3),inv(11)[2]/46, XX, t(1;10)(p10;p10)[1]/46, XX, +11[1]/46, XX, inv(11)[1]/46, XX[14] Molecular at Screening Unknown CRS None Best Response MRD-negative MLFS (until Day 84), now MRD-positive MLFS (currently Day 117)
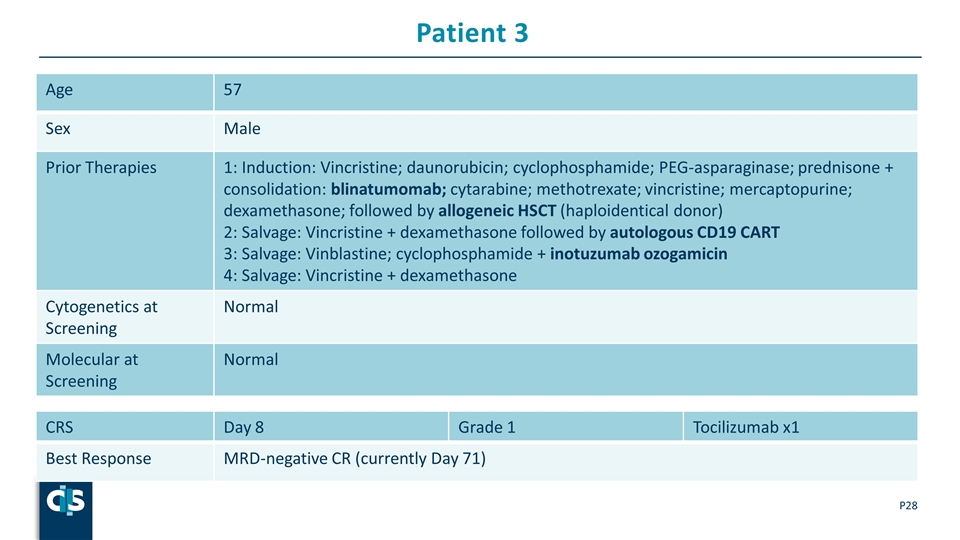

Patient 3 P Age 57 Sex Male Prior Therapies 1: Induction: Vincristine; daunorubicin; cyclophosphamide; PEG-asparaginase; prednisone + consolidation: blinatumomab; cytarabine; methotrexate; vincristine; mercaptopurine; dexamethasone; followed by allogeneic HSCT (haploidentical donor) 2: Salvage: Vincristine + dexamethasone followed by autologous CD19 CART 3: Salvage: Vinblastine; cyclophosphamide + inotuzumab ozogamicin 4: Salvage: Vincristine + dexamethasone Cytogenetics at Screening Normal Molecular at Screening Normal CRS Day 8 Grade 1 Tocilizumab x1 Best Response MRD-negative CR (currently Day 71)

Summary of UCART22 DL3 data Five subjects were dosed at DL3 (5 x 106 cells/kg) with UCART22 Process 1 (P1) using FCA LD: No safety issues, no Grade 2 or higher CRS 3 out of 5 clinical responses (60% ORR): 1 MRD neg. CR, 1 MRD neg. CRi, 1 MLFS All 3 of the responders failed multiple lines of prior therapy including chemotherapy, CD19 directed autologous CAR T cell therapy, and allogeneic stem cell transplant. Additionally, 1 of the 3 failed prior blinatumomab and inotuzumab.

Next steps for BALLI-01 Dosing started with UCART22 Process 2 (P2) made by Cellectis UCART22 P2 product candidate has shown a significantly higher potency in vitro than P1 1st subject dosing at DL2 (1 x 106 cells/kg) Next data set with P2 expected in 2023

SUMMARY AMELI-01 (UCART123) Adding alemtuzumab to the FC lymphodepletion regimen was associated with improved LD and significantly higher UCART123v1.2 cell expansion, which correlated with improved activity One patient in the DL2 FCA arm achieved >90% blast reduction at Day 28 One patient in the DL2 FCA arm achieved a long term durable MRD negative CR (now past 12 months) The study is enrolling patients in the FCA 2-dose regimen arm BALLI-01 (UCART22) 3 out of 5 clinical responses (60% ORR) at DL3: 1 MRD neg. CR, 1 MRD neg. CRi, 1 MLFS UCART22 Process 2 (P2) made by Cellectis at the Raleigh facility is now being used in the clinical study.

Discover, Create, Develop, Produce and Test Paris Paris, France ALPHA Study HQ, PD/AD, Starting Materials New York, New York Innovation, Clinical Development ̴25,000 sq ft. facility Gene Editing platform – TALEN® I/O discovery platform Gene therapy discovery platform Clinical development Raleigh, North Carolina UCART – Clinical & potential for Commercial ̴82,000 sq ft. facility Cell therapy GMP manufacturing QC labs Warehouse Cryogenic Storage rooms ̴55,000 sq ft. facility Process & analytical development Raw materials manufacturing QC labs Warehouse Cryogenic Storage rooms

Expected 2023 Milestones ALL, acute lymphoblastic leukemia; AML, acute myeloid leukemia; DL, dose level; FC, fludarabine + cyclophosphamide; FCA, fludarabine + cyclophosphamide + alemtuzumab; MM, multiple myeloma; NHL, non-Hodgkin’s lymphoma; RP2D, recommended Phase 2 dose; r/r, relapsed/refractory. 1st in human data update Data update with in-house manufactured product Enroll DL1 with FC lymphodepletion Data update with 2-dose regimen UCART22 r/r B-ALL UCART123 r/r AML UCARTCS1 r/r MM UCART20x22 r/r NHL

Thank You Cellectis Paris 8, rue de la Croix Jarry 75013 Paris – France Cellectis New York 430 East 29th Street New York, NY, 10016 – USA Cellectis Raleigh 2500 Sumner Boulevard Raleigh, NC, 27616 – USA Reach us at: investors@cellectis.com