 Summary of Allegations in the Complaint Filed by Tenet Healthcare Corporation Against Community Health Systems April 11, 2011 Exhibit 99.2 |
  2 Additional Information Tenet Healthcare Corporation (“Tenet”) will file with the Securities and Exchange Commission (“SEC”) a proxy statement, accompanied by a WHITE proxy card, in connection with its 2011 annual meeting of stockholders. Any definitive proxy statement will be mailed to stockholders of Tenet. INVESTORS AND SECURITYHOLDERS OF TENET ARE URGED TO READ THESE AND OTHER DOCUMENTS FILED WITH THE SEC CAREFULLY IN THEIR ENTIRETY WHEN THEY BECOME AVAILABLE BECAUSE THEY WILL CONTAIN IMPORTANT INFORMATION. Investors and securityholders will be able to obtain free copies of these documents (when available) and other documents filed with the SEC by Tenet through the website maintained by the SEC at http://www.sec.gov. The information contained in this filing is a summary of allegations made in a complaint filed by Tenet against Community Health Systems, Inc., Wayne T. Smith, and W. Larry Cash on April 11, 2011, in the United States District Court for the Northern District of Texas. A copy of the complaint has been filed by Tenet with the SEC and is available through the website maintained by the SEC at http://www.sec.gov. Certain Information Regarding Participants Tenet and certain of its respective directors and executive officers are deemed to be participants under the rules of the SEC. Information regarding these participants is contained in a filing under Rule 14a-12 filed by Tenet with the SEC on January 7, 2011. This filing and other documents can be obtained free of charge from the source indicated above. Additional information regarding the interests of these participants in any proxy solicitation and a description of their direct and indirect interests, by security holdings or otherwise, will also be included in any proxy statement and other relevant materials to be filed with the SEC if and when they become available. Legal disclaimer |
  3 Overview CHS has for many years systematically billed cases as higher-paying inpatient admissions that would have been billed as lower-paying outpatient observations in most U.S. hospitals. CHS’ strategy specifically focuses on converting emergency room visits to medically unnecessary inpatient admissions. When patients present themselves to hospitals, they are either 1) seen and discharged; 2) placed in outpatient observation status; or 3) admitted as inpatients. Doctors make the treatment decision, with input from hospital employees. Most (>75%) U.S. hospitals use one of two objective systems as the basis for these determinations. CHS uses its own set of “Admissions Justifications” called the “Blue Book.” The difference in Medicare payments between an outpatient observation stay and an inpatient admission is substantial. Other payers (e.g., Medicaid and Managed Care) generally pay more for inpatient admissions than for observations, but actual rates depend on contracts. Only Medicare fee-for-service data is publicly available. CHS’ use of observation status is less than half the national average rate for U.S. hospitals. There is no legitimate explanation for the difference. No other publicly traded hospital company follows a similar practice. |
  4 CHS’ strategy of driving up admissions and driving down observations is unsustainable: It depends on a continuing pipeline of acquisitions of hospitals with normal observation rates that can be driven down. CHS dropped Triad’s observation rate 52% following the acquisition. Low observations, one-day stays, and related issues are already a focus area of government investigators and contractors. Implications for CHS: Unwinding the strategy will materially reduce admissions, revenues, profits, and cash flows going forward. Potential liability is well in excess of $1 billion for 2006 – 2009 for the Medicare fee- for-service portion of CHS’ business alone. Serious questions are raised regarding the accuracy of CHS’ historical financial statements. Implications for CHS’ $6 proposal to acquire Tenet: CHS’ stock is worth less than stated. CHS’ ability to finance the cash portion of the offer may be impaired. Overview, cont. |
  5 What is the nature of this litigation? The litigation seeks to compel CHS to disclose fully its unique and non-industry standard patient admissions criteria and billing practices and the financial and legal implications arising from them. Under SEC rules, CHS’ statements are proxy solicitation materials directed toward Tenet’s stockholders. CHS’ actions have resulted in materially misleading financial reports and statements: • Admissions statistics and trends have been overstated. • Revenues, profits, and cash flows have been overstated. • CHS’ explanations of business trends have been misleading. • CHS’ explanations of synergies from acquired hospitals have been misleading and incomplete. CHS has followed an unsustainable business practice that is inconsistent with Federal regulations. Substantial undisclosed liabilities may exist to Medicare, state Medicaid programs, private insurance companies, and patients. The litigation seeks to compel CHS to fully and accurately disclose the risks and financial impact of its admissions strategy, and to prevent further misleading statements. |
  6 Has CHS violated Medicare requirements? Medicare reimburses hospitals only for treatment that is “reasonable and necessary.” 42 U.S.C. § 1395y(a)(1)(A). Inpatient care rather than outpatient care is required only if the patient’s medical condition, safety or health would be significantly and directly threatened if care was provided in a less intensive setting. Medicare Program Integrity Manual, Chapter 6, Section 6.5.2. Outpatient observation is a well-defined set of specific, clinically appropriate services, which include ongoing short term treatment, assessment and reassessment, rendered before a decision can be made regarding whether a patient will require further treatment as an inpatient or is able to be discharged. Observation services are commonly ordered for patients who present to the emergency department and who require a period of treatment or monitoring before making a decision on admission or discharge. Medicare Benefit Policy Manual, Chapter 6, Section 20.6. See also Medicare Claims Processing Manual, Chapter 4, Section 290. CHS causes patients to be admitted to its hospitals who should be observed under Medicare requirements. CHS overbills these cases as inpatient admissions when they should be billed as outpatient observations. CHS systematically overbills Medicare and likely other payers. |
  7 How did Tenet learn of these practices? CHS stated on a December 10, 2010 conference call that a combination with Tenet would offer opportunities for synergies. Tenet conducted due diligence to evaluate potential synergies that might be created through a combination with CHS. Tenet’s independent consultant, using the American Hospital Directory database, found significant discrepancies between admission patterns at CHS and the industry. Tenet then engaged a second consulting firm, Avalere Health LLC, to perform a second independent analysis using the Centers for Medicare & Medicaid Services’ Inpatient Prospective Payment System Standard Analytic Files (which contains source data from which the MedPAR database is constructed) and Outpatient Standard Analytic Files. Each analysis found CHS’ observation rate* to be significantly lower than the industry and its peer companies. CHS “grew” admissions by implementing dramatic reductions in observation status at hospitals it acquired, particularly in the case of Triad. Two independent consultants have confirmed that CHS’ observation rate is less than half of the national average. * A hospital’s “observation rate” is essentially the percentage of patients treated in a hospital bed that are billed as “observation” rather than “inpatient.” |
  8 CHS’ strategy inflates admissions, revenues, profits, and cash flows CHS admitted approximately 62,000 Medicare fee-for-service patients from 2006-2009 (approximately 20,000 in 2009 alone) who would have been observed as outpatients if CHS’ observation rate were at the national average. CHS admitted approximately 82,000 Medicare fee-for-service patients from 2006-2009 (approximately 31,000 in 2009 alone) who would have been observed as outpatients if CHS’ observation rate were the same as LifePoint. Taking only CHS’ highest volume and lowest acuity Medicare patients, CHS receives, on average, over $3,300 (or approximately 257%) more per “admitted” patient than “observed” patient. Medicare fee-for-service patients generated 27% of CHS’ net operating revenue in 2010. The effect of CHS’ admissions strategy on its performance is much greater if the strategy has been applied across all patient categories. This practice results in greater profits to CHS, but additional costs to Medicare, and likely to Medicaid programs, private insurance companies, and patients. CHS systematically overbills Medicare, and likely other payers, overstating profits. |
  9 These practices may subject CHS to substantial undisclosed liability Under the Federal False Claims Act, the government may recover damages of up to three times the originally billed amount, plus penalties of up to $11,000 per false claim. 31 USC § 3729(a). As a result of CHS’ admissions practices, it may have overbilled payers for Medicare fee- for-service patients by approximately $280 million to $377 million in 2006-2009 alone. If treated as false claims, this conduct could result in liabilities well in excess of $1 billion for 2006-2009 alone. As the Blue Book was copyrighted in 2000, it appears the practice of driving down observation status has existed for at least ten years. During this same period, CHS likely overbilled other payers as well, such as Medicare Advantage plans. CHS’ hospitals may also be subject to exclusion from participating in Medicare. CHS may have significant financial exposure and could face exclusion from participating in Medicare. * |
  10 CHS’ admissions practices are not sustainable The Office of Inspector General of the U.S. Department of Health and Human Services (“OIG”) closely scrutinizes medically unnecessary inpatient admissions. In late 2010, Medicare Recovery Audit Contractors (RACs) began recovering overpayments from medically unnecessary inpatient admissions. Numerous non-CHS hospitals with low observation rates have been investigated by the U.S. Department of Justice. In its 10-K, CHS disclosed that the OIG issued a subpoena for documents related to, among other things, CHS’ admissions criteria, case management, coding, billing, and compliance in its hospital in Laredo, Texas. CHS also disclosed that the Attorney General of Texas issued Civil Investigative Demands for all of CHS’ hospitals in Texas concerning “emergency department procedures and billing.” |
  11 CHS’ observation rate is much lower than other large hospital groups and the industry as a whole * Observation rate is defined as total unique observation claims divided by the sum of total unique observation claims and total inpatient short-stay acute care hospital claims. ** National average represents all short-stay acute care hospitals with emergency departments and observation stays, with the exception of critical access hospital (CAHs); for a total of 3,004 hospitals in 2009. *** Our analysis limited the 130 CHS hospitals to 111 hospitals in 2009, which excluded 3 non-inpatient short-stay acute care hospitals, 4 hospitals acquired in 2010, 6 CAHs, and 6 hospitals that did not bill for ER visits and/or observation stays. Source: Analysis based on the Centers for Medicare & Medicaid Services’ Outpatient Standard Analytic Files (SAFs) for CYs 2006-2009 and the Inpatient Prospective Payment System SAFs for CYs 2006-2009; the inpatient SAFs represent similar data found in MedPAR but more granular since the SAFs’ unit of analysis is the claim and MedPAR data is aggregated to the beneficiary stay. Other publicly traded hospital groups have observation rates near or above the industry average. |
  12 CHS’ hospitals, classified by facility type, have observation rates well below national averages CHS’ observation rates by Medicare facility type are well below the rates for similar facilities across the U.S. * Non-CHS Average is comprised of all inpatient short-stay acute care hospitals excluding all CHS hospitals. |
  13 CHS’ hospitals have less than half the observation rate of hospitals in the same markets Observation rates for hospitals within the 3-digit zip codes of CHS hospitals are more than two times that of CHS hospitals. The location of CHS hospitals does not explain their low observation rate. |
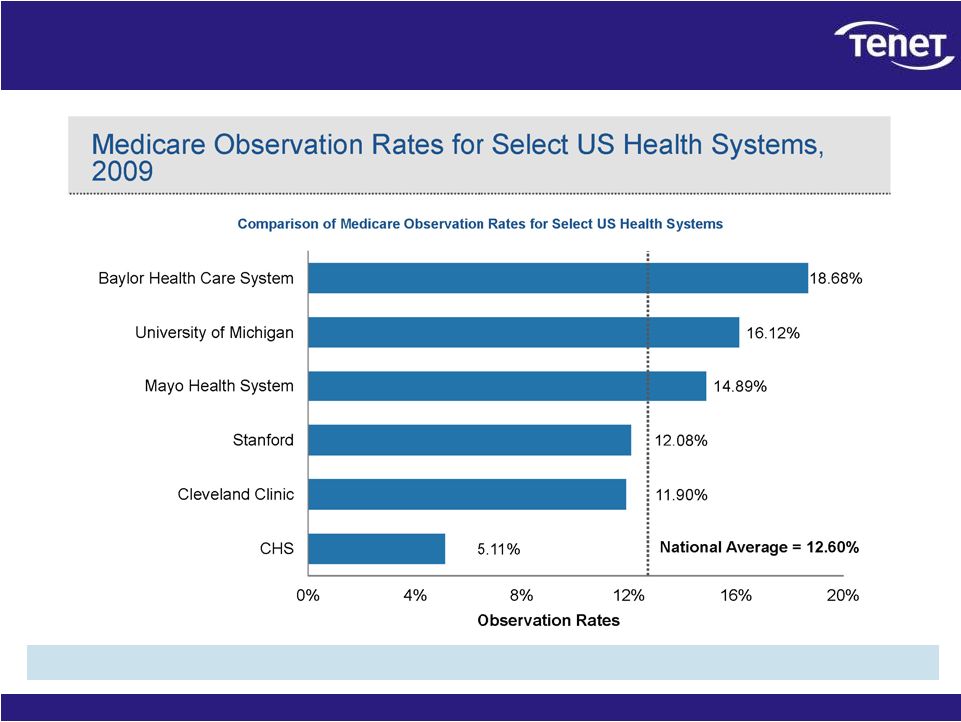  14 Prominent hospital groups do not have low observation rates Nationally recognized hospital groups have observation rates well in excess of CHS’. |
  15 The lower acuity mix of CHS’ hospitals does not explain CHS’ low observation rate Hospitals with lower acuity – like CHS – tend to have higher, not lower, observation rates. A hospital’s Medicare “Case Mix Index” measures the acuity level of its patients. Hospitals with a higher Case Mix Index see more acutely ill patients that require more complex or extensive treatments. Hospitals with a lower Case Mix Index see less acutely ill patients that require less complex or extensive treatments. The average CHS hospital has a lower Case Mix Index (1.28) than the average hospital nationally (1.43). This makes sense – CHS’ predominantly rural hospitals tend to see less acute patients who require less complex or extensive treatments. Statistical analysis shows that hospitals with a lower Case Mix Index have higher, not lower, observation rates. |
  16 There is no reasonable explanation for CHS’ high admission rate and low observation rate It’s not the facility type: CHS’ observation rate is well below industry peers with similar facility types including other rural hospitals. It’s not the location: CHS’ hospitals have less than half the observation rate of other hospitals in the same markets. It’s not the quality of care: CHS’ observation rate is lower than hospital groups known for high quality. It’s not the acuity mix: CHS’ lower acuity hospitals should result in a higher observation rate – not lower. |
  17 CHS uses the Blue Book to drive admissions higher and observations lower Approximately three-quarters of U.S. hospitals, as well as many Medicare auditors, utilize one of two sets of independent, evidence-based clinical criteria to determine whether a patient qualifies for inpatient admission. • Approximately 3,700 U.S. hospitals use the InterQual Criteria, developed by McKesson Corporation. • Approximately 1,000 U.S. hospitals use the Milliman Care Guidelines, developed by Milliman, Inc. • InterQual and Milliman were developed by independent physicians and contain thousands of medical references. CHS uses a 40-page “Blue Book.” • The CHS Blue Book was developed by CHS, copyrighted in 2000, and lacks a single reference to a medical journal or other independent source. • The Blue Book is utilized only by CHS’ hospitals. Unlike the InterQual and Milliman criteria, the Blue Book criteria are called “Admission Justifications.” In numerous cases, including those under scrutiny by regulators, the Blue Book justifies admission when standard clinical practice and InterQual and Milliman do not. CHS’ Blue Book is inconsistent with industry standard practice, but drives higher revenues and profits. |
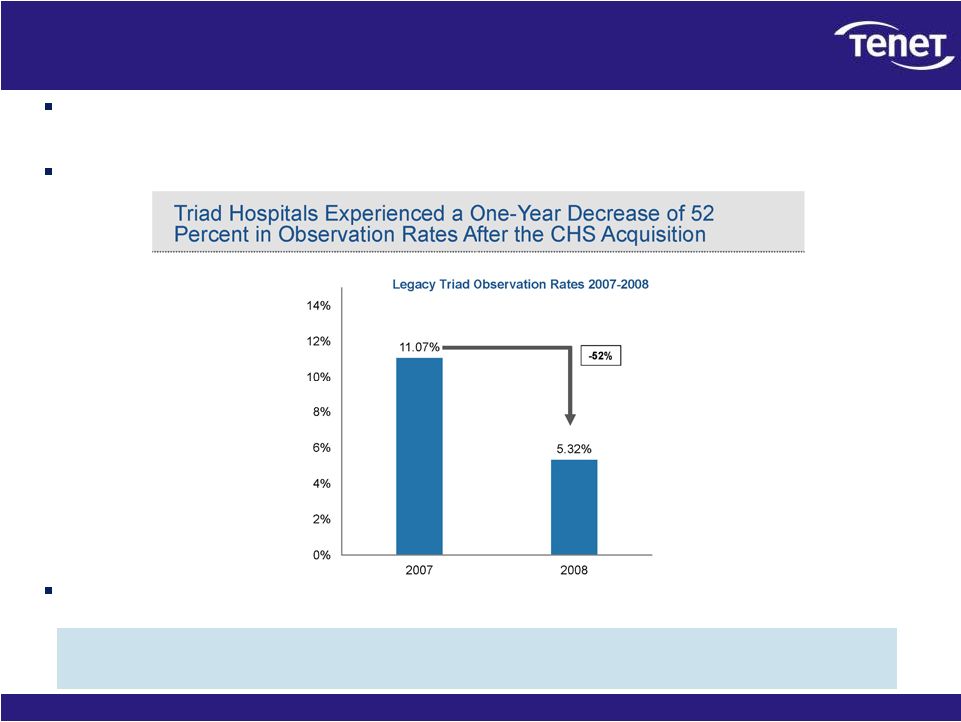  18 The Triad case study CHS has repeatedly cited the “synergies” it achieved in the acquisition of Triad Hospitals, Inc. in 2007. Never has it disclosed that these synergies were based on driving medically unnecessary admissions and reducing observations. Prior to its acquisition by CHS, Triad’s hospitals had an observation rate above the national average. Following CHS’ acquisition, the observation rate of the acquired Triad hospitals dropped by 52% while observation rates nationally were increasing. A potentially material portion of the “synergies” achieved at Triad resulted from driving down observation rates. |
  19 Tenet’s lawsuit seeks to compel CHS to disclose its admissions practices. CHS has increased its revenues and its profits by inappropriately billing Medicare, and likely state Medicaid programs and other payers, for higher-paying inpatient admissions rather than lower-paying outpatient observation stays. No other publicly traded hospital company follows a similar practice. CHS’ strategy is unsustainable; unwinding the practice will materially reduce admissions revenues, profits, and cash flows; and it has exposed the company to significant potential liabilities. Improper billings for Medicare fee-for-service patients are estimated at $280 million to $377 million between 2006-2009 alone. Revenue from Medicare fee-for-service patients represents only 27% of CHS’ net operating revenues. Revenues from other payers are also likely impacted. Liabilities for this conduct related to Medicare fee-for-service patients alone could be well in excess of $1 billion. The implications for CHS’ proposal to acquire Tenet: CHS’ stock is worth less than stated. CHS’ ability to finance the cash portion may be impaired. Summary |