Management Presentation January 2017 Liver Meeting of the American Association for the Study of Liver Diseases October 23rd, 2017

Disclaimer This presentation contains forward-looking statements. Forward-looking statements are neither historical facts nor assurances of future performance. Instead, they are based on Dova’s current beliefs, expectations and assumptions regarding the future of Dova’s business, future plans and strategies, Dova’s clinical results and other future conditions. All statements other than statements of historical facts contained in this presentation, including statements regarding future results of operations and financial position, business strategy, current and prospective product candidates, planned clinical trials and preclinical activities, product approvals, degree of market acceptance of approved products, research and development costs, current and prospective collaborations, timing and likelihood of success, plans and objectives of management for future operations, and future results of anticipated product candidates, are forward-looking statements. The words ”may,” “will,” “should,” “expect,” “plan,” “anticipate,” “could,” “intend,” “target,” “project,” “estimate,” “believe,” “estimate,” “predict,” “potential” or “continue” or the negative of these terms or other similar expressions are intended to identify forward-looking statements, although not all forward-looking statements contain these identifying words. The forward-looking statements in this presentation represent the presenters’ or Dova’s views as of the date of this presentation. Although Dova believes the expectations reflected in such forward-looking statements are reasonable, Dova can give no assurance that such expectations will prove to be correct. Accordingly, readers are cautioned not to place undue reliance on these forward-looking statements. Except as required by applicable law, Dova does not plan to publicly update or revise any forward-looking statements contained herein, whether as a result of any new information, future events, changed circumstances or otherwise. No representations or warranties (expressed or implied) are made about the accuracy of any such forward-looking statements. New risk factors and uncertainties may emerge from time to time, and it is not possible to predict all risk factors and uncertainties. For further information regarding these risks, uncertainties and other factors, you should read the “Risk Factors” section of Dova’s Quarterly Report on Form 10-Q for the quarter ended June 30, 2017, filed with the U.S. Securities and Exchange Commission (“SEC”) on August 14, 2017 and the other filings Dova makes with the SEC from time to time. Certain information contained in this presentation and statements made orally during this presentation relates to or is based on studies, publications, surveys and other data obtained from third-party sources and Dova’s own internal estimates and research. While Dova believes these third-party sources to be reliable as of the date of this presentation, it has not independently verified, and makes no representation as to the adequacy, fairness, accuracy or completeness of, any information obtained from third-party sources.

Dr. Lee Allen, CMO: Introduction Avatrombopag is an orally administered thrombopoietin receptor agonist that mimics the effects of endogenous thrombopoietin leading to the production of platelets Two completed pivotal Phase 3 clinical trials, ADAPT-1 and ADAPT-2, evaluated avatrombopag for the treatment of thrombocytopenia in patients with chronic liver disease scheduled to undergo a planned medical procedure who were undergoing procedures that had an associated bleeding risk Based on the positive safety and efficacy data, we announced the submission of our New Drug Application to the FDA on September 21st 3

Professor of Medicine at the University of California San Francisco, Division of Gastroenterology, and the Principal Investigator of our ADAPT-1 and ADAPT-2 clinical trials Nationally and internationally recognized for her work related to viral hepatitis in the setting of liver transplantation Author of more than 275 original articles, reviews and book chapters Served as Associate Editor for Hepatology and Deputy Editor for Liver Transplantation Associate Editor for Hepatology Communications Investigator on several NIH-funded clinical studies in hepatitis B and Non-alcoholic Fatty Liver Disease Investigator on several ongoing clinical trials Dr. Norah Terrault: Bio

Superiority of Avatrombopag to Placebo for the Treatment of Chronic Liver Disease-Associated Thrombocytopenia in Patients Undergoing Scheduled Procedures: Results of 2 Randomized, Placebo-Controlled Phase 3 Studies ADAPT-1 and ADAPT-2 Norah Terrault1, Francesco Bibbiani2, Yi-Cheng Chen3, Namiki Izumi4, Zeid Kayali5, Jose R. Lazcano Soto6, Paul Mitrut7, Won Young Tak8, Tarek I. Hassanein9 1University of California San Francisco, CA, USA; 2Eisai Medical Research Inc., Woodcliff Lake, NJ, United States; 3Chang Gung Memorial Hospital and University, Taoyuan, Taiwan; 4Musashino Red Cross Hospital, Tokyo, Japan; 5Inland Empire Liver Foundation, Rialto, CA, USA; 6IAAN Mexico, Durango, Mexico; 7University of Medicine and Pharmacy of Craiova, Romania; 8Kyungpook National University, Daegu, Korea; 9Southern California GI and Liver Centers, Coronado, USA

Thrombocytopenia and Chronic Liver Disease Severe thrombocytopenia (platelet count <50 x 109/L) is common in patients chronic liver disease Platelet transfusions are current standard of care to reduce risk of bleeding during invasive procedures with Associated with risk refractoriness pharmacological of transfusion reactions, infections and induction of platelet No treatments are currently licensed for this indication It binds to a different site on the TPO receptor than endogenous TPO, so effects of avatrombopag and TPO are additive the Afdhal N et al. J Hepatol. 2008; 48(6): 1000-1007; Hod E and Schwartz J. Br J Haematol. 2008; 142(2): 348-360; Giannini EG. Aliment Pharmacol Ther. 2006; 23(8): 1055-1065 Meehan KR et al. Am J Hematol. 2000; 64(4): 251-256 Rebulla P. Haematologica. 2005; 90(2): 247-253 6 Avatrombopag-an oral, small molecule TPO receptor agonist being developed to provide a measured increase in platelet count as an alternative to platelet transfusions

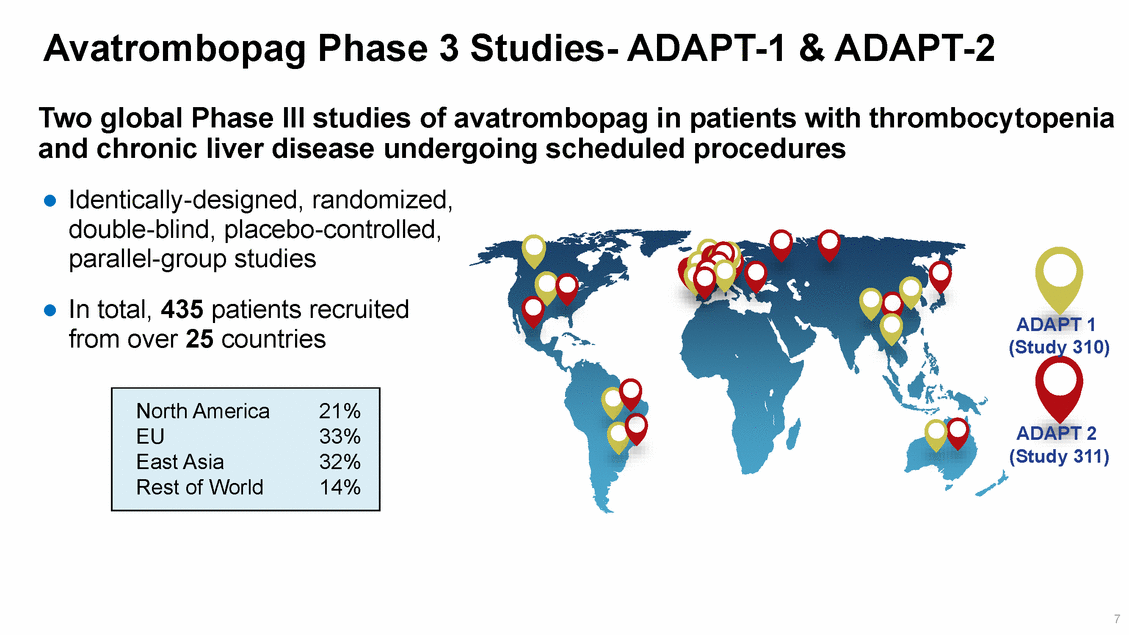
Avatrombopag Phase 3 Studies-ADAPT-1 & ADAPT-2 Two global Phase III studies of avatrombopag in patients with thrombocytopenia and chronic liver disease undergoing scheduled procedures Identically-designed, randomized, double-blind, placebo-controlled, parallel-group studies In total, 435 patients recruited ADAPT 1 (Study 310) from over 25 countries ADAPT 2 (Study 311) 7 North America 21% EU 33% East Asia 32% Rest of World 14%
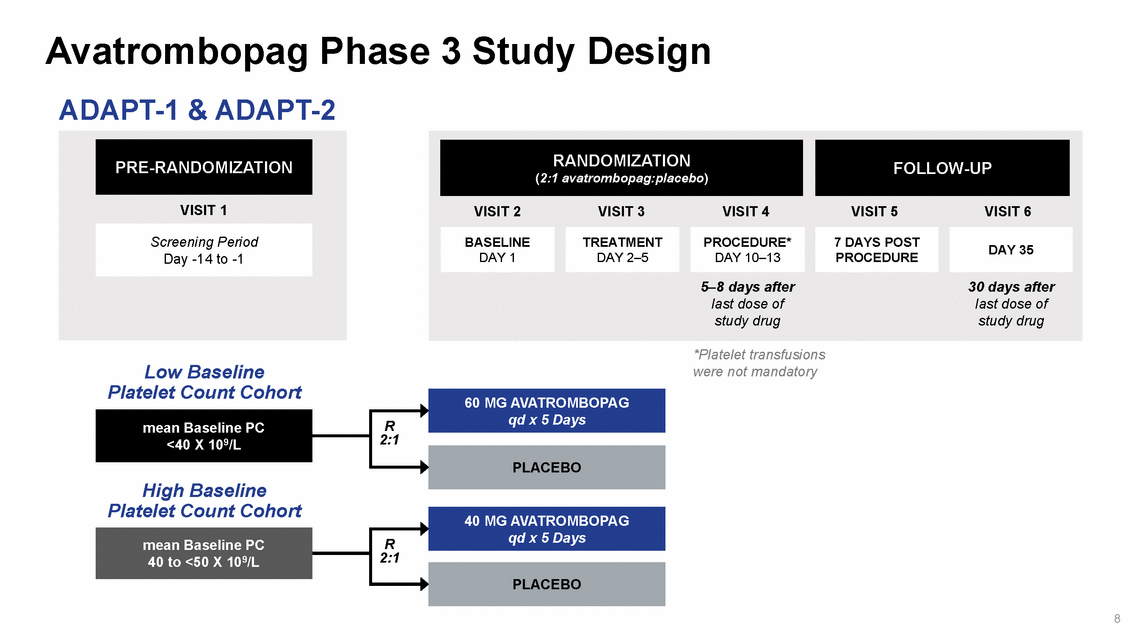
Avatrombopag Phase 3 Study Design ADAPT-1 & ADAPT-2 *Platelet transfusions were not mandatory Low Baseline Platelet Count Cohort R 2:1 High Baseline Platelet Count Cohort R 2:1 8 PLACEBO mean Baseline PC 40 to <50 X 109/L 40 MG AVATROMBOPAG qd x 5 Days PLACEBO mean Baseline PC <40 X 109/L 60 MG AVATROMBOPAG qd x 5 Days VISIT 2VISIT 3VISIT 4VISIT 5VISIT 6 PROCEDURE 5–8 days after 30 days after last dose oflast dose of study drugstudy drug 7 DAYS POST DAY 35 PROCEDURE* DAY 10–13 TREATMENT DAY 2–5 BASELINE DAY 1 FOLLOW-UP RANDOMIZATION (2:1 avatrombopag:placebo) VISIT 1 Screening Period Day -14 to -1 PRE-RANDOMIZATION
Avatrombopag Phase 3 Study Population Criteria ADAPT-1 & ADAPT-2 disorders, or cardiovascular disease syndromes agents within 7 days of screening (females) *Platelet counts were measured on 2 separate occasions: During the Screening Period and at Baseline at least 1 day apart with neither platelet count >60 x 109/L 9 MAIN INCLUSION CRITERIA MAIN EXCLUSION CRITERIA Aged >18 years History of arterial or venous thrombosis, hematologic Chronic liver disease Known medical history of genetic pro-thrombotic Mean Baseline platelet count <50 x 109/L* Platelet transfusion or use of erythropoietin-stimulating MELD score <24 at screening Portal vein flow <10 cm/sec at Screening Scheduled to undergo an invasive procedure Hemoglobin <8 g/dL or >18 g/dL (males) or >15 g/dL Hepatocellular carcinoma (HCC) allowed if Barcelona Clinic Liver Cancer Stage A or B

ADAPT-1 & ADAPT-2: Outcome Measures PRIMARY EFFICACY ENDPOINT: SECONDARY EFFICACY ENDPOINTS: SAFETY ENDPOINTS: 10 Adverse events, serious adverse events, Adverse Events of Special Interest (AESI) Proportion of patients achieving the target platelet count (>50 x 109/L) Magnitude of change in platelet count from Baseline to Procedure Day Proportion of patients not requiring platelet transfusion or any bleeding rescue procedure up to 7 days post-procedure Rescue procedures included: platelet transfusion, fresh frozen plasma (FFP), cryoprecipitate, vitamin K (phytonadione), desmopression, recombinant activated factor VII, aminocaproic acid, tranexamic acid, whole blood transfusion, packed red cell transfusion, surgical intervention or interventional radiology

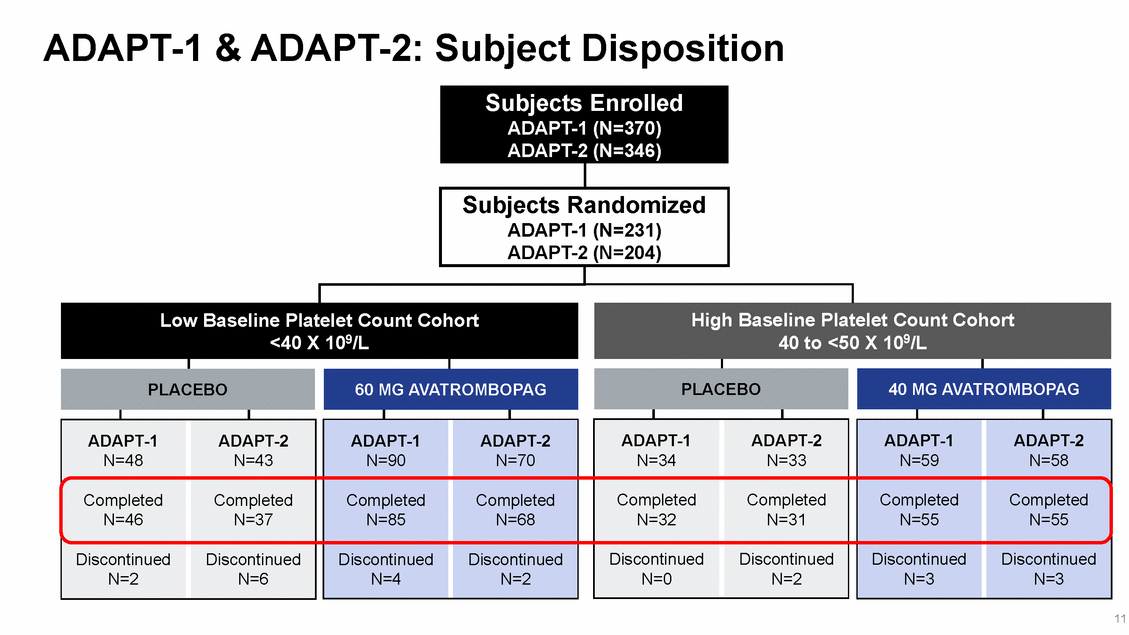
ADAPT-1 & ADAPT-2: Subject Disposition 11 Subjects Enrolled ADAPT-1 (N=370) ADAPT-2 (N=346) Subjects Randomized ADAPT-1 (N=231) ADAPT-2 (N=204) Low Baseline Platelet Count Cohort <40 X 109/L High Baseline Platelet Count Cohort 40 to <50 X 109/L PLACEBO 60 MG AVATROMBOPAG PLACEBO 40 MG AVATROMBOPAG ADAPT-1 N=48 Completed N=46 Discontinued N=2 ADAPT-2 N=43 Completed N=37 Discontinued N=6 ADAPT-1 N=90 Completed N=85 Discontinued N=4 ADAPT-2 N=70 Completed N=68 Discontinued N=2 ADAPT-1 N=34 Completed N=32 Discontinued N=0 ADAPT-2 N=33 Completed N=31 Discontinued N=2 ADAPT-1 N=59 Completed N=55 Discontinued N=3 ADAPT-2 N=58 Completed N=55 Discontinued N=3
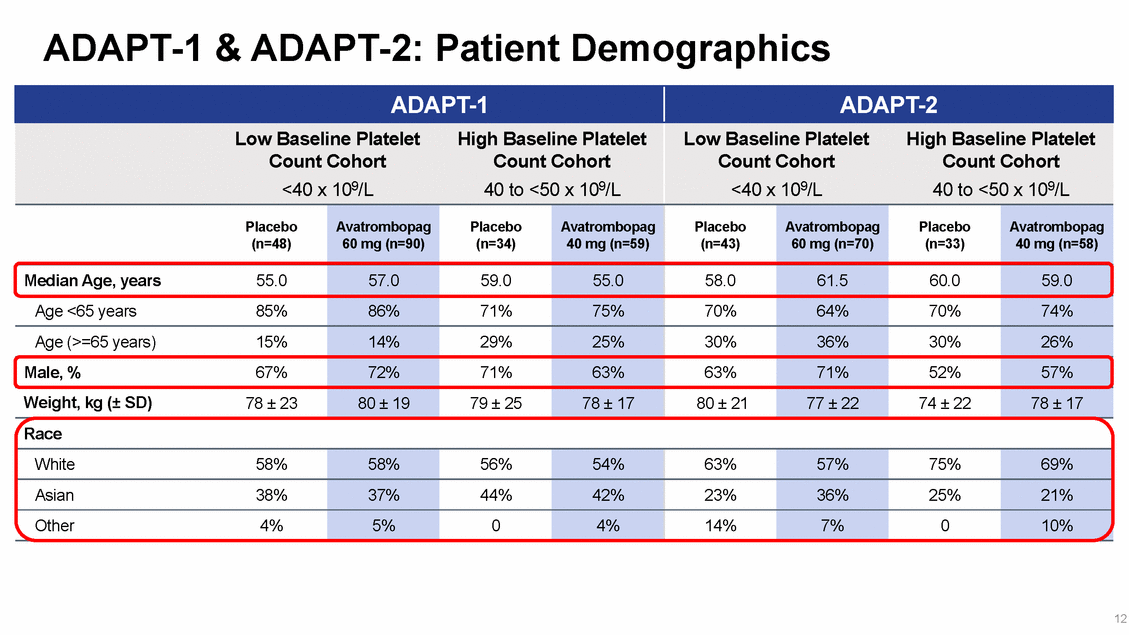
ADAPT-1 & ADAPT-2: Patient Demographics Race 12 White58% 58% 56% 54% 63% 57% 75% 69% Asian38% 37% 44% 42% 23% 36% 25% 21% Other4% 5% 0 4% 14% 7% 0 10% ADAPT-1 ADAPT-2 Low Baseline PlateletHigh Baseline Platelet Count CohortCount Cohort <40 x 109/L 40 to <50 x 109/L Low Baseline PlateletHigh Baseline Platelet Count CohortCount Cohort <40 x 109/L 40 to <50 x 109/L Placebo (n=48) Avatrombopag 60 mg (n=90) Placebo (n=34) Avatrombopag 40 mg (n=59) Placebo (n=43) Avatrombopag 60 mg (n=70) Placebo (n=33) Avatrombopag 40 mg (n=58) Median Age, years55.0 57.0 59.0 55.0 58.0 61.5 60.0 59.0 Age <65 years85% 86% 71% 75% 70% 64% 70% 74% Age (>=65 years)15% 14% 29% 25% 30% 36% 30% 26% Male, %67% 72% 71% 63% 63% 71% 52% 57% Weight, kg (± SD)78 ± 23 80 ± 19 79 ± 25 78 ± 17 80 ± 21 77 ± 22 74 ± 22 78 ± 17
APAPT-1 & ADAPT-2: Disease Characteristics 13 ADAPT-1 ADAPT-2 Low Baseline PlateletHigh Baseline Platelet Count CohortCount Cohort <40 x 109/L 40 to <50 x 109/L Low Baseline PlateletHigh Baseline Platelet Count CohortCount Cohort <40 x 109/L 40 to <50 x 109/L Placebo (n=48) Avatrombopag 60 mg (n=90) Placebo (n=34) Avatrombopag 40 mg (n=59) Placebo (n=43) Avatrombopag 60 mg (n=70) Placebo (n=33) Avatrombopag 40 mg (n=58) Mean Baseline Platelet Count Cohort (± SD)31 ± 7 31 ± 7 45 ± 3 44 ± 3 33 ± 6 33 ± 5 45 ± 3 44 ± 4 Disease Etiology, % Alcoholic Liver Disease15 15 6 19 16 17 15 10 Chronic Viral Hepatitis63 56 79 63 61 49 55 50 Nonalcoholic Steatohepatitis8 7 0 7 12 14 15 10 Other15 23 15 11 12 20 15 29 Hepatocellular Carcinoma, %23 24 21 29 33 30 33 26 Mean MELD Score (SD)11 (3) 11 (3) 10 (3) 12 (4) 11 (3) 11 (3) 11 (4) 11 (4) Child-Turcotte-Pugh Grade, % Grade A63 55 61 53 49 64 49 55 Grade B35 43 36 38 49 29 36 38 Grade C2 2 3 9 2 7 15 7
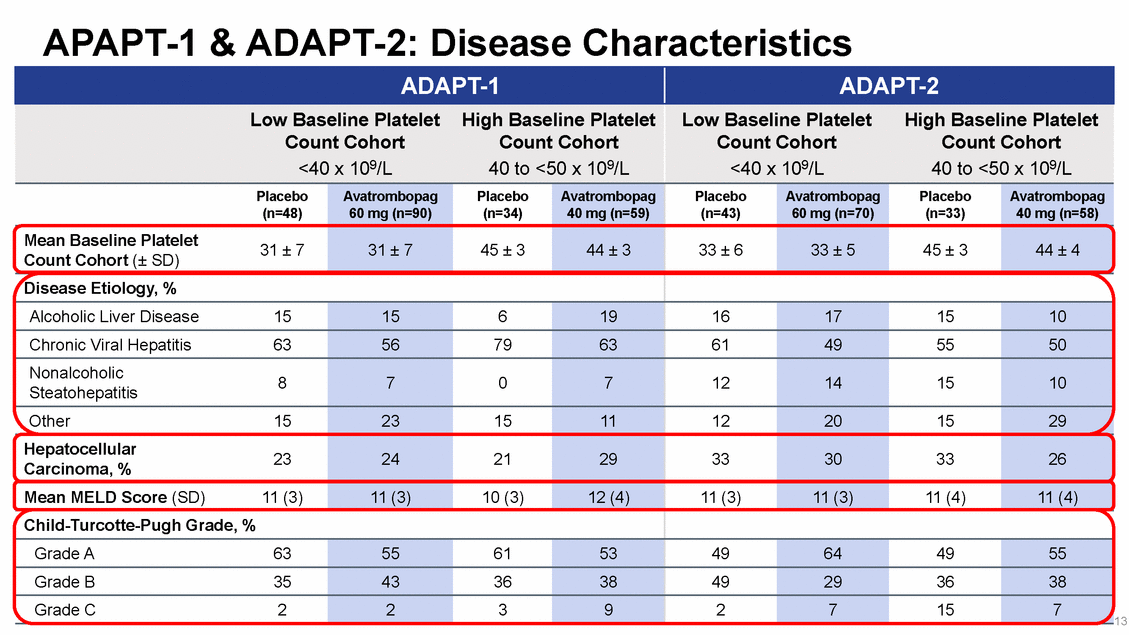
ADAPT-1 & ADAPT-2: Scheduled Procedures by Bleeding Risk Count Cohort Count Cohort Upper GI endoscopy +/-biopsy 14 Low Bleeding Risk Procedures Thoracentesis Paracentesis Endoscopy Upper GI endoscopy +/-variceal banding, +/-sclerotherapy Colonoscopy +/-polypectomy/biopsy Moderate Bleeding Risk Procedures Liver biopsy Bronchoscopy +/-biopsy Ethanol ablation Chemoembolization for HCC High Bleeding Risk Procedures Biliary interventions Dental procedures Transjugular intrahepatic portosystemic shunt Laparoscopic interventions Nephrostomy tube placement Radiofrequency ablation Renal biopsy Vascular catheterization ADAPT-1 ADAPT-2 Low Baseline PlateletHigh Baseline Platelet BleedingCount CohortCount Cohort Risk<40 x 109/L 40 to <50 x 109/L Low Baseline PlateletHigh Baseline Platelet <40 x 109/L 40 to <50 x 109/L Placebo (n=48) Avatrombopag 60 mg (n=90) Placebo (n=34) Avatrombopag 40 mg (n=59) Placebo (n=43) Avatrombopag 60 mg (n=70) Placebo (n=33) Avatrombopag 40 mg (n=58) Low%68 67 66 59 53 60 53 58 Moderate %20 12 9 20 23 16 28 16 High %13 21 25 21 25 24 19 26
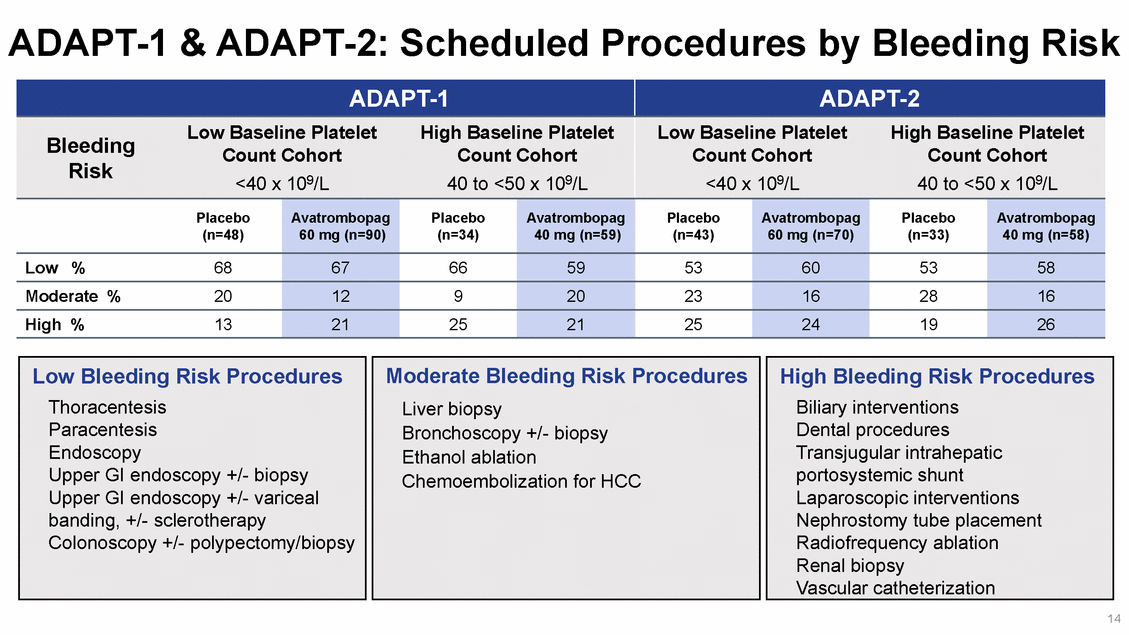
ADAPT-1 & ADAPT-2: Primary Endpoint Proportion of Patients Who Did NOT Require Platelet Transfusion or Any Low Baseline Platelet Count Cohort <40 x 109/L Rescue Procedure for Bleeding* High Baseline Platelet Count Cohort 40 to <50 x 109/L 100 90 80 70 60 50 40 30 20 10 *Full Analysis Set 0 15 ADAPT-1 ADAPT-2 ADAPT-1 ADAPT-2 Patients (%) Placebo Avatrombopag p<0.0001p<0.0006p<0.0001p<0.0001 88% 88% 69% 66% 38% 35% 33% 23%
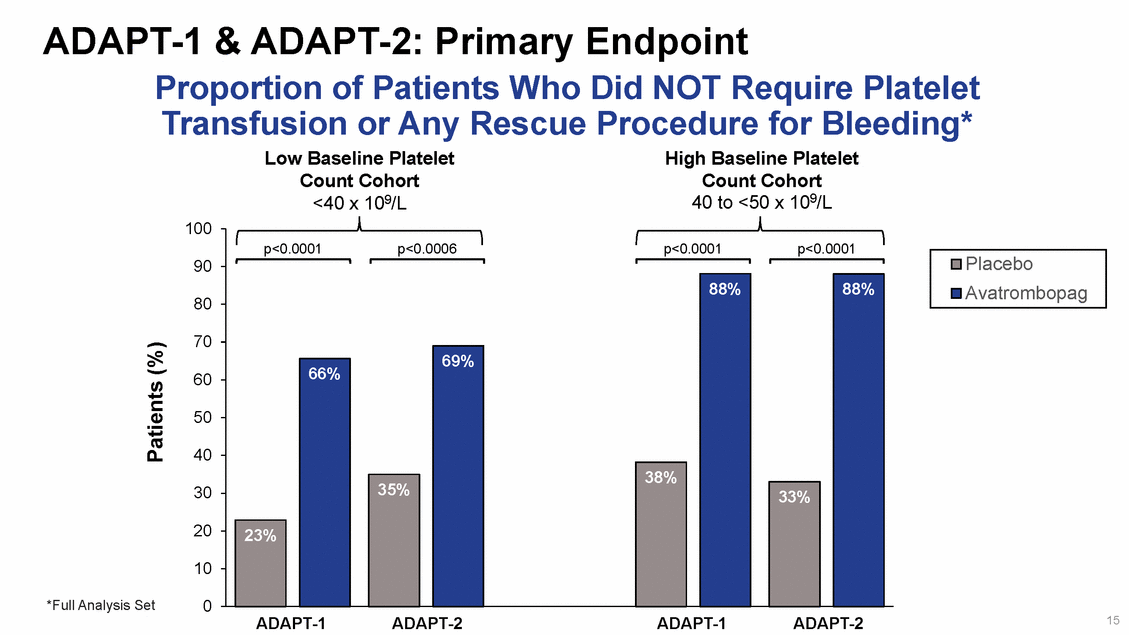
ADAPT-1 & ADAPT-2: Secondary Endpoint Proportion of Patients Who Achieved Platelet Counts > 50 x 109/L Low Baseline Platelet Count Cohort <40 x 109/L on Procedure Day* High Baseline Platelet Count Cohort 40 to <50 x 109/L 100 90 80 70 60 50 40 30 20 10 0 *Full Analysis Set 16 ADAPT-1 ADAPT-2 ADAPT-1 ADAPT-2 Patients (%) Placebo Avatrombopag p<0.0001p<0.0001p<0.0001p<0.0001 93% 88% 39% 4% 69% 7% 67% 21%
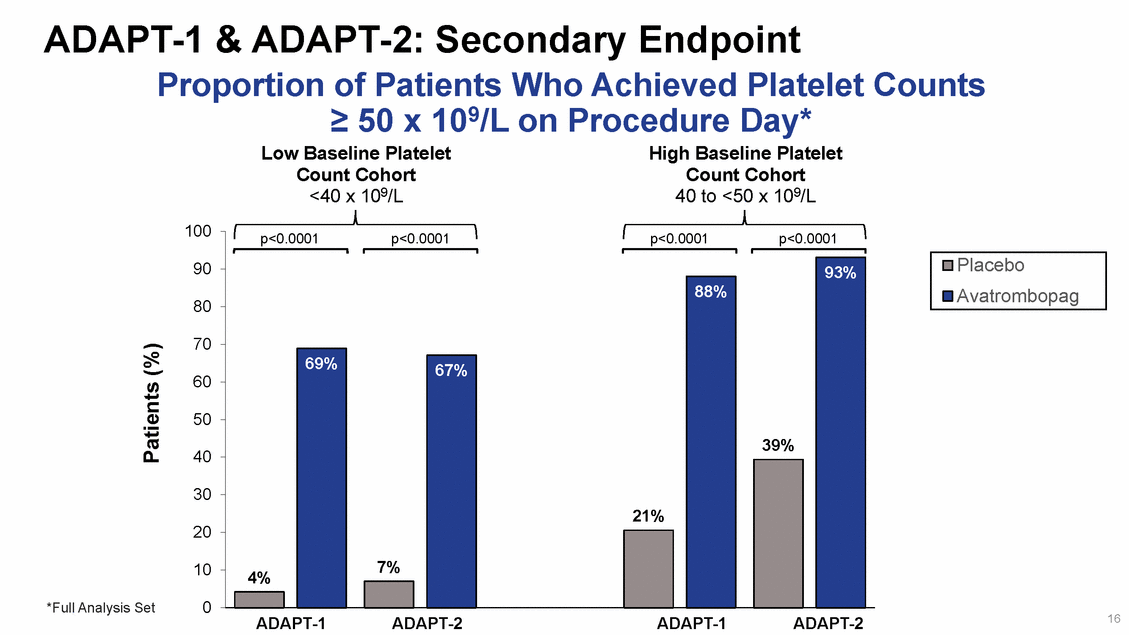
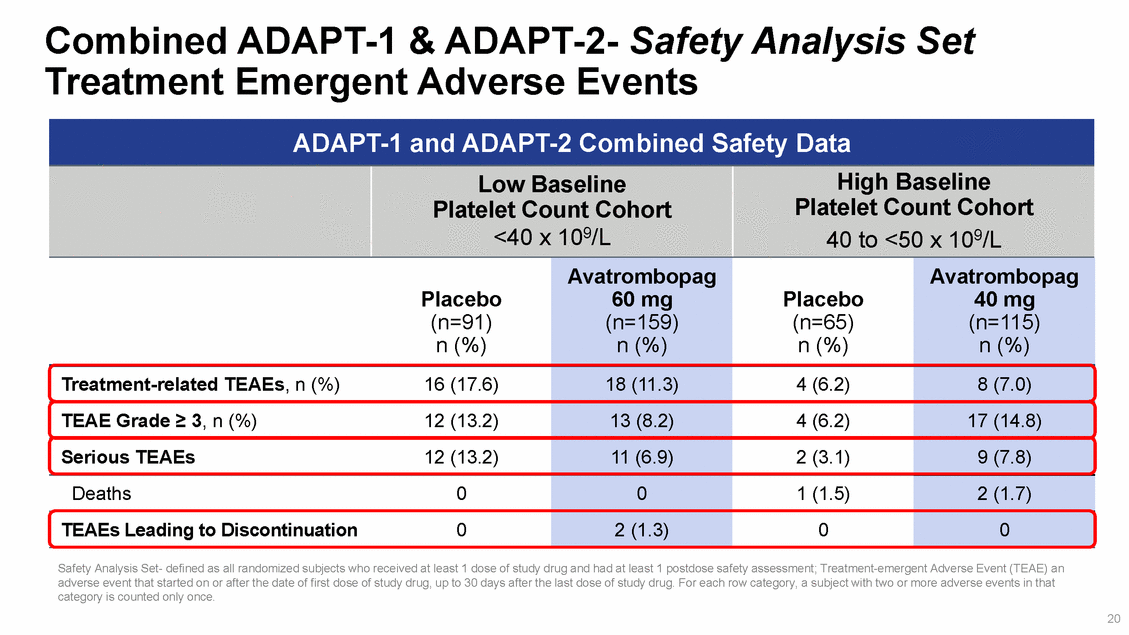
ADAPT-1 & ADAPT-2: Secondary Endpoint Magnitude of Change in Platelet Count from Baseline to Procedure Day* Low Baseline Platelet Count Cohort <40 x 109/L High Baseline Platelet Count Cohort 40 to <50 x 109/L 50 45 40 35 30 25 20 15 10 5 *Full Analysis Set #Hodges-Lehmann Estimator 0 17 ADAPT-1 ADAPT-2 ADAPT-1 ADAPT-2 Mean Change in Platelet Count x 109/L Placebo Avatrombopag 28 x 109/L# 25 x 109/L # 33 x 109/L # 36 x 109/L # p<0.0001p<0.0001p<0.0001p<0.0001 45 37 6 1 32 3 31 1
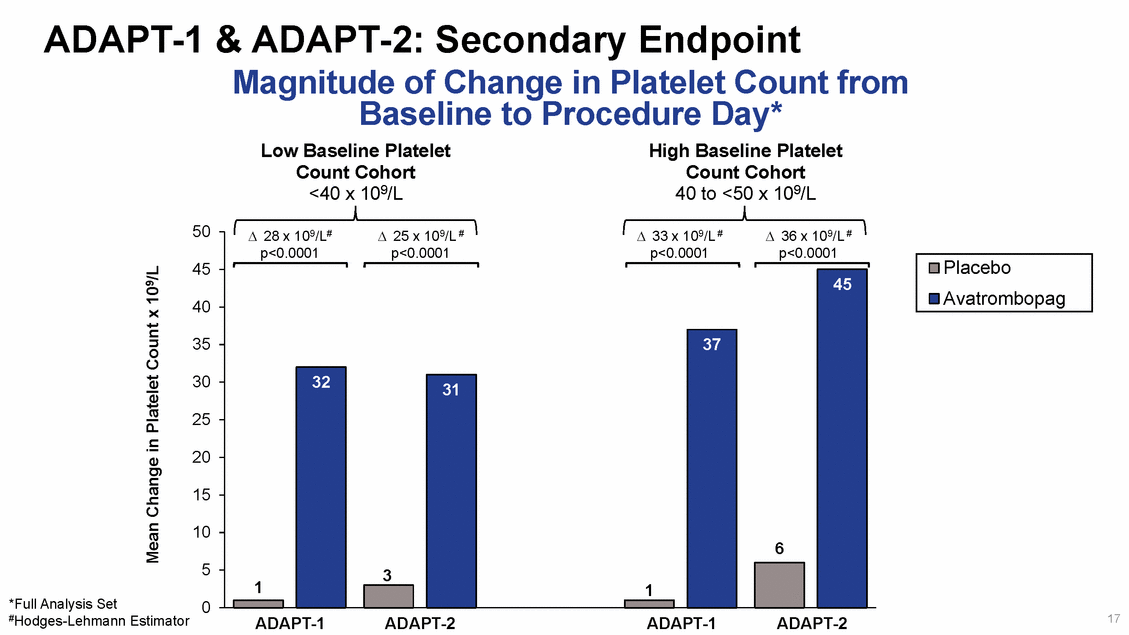
ADAPT-1 & ADAPT-2: Change in Platelet Count Over Time Platelet counts reproducibly increased from Day 4, peaked at Day 10-13, and returned to Baseline levels by Day 35 Only 3 (1.1%) avatrombopag-treated patients had platelet counts >200 x109/L at any time during the study ADAPT-1 ADAPT-2 100 100 90 90 80 80 70 70 60 60 50 50 40 40 30 30 0 5 10 15 20 25 30 35 0 5 10 15 20 25 30 35 Days Visit 15 Day 17 Days Visit 2 Day 1 Baseline Visit 3 Day 4 Visit 4 Day 10 Procedure Day Visit 6 Day 35 Visit 2 Day 1 Baseline Visit 3 Day 4 Visit 4 Day 10 Procedure Day Visit 15 Day 17 Visit 6 Day 35 18 Mean Platelet Count x 109/L Mean Platelet Count x 109/L DOSING DOSING ort: ort: Low Baseline Platelet Count Cohort: 60 mg Avatrombopag Placebo High Baseline Platelet Count Cohort: 40 mg Avatrombopag Placebo Low Baseline Platelet Count Coh 60 mg Avatrombopag Placebo High Baseline Platelet Count Coh 40 mg Avatrombopag Placebo
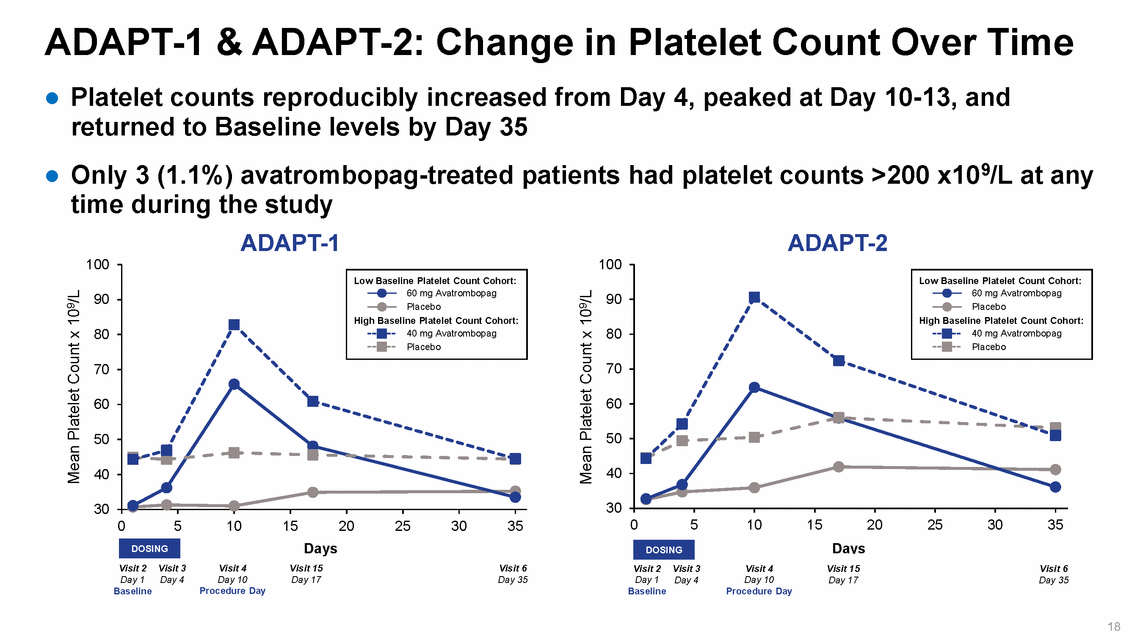
Combined ADAPT-1 & ADAPT-2-Safety Analysis Set Most Frequently Reported TE-Emergent Adverse Events Platelet Count Cohort Safety Analysis Set-defined as all randomized subjects who received at least 1 dose of study drug and had at least 1 postdose safety assessment; Treatment-emergent Adverse Event (TEAE) an adverse event that started on or after the date of first dose of study drug, up to 30 days after the last dose of study drug. For each row category, a subject with two or more adverse events in that category is counted only once. 19 ADAPT-1 and ADAPT-2 Combined Safety Data Low Baseline Platelet Count Cohort <40 x 109/L High Baseline 40 to <50 x 109/L Placebo (n=91) n (%) Avatrombopag 60 mg (n=159) n (%) Placebo (n=65) n (%) Avatrombopag 40 mg (n=115) n (%) TEAEs, n (%)53 (58.2) 89 (56.0) 33 (50.8) 59 (51.3) Pyrexia (fever)8 (8.8) 18 (11.3) 6 (9.2) 9 (7.8) Abdominal pain6 (6.6) 10 (6.3) 4 (6.2) 8 (7.0) Nausea7 (7.7) 10 (6.3) 4 (6.2) 8 (7.0) Headache7 (7.7) 7 (4.4) 3 (4.6) 8 (7.0) Diarrhea4 (4.4) 7 (4.4) 2 (3.1) 3 (2.6) Fatigue4 (4.4) 7 (4.4) 1 (1.5) 3 (2.6)
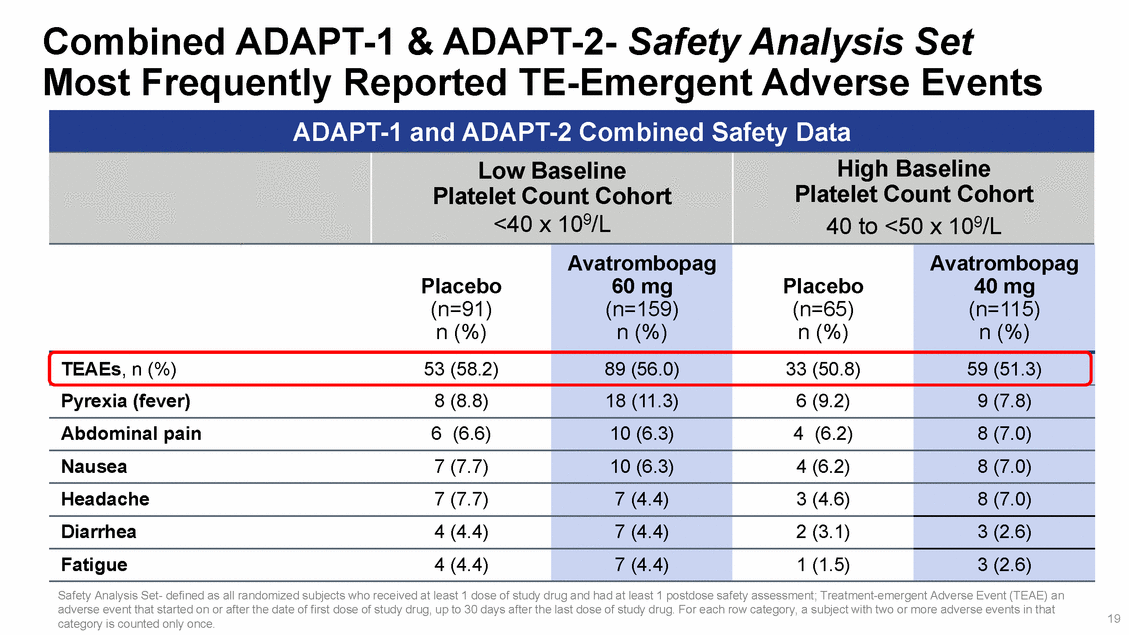
Combined Treatment ADAPT-1 & ADAPT-2-Safety Analysis Set Emergent Adverse Events Platelet Count Cohort Safety Analysis Set-defined as all randomized subjects who received at least 1 dose of study drug and had at least 1 postdose safety assessment; Treatment-emergent Adverse Event (TEAE) an adverse event that started on or after the date of first dose of study drug, up to 30 days after the last dose of study drug. For each row category, a subject with two or more adverse events in that category is counted only once. 20 ADAPT-1 and ADAPT-2 Combined Safety Data Low Baseline Platelet Count Cohort <40 x 109/L High Baseline 40 to <50 x 109/L Placebo (n=91) n (%) Avatrombopag 60 mg (n=159) n (%) Placebo (n=65) n (%) Avatrombopag 40 mg (n=115) n (%) Treatment-related TEAEs, n (%)16 (17.6) 18 (11.3) 4 (6.2) 8 (7.0) TEAE Grade > 3, n (%)12 (13.2) 13 (8.2) 4 (6.2) 17 (14.8) Serious TEAEs12 (13.2) 11 (6.9) 2 (3.1) 9 (7.8) Deaths0 0 1 (1.5) 2 (1.7) TEAEs Leading to Discontinuation0 2 (1.3) 0 0
ADAPT-1 & ADAPT-2: Deaths & Adverse Events Leading to Discontinuation TEAEs Leading to Study Drug Discontinuation N=2 (1.3%) in ADAPT-1 both in the 60 mg Avatrombopag Myalgia and anemia; possibly study drug-related Pyrexia; unrelated to study drug Treatment Group Deaths N=2 (1.7%) in ADAPT-1 both in the 40 mg Avatrombopag not considered to be study drug-related 54 yo male died of multiorgan failure on study Day 40 54 yo female died of hepatic coma on study Day 34 Treatment Group; N=1 (1.5%) in ADAPT-2 In the Placebo Treatment Group; not considered to be study drug-related 53 yo male died of acute myocardial infarction and multiple organ dysfunction on study Day 31 21

ADAPT-1 & ADAPT-2: Adverse Events of Special Interest Medically Significant Events N=1 (0.4% in avatrombopag-exposed) TEAE of partial portal vein thrombosis 71 yo male in the 40 mg Avatrombopag treatment group on Study Day 18 (Visit 5), 13 days after the last dose Scheduled Procedure: Upper gastrointestinal endoscopy with variceal banding Platelet count 45 x109/L at Baseline that increased to 77 x 109/L on Procedure Day (study Day 11), and then decreased to 61 x 109/L on Day 18 and 45 x109/L on study Day 37 Event was judged as non-serious and potentially drug-related 22

Summary and Conclusions Avatrombopag was superior to placebo in: Reducing the need for platelet transfusion or any rescue procedure for bleeding following a scheduled procedure Increasing the proportion of patients achieving the target platelet count (>50 x 109/L) Increasing the platelet count from Baseline to Procedure Day Platelet counts reproducibly increased after 4 and returned to Baseline by Day 35 days, peaked after 10-13 days, Safety profile of avatrombopag was similar to placebo 23 Avatrombopag offers a safe and effective alternative to platelet transfusion for patients with thrombocytopenia and chronic liver disease undergoing scheduled procedures

Questions & Answers
